 Back
BackBlood Vessels and Circulation: Structure, Function, and Regulation
Study Guide - Smart Notes

Blood Vessels and Circulation
Introduction to Blood Vessels
The blood vessels form a closed system of tubes that transport blood throughout the body. They are classified by size and histological organization and play a critical role in cardiovascular regulation. The largest vessels, the pulmonary trunk and aorta, are directly attached to the heart and serve as the main conduits for blood flow to the pulmonary and systemic circuits, respectively.
Types of Blood Vessels
Arteries, Arterioles, Capillaries, Venules, and Veins
Arteries: Carry blood away from the heart. They have thick, elastic walls to withstand high pressure.
Arterioles: Small branches of arteries that lead to capillary beds; regulate blood flow into capillaries.
Capillaries: The smallest blood vessels with thin walls, serving as the site of exchange between blood and interstitial fluid.
Venules: Smallest branches of veins that collect blood from capillaries.
Veins: Return blood to the heart; have thinner walls and lower pressure than arteries, and often contain valves to prevent backflow.
Blood Vessel Structure
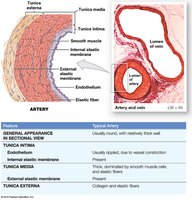
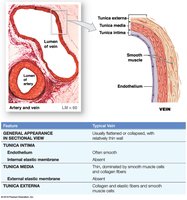
Layers of Blood Vessel Walls
Tunica intima (inner layer): Endothelial lining, connective tissue, and in arteries, an internal elastic membrane.
Tunica media (middle layer): Concentric sheets of smooth muscle in loose connective tissue; responsible for vasoconstriction and vasodilation. In arteries, separated from the externa by an external elastic membrane.
Tunica externa (outer layer): Collagen and elastic fibers; anchors vessel to adjacent tissues. In veins, may contain smooth muscle cells. Large vessels contain vasa vasorum (small vessels that supply the vessel wall).
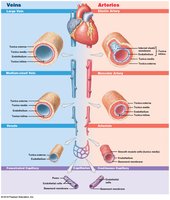
Differences Between Arteries and Veins
Arteries have thicker walls and higher blood pressure than veins.
Arteries have a small, round lumen; veins have a large, irregular lumen.
Arteries are more elastic; veins have valves to prevent backflow.
Types of Arteries
Elastic, Muscular Arteries, and Arterioles
Elastic arteries (conducting arteries): Large vessels (e.g., aorta, pulmonary trunk) with many elastic fibers; help even out pulse force.
Muscular arteries (distribution arteries): Medium-sized, with a thick tunica media rich in smooth muscle.
Arterioles (resistance vessels): Smallest arteries, with little or no tunica externa and thin or incomplete tunica media; regulate blood flow into capillary beds.
Vasoconstriction and Vasodilation
Vasoconstriction: Contraction of arterial smooth muscle, reducing lumen diameter.
Vasodilation: Relaxation of arterial smooth muscle, increasing lumen diameter.
These processes affect afterload on the heart, peripheral blood pressure, and capillary blood flow.
Aneurysm
An aneurysm is a bulge in an arterial wall caused by a weak spot in elastic fibers; may rupture under pressure, causing hemorrhage.
Capillaries
Structure and Function
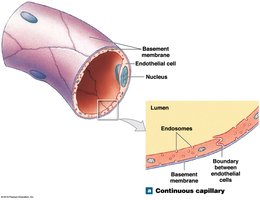
Capillaries are the smallest blood vessels, consisting of an endothelial tube inside a thin basement membrane. They lack tunica media and externa, and their diameter is similar to that of a red blood cell. Capillaries are the primary site for exchange of materials between blood and interstitial fluid.

