 Back
BackBlood Vessels and Circulation: Structure, Function, and Regulation
Study Guide - Smart Notes

The Cardiovascular System: Blood Vessels and Circulation
Overview of Blood Vessel Types
The cardiovascular system consists of a network of blood vessels that transport blood throughout the body. These vessels are classified based on their structure and function.
Arteries: Carry blood away from the heart to organs and tissues.
Arterioles: Small branches of arteries leading to capillaries.
Capillaries: Microscopic vessels where exchange of gases, nutrients, and wastes occurs.
Venules: Small vessels that collect blood from capillaries.
Veins: Return blood to the heart.
Example: The aorta is the largest artery, while the venae cavae are the largest veins.
Structure of Vessel Walls
Blood vessel walls are composed of three layers, each with distinct functions:
Tunica intima: Innermost layer, lined by endothelium and a basement membrane.
Tunica media: Middle layer, primarily smooth muscle and elastic fibers; regulates vessel diameter.
Tunica externa (adventitia): Outermost layer, connective tissue that stabilizes and anchors the vessel.
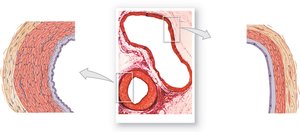
Differences Between Arteries and Veins
Arteries and veins differ in structure and function:
Arteries have thicker walls, smaller lumens, and more elastic fibers to withstand higher pressure.
Veins have thinner walls, larger lumens, and often contain valves to prevent backflow due to lower pressure.
Key Point: Smooth muscle in arteries allows for vasoconstriction (narrowing) and vasodilation (widening) to regulate blood flow and pressure.
Types of Arteries
Elastic arteries: Largest arteries (e.g., aorta), rich in elastic fibers, absorb pressure changes during heartbeats.
Muscular arteries: Medium-sized, more smooth muscle, distribute blood to organs and muscles.
Arterioles: Smallest arteries, control blood flow into capillary beds by changing diameter.
Capillaries and Capillary Beds
Capillaries are the only vessels where exchange occurs between blood and interstitial fluid. They form interconnected networks called capillary beds, regulated by precapillary sphincters.
Thin walls (endothelium and basement membrane) allow for efficient diffusion.
Vasomotion: Rhythmic opening and closing of precapillary sphincters controls blood flow through capillary beds (autoregulation).
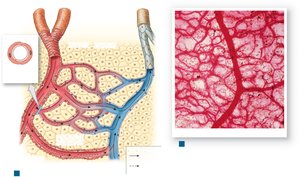
Alternate Routes for Blood Flow
Anastomosis: Joining of blood vessels to provide alternate routes for blood flow.
Arteriovenous anastomosis: Direct connection between arteriole and venule, bypassing capillary bed.
Arterial anastomosis: Fusion of arteries before branching into arterioles, ensuring blood supply to vital organs.
Veins and Venous Return
Veins return blood to the heart and are classified by size:
Venules: Smallest veins, collect blood from capillaries.
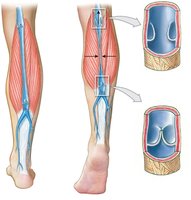
Medium-sized veins: Contain valves to prevent backflow, especially in limbs.
Large veins: Include the superior and inferior venae cavae.
Example: Varicose veins result from malfunctioning venous valves.
Summary Table: Structure of Blood Vessels
Vessel Type | Wall Structure | Function |
|---|---|---|
Elastic Artery | Thick tunica media, many elastic fibers | Absorb pressure changes |
Muscular Artery | Thick tunica media, more smooth muscle | Distribute blood to organs |
Arteriole | Thin wall, 1-2 layers smooth muscle | Control blood flow to capillaries |
Capillary | Endothelium only | Exchange of substances |
Venule | Thin wall, little/no smooth muscle | Collect blood from capillaries |
Vein | Thin wall, valves present | Return blood to heart |
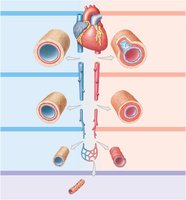
Hemodynamics: Blood Flow, Pressure, and Resistance
Blood Flow and Cardiac Output
Blood flow is the volume of blood moving through a vessel, tissue, or organ per unit time. It is directly related to cardiac output (CO).
Increased CO increases blood flow through capillaries.
Blood flow is also influenced by pressure gradients and resistance.
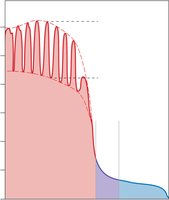
Blood Pressure and Its Regulation
Blood pressure is the force exerted by blood against vessel walls. It is highest in the aorta and lowest in the venae cavae.
Systolic pressure: Peak pressure during ventricular contraction.
Diastolic pressure: Minimum pressure during ventricular relaxation.
Pulse pressure: Difference between systolic and diastolic pressures.
Peripheral Resistance
Resistance opposes blood flow and is determined by:
Vascular resistance: Friction between blood and vessel walls; depends on vessel length and diameter.
Viscosity: Thickness of blood; higher viscosity increases resistance.
Turbulence: Irregular flow increases resistance, often at branch points or due to disease.
