 Back
BackAutonomic Nervous System: Structure, Function, and Integration
Study Guide - Smart Notes

Autonomic Nervous System (ANS)
Overview of the ANS
The Autonomic Nervous System (ANS) is a division of the peripheral nervous system responsible for regulating involuntary physiological processes, including heart rate, blood pressure, respiration, digestion, and sexual arousal. It operates largely without conscious control, integrating signals from the central nervous system (CNS) and peripheral nervous system (PNS) to maintain homeostasis.
Central Nervous System (CNS): Consists of the brain and spinal cord; processes and integrates sensory information and coordinates motor output.
Peripheral Nervous System (PNS): Includes all neural tissue outside the CNS; divided into sensory (afferent) and motor (efferent) divisions.
Somatic Nervous System (SNS): Controls voluntary movements of skeletal muscles.
Autonomic Nervous System (ANS): Controls involuntary effectors such as smooth muscle, cardiac muscle, glands, and adipose tissue.
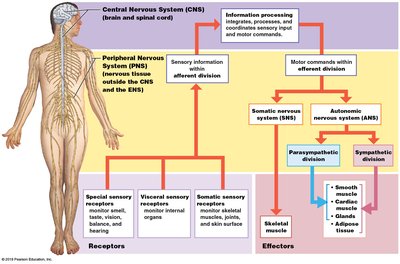
Functional Organization of the Nervous System
The nervous system is organized into sensory input, information processing, and motor output. Sensory receptors detect changes in the environment and send information to the CNS, which processes the information and sends commands to effectors via the PNS.
Receptors: Specialized cells or structures that detect stimuli (e.g., special sensory receptors, visceral sensory receptors, somatic sensory receptors).
Effectors: Target organs or tissues that respond to neural commands (e.g., skeletal muscle, smooth muscle, cardiac muscle, glands, adipose tissue).
Divisions of the ANS
The ANS is divided into two main branches, each with distinct anatomical and functional characteristics:
Sympathetic Division: Prepares the body for 'fight or flight' responses; dominant during physical or emotional stress. Increases heart rate, dilates pupils, inhibits digestion, and increases blood flow to muscles.
Parasympathetic Division: Promotes 'rest and digest' activities; dominant during restful states. Decreases heart rate, constricts pupils, stimulates digestion, and conserves energy.
Dual and Single Innervation
Dual Innervation: Most organs receive input from both sympathetic and parasympathetic divisions, often with opposing effects (e.g., heart rate, pupil diameter, digestive activity).
Single Innervation: Some effectors receive input from only one division (e.g., sweat glands and most blood vessels receive only sympathetic input; lacrimal glands receive only parasympathetic input).
Structure of the ANS
Efferent Pathways
The ANS uses a two-neuron efferent pathway:
Preganglionic Neuron: Cell body in the CNS; axon projects to an autonomic ganglion in the PNS.
Ganglionic (Postganglionic) Neuron: Cell body in the autonomic ganglion; axon projects to the effector organ.
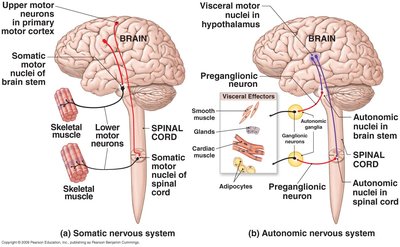
Anatomical Differences: Sympathetic vs. Parasympathetic
Sympathetic (Thoraco-lumbar Division):
Preganglionic neurons originate in the lateral horns of spinal cord segments T1-L2.
Preganglionic axons are typically short; ganglia are close to the CNS (sympathetic chain ganglia, collateral ganglia, adrenal medulla).
Parasympathetic (Cranio-sacral Division):
Preganglionic neurons originate in brainstem nuclei (cranial nerves III, VII, IX, X) and sacral spinal cord segments S2-S4.
Preganglionic axons are typically long; ganglia are near or within the effector organ (intramural ganglia).
Organization and Anatomy of the Sympathetic Division
Sympathetic Chain Ganglia
Located in two chains on either side of the vertebral column.
Innervate head, body wall, limbs, and thoracic viscera (heart, lungs).
Collateral Ganglia
Located near large abdominal arteries (celiac, superior mesenteric, inferior mesenteric ganglia).
Innervate abdominal and pelvic viscera; decrease digestive activity and blood flow to these organs.
Adrenal Medulla
Central portion of the adrenal gland; contains modified postganglionic neurons.
Secretes epinephrine (E) and norepinephrine (NE) into the bloodstream, producing widespread effects.
