 Back
BackBlood Vessels and Circulation: Structure, Function, and Regulation
Study Guide - Smart Notes

Blood Vessels and Circulation
Introduction to Blood Vessels
Blood vessels are essential components of the cardiovascular system, classified by size and histological organization. They regulate blood flow and pressure throughout the body, connecting the heart to all tissues.
Pulmonary trunk: Carries blood from the right ventricle to the pulmonary circulation.
Aorta: Carries blood from the left ventricle to systemic circulation.
Types of Blood Vessels
Arteries, Arterioles, Capillaries, Venules, and Veins
Blood vessels are categorized based on their structure and function.
Arteries: Carry blood away from the heart; thick-walled and elastic.
Arterioles: Small branches of arteries leading to capillary beds; regulate blood flow.
Capillaries: Smallest vessels; site of exchange between blood and interstitial fluid.
Venules: Small branches of veins collecting blood from capillaries.
Veins: Return blood to the heart; thinner walls, lower pressure, and contain valves.
Structural Layers of Blood Vessels
Blood vessels have three main layers:
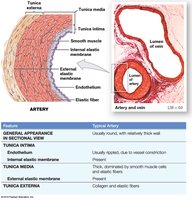
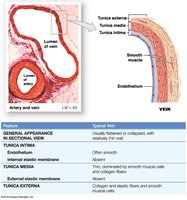
Tunica intima: Inner layer; endothelial lining and connective tissue. Arteries have an internal elastic membrane.
Tunica media: Middle layer; concentric sheets of smooth muscle and elastic fibers. Responsible for vasoconstriction and vasodilation.
Tunica externa: Outer layer; anchors vessel, contains collagen and elastic fibers, and vasa vasorum in large vessels.
Differences Between Arteries and Veins
Arteries: Thicker walls, higher pressure, small round lumen, more elastic, folded endothelium when constricted.
Veins: Thinner walls, lower pressure, large irregular lumen, contain valves to prevent backflow.
Types of Arteries
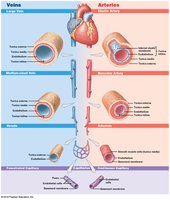
Elastic arteries: Large vessels (e.g., aorta); tunica media rich in elastic fibers, evens out pulse force.
Muscular arteries: Medium-sized; tunica media with many muscle cells.
Arterioles: Smallest arteries; little or no tunica externa, thin or incomplete tunica media.
Aneurysm
Aneurysm: Bulge in arterial wall due to weak spot in elastic fibers; may rupture under pressure.
Capillaries: Structure and Function
Capillary Types
Capillaries are the site of exchange between blood and tissues.
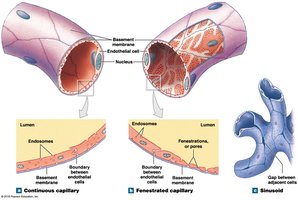
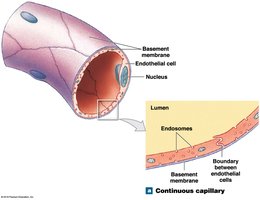
Continuous capillaries: Complete endothelial lining; found in most tissues except epithelia and cartilage. Restricts permeability in CNS and thymus (blood-brain barrier).
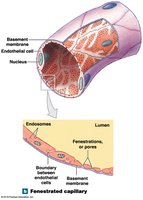
Fenestrated capillaries: Have pores; permit rapid exchange of water and larger solutes. Found in choroid plexus, endocrine organs, kidneys, and intestines.
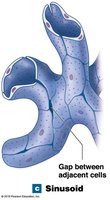
Sinusoids: Gaps between endothelial cells; allow free exchange of water and large plasma proteins. Found in liver, spleen, bone marrow, and endocrine organs.

Capillary Beds and Blood Flow Regulation
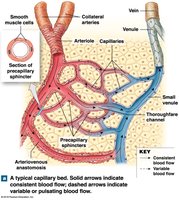
Capillary beds: Networks connecting arterioles and venules.
Precapillary sphincters: Guard capillary entrances; regulate blood flow in pulses.
Thoroughfare channels: Direct connections between arterioles and venules.
Collaterals: Multiple arteries supplying one capillary bed; allow circulation if one artery is blocked.
Anastomoses: Fusion of collateral arteries or direct arteriole-venule connections.
