 Back
BackBlood Vessels and Hemodynamics: ANP Study Guide
Study Guide - Smart Notes

Blood Vessels: Structure and Function
Overview of Blood Vessels
Blood vessels are essential components of the circulatory system, responsible for transporting blood throughout the body. They are classified into arteries, veins, and capillaries, each with distinct structural and functional characteristics.
Arteries: Carry blood away from the heart. Elastic arteries are large and stretchy, helping absorb pressure; muscular arteries are smaller and control blood flow to organs.
Veins: Carry blood toward the heart. They have thinner walls, larger lumens, and valves to prevent backflow.
Capillaries: Site of exchange of gases, nutrients, and wastes between blood and tissues. They are composed of simple squamous epithelium for efficient exchange.
Tunics of Blood Vessels
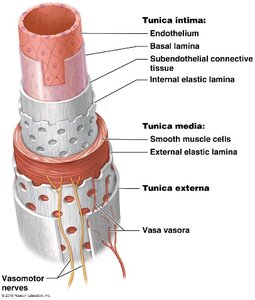
Blood vessels have three main layers, or tunics, each with specific tissue types and functions:
Tunica Intima (interna): Composed of endothelium, basal lamina, subendothelial connective tissue, and internal elastic lamina. Provides a smooth lining to reduce friction.
Tunica Media: Contains smooth muscle cells and elastic fibers. Responsible for vasoconstriction and vasodilation, controlled by the autonomic nervous system (ANS).
Tunica Externa: Made of connective tissue, provides protection and structural support.
Structural Differences Between Arteries and Veins
Arteries: Thicker walls, smaller lumen, no valves.
Veins: Thinner walls, larger lumen, presence of valves.
Atherosclerosis
Atherosclerosis is a disease characterized by the buildup of plaque in arteries, often caused by injury to the endothelium due to high blood pressure, high cholesterol, or diabetes. Treatment includes lifestyle changes, medications, and possible surgical interventions.

Hemodynamics: Physiology of Blood Flow
Factors Influencing Blood Flow
Hemodynamics refers to the study of blood flow and its regulation. Blood flow is influenced by pressure, resistance, and velocity.
Pressure: As pressure increases, blood flow increases.
Resistance: As resistance increases, blood flow decreases.
Velocity: As cross-sectional area increases, velocity decreases. Velocity is slowest in capillaries, which is beneficial for exchange of gases and nutrients.
Factors Affecting Blood Pressure
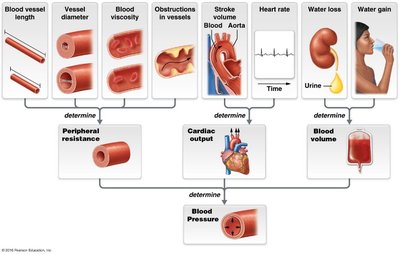
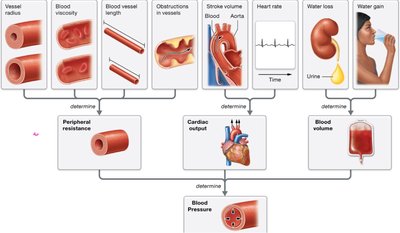
Blood pressure is determined by peripheral resistance, cardiac output, and blood volume. Each factor is influenced by vessel radius, blood viscosity, vessel length, obstructions, heart rate, stroke volume, water loss, and water gain.
Factor | Effect on Resistance (R) |
|---|---|
Blood vessel length | Increase length → Increase R |
Blood viscosity | Increase viscosity → Increase R |
Blood vessel radius | Decrease radius → Increase R |
Obstruction | Increase obstruction → Increase R |
Cardiac Output (CO): Increase in CO increases BP. Blood Volume: Increase in blood volume increases BP.
Equation:
Blood Pressure Variations in Circulation
Blood pressure differs between the pulmonary and systemic circuits. Pulmonary circuit has low blood pressure to protect the lungs, while systemic circuit has high blood pressure to supply the body.
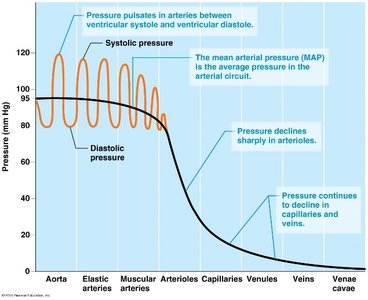
Systolic Pressure: Pressure in the artery during ventricular contraction.
Diastolic Pressure: Pressure in the artery during ventricular relaxation.
Pulse Pressure: Difference between systolic and diastolic pressure.
Mean Arterial Pressure (MAP): Average pressure in the arterial circuit. Calculated as:
Venous Return
Venous return is the flow of blood back to the heart. Since venous pressure is low, veins rely on valves, smooth muscle, skeletal muscle pump, and respiratory pump to assist blood return.
