 Back
BackAutonomic Nervous System: Structure, Function, and Neurotransmitters
Study Guide - Smart Notes

Autonomic Nervous System (ANS) Overview
General Structure and Function
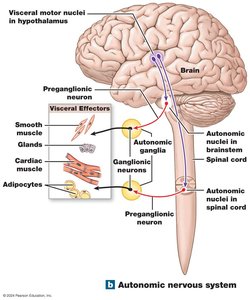
The Autonomic Nervous System (ANS) is responsible for involuntary regulation of internal organs, maintaining homeostasis through control of visceral effectors such as smooth muscle, cardiac muscle, glands, and adipose tissue. The ANS operates through a two-neuron pathway: a preganglionic neuron originating in the CNS and a postganglionic neuron located in autonomic ganglia, which innervates target tissues.
Visceral motor nuclei in the hypothalamus initiate autonomic responses.
Preganglionic neurons originate in the brainstem or spinal cord.
Autonomic ganglia house ganglionic neurons that relay signals to effectors.
Postganglionic axons innervate visceral effectors.
Divisions of the ANS
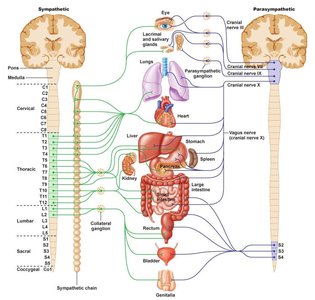
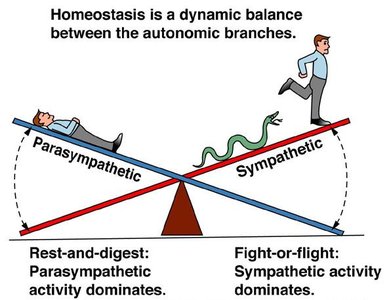
The ANS is divided into two main branches: the Sympathetic Division (fight or flight) and the Parasympathetic Division (rest and digest). These divisions have opposing effects and work together to maintain physiological balance.
Sympathetic Division: Prepares the body for emergencies and stress.
Parasympathetic Division: Promotes relaxation and energy conservation.
Sympathetic Division
Anatomical Organization
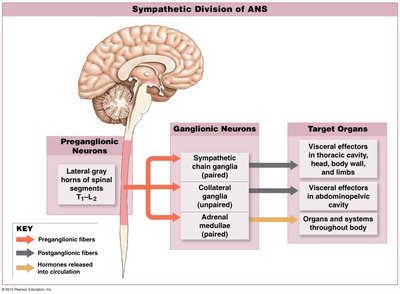
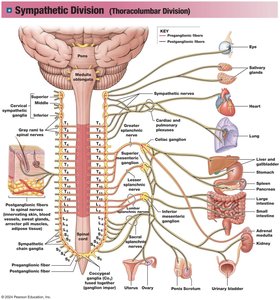
The Sympathetic Division is structured to mobilize resources during stressful situations. Preganglionic fibers originate in the thoracic and lumbar segments (T1-L2) of the spinal cord. Sympathetic ganglia are located near the spinal cord and include chain ganglia, collateral ganglia, and the adrenal medullae.
Chain ganglia: Paired structures alongside the spinal cord, controlling effectors in the body wall, thoracic cavity, head, neck, and limbs.
Collateral ganglia: Unpaired, anterior to the spinal cord, controlling abdominopelvic tissues and organs.
Adrenal medullae: Modified ganglia within the adrenal gland, releasing hormones directly into the bloodstream.
Preganglionic axons: Short, originating from T1-L2.
Postganglionic axons: Long, innervating multiple targets.
Functions and Effects
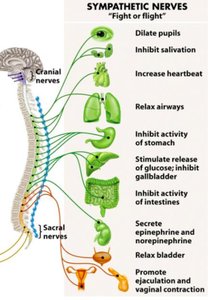
The sympathetic division increases alertness and prepares the body for rapid action. Its effects include:
Heightened mental alertness
Pupil dilation
Increased metabolic rate and ATP production
Reduced digestive and urinary functions
Activation of energy reserves
Increased respiratory rate and dilation of passageways
Increased heart rate and blood pressure
Activation of sweat glands
Orgasm
Activation Mechanisms
Sympathetic activation involves a coordinated response, often affecting the entire division simultaneously. This includes increased alertness, stimulation of the reticular activating system, elevated muscle tone, mobilization of energy reserves, and breakdown of glycogen and lipids.
Parasympathetic Division
Anatomical Organization
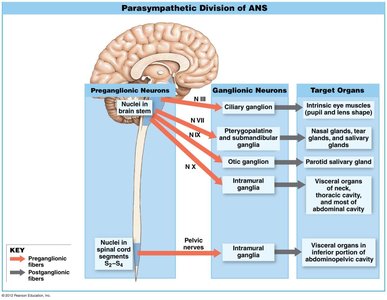
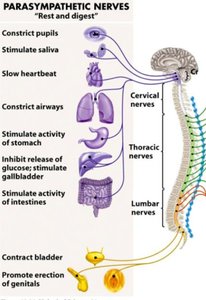
The Parasympathetic Division produces more targeted effects than the sympathetic division. Preganglionic fibers originate in the brainstem (cranial nerves III, VII, IX, X) and sacral segments (S2-S4). Ganglia are located near or within target organs, including terminal and intramural ganglia.