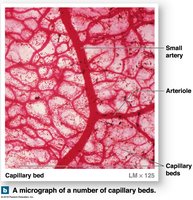
Angiogenesis
Angiogenesis: Formation of new blood vessels, stimulated by VEGF; occurs during development and in response to hypoxia.
Veins: Structure and Function
Types of Veins
Venules: Small veins collecting blood from capillaries.
Medium-sized veins: Thin tunica media, few muscle cells, tunica externa with elastic fibers.
Large veins: All three tunica layers; thick tunica externa, thin tunica media.
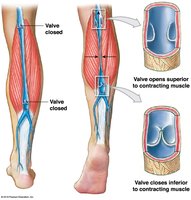
Venous valves: Folds of tunica intima; prevent backflow, aid venous return.
Distribution of Blood and Capacitance
Blood Volume Distribution
Heart, arteries, and capillaries: 30–35% of blood volume.
Venous system: 65–70% of blood volume; large networks in liver, bone marrow, skin.
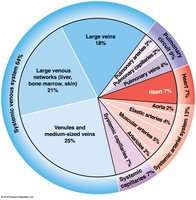
Capacitance
Capacitance: Ability of a vessel to stretch; veins stretch more than arteries and act as blood reservoirs.
Venoconstriction: Veins constrict in response to blood loss, increasing blood in arterial system and capillaries.
Pressure and Resistance in the Cardiovascular System
Factors Influencing Blood Pressure
Pressure (P): Generated by the heart; flow is proportional to pressure gradient (∆P) divided by resistance (R).
Resistance: Affected by vascular resistance (friction), blood viscosity, and turbulence.
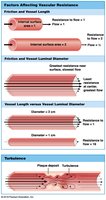
Cardiovascular Pressures and Blood Flow
Vessel luminal diameter, cross-sectional area, pressure, and velocity of blood flow vary across the systemic circuit.
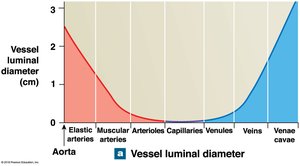
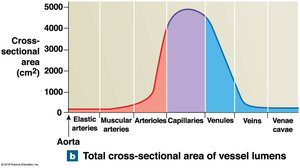
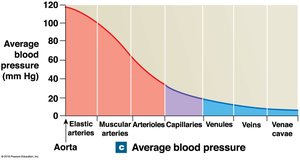
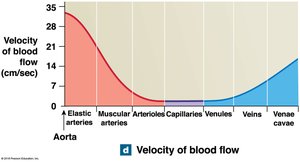
Arterial Blood Pressure
Systolic pressure: Peak during ventricular systole.
Diastolic pressure: Minimum at end of ventricular diastole.
Pulse pressure: Difference between systolic and diastolic.
Mean arterial pressure (MAP):
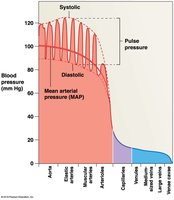
Venous Pressure and Return
Venous pressure is low; return assisted by skeletal muscle compression and respiratory pump.
Capillary Exchange: Diffusion, Filtration, and Reabsorption
Mechanisms of Exchange
Diffusion: Movement from high to low concentration; routes depend on molecule size and solubility.
Filtration: Driven by hydrostatic pressure; water and small solutes forced through capillary wall.
Reabsorption: Driven by osmotic pressure; blood colloid osmotic pressure (BCOP) pulls water into capillaries.
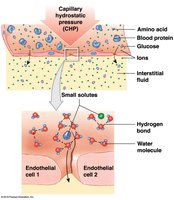
Interplay of Filtration and Reabsorption
Net filtration pressure (NFP) determines direction of fluid movement:
At arterial end: filtration dominates; at venous end: reabsorption dominates.
Excess fluid enters lymphatic vessels.
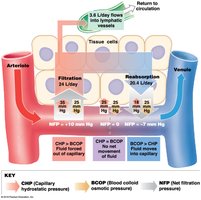
Regulation of Blood Flow and Pressure
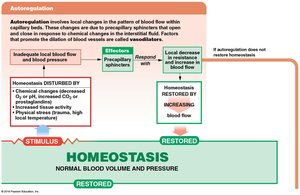
Control Mechanisms
Autoregulation: Immediate, localized adjustments via precapillary sphincters.
