 Back
BackBlood: Structure, Function, and Clinical Relevance
Study Guide - Smart Notes

Blood Characteristics
Overview of Blood
Blood is a specialized connective tissue composed of cells suspended in a liquid extracellular matrix called plasma. It plays a vital role in transporting substances, regulating physiological parameters, and protecting the body against disease.
Hematocrit: The percentage of red blood cells (RBCs) in the blood, typically around 45% in healthy adults.
Plasma: The liquid component of blood, making up about 55% of total blood volume.
Cells: Includes erythrocytes (RBCs), leukocytes (WBCs), and platelets.
Note: The mention of "Actin (hormone)" is likely a confusion; actin is a cytoskeletal protein, not a hormone. Blood flow is regulated by hormones such as epinephrine and vasopressin.
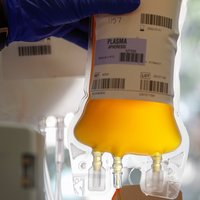
Plasma
Composition and Function
Plasma is the extracellular matrix of blood, consisting mainly of water and dissolved substances. It serves as the medium for transporting nutrients, hormones, and waste products throughout the body.
Water: Makes up about 92% of plasma, serving as a solvent for carrying other substances.
Electrolytes: Simple ions such as sodium, potassium, calcium, and chloride that help maintain osmotic balance and proper cell function.
Nutrients: Glucose, amino acids, fatty acids, and vitamins are transported by plasma to cells.
Plasma Proteins:
Albumins: Maintain osmotic pressure and transport substances.
Globulins: Involved in immune responses and transport of lipids and fat-soluble vitamins.
Fibrinogen: Essential for blood clotting.
Red Blood Cells (Erythrocytes)
Structure and Function
Red blood cells are the most numerous cells in the blood and are specialized for oxygen transport. Their unique biconcave disc shape increases surface area for gas exchange and flexibility for passage through capillaries.
Biconcave Disc: Increases surface area for efficient gas exchange.
Lack of Nucleus and Mitochondria: Maximizes space for hemoglobin and prevents consumption of transported oxygen.

Hemoglobin and RBC Lifecycle
Hemoglobin is the protein responsible for oxygen transport in RBCs. The oxygen-carrying capacity of blood is determined by the amount of hemoglobin present. Old RBCs are removed by the liver and spleen, where hemoglobin is broken down and bilirubin is produced as a waste product. Erythropoietin, a hormone produced by the kidneys, stimulates RBC production in response to low oxygen levels.
Hemoglobin: Binds and transports oxygen and carbon dioxide.
Bilirubin: A yellow pigment formed from the breakdown of hemoglobin, excreted in bile.
Erythropoietin: Hormone that stimulates RBC production in the bone marrow.
RBC Formation and Nutritional Requirements
Red blood cell production (erythropoiesis) occurs in the red bone marrow. Erythroblasts are precursor cells that synthesize hemoglobin. Adequate levels of vitamin B12, folic acid, and iron are essential for normal RBC formation.
Vitamin B12 and Folic Acid: Required for DNA synthesis during RBC production.
Iron: Essential component of hemoglobin.
Anemia: Types and Causes
Anemia is a condition in which the blood cannot carry sufficient oxygen to tissues. It can result from various causes:
Hemorrhagic Anemia: Due to blood loss from internal or external bleeding.
Hemolytic Anemia: Caused by premature destruction of RBCs (e.g., malaria infection).
Aplastic Anemia: Failure of red bone marrow, often due to radiation exposure.
Sickle Cell Anemia: Genetic disorder causing abnormal hemoglobin and misshapen RBCs.

Blood Typing
ABO Blood Groups and Transfusion Compatibility
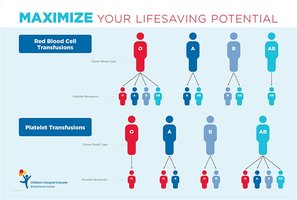
Blood typing is essential for safe transfusions. The ABO system classifies blood based on the presence of antigens on RBC surfaces:
Type A: Has A antigens on RBCs and anti-B antibodies in plasma.
Type B: Has B antigens and anti-A antibodies.
Type AB: Has both A and B antigens; universal recipient for RBCs.
Type O: Has no A or B antigens; universal donor for RBCs.
AB is considered the universal recipient, while O is the universal donor for red blood cells.
White Blood Cells (Leukocytes)
Function and Types
White blood cells are crucial for immune defense. They have a nucleus and can leave the bloodstream (diapedesis) to migrate to sites of infection or injury.
Granular Leukocytes: Short-lived cells with granules in their cytoplasm.
Neutrophils: Most abundant, phagocytize bacteria and debris.
Eosinophils: Combat parasitic infections and modulate allergic responses.
Basophils: Release histamine and heparin during inflammatory reactions.
Agranular Leukocytes: Lack visible granules.
Monocytes: Differentiate into macrophages, which phagocytize pathogens and debris.
Lymphocytes: Include B cells (produce antibodies) and T cells (cell-mediated immunity).
Clinical Relevance
Blood samples are used to diagnose diseases by counting and analyzing WBCs. Abnormal counts can indicate infections, immune disorders, or blood cancers.
Mononucleosis: Viral infection causing increased lymphocytes.
Leukemia: Cancer of blood-forming tissues, leading to abnormal WBC proliferation.
Hemostasis
Mechanism of Blood Clotting
Hemostasis is the process that stops blood loss after vessel injury. It involves three main steps:
Vasoconstriction: Narrowing of blood vessels to reduce blood flow, triggered by endothelins.
Platelet Plug Formation: Platelets adhere to the injury site and aggregate to form a temporary plug.
Blood Clotting (Coagulation): Fibrinogen is converted to fibrin, forming a stable clot.
The vascular spasm response typically lasts up to 30 minutes but can persist for hours.
Summary Table: Main Components of Blood
Component | Main Function | Key Features |
|---|---|---|
Plasma | Transport of nutrients, waste, hormones | 92% water, proteins (albumin, globulin, fibrinogen), electrolytes |
Red Blood Cells (Erythrocytes) | Oxygen and carbon dioxide transport | Biconcave, no nucleus, hemoglobin-rich |
White Blood Cells (Leukocytes) | Immune defense | Granular (neutrophils, eosinophils, basophils), agranular (monocytes, lymphocytes) |
Platelets | Blood clotting | Cell fragments, initiate clotting cascade |
