 Back
BackBlood, Cardiovascular, Lymphatic, and Immune Systems: ANP College Study Notes
Study Guide - Smart Notes

Blood
Functions of Blood
Blood is a vital connective tissue with multiple essential functions in the human body.
Transport: Carries gases (O2 and CO2), nutrients, metabolic wastes, hormones, and stem cells throughout the body.
Protection: Involves white blood cells, antibodies, and proteins that neutralize pathogens, initiate inflammation, and enable blood clotting.
Regulation: Maintains fluid balance, stabilizes pH, and regulates body temperature.
Erythrocytes (Red Blood Cells)
Erythrocytes are specialized cells responsible for gas transport.
Main Functions:
Transport oxygen from the lungs to tissues.
Carry carbon dioxide from tissues to the lungs for exhalation.

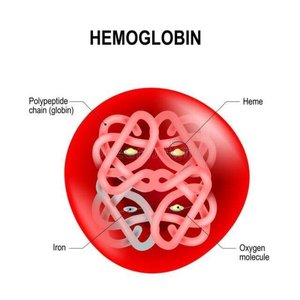
Hemoglobin
Hemoglobin is the red, iron-containing protein in erythrocytes that binds and transports gases.
Structure: Composed of four polypeptide chains (globins), each bound to a heme group containing an iron atom.
Function: Each iron atom binds one O2 molecule, so one hemoglobin can carry up to four O2 molecules. Hemoglobin also transports about 5% of CO2 (which binds to globin chains).
Simultaneous Transport: Hemoglobin can carry both O2 and CO2 at the same time.
Blood Typing
Blood typing is based on the presence of specific antigens on the surface of erythrocytes and the corresponding antibodies in plasma.
Antigens: Cell surface markers that help the body distinguish self from non-self.
Antibodies: Proteins that recognize and bind to antigens, initiating an immune response. When antibodies bind to antigens on cells, they cause agglutination (clumping).
Blood Types: The body naturally produces antibodies against antigens of other blood types.

Universal Donor and Recipient
Universal Donor: Type O (no antigens on RBCs, but both anti-A and anti-B antibodies in plasma).
Universal Recipient: Type AB (no antibodies in plasma, both antigens on RBCs).
Antibodies are found in plasma, not on RBCs.
Leukocytes (White Blood Cells)
Leukocytes are immune cells classified by the presence or absence of granules in their cytoplasm.
Granulocytes: Contain granules with enzymes and chemicals for defense.
Neutrophils
Eosinophils
Basophils
Agranulocytes: Lack specific granules.
Monocytes
Lymphocytes

Platelets and Hemostasis
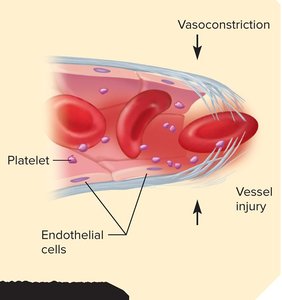
Platelets are cell fragments essential for stopping bleeding (hemostasis), which occurs in three stages:
Vascular spasm: Vasoconstriction reduces blood flow after vessel injury.
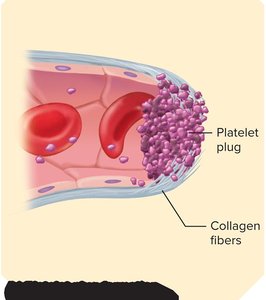
Platelet plug formation: Platelets adhere to exposed collagen fibers and each other, forming a temporary plug.
Coagulation: Fibrin forms a mesh that traps blood cells, creating a stable clot.

Agglutination vs. Coagulation
Agglutination: RBCs stick together due to antibodies (important in blood typing and transfusion reactions).
Coagulation: Blood cells and platelets are held together by fibrin (important in hemostasis).

Cardiovascular System
Blood Flow Through the Heart
The heart pumps blood through two circuits: pulmonary (to the lungs) and systemic (to the body).
Deoxygenated blood returns from tissues via the superior and inferior vena cava to the right atrium.
Blood flows through the right atrioventricular (AV) valve into the right ventricle.
Right ventricle contracts, sending blood through the pulmonary semilunar valve into the pulmonary trunk and to the lungs.
Oxygenated blood returns from the lungs via pulmonary veins to the left atrium.
Blood flows through the left AV valve into the left ventricle.
Left ventricle contracts, ejecting blood through the aortic semilunar valve into the aorta for systemic circulation.

The Cardiac Cycle
The cardiac cycle is one complete contraction and relaxation of all four heart chambers, from the start of one heartbeat to the next.
Systole: Contraction phase; blood is expelled from the chamber.
Diastole: Relaxation phase; chamber refills with blood.

