 Back
BackBone Development, Growth, Remodeling, and Disorders
Study Guide - Smart Notes

Bones and Skeletal Tissue: Development and Growth
Ossification (Bone Formation)
Ossification, also known as osteogenesis, is the process by which bone tissue is formed. This process begins in the second month of embryonic development and continues throughout life as bones grow and remodel.
Endochondral Ossification: Bone forms by replacing hyaline cartilage. Most bones of the skeleton are formed this way.
Intramembranous Ossification: Bone develops directly from mesenchymal tissue. This process forms the flat bones of the skull, clavicle, and some facial bones.
Remodeling and Repair: Bone tissue is continuously remodeled and repaired throughout life.
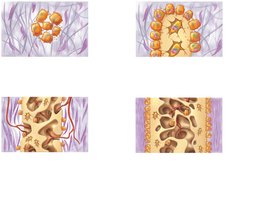
Endochondral Ossification
Endochondral ossification is the process by which most bones are formed, especially long bones. It involves the replacement of hyaline cartilage with bone tissue.
Bone collar forms around the diaphysis of the hyaline cartilage model.
Cartilage in the center of the diaphysis calcifies and develops cavities.
The periosteal bud invades the internal cavities, and spongy bone forms.
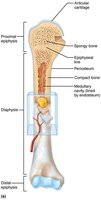
The diaphysis elongates, a medullary cavity forms, and secondary ossification centers appear in the epiphyses.
The epiphyses ossify, leaving hyaline cartilage only in the epiphyseal plates and articular cartilages.
Key Terms
Diaphysis: Shaft of a long bone.
Epiphysis: End of a long bone.
Epiphyseal Plate: Growth plate made of cartilage, responsible for lengthwise growth.
Medullary Cavity: Central cavity of bone shafts where marrow is stored.
Example: Long Bone Formation
Endochondral ossification is responsible for the formation of the femur, tibia, and other long bones.
Intramembranous Ossification
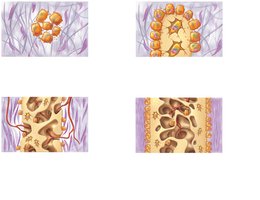
Intramembranous ossification forms bones directly from mesenchymal tissue, without a cartilage precursor. This process is essential for the development of flat bones.
Ossification centers appear in the fibrous connective tissue membrane.
Osteoid is secreted within the membrane and calcifies.
Trapped osteoblasts become osteocytes.
Woven bone and periosteum form.
Lamellar bone replaces woven bone, and red marrow appears.
Key Terms
Mesenchymal Cells: Embryonic cells that differentiate into osteoblasts.
Osteoblasts: Bone-forming cells.
Osteocytes: Mature bone cells.
Osteoid: Unmineralized bone matrix.
Example: Skull Formation
Intramembranous ossification forms the frontal, parietal, occipital, temporal bones, and the clavicle.
Bone Growth: Postnatal Development
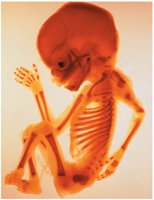
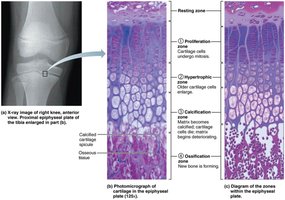
Interstitial Growth (Lengthwise Growth)
Long bones grow in length at the epiphyseal plate through interstitial growth. This process continues until adolescence, when the epiphyseal plate closes and forms the epiphyseal line.
Epiphyseal Plate: Cartilage growth plate responsible for longitudinal bone growth.
Epiphyseal Line: Remnant of the epiphyseal plate in adults.
Growth Stops: Females around 18 years, males around 21 years.
Appositional Growth (Widthwise Growth)
Bones increase in thickness or diameter through appositional growth. Osteoblasts in the periosteum add bone matrix to the external surface, while osteoclasts remove bone from the internal surface.
Osteoblasts: Build new bone on the periosteal surface.
Osteoclasts: Remove bone from the endosteal surface.
Response to Stress: Bones thicken in response to increased mechanical stress.
Disorders of Bone Growth
Dwarfism
Dwarfism refers to conditions resulting in short stature due to abnormal bone growth.
Achondroplastic Dwarfism: Failure of cartilage growth in the metaphysis due to a spontaneous mutation.
Pituitary Dwarfism: Lack of growth hormone, resulting in normal body proportions but short stature.

Bone Remodeling
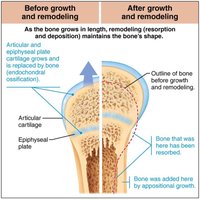
Growth and Remodeling During Youth
Bone growth and remodeling are dynamic processes that occur throughout life. During youth, bones grow in length and width, and remodeling maintains bone shape and strength.