Neural mechanisms: Cardiovascular center in medulla oblongata; baroreceptor and chemoreceptor reflexes.
Endocrine mechanisms: Hormones (E, NE, ADH, angiotensin II, EPO, ANP, BNP) regulate blood pressure and volume.
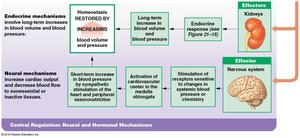
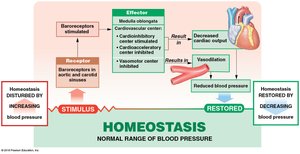
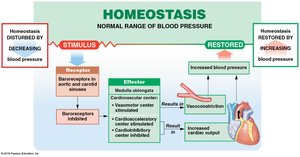
Baroreceptor and Chemoreceptor Reflexes
Baroreceptors: Monitor blood pressure in carotid sinuses, aortic sinuses, and right atrium.
Chemoreceptors: Monitor pH, O2, and CO2 in blood; coordinate cardiovascular and respiratory activities.
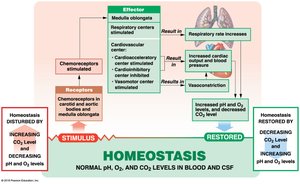
Hormonal Regulation
ADH: Elevates blood pressure, reduces water loss.
Angiotensin II: Stimulates aldosterone, ADH, thirst, cardiac output, and vasoconstriction.
EPO: Stimulates vasoconstriction and RBC production.
Natriuretic peptides (ANP, BNP): Reduce blood volume and pressure.
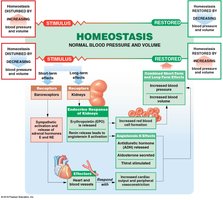
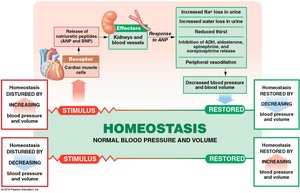
Cardiovascular Adaptation
Special Circulation
Brain: High priority; cerebral vessels dilate when peripheral vessels constrict.
Heart: Coronary arteries supply blood; demand increases with activity.
Lungs: Perfusion regulated by O2 levels in alveoli.
Response to Exercise
Light exercise: Vasodilation, increased venous return, increased cardiac output.
Heavy exercise: Sympathetic activation, maximum cardiac output, blood redirected to muscles, lungs, heart.
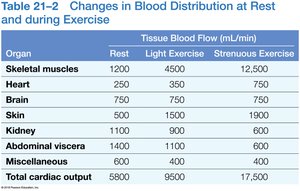
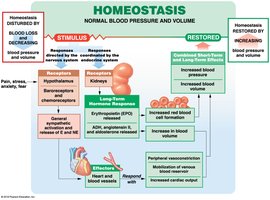
Response to Hemorrhaging
Short-term: Reflexes increase cardiac output and vasoconstriction.
Long-term: Fluid recall, hormone release, increased RBC production.
Shock: Failure to restore blood pressure after significant blood loss.
Major Arteries and Veins
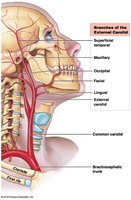
Arteries of the Neck and Head
Carotid sinus: Contains baroreceptors; important for blood pressure regulation.
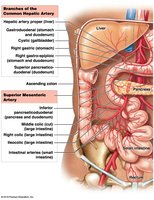
Arteries Supplying Abdominopelvic Organs
Arterial blood supply to the liver is crucial for nutrient processing.
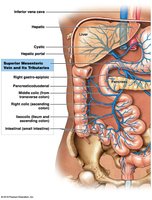
The Hepatic Portal System
Connects capillary beds of digestive organs to the liver for processing.
Blood collects in hepatic veins and empties into the inferior vena cava.
Summary of Learning Outcomes
Distinguish among types of blood vessels based on structure and function.
Describe factors influencing blood pressure and capillary exchange.
Explain control mechanisms regulating blood flow and pressure.
Identify principal vessels and special circulations.
Describe pulmonary and systemic circuits.
Identify major arteries and veins.
Discuss differences between fetal and adult circulation.
Explain effects of aging and interactions with other organ systems.