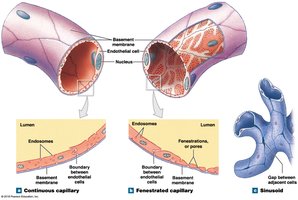
Types of Capillaries
Continuous capillaries: Complete endothelial lining; found in most tissues except epithelia and cartilage. Permit diffusion of water, small solutes, and lipid-soluble materials; block blood cells and plasma proteins. Specialized forms in CNS and thymus (e.g., blood-brain barrier).
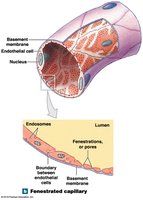
Fenestrated capillaries: Have pores in the endothelial lining; allow rapid exchange of water and larger solutes. Found in choroid plexus, endocrine organs, kidneys, and intestinal tract.
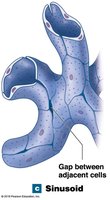
Sinusoids (sinusoidal capillaries): Have gaps between endothelial cells; permit free exchange of water and large plasma proteins. Found in liver, spleen, bone marrow, and endocrine organs.
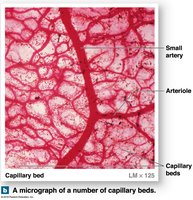
Capillary Beds and Anastomoses
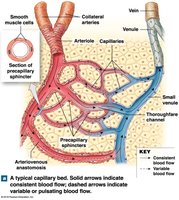
Capillary beds (plexuses): Networks connecting arterioles and venules; blood flow regulated by precapillary sphincters.
Thoroughfare channels: Direct connections between arterioles and venules, bypassing capillary beds.
Collaterals: Multiple arteries supplying one capillary bed; allow circulation if one artery is blocked.
Anastomoses: Fusion of two collateral arteries (arterial anastomosis) or direct connections between arterioles and venules (arteriovenous anastomoses).
Angiogenesis
Formation of new blood vessels, stimulated by vascular endothelial growth factor (VEGF).
Occurs during embryonic development and in response to hypoxia (oxygen starvation).
Veins
Structure and Function
Veins collect blood from capillaries and return it to the heart.
Compared to arteries, veins have larger diameters, thinner walls, and lower blood pressure.
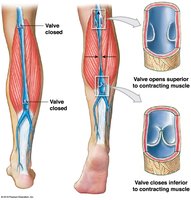
Venous valves (folds of tunica intima) prevent backflow of blood; compression of veins by skeletal muscles aids venous return.
Weakening of vein walls near valves can result in varicose veins or hemorrhoids.
Distribution of Blood
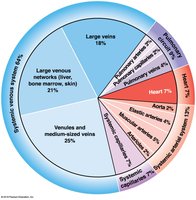
Blood Volume in Circulatory System
Heart, arteries, and capillaries contain 30–35% of blood volume.
Venous system contains 65–70% of blood volume; one-third is in large venous networks of the liver, bone marrow, and skin.
Veins act as blood reservoirs due to their high capacitance (ability to stretch).
Hemodynamics: Pressure and Resistance
Blood Flow, Pressure, and Resistance
Total capillary blood flow equals cardiac output and is determined by pressure (P) and resistance (R).
Pressure gradient (ΔP): Difference in pressure from one end of a vessel to the other; flow (F) is proportional to ΔP/R.
Blood pressure (BP): Arterial pressure measured in mm Hg.
Capillary hydrostatic pressure (CHP): Pressure within capillary beds.
Venous pressure: Pressure in the venous system.
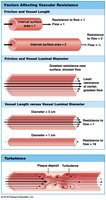
Factors Affecting Resistance
Vascular resistance: Due to friction between blood and vessel walls; increases exponentially as vessel diameter decreases.
Blood viscosity: Whole blood is about four times as viscous as water.
Turbulence: Swirling action that disturbs smooth flow, often caused by plaques or vessel branching.
Cardiovascular Pressures and Blood Flow
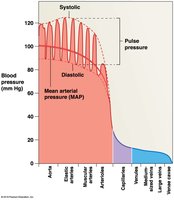
Vessel luminal diameter, total cross-sectional area, pressure, and velocity of blood flow vary throughout the systemic circuit.
