 Back
BackAnatomy of the Skeletal System: Bones and Skeletal Tissues
Study Guide - Smart Notes

Anatomy of the Skeletal System
Overview of Bones and Skeletal Tissues
The skeletal system is composed of bones and cartilage, providing structural support, protection, and facilitating movement. Bones are dynamic organs that respond to mechanical stress and play a crucial role in mineral storage, blood cell formation, and hormone production.
Support: Bones form the framework that supports the body and cradles soft organs.
Protection: Bones protect vital organs (e.g., skull protects the brain, rib cage protects the heart and lungs).
Anchorage & Movement: Muscles attach to bones, enabling movement.
Mineral Storage: Bones store calcium and phosphorus, releasing them as needed.
Blood Cell Formation: Hematopoiesis occurs in red bone marrow.
Fat Storage: Yellow bone marrow stores fat.
Hormone Production: Osteocalcin regulates bone formation and influences metabolism.
Cartilage Tissue
Cartilage is a tough, flexible connective tissue found in various parts of the body. It is avascular and lacks nerve fibers, making it slow to heal. Cartilage consists of chondrocytes (mature cells) in lacunae, surrounded by a jelly-like extracellular matrix rich in glycosaminoglycans (GAGs) and collagen fibers.
Chondroblasts: Immature cells that actively form cartilage.
Chondrocytes: Mature cells that maintain cartilage.
Lacunae: Small cavities housing chondrocytes.
Perichondrium: Dense connective tissue layer surrounding cartilage, providing nutrients and aiding repair.
Types of Cartilage
Hyaline Cartilage: Most abundant; provides firm support and pliability; found in articular surfaces, costal cartilages, nose, trachea.
Elastic Cartilage: Contains more elastic fibers; found in external ear and epiglottis.
Fibrocartilage: Rows of chondrocytes and thick collagen fibers; great tensile strength; found in intervertebral discs and pubic symphysis.
Growth of Cartilage
Appositional Growth: New matrix is added to the surface, increasing width.
Interstitial Growth: Chondrocytes divide and secrete new matrix within cartilage, increasing length.
Cartilage growth ends during adolescence.
Classification and Structure of Bones
Classification of Bones
There are 206 named bones in the human skeleton, classified by shape:
Long Bones: Longer than they are wide (e.g., femur, humerus).
Short Bones: Cube-shaped (e.g., carpals, tarsals).
Flat Bones: Thin, flattened, and usually curved (e.g., sternum, skull).
Irregular Bones: Complex shapes (e.g., vertebrae, hip bones).
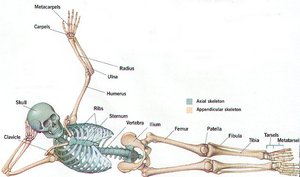
Axial vs. Appendicular Skeleton
Axial Skeleton: Skull, vertebral column, rib cage; supports and protects organs.
Appendicular Skeleton: Limbs and girdles; facilitates movement.
Structure of a Typical Long Bone
Diaphysis: Tubular shaft; collar of compact bone surrounds medullary cavity (yellow marrow in adults).
Epiphyses: Bone ends; compact bone externally, spongy bone internally; articular cartilage covers joint surfaces.
Epiphyseal Line: Remnant of growth plate; marks fusion of diaphysis and epiphysis.
Membranes: Periosteum (outer covering), Endosteum (internal lining).
Structure of Short, Irregular, and Flat Bones
Thin plates of spongy bone covered by compact bone.
No shaft, marrow cavity, or epiphyses; bone marrow found between trabeculae.
Microscopic Anatomy of Bone
Types of Bone Cells
Osteoprogenitor (osteogenic) cells: Stem cells that differentiate into osteoblasts.
Osteoblasts: Bone-forming cells; secrete osteoid.
Osteocytes: Mature bone cells; maintain bone matrix.
Osteoclasts: Bone-resorbing cells; break down bone matrix.
