 Back
BackBlood Vessels and Circulatory Physiology: Structure, Function, and Regulation
Study Guide - Smart Notes

Blood Vessel Structure and Function
Overview of Arteries, Veins, and Capillaries
Blood vessels are essential components of the circulatory system, responsible for transporting blood throughout the body. They are classified into arteries, veins, and capillaries, each with distinct structural and functional characteristics.
Arteries: Efferent vessels carrying blood away from the heart.
Veins: Afferent vessels carrying blood toward the heart.
Capillaries: Microscopic, thin-walled vessels connecting the smallest arteries to the smallest veins, facilitating exchange of gases, nutrients, and wastes.
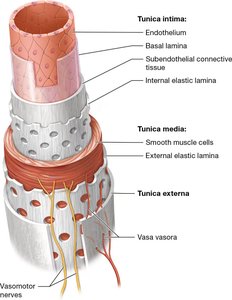
Blood Vessel Wall Layers (Tunics)
The walls of blood vessels are composed of three main layers, known as tunics:
Tunica intima: The innermost layer, consisting of endothelium, basal lamina, and subendothelial connective tissue.
Tunica media: The middle layer, primarily composed of smooth muscle cells and elastic fibers, responsible for vasoconstriction and vasodilation.
Tunica externa (adventitia): The outermost layer, made of connective tissue and containing vasa vasora (small vessels that supply the vessel wall).
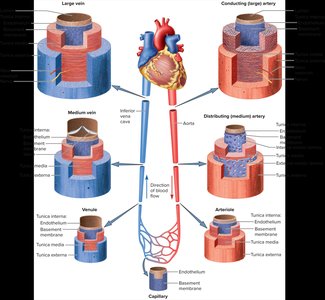
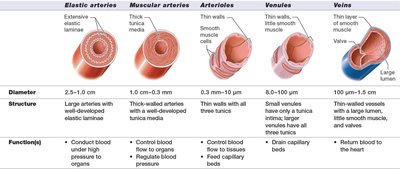
Types of Arteries and Veins
Arteries and veins are further classified based on their size, structure, and function:
Type | Diameter | Structure | Function(s) |
|---|---|---|---|
Elastic arteries | 2.5–1.0 cm | Large arteries with extensive elastic laminae | Conduct blood under high pressure |
Muscular arteries | 1.0 cm–0.3 mm | Thick-walled arteries with well-developed tunica media | Control blood flow to organs, regulate blood pressure |
Arterioles | 0.3 mm–10 μm | Thin walls with smooth muscle | Control blood flow to tissues, feed capillary beds |
Venules | 8.0–100 μm | Small veins, thin walls | Drain capillary beds |
Veins | 100 μm–1.5 cm | Thin-walled vessels with smooth muscle and valves | Return blood to the heart |
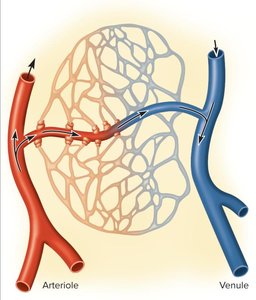
Capillary Beds and Microcirculation
Structure and Function of Capillary Beds
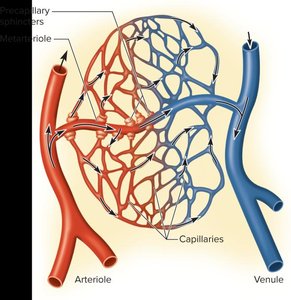
Capillary beds are networks of capillaries supplied by a single arteriole. They facilitate exchange between blood and tissues.
Typically consist of 10–100 capillaries per bed.
Precapillary sphincters regulate blood flow into capillaries, opening or closing in response to tissue needs.
Types of Capillaries
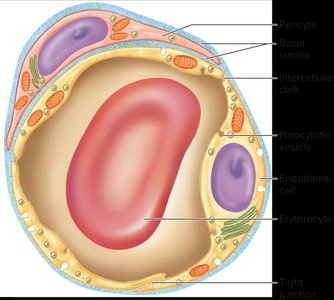
Capillaries are classified based on their permeability:
Continuous capillaries: Have tight junctions and limited permeability.
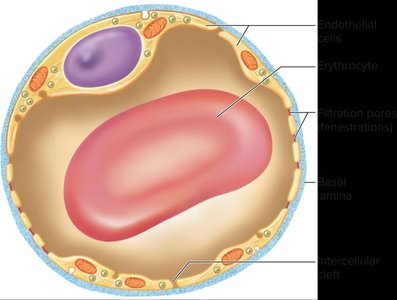
Fenestrated capillaries: Possess pores (fenestrations) for increased permeability, found in organs requiring rapid exchange (e.g., kidneys, intestines).
