 Back
BackBones and Skeletal Tissues: Structure, Function, and Development
Study Guide - Smart Notes

Chapter 6: Bones and Skeletal Tissues
6-1 Cartilage: Basic Structure, Types, and Locations
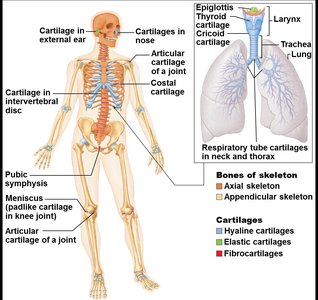
Cartilage is a resilient, semi-rigid connective tissue that provides support and flexibility to different parts of the skeleton. It is avascular and lacks nerves, relying on diffusion for nutrient delivery. The perichondrium, a dense connective tissue, surrounds cartilage and aids in nutrient supply and resistance to outward expansion.
Chondrocytes reside in spaces called lacunae within the extracellular matrix.
Three main types of cartilage:
Hyaline cartilage: Most abundant; provides support, flexibility, and resilience. Found in articular, costal, respiratory, and nasal cartilages.
Elastic cartilage: Contains elastic fibers; found in the external ear and epiglottis.
Fibrocartilage: Contains thick collagen fibers; provides tensile strength. Found in menisci of the knee and intervertebral discs.
Growth occurs by appositional growth (matrix secreted on external surface) and interstitial growth (matrix secreted within).
Cartilage can calcify with age but is not bone.
Type | Location | Main Features |
|---|---|---|
Hyaline | Joints, ribs, nose, respiratory tract | Support, flexibility |
Elastic | Ear, epiglottis | Elasticity |
Fibrocartilage | Knee, intervertebral discs | Tensile strength |
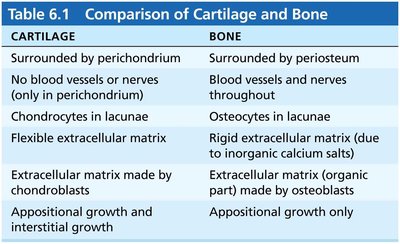
Comparison of Cartilage and Bone
Cartilage and bone are both connective tissues but differ in structure, function, and growth patterns.
Cartilage | Bone |
|---|---|
Surrounded by perichondrium | Surrounded by periosteum |
No blood vessels or nerves (except in perichondrium) | Blood vessels and nerves throughout |
Chondrocytes in lacunae | Osteocytes in lacunae |
Flexible extracellular matrix | Rigid extracellular matrix (due to inorganic calcium salts) |
Matrix made by chondroblasts | Matrix (organic part) made by osteoblasts |
Appositional and interstitial growth | Appositional growth only |
6-2 Classification of Bones by Location and Shape
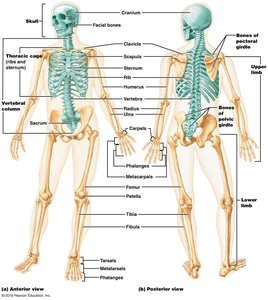
The adult human skeleton consists of 206 named bones, divided into axial and appendicular groups. Bones are also classified by shape: long, short, flat, and irregular.
Axial skeleton: Skull, vertebral column, rib cage (long axis of body).
Appendicular skeleton: Limbs and girdles attaching limbs to axial skeleton.
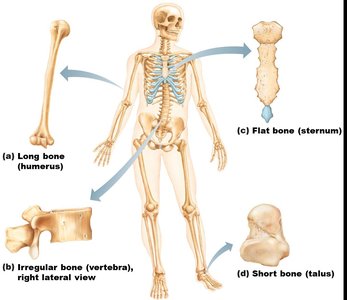
Long bones: Longer than wide (e.g., humerus).
Short bones: Cube-shaped (e.g., wrist, ankle); sesamoid bones (e.g., patella).
Flat bones: Thin, flat, slightly curved (e.g., sternum, ribs, skull bones).
Irregular bones: Complicated shapes (e.g., vertebrae, coxal bones).
6-3 Functions of the Skeletal System
The skeletal system performs several vital functions essential for human survival and movement.
Support: Framework for the body and soft organs.
Protection: Shields brain, spinal cord, and vital organs.
Movement: Acts as levers for muscle action.
Mineral storage: Reservoir for calcium, phosphorus, and growth factors.
Blood cell formation: Hematopoiesis in red marrow cavities.
Triglyceride storage: Fat storage in bone cavities (energy source).
Hormone production: Osteocalcin regulates insulin secretion and protects against obesity and diabetes.
6-4 Structure of Bones: Tissue Levels
Bones are organs composed of several tissue types, including osseous tissue, nervous tissue, cartilage, fibrous connective tissue, muscle, and epithelial cells in blood vessels. Bone structure is studied at three levels: gross anatomy, microscopic, and chemical.
Gross anatomy: Macroscopic structure (shape, markings, membranes).
Microscopic anatomy: Cellular and tissue organization.
Chemical composition: Organic and inorganic components.
6-5 Gross Anatomy of Bones
Bone Textures
Compact bone: Dense outer layer; smooth and solid.