Microscopic Anatomy of Compact Bone
Osteon (Haversian system): Structural unit; cylindrical, parallel to bone axis; consists of concentric lamellae.
Central (Haversian) Canal: Contains blood vessels and nerves.
Perforating (Volkmann’s) Canals: Connect periosteum, medullary cavity, and central canal.
Lacunae: Small cavities with osteocytes.
Canaliculi: Hairlike canals connecting lacunae; allow communication and nutrient/waste exchange.
Interstitial Lamellae: Fill gaps between osteons.
Circumferential Lamellae: Extend around bone shaft; resist twisting.
Microscopic Anatomy of Spongy Bone
Contains trabeculae, lamellarly arranged osteocytes, and canaliculi.
Trabeculae align along lines of stress; confer strength.
No osteons; nutrients diffuse through canaliculi from marrow spaces.
Chemical Composition of Bone
Organic Components: Osteogenic cells, osteoblasts, osteocytes, bone-lining cells, osteoclasts, and osteoid (ground substance and collagen fibers).
Inorganic Components: Hydroxyapatites (calcium phosphate crystals); provide hardness and resistance to compression.
Bone strength: Half as strong as steel in compression, as strong as steel in tension.
Bone Formation and Growth
Ossification (Bone Development)
Endochondral Ossification: Bone forms by replacing hyaline cartilage; most bones below the skull.
Intramembranous Ossification: Bone develops from fibrous connective tissue; forms flat bones (skull, clavicles).
Steps in Intramembranous Ossification
Ossification centers form as mesenchymal cells become osteoblasts.
Osteoid is secreted and calcified.
Woven bone forms around blood vessels, creating trabeculae.
Lamellar bone replaces woven bone; red bone marrow appears.
Postnatal Bone Growth
Long bones lengthen by interstitial growth at epiphyseal plates.
Bones grow in thickness by appositional growth.
Epiphyseal plate closure marks end of longitudinal growth (age 18-21).
Bone Remodeling
Bone deposit and resorption occur at periosteum and endosteum surfaces.
Remodeling units: osteoblasts and osteoclasts coordinate the process.
Spongy bone replaced every 3-4 years; compact bone every 10 years.
Hormonal Regulation of Bone Growth
Growth Hormone: Stimulates epiphyseal plate activity.
Thyroid Hormone: Modulates growth hormone activity.
Sex Hormones: Promote growth spurts and induce epiphyseal plate closure.
Control of Bone Remodeling
Parathyroid Hormone (PTH): Increases blood calcium by stimulating osteoclasts.
Calcitonin: Lowers blood calcium levels (minor effect).
Mechanical and gravitational forces drive remodeling to keep bone strong.
Bone Markings
Types of Bone Markings
Projections: Outward bulges for muscle, ligament, and tendon attachment.
Depressions and Openings: Allow passage of blood vessels and nerves.
Surfaces: Areas involved in joint formation.
Refer to Table 6.2 for detailed bone markings.
Osteoporosis
Overview
Osteoporosis is a group of diseases where bone resorption exceeds formation, leading to porous and fragile bones. Commonly affects the spine and neck of femur.
Risk Factors: Age, post-menopausal women, insufficient exercise, poor diet, smoking, genetics, diabetes mellitus.
Estrogen: Promotes bone health by restraining osteoclast activity.
Bone Repair
Stages of Fracture Repair
Hematoma Formation: Blood clot forms; cells die; inflammation occurs.
Fibrocartilaginous Callus Formation: Blood vessels invade; fibroblasts, chondroblasts, and osteoblasts lay down new tissue.
Bony Callus Formation: Cartilage is converted to trabecular bone (~2 months).
Bone Remodeling: Excess material removed; compact bone restored.
Final structure resembles original bone and responds to mechanical stress.
Additional info: These notes expand on brief points with academic context, definitions, and examples to ensure completeness and clarity for exam preparation.