Veins and Venous Return
Characteristics of Veins
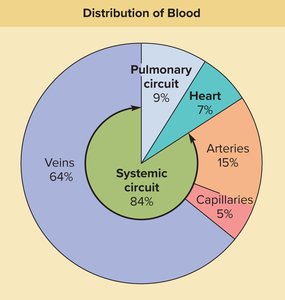
Veins are capacitance vessels, meaning they have a greater capacity for blood containment than arteries. They are thin-walled, flaccid, and collapse when empty. Blood flow in veins is steady and non-pulsatile, and veins are subjected to relatively low blood pressure.
Mechanisms of Venous Return
Venous return is assisted by several mechanisms:
Pressure gradient: Blood moves from higher to lower pressure.
Gravity: Assists drainage from head and neck.
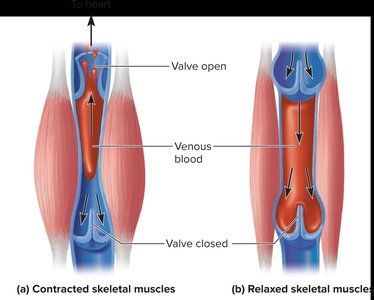
Skeletal muscle pump: Muscle contractions compress veins, pushing blood toward the heart.
Thoracic (respiratory) pump: Pressure changes during breathing facilitate venous return.
Cardiac suction: Slight pull during ventricular systole draws blood into the atria.
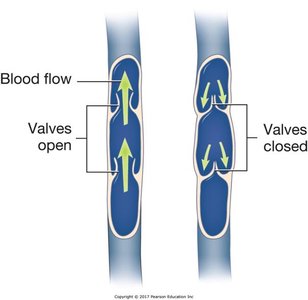
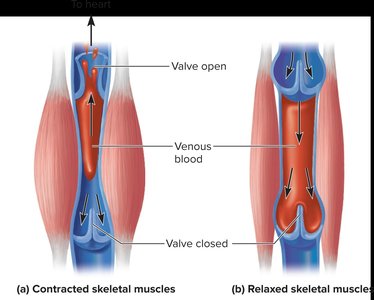
Venous Valves
Veins contain valves that prevent backflow of blood, ensuring unidirectional flow toward the heart.
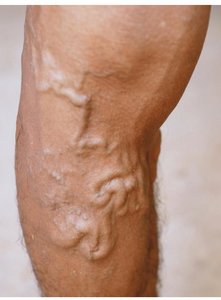
Varicose Veins
Varicose veins occur when blood pools in the lower legs, stretching the veins and causing valve cusps to pull apart. This leads to backflow, vessel distension, and irregular dilations. Risk factors include hereditary weakness, obesity, pregnancy, and prolonged standing.
Physiology of Blood Flow and Blood Pressure
Blood Pressure Measurement
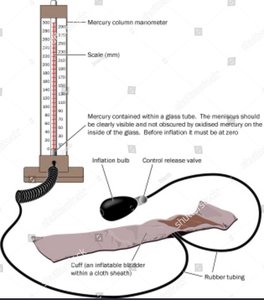
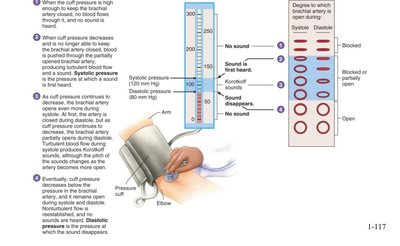
Blood pressure is the force exerted by blood against arterial walls. It is measured using a sphygmomanometer, which detects Korotkoff sounds as pressure is released from the cuff.
Blood Pressure Variance in Circuits
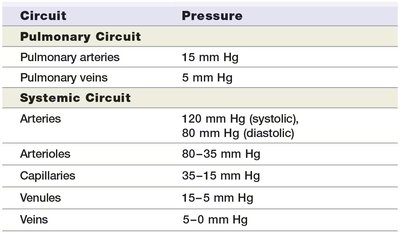
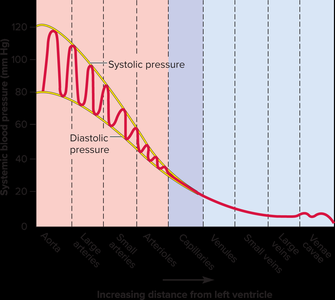
Blood pressure varies throughout the circulatory system:
Circuit | Pressure |
|---|---|
Pulmonary arteries | 15 mm Hg |
Pulmonary veins | 5 mm Hg |
Systemic arteries | 120 mm Hg (systolic), 80 mm Hg (diastolic) |
Arterioles | 80–35 mm Hg |
Capillaries | 35–15 mm Hg |
Venules | 15–5 mm Hg |
Veins | 5–0 mm Hg |
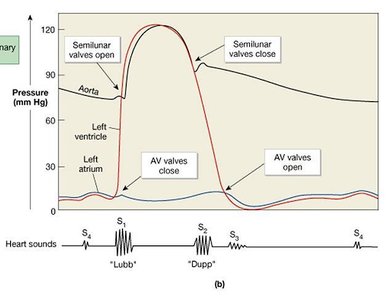
Mean Arterial Pressure (MAP)
MAP is the average blood pressure in the arteries, crucial for organ perfusion. It is calculated as:
Normal MAP: 70–100 mm Hg; minimum 60 mm Hg required for organ perfusion.
