Back
BackBlood Vessels and Circulation: Structure, Function, and Clinical Relevance
Study Guide - Smart Notes

Blood Vessels and Circulation
Overview of the Circulatory System
The circulatory system is responsible for transporting blood, nutrients, gases, and waste products throughout the body. It consists of a vast network of blood vessels, including arteries, veins, and capillaries, which collectively span approximately 60,000 miles in the human body.
Arteries: Carry blood away from the heart under high pressure.
Veins: Return blood to the heart, often against gravity, and contain valves to prevent backflow.
Capillaries: Facilitate exchange of gases, nutrients, and waste between blood and tissues.

Structure of Blood Vessels
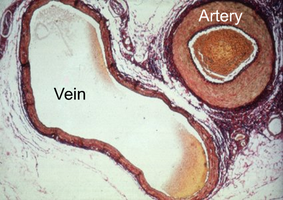
Blood vessels are composed of three distinct layers, known as tunics, each with specialized functions and structural features.
Tunica Intima (Interna): The innermost layer, consisting of endothelial cells lining the lumen; provides a smooth surface for blood flow.
Tunica Media: The middle layer, composed of smooth muscle and elastic fibers; responsible for vasoconstriction and vasodilation. This layer is thicker in arteries than in veins.
Tunica Externa (Adventitia): The outermost layer, made of connective tissue; provides structural support and protection. Thicker in veins than arteries.
Types of Arteries
Arteries are classified based on their structure and function:
Conducting (Elastic) Arteries: Large arteries like the aorta; rich in elastic fibers to maintain blood pressure.
Distributing (Muscular) Arteries: Medium-sized arteries; deliver blood to specific organs.
Resistance Arteries: Small arteries and arterioles; regulate blood flow and pressure.
Metarterioles: Connect arterioles to capillaries.
Types of Veins
Veins are capacitance vessels that store most of the blood volume at rest and rely on valves and skeletal muscle contraction for venous return.
Veins: Have thinner tunica media and thicker tunica externa; contain one-way valves.
Venules: Small veins connecting to capillaries; highly permeable.
Varicosity: Occurs when valves become stretched and incompetent, leading to varicose veins.
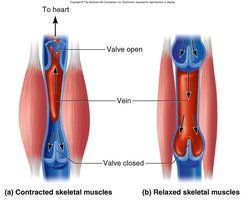
Skeletal Muscle Pump
The skeletal muscle pump aids venous return by compressing veins during muscle contraction, forcing blood toward the heart and preventing backflow via venous valves.
Capillaries and Capillary Beds
Types of Capillaries
Capillaries are the smallest blood vessels and are specialized for exchange. There are three main types:
Continuous Capillaries: Most common; tight junctions with intercellular clefts allow limited passage of fluids and small solutes. Found in skin, muscles, and the blood-brain barrier.
Fenestrated Capillaries: Have pores (fenestrations) that increase permeability; found in kidneys, small intestine, and endocrine glands.
Sinusoidal Capillaries: Large, leaky capillaries with incomplete basement membranes; allow passage of large molecules and cells. Found in liver, bone marrow, and lymphoid tissues.
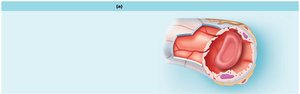