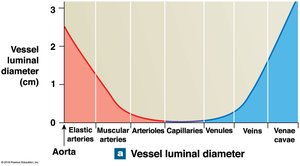
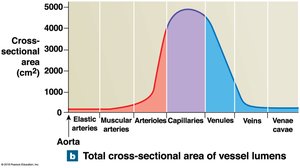
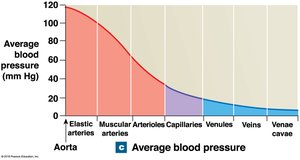
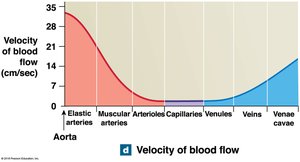
Arterial Blood Pressure
Systolic pressure: Peak arterial pressure during ventricular systole.
Diastolic pressure: Minimum arterial pressure at end of ventricular diastole.
Pulse pressure: Difference between systolic and diastolic pressure.
Mean arterial pressure (MAP):
Normal BP: 120/80 mm Hg; hypertension: >140/90 mm Hg; hypotension: abnormally low BP.
Venous Return
Venous pressure is low; return of blood to the heart is assisted by skeletal muscle contraction and the respiratory pump.
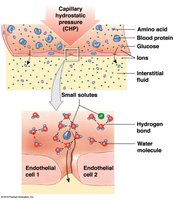
Capillary Exchange
Mechanisms of Exchange
Diffusion: Movement of substances from high to low concentration.
Filtration: Driven by hydrostatic pressure; water and small solutes forced through capillary wall.
Reabsorption: Driven by osmotic pressure; water moves into capillaries due to higher solute concentration (blood colloid osmotic pressure, BCOP).
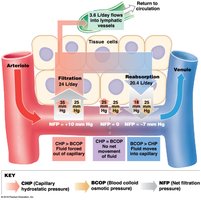
Net Filtration Pressure (NFP)
Determined by the balance between hydrostatic and osmotic pressures:
At the arterial end, filtration predominates; at the venous end, reabsorption predominates. Excess fluid enters lymphatic vessels.
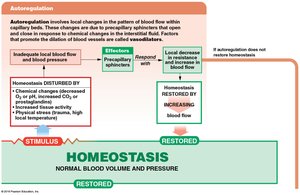
Regulation of Blood Flow and Pressure
Control Mechanisms
Autoregulation: Immediate, localized adjustments via precapillary sphincters in response to local chemical changes.
Neural mechanisms: Rapid responses via the cardiovascular center in the medulla oblongata (cardiac and vasomotor centers).
Endocrine mechanisms: Hormonal regulation for long-term adjustments (e.g., ADH, angiotensin II, EPO, natriuretic peptides).
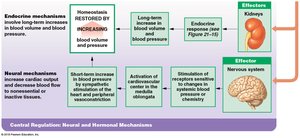
Baroreceptor and Chemoreceptor Reflexes
Baroreceptors: Detect changes in blood pressure in carotid sinuses, aortic sinuses, and right atrium; trigger reflexes to maintain homeostasis.
Chemoreceptors: Monitor pH, O2, and CO2 levels; coordinate cardiovascular and respiratory responses.
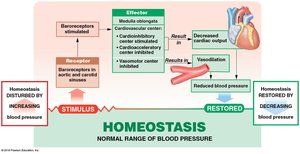
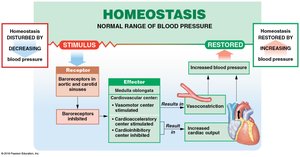
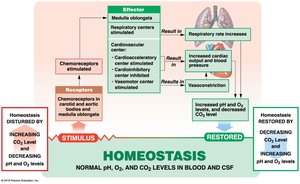
Hormonal Regulation
ADH: Increases blood pressure by reducing water loss at kidneys.
Angiotensin II: Stimulates vasoconstriction, aldosterone, and ADH release.