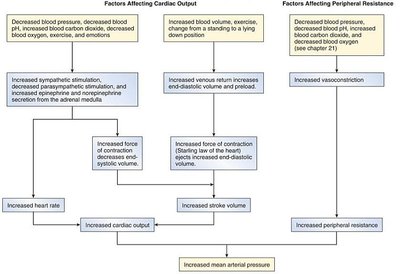
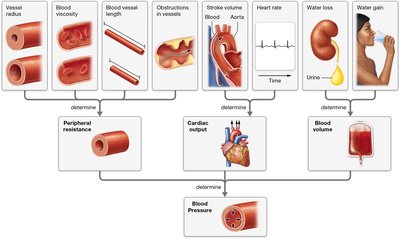
Factors Affecting Blood Pressure
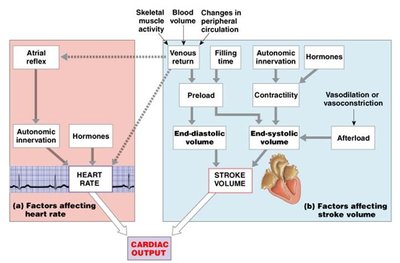
Blood pressure is determined by cardiac output, blood volume, and peripheral resistance:
Cardiac output (CO): Amount of blood pumped by the heart per minute ().
Blood volume: Total volume of blood in the circulatory system.
Peripheral resistance: Resistance to blood flow, primarily regulated by vessel diameter.
Peripheral Resistance and Flow Dynamics
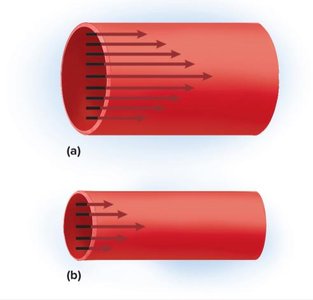
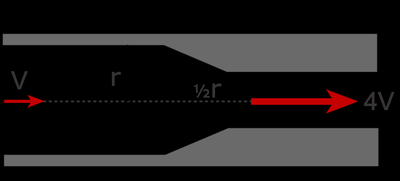
Resistance to flow is influenced by blood viscosity, vessel length, and vessel radius. Flow is directly proportional to pressure difference and inversely proportional to resistance:
Resistance is calculated as , where v is viscosity, l is length, and D is diameter.
Regulation of Blood Pressure
Local, Neural, and Hormonal Control
Blood pressure is regulated by local, neural, and hormonal mechanisms:
Local control: Autoregulation, vasoactive chemicals, reactive hyperemia, and angiogenesis.
Neural control: Baroreflex, chemoreflex, and medullary ischemic reflex via the vasomotor center.
Hormonal control: Angiotensin II, aldosterone, natriuretic peptides, antidiuretic hormone (ADH), epinephrine, and norepinephrine.
Capillary Exchange and Tissue Perfusion
Mechanisms of Capillary Exchange
Capillary exchange involves diffusion, filtration, and osmosis:
Diffusion: Movement of gases and solutes across the capillary wall.
Filtration: Driven by hydrostatic pressure, moving fluid out of capillaries.
Osmosis: Driven by colloid osmotic pressure, moving fluid into capillaries.


Edema and Capillary Exchange
Edema occurs when excess fluid accumulates in tissues due to increased capillary filtration, reduced reabsorption, or obstructed lymphatic drainage. Causes include inflammation, decreased plasma proteins, and venous blockage.
Anatomy of Systemic Arteries and Veins
Major Arteries and Veins
The systemic circuit includes major arteries and veins supplying and draining the head, neck, thoracic cavity, abdominopelvic cavity, and limbs. The hepatic portal system is a specialized venous system that directs blood from the gastrointestinal tract to the liver for processing.
Summary Table: Blood Vessel Types
Type | Diameter | Structure | Function(s) |
|---|---|---|---|
Elastic arteries | 2.5–1.0 cm | Large arteries with extensive elastic laminae | Conduct blood under high pressure |
Muscular arteries | 1.0 cm–0.3 mm | Thick-walled arteries with well-developed tunica media | Control blood flow to organs, regulate blood pressure |
Arterioles | 0.3 mm–10 μm | Thin walls with smooth muscle | Control blood flow to tissues, feed capillary beds |
Venules | 8.0–100 μm | Small veins, thin walls | Drain capillary beds |
Veins | 100 μm–1.5 cm | Thin-walled vessels with smooth muscle and valves | Return blood to the heart |

Additional info: This study guide expands on the original notes by providing definitions, examples, and academic context for each topic, ensuring completeness and clarity for exam preparation.
