 Back
BackBones and Skeletal Tissue: Structure, Function, Development, and Disorders
Study Guide - Smart Notes

Bones and Skeletal Tissue
Skeletal Cartilage
Skeletal cartilage is a resilient tissue that provides support and flexibility to various parts of the body. It is avascular and lacks nerves, receiving nutrients from the surrounding perichondrium. There are three main types of cartilage:
Hyaline cartilage: Most abundant, provides support with flexibility.
Elastic cartilage: More flexible, found in structures like the ear.
Fibrocartilage: Highly compressible, found in intervertebral discs.
Cartilage consists of chondrocytes housed in lacunae within an extracellular matrix. Growth occurs via:
Appositional growth: New matrix added to the surface.
Interstitial growth: Chondrocytes divide and secrete new matrix from within.
Functions of Bone
Bones serve multiple essential functions in the human body:
Support: Framework for the body and soft organs.
Protection: Shields vital organs (e.g., brain, spinal cord).
Movement: Acts as levers for muscles.
Mineral storage: Reservoir for calcium and phosphate.
Blood cell formation: Hematopoiesis occurs in red marrow.
Fat storage: Yellow marrow stores fat.
Hormone production: Osteocalcin regulates metabolism.
Bone Classification
The human skeleton consists of 206 bones, classified into two main groups:
Axial skeleton: Skull, vertebral column, rib cage (protection and support).
Appendicular skeleton: Limbs and girdles (movement and support).
Bones are further classified by shape:
Long bones: Longer than wide (e.g., femur, humerus).
Short bones: Cube-shaped (e.g., carpals, tarsals).
Flat bones: Thin, flattened, and curved (e.g., sternum, skull).
Irregular bones: Complex shapes (e.g., vertebrae, hip bones).
Sesamoid bones: Form in tendons (e.g., patella).
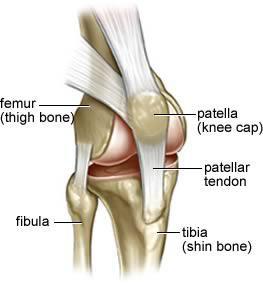
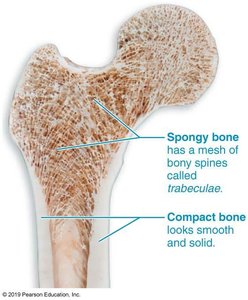
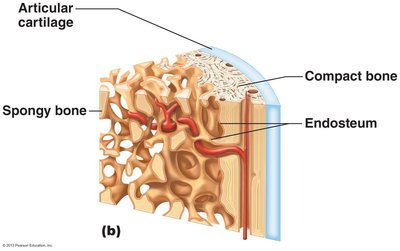
Bone Structure
Bones have a complex structure, consisting of:
Compact bone: Dense, smooth outer layer.
Spongy bone: Honeycomb structure with trabeculae and marrow cavities.
Long bones have distinct regions:
Diaphysis: Shaft, compact bone with medullary cavity.
Epiphyses: Ends, compact exterior and spongy interior.
Epiphyseal line: Separates diaphysis and epiphyses.
Membranes:
Periosteum: Outer membrane, fibrous and osteogenic layers.
Endosteum: Internal membrane, covers bone surfaces.
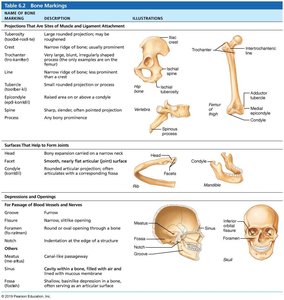
Bone Markings
Bones display markings that serve as sites for muscle, ligament, and tendon attachment, joint surfaces, and conduits for blood vessels and nerves. These include projections, depressions, and openings.
Marking | Description | Illustration |
|---|---|---|
Tuberosity | Large rounded projection | Example: humerus |
Head | Bony expansion carried on a narrow neck | Example: femur |
Foramen | Round or oval opening | Example: skull |
Fossa | Shallow depression | Example: scapula |
Condyle | Rounded articular projection | Example: mandible |
Additional info: Table includes other markings such as crest, spine, and groove. |
Microscopic Anatomy of Bone
Bones contain several cell types, each with specific functions:
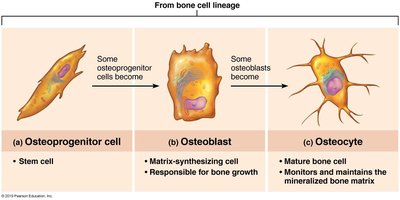
Osteogenic cells: Stem cells that differentiate into osteoblasts.