Blood Vessels and Blood Pressure
General Anatomy of Blood Vessels
Blood vessels are classified by structure and function:
Arteries: Carry blood away from the heart; have thick, muscular, and elastic walls to withstand high pressure.
Veins: Carry blood toward the heart; have thinner walls and valves to prevent backflow.
Capillaries: Microscopic vessels where exchange of gases, nutrients, and wastes occurs; composed of a single endothelial layer (tunica interna).
Vessel Wall Structure
Tunica interna: Inner lining of endothelium; selectively permeable and regulates vessel tone.
Tunica media: Middle layer of smooth muscle, collagen, and elastic tissue; responsible for vasoconstriction and vasodilation.
Tunica externa: Outer connective tissue layer (not detailed above but standard in anatomy).
Blood Pressure
Blood pressure is the force exerted by blood on vessel walls, driving blood flow from high to low pressure areas.
Arterial blood pressure: Expressed as systolic/diastolic (e.g., 120/80 mmHg).
Systolic pressure: Generated by ventricular contraction.
Diastolic pressure: Lowest pressure during ventricular relaxation.
Measured with: Sphygmomanometer.
Peripheral Resistance
Peripheral resistance is the opposition to blood flow in vessels away from the heart, determined by:
Viscosity: Thickness of blood; increased by more erythrocytes or plasma proteins.
Vessel length: Longer vessels increase resistance.
Vessel radius: Most important; vasoconstriction (narrowing) increases resistance, vasodilation (widening) decreases resistance.
Regulation of Blood Pressure and Flow
Local control: Tissues with high metabolic demand release chemicals (e.g., histamine, nitric oxide) to dilate vessels and increase perfusion. Chronic demand leads to angiogenesis (new vessel growth).
Neural control: Baroreceptors detect pressure changes and signal the medulla oblongata to adjust vessel diameter and heart rate (baroreflexes).
Hormonal control: Hormones such as epinephrine, norepinephrine, angiotensin II, natriuretic peptides, aldosterone, and antidiuretic hormone regulate vessel tone and blood volume.
Lymphatic System
Components of the Lymphatic System
Lymph: Fluid collected from tissues, returned to the bloodstream.
Lymphatic vessels: Transport lymph through the body.
Lymphatic tissue: Aggregations of lymphocytes in connective tissue (e.g., digestive and respiratory tracts).
Lymphatic organs: Structured masses of lymphatic tissue (tonsils, thymus, spleen, lymph nodes).
Lymph Vessel Structure and Movement
Similar to veins: three-layered walls and one-way valves.
No central pump; lymph moves via vessel wall contraction, skeletal muscle pump, thoracic pump (breathing), and blood flow at drainage points.
Immune System
Overview of Immunity
The immune system protects against pathogens (viruses, bacteria, fungi, protozoa, worms) using innate and adaptive mechanisms.
Innate immunity: Non-specific, present from birth; includes barriers, cells, and proteins that attack invaders and promote inflammation and fever.
Adaptive immunity: Specific, develops after exposure; tailored to particular pathogens and provides immunological memory.
Innate Immune System: Protective Cells
Neutrophils: Phagocytize bacteria and secrete chemicals to kill pathogens.
Eosinophils: Attack large parasites.
Basophils: Release histamine (vasodilator) and heparin (anticoagulant).
Monocytes: Become macrophages, phagocytize pathogens.
Natural killer (NK) cells: Destroy infected or abnormal cells by releasing perforins and enzymes.
Innate Immune System: Protective Proteins
Interferons: Released by virus-infected cells; signal neighboring cells to inhibit viral replication and activate NK cells.
Complement system: Liver-produced proteins that, when activated, destroy microbes and enhance antibody action.
Innate Immunity: Inflammation and Fever
Inflammation: Increases blood flow, brings immune cells to affected area, removes debris, and initiates repair. Causes heat, redness, swelling, and pain.
Fever: Elevated body temperature due to infection; inhibits pathogen replication, increases interferon activity, and accelerates tissue repair. Pyrogens from immune cells stimulate the hypothalamus to raise body temperature.
Adaptive Immune System
Specificity: Targets particular pathogens.
Memory: Faster, stronger response upon re-exposure to the same pathogen.
Forms of Adaptive Immunity
Cell-mediated immunity: T lymphocytes directly attack infected or abnormal cells (e.g., intracellular pathogens, cancer cells, transplant rejection).
Humoral immunity: B lymphocytes produce antibodies that tag pathogens for destruction.
Antigens and Antibodies
Antigens: Molecules (proteins, polysaccharides, glycoproteins, glycolipids) that trigger immune responses; can be cell-surface markers or toxins.
Antibodies: Y-shaped proteins secreted by plasma cells (activated B cells); bind specific antigens and mark them for destruction.

Lymphocytes
T lymphocytes: Mature in the thymus; responsible for cell-mediated immunity.
B lymphocytes: Mature in bone marrow; responsible for humoral immunity.
Both originate in red bone marrow and populate lymphatic tissues.
Antigen-Presenting Cells (APCs)
APCs (macrophages, dendritic cells) process and present antigens to T cells, using interleukins for communication.
Cell-Mediated Immunity
Cytotoxic T cells: Attack infected or abnormal cells.
Helper T cells: Stimulate cytotoxic T cells and B cells.
Memory T cells: Provide long-term immunity by remembering pathogens.
Stages: Recognition, Attack, Memory.
Humoral Immunity
B cells recognize antigens, are activated by helper T cells, undergo clonal selection, and differentiate into plasma cells (produce antibodies) and memory B cells.
Stages: Recognition, Attack, Memory.
Primary response: First exposure; Secondary response: Faster, stronger response upon re-exposure.
Active vs. Passive Immunity
Active immunity: Body produces its own antibodies/T cells (natural: infection; artificial: vaccination).
Passive immunity: Antibodies acquired from another source (natural: maternal antibodies; artificial: immune serum, e.g., anti-venoms).