Valves: Prevent backflow.
Smooth Muscle: Vasoconstriction helps push blood forward.
Skeletal Muscle Pump: Muscle contractions squeeze veins.
Respiratory Pump: Changes in thoracic and abdominal pressure during breathing move blood toward the heart.
Regulation of Blood Pressure
Short-Term Regulation
Short-term regulation modifies cardiac output and resistance, primarily through the nervous and endocrine systems.
Sympathetic Nervous System: Increases heart rate, contractility, and vasoconstriction, raising BP.
Parasympathetic Nervous System: Decreases heart rate and induces vasodilation, lowering BP.
Baroreceptors: Monitor pressure changes and trigger feedback loops for rapid BP adjustment.
Endocrine Regulation
Hormones such as epinephrine, norepinephrine, angiotensin II, ADH, aldosterone, and ANP regulate cardiac output, resistance, and blood volume.
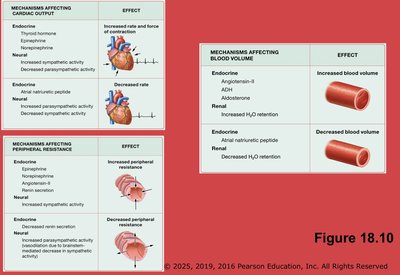
Long-Term Regulation
Long-term regulation adjusts blood volume via the urinary and endocrine systems. The kidneys play a central role by controlling water retention and excretion.
Hormone | Source | Target | Effect |
|---|---|---|---|
Angiotensin II | Liver/Kidney | Blood vessels | Vasoconstriction, ↑BP |
Aldosterone | Adrenal cortex | Kidneys | Na+ and water retention, ↑BV, ↑BP |
ADH | Posterior pituitary | Kidneys | Water retention, ↑BV, ↑BP |
ANP | Atria | Kidneys | Na+ and water excretion, ↓BV, ↓BP |
Capillaries and Tissue Perfusion
Mechanisms of Capillary Exchange
Capillary exchange occurs via three main mechanisms: diffusion and osmosis through gaps and fenestrations, transcytosis (endocytosis/exocytosis), and diffusion through endothelial membranes.
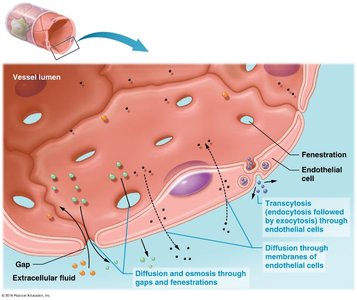
Types of Capillaries
Type | Structure | Function | Location |
|---|---|---|---|
Continuous | Least leaky | Restricts passage of substances | Muscle, brain |
Fenestrated | Has pores | Rapid exchange | Kidneys, intestine |
Sinusoid | Most leaky | Allows passage of large molecules | Liver, spleen |
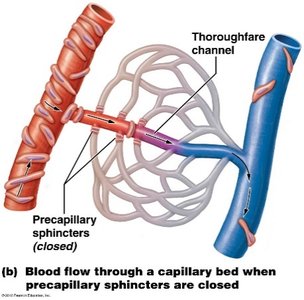
Autoregulation of Blood Flow
Myogenic Mechanism: Smooth muscle responds to changes in pressure to maintain ideal blood flow.
Metabolic Mechanism: Blood flow adjusts based on local metabolic needs (e.g., increased CO2, decreased O2, decreased pH cause vasodilation).
Capillary Pressures and Fluid Movement
Hydrostatic and Osmotic Pressures
Fluid movement across capillary walls is governed by hydrostatic and osmotic pressures:
Hydrostatic Pressure (HP): Pushes fluid out of capillaries.
Osmotic Pressure (OP): Pulls water into capillaries due to plasma proteins.
Pressure | Source | Direction |
|---|---|---|
HPc | Blood | Out of capillary |
HPif | Interstitial fluid | Into capillary |
OPc | Plasma proteins | Into capillary |
OPif | Interstitial proteins | Out of capillary |
Net Filtration Pressure (NFP):
Edema
Edema is the accumulation of excess fluid in the interstitial space, caused by excessive filtration or inadequate reabsorption.
Blood Pressure Disorders
Hypertension
Risk Factors: Smoking, obesity, high cholesterol.
Treatment: Lifestyle changes, medications, surgery.
"Silent Killer": Often asymptomatic.
Hypotension
Definition: Systolic < 90 mmHg, Diastolic < 60 mmHg.
Severe Hypotension: Circulatory shock.
Causes: Hypovolemic (low blood volume), cardiogenic (low cardiac output), anaphylactic/septic (excessive vasodilation).
Symptoms: Dizziness, fainting, cold/clammy skin, confusion, organ failure.