EPO: Stimulates red blood cell production and vasoconstriction.
Natriuretic peptides (ANP, BNP): Reduce blood volume and pressure by promoting sodium and water loss.
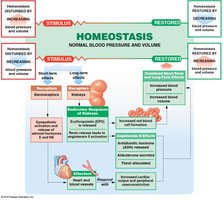
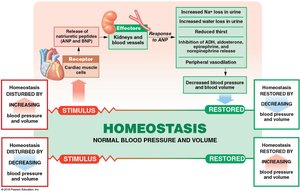
Cardiovascular Adaptation
Special Circulations
Brain: Maintains constant blood flow; cerebral vessels dilate if peripheral vessels constrict.
Heart: Coronary arteries supply blood; increased demand leads to vasodilation and increased flow.
Lungs: Blood flow regulated by O2 levels in alveoli; high O2 causes vasodilation, low O2 causes vasoconstriction.
Response to Exercise
Light exercise: Vasodilation, increased venous return, and cardiac output.
Heavy exercise: Sympathetic activation, maximal cardiac output, blood flow redirected to muscles, lungs, and heart.
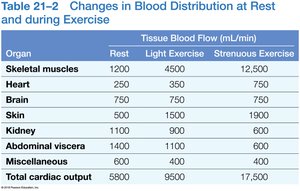
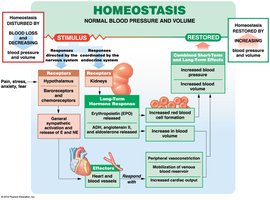
Response to Hemorrhaging
Short-term: Baroreceptor and sympathetic responses increase cardiac output and vasoconstriction.
Long-term: Hormonal responses (aldosterone, ADH, EPO) restore blood volume.
Failure to compensate leads to shock.
Major Arteries and Veins
Examples of Major Vessels
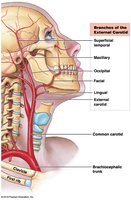
Carotid arteries: Supply the head and neck; contain baroreceptors in the carotid sinus.
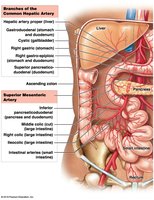
Arteries of the abdominopelvic organs: Supply digestive organs and liver.
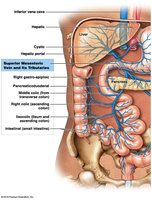
The Hepatic Portal System
Structure and Function
Connects two capillary beds; delivers nutrient-rich blood from digestive organs to the liver for processing.
After processing, blood returns to the systemic circulation via the hepatic veins and inferior vena cava.
Summary Table: Types of Blood Vessels
Vessel Type | Main Function | Key Structural Features |
|---|---|---|
Artery | Carry blood away from heart | Thick tunica media, elastic fibers, high pressure |
Arteriole | Regulate blood flow into capillaries | Thin walls, little/no tunica externa |
Capillary | Exchange of materials | Single endothelial layer, thin basement membrane |
Venule | Collect blood from capillaries | Thin walls, small diameter |
Vein | Return blood to heart | Thin tunica media, valves, low pressure |
Key Equations
Flow (F):
Mean Arterial Pressure (MAP):
Net Filtration Pressure (NFP):
Learning Outcomes
Distinguish among the types of blood vessels based on their structure and function.
Describe the factors that influence blood pressure, and explain how and where fluid and dissolved materials enter and leave the cardiovascular system.
Describe the control mechanisms that regulate blood flow and pressure in tissues, and explain how the activities of the cardiac, vasomotor, and respiratory centers are coordinated to control blood flow through the tissues.
Identify the principal blood vessels and functions of the special circulation to the brain, heart, and lungs, and explain the cardiovascular system’s homeostatic response to exercise and hemorrhaging.
Describe the pulmonary and systemic circuits of the cardiovascular system.
Identify the major arteries and veins of the pulmonary and systemic circuits.
