 Back
BackBone Remodeling and Repair: Structure, Regulation, and Healing
Study Guide - Smart Notes

Bones and Skeletal Tissues
Bone Remodeling
Bone remodeling is a dynamic process that maintains bone strength and mineral homeostasis throughout life. It involves the coordinated actions of bone deposition and resorption, replacing 5–10% of bone mass annually. Spongy bone is replaced every 3–4 years, while compact bone is replaced every 10 years. Remodeling occurs at the surfaces of both the periosteum and endosteum, with remodeling units consisting of adjacent osteoblasts and osteoclasts.
Osteoblasts: Cells responsible for bone formation; deposit new bone matrix.
Osteoclasts: Cells responsible for bone resorption; break down bone matrix.
Osteocytes: Mature bone cells derived from osteoblasts; help maintain bone tissue.
Remodeling units: Packets of osteoblasts and osteoclasts that coordinate the remodeling process.
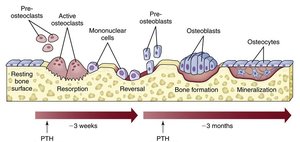
Bone Deposition
Bone deposition is the process by which osteoblasts lay down new bone matrix. The osteoid seam is a band of unmineralized bone matrix marking the area of new matrix, while the calcification front is the transition zone between osteoid seam and older mineralized bone. Triggers for deposition may include mechanical signals, increased calcium and phosphate ion concentrations, matrix proteins, and the enzyme alkaline phosphatase.
Osteoid seam: Unmineralized new bone matrix.
Calcification front: Zone where mineralization begins.
Alkaline phosphatase: Enzyme essential for mineralization.
Bone Resorption
Bone resorption is carried out by osteoclasts, which digest bone matrix by secreting lysosomal enzymes and protons (H+). The acidity dissolves calcium salts, making them soluble. Osteoclasts also phagocytize demineralized matrix and dead osteocytes, releasing waste into the blood. Osteoclast activation is regulated by parathyroid hormone (PTH) and immune T cell proteins.
Lysosomal enzymes: Digest organic bone matrix.
Protons (H+): Acidify the area, dissolving mineral salts.
PTH: Stimulates osteoclast activity in response to low blood calcium.
Control of Bone Remodeling
Bone remodeling is regulated by two main control loops: hormonal regulation and response to mechanical stress.
Hormonal regulation: Maintains calcium homeostasis in the blood, primarily through PTH and, to a lesser extent, calcitonin.
Mechanical stress: Bone adapts to the loads placed upon it, strengthening areas under greatest stress (Wolff’s law).
Hormonal Control
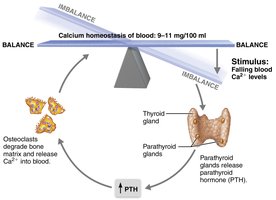
Calcium homeostasis is critical for nerve and muscle function. Of the 1200–1400 g of calcium in the body, 99% is stored in bone. Blood calcium is maintained at 9–11 mg/dl.
Parathyroid hormone (PTH): Released in response to low blood calcium; stimulates osteoclasts to resorb bone, releasing calcium into the blood.
Calcitonin: Released in response to high blood calcium; effects are minor in humans but can lower blood calcium at high doses.
Clinical Imbalances
Hypocalcemia: Low blood calcium; causes hyperexcitability of nerves and muscles.
Hypercalcemia: High blood calcium; causes nonresponsiveness and can lead to kidney stones.
Mechanical Stress and Wolff’s Law
Wolff’s law states that bones grow or remodel in response to the demands placed on them. Stress is usually off-center, causing bones to bend, with the diaphysis thickest where bending stresses are greatest. Trabeculae form along lines of stress, and large projections develop where muscles attach. Bones of inactive individuals (e.g., bedridden patients) are featureless due to lack of stress.

Bone Repair
Fractures and Their Classification
Fractures are breaks in bone, commonly caused by trauma in youth and bone thinning in old age. They are classified by:
Position of bone ends: Nondisplaced (normal position) or displaced (misaligned).
Completeness of break: Complete (all the way through) or incomplete.
Penetration of skin: Open (compound) or closed (simple).
Fractures can also be described by location, appearance, and nature of the break.
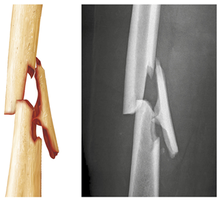
Table: Common Types of Fractures
Fracture Type | Description |
|---|---|
Comminuted | Bone fragments into three or more pieces; common in aged, brittle bones. |
Compression | Bone is crushed; common in porous bones (e.g., vertebrae). |
Spiral | Ragged break from twisting forces; common sports fracture. |
Epiphyseal | Epiphysis separates from diaphysis along growth plate. |
Depressed | Broken bone portion pressed inward; typical of skull fracture. |
Greenstick | Bone breaks incompletely; common in children. |
Fracture Treatment and Repair
Treatment involves reduction (realignment of bone ends) and immobilization. Closed reduction is manual, while open reduction uses surgical pins or wires. Healing time depends on severity, bone involved, and patient age.
Stages of Bone Repair
Hematoma formation: Torn blood vessels hemorrhage, forming a mass of clotted blood (hematoma). The site becomes swollen, painful, and inflamed.
Fibrocartilaginous callus formation: Capillaries grow into the hematoma; phagocytic cells clear debris; fibroblasts secrete collagen fibers to connect bone ends; cartilage and osteogenic cells reconstruct bone; osteoblasts form spongy bone within the matrix.
Bony callus formation: New trabeculae appear in the callus within a week; callus is converted to bony (hard) callus of spongy bone over about two months.
Bone remodeling: Begins during bony callus formation and continues for several months; excess material is removed, and compact bone is laid down to reconstruct shaft walls, restoring original structure.




Summary Table: Stages in the Healing of a Bone Fracture
Stage | Description |
|---|---|
Hematoma formation | Clotted blood forms at fracture site; inflammation occurs. |
Fibrocartilaginous callus formation | Soft callus of collagen and cartilage bridges the break. |
Bony callus formation | Spongy bone replaces soft callus, forming a hard callus. |
Bone remodeling | Excess material is removed; compact bone restores shaft. |
Additional info: Bone remodeling and repair are essential for maintaining skeletal integrity and function throughout life. Disruptions in these processes can lead to clinical conditions such as osteoporosis, delayed fracture healing, or abnormal bone growth.