Osteoblasts: Bone-forming cells that secrete matrix.
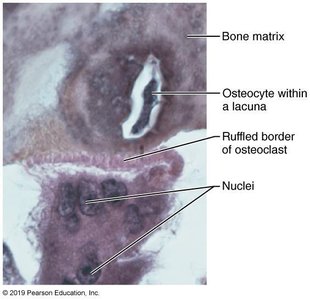
Osteocytes: Mature cells maintaining bone matrix.
Bone lining cells: Maintain bone surfaces where no remodeling occurs.
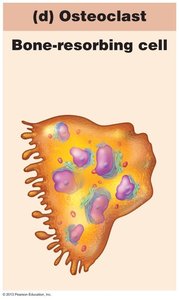
Osteoclasts: Bone-resorbing cells derived from hematopoietic stem cells.

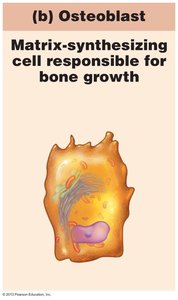
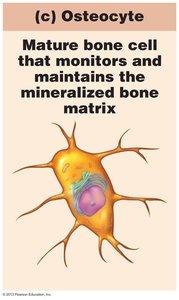
Compact Bone Structure
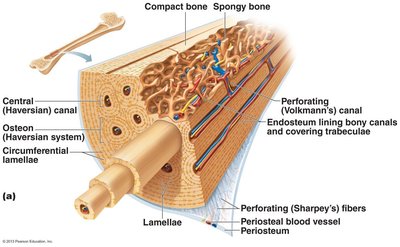
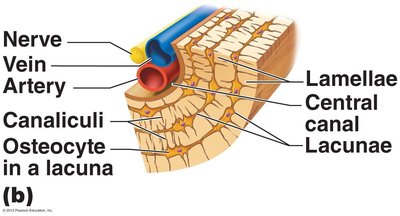
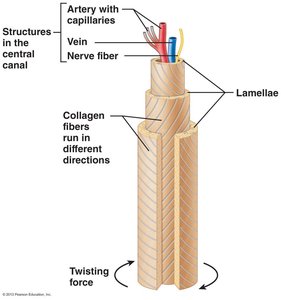
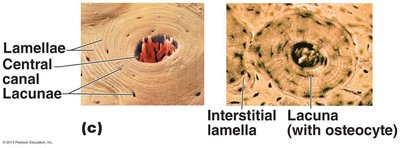
Compact bone is organized into osteons (Haversian systems), which are cylindrical structures aligned parallel to the bone's axis. Each osteon contains:
Lamellae: Concentric rings of bone matrix.
Central (Haversian) canal: Contains blood vessels and nerves.
Perforating (Volkmann's) canals: Connect blood vessels and nerves of periosteum to central canal.
Lacunae: Spaces housing osteocytes.
Canaliculi: Tiny canals connecting lacunae.
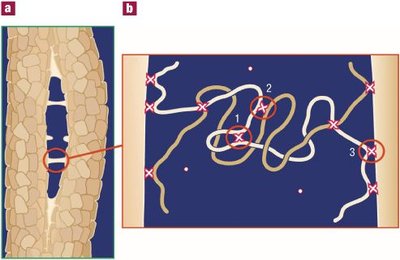
Spongy Bone Structure
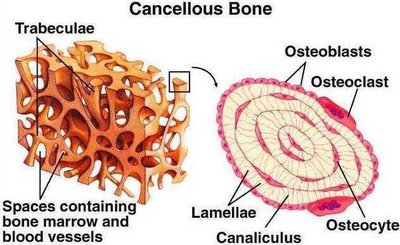
Spongy bone consists of trabeculae, which are aligned along lines of stress to provide strength. Trabeculae are composed of irregularly arranged lamellae and osteocytes interconnected by canaliculi. Unlike compact bone, spongy bone does not contain osteons.