Equation: (Poiseuille's Law; = viscosity, = length, = radius)
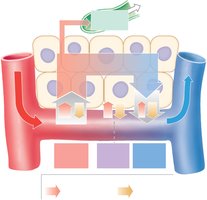
Capillary Exchange and Dynamics
Capillary exchange maintains homeostasis by allowing movement of substances between blood and interstitial fluid via:
Diffusion: Movement from high to low concentration.
Filtration: Driven by hydrostatic pressure, forces water and solutes out of capillaries.
Reabsorption: Driven by osmotic pressure, draws water back into capillaries.
Regulation of Blood Flow and Pressure
Autoregulation
Local adjustments in blood flow are made by precapillary sphincters in response to tissue needs.
Vasodilators: Promote increased blood flow (e.g., low O2, high CO2, nitric oxide).
Vasoconstrictors: Decrease blood flow (e.g., endothelin, sympathetic stimulation).
Neural Regulation
The cardiovascular center in the medulla oblongata regulates cardiac output and vessel diameter via:
Cardioacceleratory center: Increases heart rate and contractility (sympathetic).
Cardioinhibitory center: Decreases heart rate (parasympathetic).
Vasomotor center: Controls arteriolar constriction and peripheral resistance.
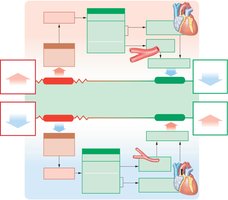
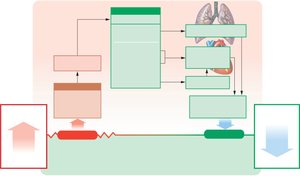
Reflex Control: Baroreceptors and Chemoreceptors
Reflexes adjust blood pressure and flow based on sensory input:
Baroreceptor reflexes: Respond to changes in blood pressure (carotid sinuses, aortic arch, right atrium).
Chemoreceptor reflexes: Respond to changes in blood chemistry (CO2, O2, pH).
Hormonal Regulation
Several hormones influence blood pressure and volume:
Epinephrine and norepinephrine: Increase cardiac output and vasoconstriction (short-term).
Antidiuretic hormone (ADH): Promotes water retention and vasoconstriction (long-term).
Angiotensin II: Increases blood pressure via vasoconstriction and stimulating aldosterone and ADH release.
Erythropoietin (EPO): Stimulates red blood cell production, increasing blood volume.
Atrial natriuretic peptide (ANP): Lowers blood pressure by increasing sodium and water excretion.
Cardiovascular Responses and Circuits
Responses to Exercise and Hemorrhage
Exercise: Increases cardiac output, vasodilation in muscles, and shunting of blood from nonessential organs.
Hemorrhage: Short-term responses include increased heart rate and vasoconstriction; long-term responses involve fluid retention and increased RBC production.
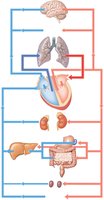
Pulmonary and Systemic Circuits
The cardiovascular system is divided into two main circuits:
Pulmonary circuit: Right ventricle → pulmonary arteries → lungs (gas exchange) → pulmonary veins → left atrium.
Systemic circuit: Left ventricle → aorta → body tissues → venae cavae → right atrium.
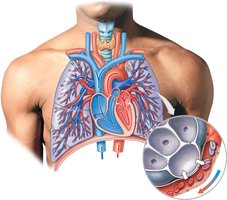
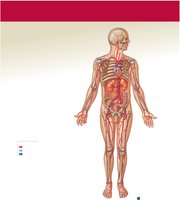
Major Systemic Arteries and Veins
Systemic arteries originate from the aorta and branch to supply all body regions. Major veins return blood to the heart via the superior and inferior venae cavae.
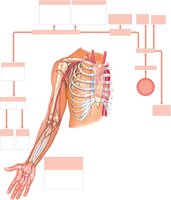
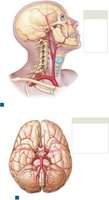
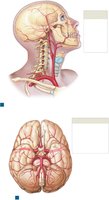
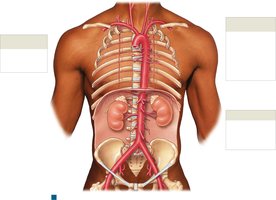
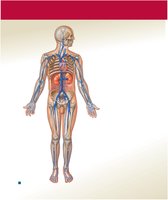
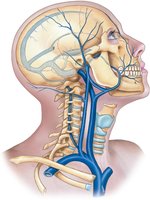
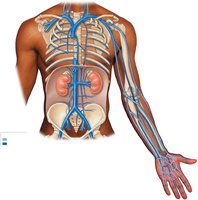
Summary Table: Major Arteries and Veins
Artery | Supplies |
|---|---|
Aorta | All systemic circulation |
Common carotid | Head and neck |
Subclavian | Upper limbs |
Renal | Kidneys |
Femoral | Lower limbs |
Vein | Drains |
|---|---|
Superior vena cava | Head, neck, upper limbs, chest |
Inferior vena cava | Lower body, abdomen, pelvis, lower limbs |
Jugular veins | Head and neck |
Renal veins | Kidneys |
Femoral veins | Lower limbs |
Key Concepts and Applications
Blood vessels are specialized for transport, exchange, and regulation of blood flow and pressure.
Homeostatic mechanisms ensure adequate perfusion of tissues under varying physiological conditions.
Understanding vessel structure and function is essential for interpreting cardiovascular health and disease.