Organization and Anatomy of the Parasympathetic Division
Cranial Nerves Involved
Cranial Nerve III (Oculomotor): Controls pupil constriction and lens shape.
Cranial Nerve VII (Facial): Controls lacrimal and salivary glands.
Cranial Nerve IX (Glossopharyngeal): Controls salivary glands.
Cranial Nerve X (Vagus): Provides 75% of parasympathetic output; controls heart, lungs, digestive tract, and most thoracic and abdominal viscera.
Sacral Outflow
Preganglionic neurons in S2-S4 segments send axons via pelvic nerves to intramural ganglia in the lower abdominal and pelvic organs.
Autonomic Activation and Effects
Sympathetic Activation
Widespread effects due to extensive branching of preganglionic axons and hormonal release from adrenal medulla.
Each preganglionic axon may synapse with 24 or more ganglionic cells.
Parasympathetic Activation
Localized effects; innervation limited to head and viscera.
Each preganglionic axon synapses with 6-8 ganglionic cells; postganglionic axons usually target a single effector.
Neurotransmitters and Receptors in the ANS
Cholinergic Synapses
Nicotinic Receptors: Found in autonomic ganglia and skeletal muscle; always excitatory.
Muscarinic Receptors: Found in visceral organs, cardiac muscle, and CNS; can be excitatory or inhibitory.
Adrenergic Synapses
Alpha (α) Receptors:
α1: Excitatory (e.g., vasoconstriction, sphincter contraction).
α2: Inhibitory (e.g., reduces GI motility and secretions).
Beta (β) Receptors:
β1: Excitatory (e.g., increases heart rate and contractility).
β2: Inhibitory (e.g., bronchodilation, vasodilation in skeletal muscle).
β3: Excitatory (e.g., lipolysis in adipose tissue).
Neurotransmitter Release
All preganglionic neurons (sympathetic and parasympathetic) release acetylcholine (ACh).
All parasympathetic postganglionic neurons release ACh.
Most sympathetic postganglionic neurons release norepinephrine (NE); some release ACh or nitric oxide (NO).
Adrenal medulla releases epinephrine (E) and norepinephrine (NE) into the bloodstream.
Integration and Control of Autonomic Functions
Autonomic Tone
Background level of activity in autonomic neurons; can be increased or decreased to modulate effector activity.
Examples: Heart rate (dual innervation), blood vessel diameter (sympathetic only).
Visceral Reflexes
Short Reflexes: Bypass the CNS; involve sensory neurons and interneurons in autonomic ganglia; control localized responses (e.g., enteric nervous system in the gut).
Long Reflexes: Involve CNS processing; coordinate activity of entire organs.
Higher Levels of Autonomic Control
Reflex centers in the hypothalamus regulate autonomic function and are influenced by the limbic system, thalamus, and cerebral cortex.
The hypothalamus is the master control center for autonomic and endocrine integration, regulating body temperature, circadian rhythms, emotions, and behavioral drives.
Pharmacology and the ANS
Propranolol: Beta-1 and beta-2 blocker; reduces heart rate and blood pressure.
Metoprolol: Beta-1 specific blocker; used for hypertension and heart disease.
Albuterol: Beta-2 agonist; used for bronchodilation in asthma.
Nicotine: Nicotinic cholinergic agonist; stimulates autonomic ganglia.
Atropine: Muscarinic cholinergic blocker; inhibits parasympathetic effects.
Summary Table: Dual Innervation Examples
Effector Organ | Sympathetic Effect (Receptor) | Parasympathetic Effect (Receptor) |
|---|---|---|
Eyes (Iris Muscle) | Contracts radial muscle (α1, widens pupil) | Contracts sphincter muscle (Muscarinic, constricts pupil) |
Heart (SA Node) | Increases heart rate (β1) | Decreases heart rate (Muscarinic) |
Arterioles (Coronary) | Constriction (α1), Dilation (β2) | Dilation (Muscarinic) |
Bronchiole Muscles | Relaxation/dilation (β2) | Constriction (Muscarinic) |
Summary Table: Sympathetic Only Innervation
Effector Organ | Sympathetic Effect (Receptor) | Parasympathetic Effect |
|---|---|---|
Kidneys | Increase renin secretion (β1) | None |
Skin (Arrector pili muscle) | Contraction (α1) | None |
Liver | Glycogenolysis and gluconeogenesis (α1 & β1) | None |
Skin (Arterioles) | Constriction (α1) | None |
Additional info: The above tables summarize the main effects of sympathetic and parasympathetic divisions on various organs, highlighting the concept of dual and single innervation in the ANS.