Spongy bone (cancellous or trabecular): Honeycomb of flat pieces called trabeculae.
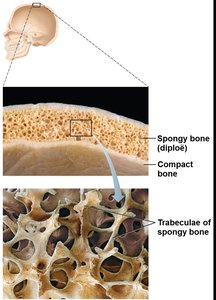
Structure of Short, Irregular, and Flat Bones
Thin plates of spongy bone covered by compact bone.
Sandwiched between periosteum (outer) and endosteum (inner).
No shaft or epiphyses; bone marrow throughout spongy bone, but no marrow cavity.
Hyaline cartilage covers surfaces at joints.
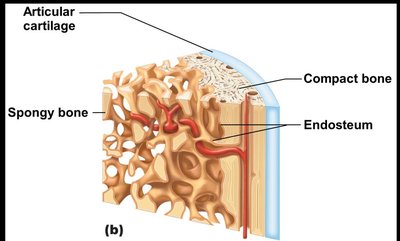
Structure of Long Bones
Diaphysis: Tubular shaft; compact bone surrounds medullary cavity.
Epiphyses: Bone ends; external compact bone, internal spongy bone, articular cartilage covers surfaces.
Epiphyseal line: Remnant of growth plate between diaphysis and epiphysis.
Membranes
Periosteum: Double-layered membrane covering external bone (except joints); outer fibrous layer (dense irregular connective tissue), inner osteogenic layer (osteogenic cells).
Endosteum: Delicate membrane covering internal bone surfaces, trabeculae, and canals; contains osteogenic cells.
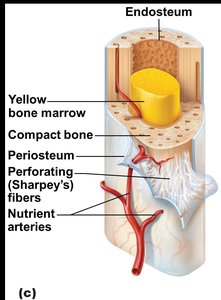
Bone Cavities
Red marrow: Hematopoietic tissue in trabecular cavities of spongy bone and heads of long bones; most active in children and some adult bones (e.g., femur, humerus).
Yellow marrow: Fat storage in medullary cavity; can convert to red marrow if needed.
Bone Markings
Projections: Sites for muscle and ligament attachment (e.g., iliac crest, ischial tuberosity).
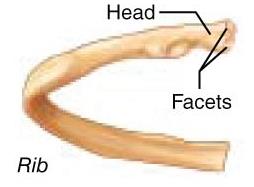
Surfaces: Form joints (e.g., head, facets).
Depressions and openings: Passageways for blood vessels and nerves (e.g., meatus, fossa, notch, groove, sinus, foramen).
6-6 Microscopic Anatomy of Bone
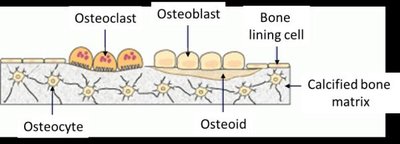
Bone Cells
Osteogenic cells: Stem cells in periosteum and endosteum; differentiate into osteoblasts or bone lining cells.
Osteoblasts: Bone-forming cells; secrete osteoid (unmineralized bone matrix).
Osteocytes: Mature bone cells in lacunae; monitor and maintain bone matrix; act as stress sensors.
Bone lining cells: Flat cells on bone surfaces; help maintain matrix (periosteal and endosteal cells).
Osteoclasts: Multinucleate cells derived from hematopoietic stem cells; resorb bone matrix.
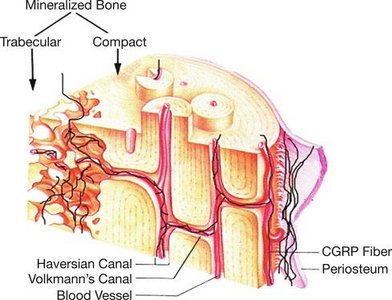
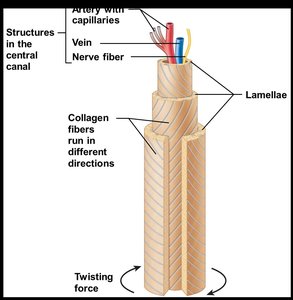
Compact Bone (Lamellar Bone)
Osteon (Haversian system): Structural unit; elongated cylinder parallel to bone's long axis; concentric lamellae resist twisting forces.
Central (Haversian) canal: Contains blood vessels and nerves.
Perforating (Volkmann's) canals: Connect blood vessels and nerves of periosteum, medullary cavity, and central canal.
Lacunae: Small cavities containing osteocytes.
Canaliculi: Hairlike canals connecting lacunae; allow communication and nutrient/waste exchange.
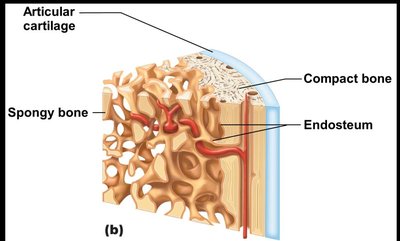
Spongy Bone
Trabeculae align along lines of stress; no osteons.
Irregularly arranged lamellae and osteocytes interconnected by canaliculi.
Capillaries in endosteum supply nutrients.