Remodeling: Involves both bone deposit (by osteoblasts) and bone resorption (by osteoclasts).
Frequency: 5-7% of bone is recycled weekly; spongy bone is replaced every 3-4 years, compact bone every 10 years.
Physiology of Osseous Tissue
Ectopic Ossification
Ectopic ossification refers to abnormal bone formation in tissues where bone should not exist. This can occur due to genetic or environmental factors.
Calcium Homeostasis and Hormonal Control
Calcium Regulation
Blood calcium levels are tightly regulated between 9–11 mg/100 ml. Hormones control bone remodeling to maintain calcium balance.
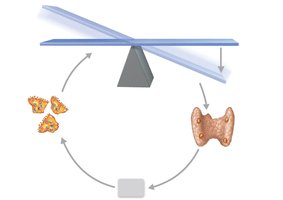
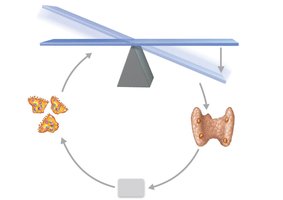
Parathyroid Hormone (PTH): Released in response to low blood calcium; stimulates osteoclasts to resorb bone and release calcium.
Calcitonin: Released in response to high blood calcium; stimulates osteoblasts to deposit bone and lower calcium levels.
Equation: Calcium Homeostasis
Homeostatic Imbalance
Hypocalcemia: Low blood calcium causes hyperexcitability of nerves and muscles.
Hypercalcemia: High blood calcium causes nonresponsiveness of nerves and muscles.
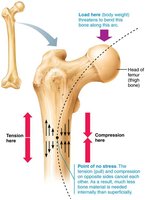
Mechanical Stress and Bone Remodeling
Wolf’s Law
Wolf’s Law states that bones grow or remodel in response to mechanical demands. Increased stress from muscle activity or weight-bearing leads to thicker, stronger bones.
Handedness: Bones of the dominant hand are thicker.
Active Muscles: Weight lifters have thicker bones.
Inactivity: Bedridden individuals and fetuses have thinner bones.
Fractures and Healing
Fracture Classification
Fractures are classified based on the position of bone ends, completeness of the break, and whether the skin is penetrated.
Nondisplaced: Bone ends retain normal position.
Displaced: Bone ends are out of alignment.
Complete: Bone is broken through.
Incomplete: Bone is not broken through.
Open (Compound): Skin is penetrated.
Closed (Simple): Skin is not penetrated.
Common Types of Fractures
Fracture Type | Description and Comments |
|---|---|
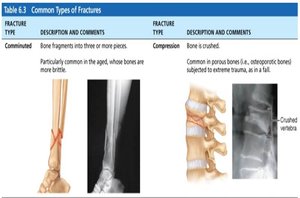
Comminuted | Bone fragments into three or more pieces. Common in aged, brittle bones. |
Compression | Bone is crushed. Common in porous bones subjected to trauma. |
Fracture Type | Description and Comments |
|---|---|
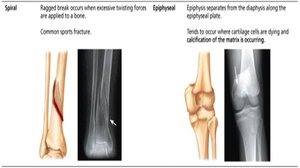
Spiral | Ragged break from excessive twisting forces. Common sports fracture. |
Epiphyseal | Epiphysis separates from diaphysis along epiphyseal plate. Occurs where cartilage cells are dying. |
Fracture Type | Description and Comments |
|---|---|
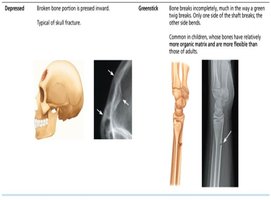
Depressed | Broken bone portion is pressed inward. Typical of skull fracture. |
Greenstick | Bone breaks incompletely, like a green twig. Common in children. |
Healing of Fractures
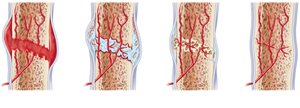
Bone healing occurs in four stages:
Hematoma forms.
Fibrocartilaginous callus forms.
Bony callus forms.
Bone remodeling occurs.
Bone Disorders: Osteoporosis
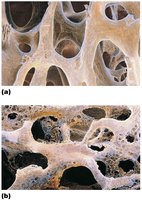
Osteoporosis
Osteoporosis is a severe loss of bone density where bone resorption exceeds bone deposit. It is most common in postmenopausal women and increases with age.
Risk Factors: Insufficient exercise, poor diet, smoking, genetics, hormone-related conditions, hyperthyroidism, diabetes mellitus, alcohol, and certain medications.
Effects: Bones become fragile and more likely to fracture.
Additional info:
Bone remodeling is essential for maintaining calcium homeostasis and adapting to mechanical stress.
Osteoblasts and osteoclasts are key cells in bone formation and resorption.
Proper nutrition and physical activity are crucial for bone health throughout life.