Long preganglionic axons: Originate in brainstem and sacral region.
Ganglia: Located within or adjacent to target organs.
Short postganglionic axons: Innervate specific targets.
Vagus nerve: Contributes to about 75% of all parasympathetic output.
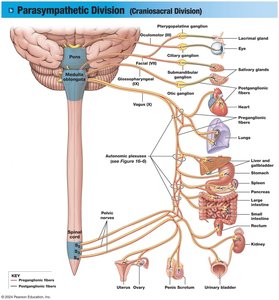
Functions and Effects
The parasympathetic division promotes relaxation, food processing, and nutrient absorption. Its effects include:
Decreased metabolic rate and ATP production
Decreased heart rate and blood pressure
Constriction of respiratory passages
Increased secretion by salivary and digestive glands
Increased blood flow to digestive tract
Stimulation of urination and defecation
Constriction of pupils
Sexual arousal and erection
Activation Mechanisms
Unlike the sympathetic division, the parasympathetic division does not activate the entire system at once. Its functions are considered the default state, focusing on relaxation and nutrient absorption.
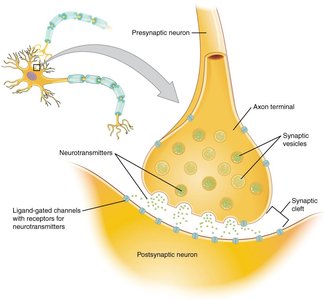
Neurotransmitters and Receptors
Acetylcholine (ACh)
Acetylcholine is released by cholinergic neurons and acts on two types of receptors:
Nicotinic receptors: Found in neuromuscular junctions and both divisions of the ANS; ionotropic, causing excitation.
Muscarinic receptors: Found in the parasympathetic division; metabotropic, can be excitatory or inhibitory.
ACh is rapidly broken down by acetylcholinesterase (AChE) and cholinesterase.
Norepinephrine and Epinephrine
Norepinephrine is released by adrenergic neurons, with effects lasting longer than ACh. It is reabsorbed and broken down by monoamine oxidase (MAO) and catechol-O-methyltransferase (COMT). Epinephrine stimulates both alpha and beta receptors.
Alpha receptors: Metabotropic; alpha-1 (excitatory), alpha-2 (inhibitory).
Beta receptors: Metabotropic; beta-1 (excitatory, increases heart rate), beta-2 (inhibitory, relaxes respiratory muscles), beta-3 (excitatory, in adipose tissue).
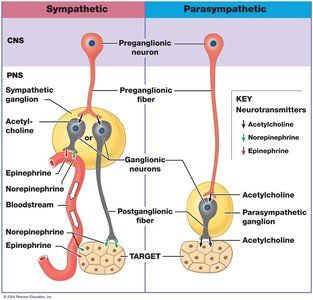
Neurotransmitter Pathways in ANS
Sympathetic Division: Preganglionic neurons release acetylcholine (nicotinic receptors); postganglionic neurons release mostly norepinephrine (alpha and beta receptors).
Parasympathetic Division: Preganglionic neurons release acetylcholine (nicotinic receptors); postganglionic neurons release acetylcholine (muscarinic receptors).
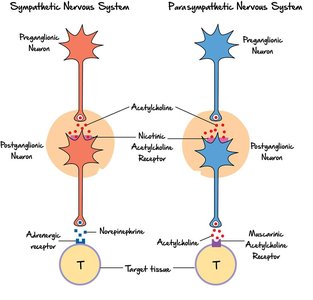
Comparison of Sympathetic and Parasympathetic Divisions
Structural and Functional Differences
The following table summarizes the key differences between the sympathetic and parasympathetic divisions:
Characteristic | Sympathetic | Parasympathetic |
|---|---|---|
Origin of Preganglionic Neuron | Spinal Segments T1-L2 | Cranial Nerves III, VII, IX, X; Sacral Segments S2-S4 |
Location of Peripheral Ganglia | Near spinal cord | Near or within target organ/tissue |
Preganglionic Fiber Length | Short | Long |
Postganglionic Fiber Length | Long | Short |
Preganglionic Neurotransmitter (receptor) | ACh (Nicotinic) | ACh (Nicotinic) |
Postganglionic Neurotransmitter (receptor) | Mostly Norepinephrine (Alpha and Beta) | Acetylcholine (Muscarinic) |
Target Area | Broad | Specific |
General Function | Stimulates metabolism, increases alertness, prepares for emergency | Promotes relaxation, nutrient uptake, energy storage |
Example: During a stressful event, the sympathetic division increases heart rate and dilates pupils, while the parasympathetic division slows heart rate and constricts pupils during relaxation.
Additional info: The ANS is essential for maintaining homeostasis and adapting to changing internal and external environments.