6-7 Chemical Composition of Bone
Organic components: Osteogenic cells, osteoblasts, osteocytes, bone-lining cells, osteoclasts, and osteoid (ground substance and collagen fibers). Provide tensile strength and flexibility.
Inorganic components: Hydroxyapatites (mineral salts, mainly calcium phosphate crystals); 65% of bone by mass. Responsible for hardness and resistance to compression.
Bones are half as strong as steel in resisting compression and as strong as steel in tension. Their mineral composition allows them to last long after death, revealing information about ancient populations.
6-8 Bone Development (Ossification)
Ossification (osteogenesis) is the process of bone tissue formation, beginning in the second month of development and continuing throughout life.
Endochondral ossification: Bone forms by replacing hyaline cartilage; forms most of the skeleton.
Intramembranous ossification: Bone develops from fibrous membrane; forms flat bones (e.g., clavicles, cranial bones).
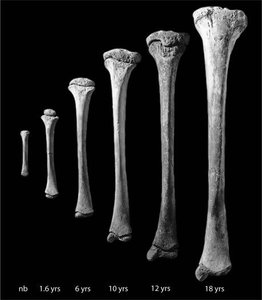
Postnatal bone growth: Interstitial (length) and appositional (thickness) growth.
Bone remodeling and repair: Occurs throughout life; involves both deposition and resorption.
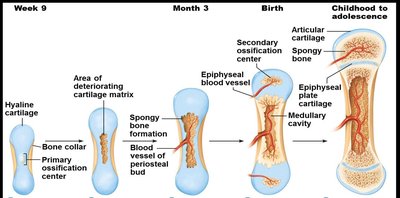
Steps in Endochondral Ossification
Bone collar forms around diaphysis of cartilage model.
Central cartilage in diaphysis calcifies, then develops cavities.
Periosteal bud invades cavities, forming spongy bone.
Diaphysis elongates and medullary cavity forms.
Epiphyses ossify.
Steps in Intramembranous Ossification
Mesenchymal cells cluster and differentiate into osteoblasts, forming ossification centers.
Osteoblasts secrete osteoid, which calcifies; osteoblasts become osteocytes.
Osteoid is laid down around blood vessels, forming immature trabeculae; periosteum forms.
Trabeculae are remodeled to form compact bone; red marrow develops.
Postnatal Bone Growth
Interstitial growth: Increases length of long bones; requires epiphyseal cartilage (growth plate).
Appositional growth: Increases bone thickness; occurs throughout life.
Zones of Epiphyseal Plate (Growth in Length)
Resting (quiescent) zone: Relatively inactive cartilage on epiphyseal side.
Proliferation (growth) zone: Rapidly dividing cartilage on diaphysis side; pushes epiphysis away from diaphysis.
Hypertrophic zone: Older chondrocytes enlarge and lacunae erode.
Calcification zone: Matrix calcifies, chondrocytes die.
Ossification zone: Calcified cartilage spicules are eroded by osteoclasts and covered with new bone by osteoblasts.
6-9 Bone Homeostasis
Bone is a dynamic tissue, constantly remodeled through bone deposit (by osteoblasts) and resorption (by osteoclasts). About 5-7% of bone mass is recycled weekly. Remodeling is regulated by hormonal (calcium homeostasis) and mechanical (stress) factors.
Calcium functions: Nerve and muscle impulse transmission, bone and teeth strength, blood coagulation, gland and nerve secretion, cell division.
99% of body calcium is in bones; blood calcium is tightly regulated (9-11 mg/dl).
Intestinal absorption requires vitamin D; dietary intake is essential.
Hormonal Regulation of Blood Calcium
Parathyroid hormone (PTH): Released when blood Ca2+ is low; stimulates osteoclasts to resorb bone, releasing Ca2+ into blood.
Negative feedback loop: When Ca2+ rises, PTH release ends.
6-10 Bone Fractures and Repair
Fracture classifications:
Position of bone ends: Nondisplaced (normal position) vs. displaced (misaligned).
Completeness: Complete (all the way through) vs. incomplete.
Skin penetration: Open (compound) vs. closed (simple).
Repair steps:
Hematoma formation
Fibrocartilaginous callus formation
Bony callus formation
Bone remodeling
6-11 Bone Disorders
Osteoporosis: Bone-thinning disease; common in postmenopausal women and elderly men; increases fracture risk.
Osteomalacia/Rickets: Poorly mineralized (soft) bones due to calcium/vitamin D deficiency; rickets is the childhood form, causing deformities.
Paget's Disease: Excessive, haphazard bone deposition and resorption; reduced mineralization; spotty bone weakening.
Bony spurs: Abnormal bone projections due to overgrowth; common in aging bones.
Osteosarcoma: Aggressive bone cancer, primarily in long bones of young adults; metastasizes to lungs.
Summary Table: Learning Objectives
Identify and describe characteristics of skeletal cartilage and bone.
Classify bones by location and shape.
List functions of the skeletal system.
Describe gross and microscopic anatomy of bones.
Understand chemical composition and its functional implications.
Explain ossification, bone growth, remodeling, and repair.
Describe bone homeostasis and calcium regulation.
List fracture types and repair steps.
Describe major bone disorders.