Bone Chemical Composition
Bones are composed of both organic and inorganic components:
Organic: Bone cells and osteoid (ground substance and collagen fibers), providing flexibility and tensile strength.
Inorganic: Mineral salts (hydroxyapatites), providing hardness and resistance to compression.
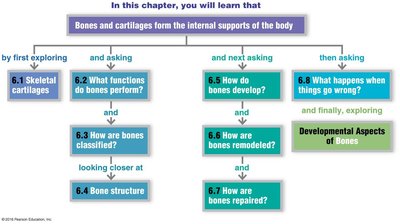
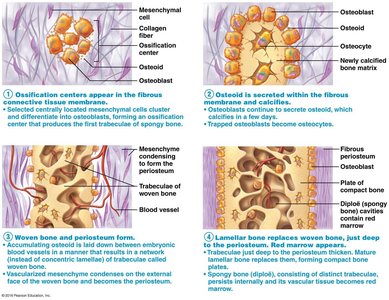
Bone Development (Ossification)
Ossification is the process of bone formation, which occurs during embryonic development, growth, and repair. There are two main types:
Endochondral ossification: Bone forms by replacing hyaline cartilage (all bones except skull and clavicle).
Intramembranous ossification: Bone develops from fibrous membrane (skull and clavicle).
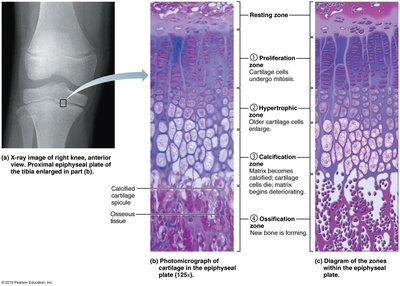
Postnatal Bone Growth
Growth in Length
Occurs at the epiphyseal plate via interstitial growth:
Resting zone: Inactive chondrocytes.
Proliferation zone: Rapid cell division.
Hypertrophic zone: Older chondrocytes enlarge.
Calcification zone: Matrix calcifies, chondrocytes die.
Ossification zone: New bone forms.
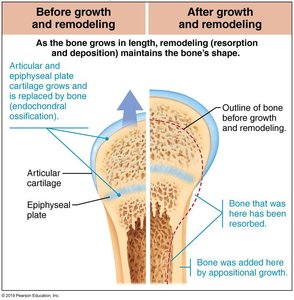
Growth in Width
Appositional growth occurs as osteoblasts add bone to the periosteum, while osteoclasts remove bone from the endosteum.
Bone Remodeling
Bone remodeling is a continuous process involving bone formation and resorption at periosteal and endosteal surfaces. It is regulated by:
Negative feedback loop for calcium homeostasis: Maintains blood Ca2+ levels.
Mechanical and gravitational forces: Wolff's Law states bone adapts to the demands placed on it.
Bone Repair
Bone repair occurs in several stages following a fracture:
Hematoma formation: Blood clots at fracture site.
Soft callus formation: Granulation tissue forms, phagocytes clean debris, fibrocartilaginous callus develops.
Hard callus formation: Spongy bone replaces soft callus.
Bone remodeling: Spongy bone is replaced by compact bone.
Homeostatic Imbalances of Bone
Several disorders affect bone health:
Osteomalacia and Rickets: Poor mineralization, pain when bearing weight.
Osteoporosis: Bone resorption exceeds deposition, leading to decreased bone mass.
Paget's Disease: Excessive bone formation and resorption, causing weak and deformed bones.
Cleft palate, herniated disc, scoliosis, kyphosis, lordosis: Structural abnormalities.
Colle's fracture: Distal radius break.
Pott's fracture: Distal fibula/tibia fracture.
Carpal tunnel syndrome: Compression of the median nerve in the wrist.
Example: Colle's fracture is common in falls, especially in elderly individuals with osteoporosis.
Example: Pott's fracture often results from ankle injuries.
Example: Carpal tunnel syndrome is associated with repetitive wrist movements.
Additional info: Disorders may require medical intervention, including surgery, immobilization, or physical therapy.
