 Back
BackHeart Part 4 Cardiac Output and Heart Rate Regulation: ANP Study Guide
Study Guide - Smart Notes

Cardiac Output (Q)
Definition and Calculation
Cardiac output (Q) is the amount of blood pumped by each ventricle in one minute. It is a fundamental measure of cardiovascular function and is influenced by both heart rate and stroke volume.
Heart Rate (HR): Number of beats per minute (bpm).
Stroke Volume (SV): Amount of blood ejected per beat (ml/beat).
Formula:
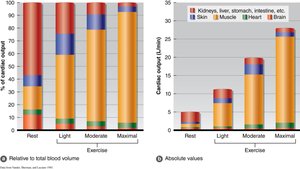
Resting Q: Approximately 5 L/min (HR ~70 bpm, SV ~70 ml/beat).
Maximal Q: Can reach 20-25 L/min in sedentary individuals, up to 35 L/min in endurance athletes.
Cardiac output changes in response to alterations in heart rate and/or stroke volume.
Stroke Volume Regulation
Stroke Volume Formula and Influencing Factors
Stroke volume (SV) is determined by the difference between end-diastolic volume (EDV) and end-systolic volume (ESV):
Formula:
Typical values: EDV ~120 ml, ESV ~50 ml, SV ~70 ml/beat.
Three main factors: Preload, Contractility, Afterload.
Preload
Preload refers to the degree of stretch of the heart muscle before contraction. It is primarily determined by venous return—the amount of blood returning to the heart.
Greater stretch leads to greater filling and increased ejection (Frank-Starling law).
Slow heart rate and exercise increase venous return, stretching ventricles and increasing force of contraction.
Length-tension relationship: Not ideal at rest due to myofilament overlap.
Contractility
Contractility is the contractile strength at a given muscle length, independent of muscle stretch and EDV.
Increased contractility lowers ESV.
Sympathetic nervous system (SNS) stimulation increases Ca++ influx, leading to more cross-bridge formation and greater force of contraction.
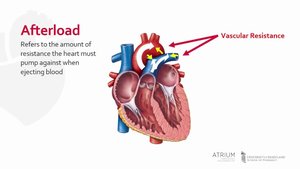
Afterload
Afterload is the back pressure exerted by arterial blood, representing the pressure ventricles must overcome to eject blood.
Greater afterload requires greater pressure to open semilunar (SL) valves.
Hypertension increases afterload, elevating ESV and reducing SV.
Heart Rate Regulation
Main Regulators
Heart rate is regulated by the autonomic nervous system (ANS) and hormones.
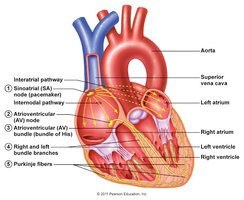
Autonomic Nervous System (ANS)
Sympathetic Nervous System (SNS): Activated by emotional or physical stressors. Norepinephrine binds to Beta-1 receptors, causing pacemaker cells to fire more rapidly, increasing HR, decreasing filling time (EDV), increasing contractility, and decreasing ESV.
Parasympathetic Nervous System (PNS): Opposes SNS effects. Acetylcholine hyperpolarizes pacemaker cells via K+ channels, slowing HR. No effect on contractility.
Vagal Tone: At rest, PNS dominates, decreasing intrinsic SA node rate from 100 to ~70 bpm. Cutting the vagus nerve increases HR to ~100 bpm at rest.
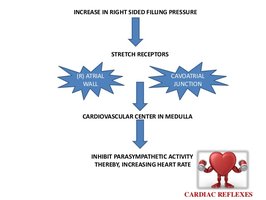
Atrial (Bainbridge) Reflex: Sympathetic reflex caused by increased venous return, stretching atrial walls and stimulating the SA node to increase HR.
Chemical Regulation
Epinephrine: Released from the adrenal medulla, increases HR and contractility.
Thyroxine: Increases HR and enhances effects of catecholamines.
Other Factors Affecting Heart Rate
Age: Fetus has fastest HR; HR declines with age.
Sex: Females generally have faster HR than males.
Exercise: Increases HR; chronic exercise lowers resting HR (increased vagal tone).
Body Temperature: Increased body temperature raises HR.
Abnormal Heart Rate
Tachycardia and Bradycardia
Tachycardia: Abnormally fast HR (>100 bpm); persistent tachycardia can lead to fibrillation.
Bradycardia: Low HR (<60 bpm); can result in poor blood circulation. Normal and desirable in endurance training due to increased stroke volume.
Factors Influencing Cardiac Output
Cardiac output is influenced by heart rate, stroke volume, preload, contractility, afterload, and various physiological and chemical factors.
Summary Table: Factors Affecting Cardiac Output
Factor | Effect on Cardiac Output | Mechanism |
|---|---|---|
Heart Rate | Increase/Decrease | ANS, hormones, exercise, temperature |
Stroke Volume | Increase/Decrease | Preload, contractility, afterload |
Preload | Increase | Venous return, Frank-Starling law |
Contractility | Increase | SNS, Ca++ influx |
Afterload | Decrease | Arterial pressure, hypertension |
Hormones | Increase | Epinephrine, thyroxine |