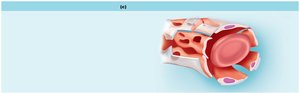
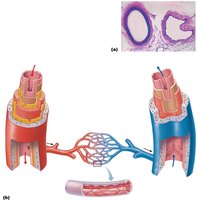
Capillary Beds and Microcirculation
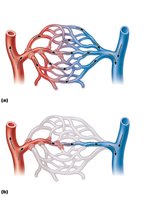
Capillary beds consist of networks of capillaries that regulate blood flow through tissues. Blood flow is controlled by precapillary sphincters, allowing for exchange or shunting of blood.
Vascular Shunt: Direct connection between arteriole and venule, bypassing true capillaries.
True Capillaries: Branch off the metarteriole and are the main sites of exchange.
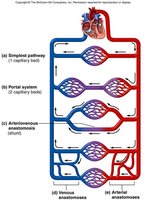
Circulatory Routes
Types of Circulatory Routes
Blood can travel through various routes in the body:
Simple Pathway: Artery → Capillary Bed → Vein
Portal System: Two capillary beds in series (e.g., hepatic portal system)
Anastomosis: Merging of blood vessels to provide alternate pathways for blood flow
Hepatic Portal Circulation
The hepatic portal system transports nutrient-rich blood from the digestive organs to the liver for processing and detoxification before returning to the systemic circulation.
Key vessels: Gastric veins, splenic vein, inferior/superior mesenteric veins, hepatic portal vein
Capillary Exchange and Fluid Movements
Forces Governing Capillary Exchange
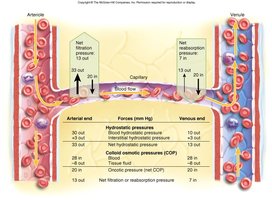
Fluid movement across capillary walls is determined by hydrostatic and osmotic pressures:
Capillary Hydrostatic Pressure (HPc): Pushes fluid out of capillaries; higher at arterial end.
Capillary Colloid Osmotic Pressure (OPc): Draws fluid into capillaries due to plasma proteins.
Net Filtration Pressure (NFP): The balance of these forces determines the direction of fluid movement.
Blood Flow and Pressure
Blood Flow: Laminar vs. Turbulent
Blood flow refers to the volume of blood moving through a vessel per unit time. It can be:
Laminar Flow: Smooth, orderly flow; faster in the center of the vessel.
Turbulent Flow: Disrupted flow, often audible; occurs in larger vessels or areas of constriction.
Resistance and Blood Pressure
Resistance is the opposition to blood flow, primarily due to vessel diameter, blood viscosity, and vessel length. Blood pressure is determined by cardiac output, blood volume, and resistance.
Normal blood pressure is approximately 120/75 mm Hg. Hypertension and hypotension are defined by deviations from this range.
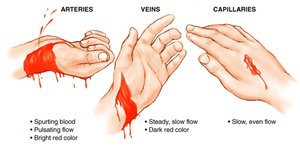
Medical Procedures Involving Blood Vessels
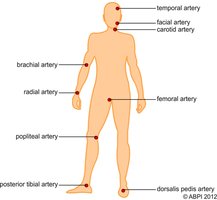
Pulse: Commonly measured at carotid or radial artery.
Bypass Surgery: Uses the great saphenous vein.
Venipuncture: Blood is often drawn from the median cubital vein.
Venous Return and Vein Diseases
Factors Aiding Venous Return
Venous return is facilitated by several mechanisms:
Pressure gradient
Gravity
Respiratory pump
Skeletal muscle pump
Cardiac suction
Venous valves
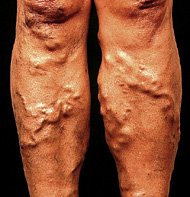
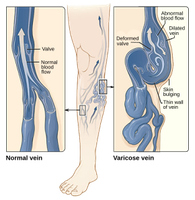
Varicose Veins
Varicose veins are dilated, twisted veins resulting from incompetent valves, often due to heredity or conditions that inhibit venous return.
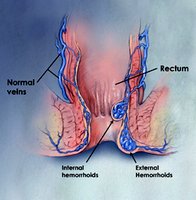
Hemorrhoids
Hemorrhoids are enlarged veins in the rectum and anus, caused by elevated venous pressure and impaired drainage.
Regulation of Blood Pressure
Short-Term Regulation
Blood pressure is regulated short-term by neural and hormonal mechanisms:
Baroreceptors: Detect stretch in arteries; inhibit SNS and stimulate PNS to lower BP.
Chemoreceptors: Respond to changes in O2, CO2, and H+; stimulate SNS to raise BP.
Hormones: Epinephrine, norepinephrine, renin, angiotensin, and ADH increase BP.
Long-Term Regulation
Long-term regulation is primarily hormonal and involves the kidneys:
ADH: Increases vasoconstriction and water reabsorption.
Renin-Angiotensin-Aldosterone System: Increases vasoconstriction and sodium/water retention.
ANP: Decreases BP by inhibiting renin, aldosterone, and ADH.
Circulatory Shock
Types of Shock
Cardiogenic Shock: Heart fails to maintain circulation.
Hypovolemic Shock: Caused by significant blood loss.
Vascular Shock: Due to extreme vasodilation.
Obstructed Venous Return Shock: Blockage impedes blood flow.
Fetal Circulation
Adaptations in Fetal Circulation
Fetal circulation bypasses the nonfunctional lungs via specialized vessels:
Ductus Arteriosus: Connects aorta and pulmonary trunk; becomes ligamentum arteriosum after birth.
Foramen Ovale: Connects right and left atria; becomes fossa ovalis after birth.
Umbilical Vein: Carries oxygen-rich blood to fetus.
Umbilical Arteries: Carry oxygen-poor blood to placenta.
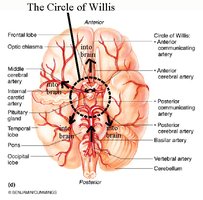
Cerebral Arterial Circulation
Circle of Willis
The Circle of Willis is an arterial anastomosis at the base of the brain, ensuring constant blood supply to cerebral tissues. It includes the anterior and posterior communicating arteries, anterior and posterior cerebral arteries, basilar artery, and middle cerebral artery.