 Back
BackCardiovascular Physiology: Structure, Function, and Regulation
Study Guide - Smart Notes

Cardiovascular Physiology
Functions of the Cardiovascular System
The cardiovascular system is essential for maintaining homeostasis by transporting materials throughout the body, facilitating cell-to-cell communication, supporting immune responses, and regulating body temperature.
Transport of Materials: Includes oxygen, nutrients, hormones, metabolic wastes, and immune cells.
Cell-to-Cell Communication: Hormones and signaling molecules are distributed via the blood.
Immune Responses: Immune cells circulate to detect and respond to pathogens.
Thermoregulation: Blood flow adjusts to regulate heat distribution.
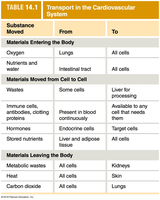
Substance Moved | From | To |
|---|---|---|
Oxygen | Lungs | All cells |
Nutrients and water | Intestinal tract | All cells |
Wastes | Some cells | Liver for processing |
Immune cells, antibodies, clotting proteins | Present in blood continuously | Available to any cell that needs them |
Hormones | Endocrine cells | Target cells |
Stored nutrients | Liver and adipose tissue | All cells |
Metabolic wastes | All cells | Kidneys |
Heat | All cells | Skin |
Carbon dioxide | All cells | Lungs |
Organization of the Cardiovascular System
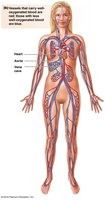
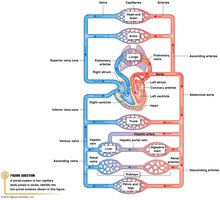
The cardiovascular system consists of the heart and blood vessels, which are organized into two main circuits: systemic and pulmonary. Blood flows in a closed loop, starting and ending at the aorta.
Heart: Pumps blood through vessels.
Arteries: Carry blood away from the heart.
Veins: Return blood to the heart.
Capillaries: Sites of exchange between blood and tissues.
Blood Flow, Pressure, and Resistance
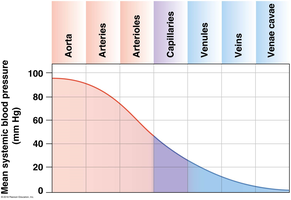
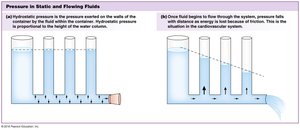
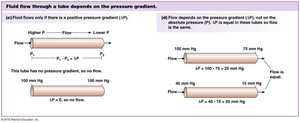
Blood flow is driven by pressure gradients and opposed by resistance. The relationship among these factors is described by several key equations and principles.
Pressure Gradient (ΔP): Drives blood flow from high to low pressure.
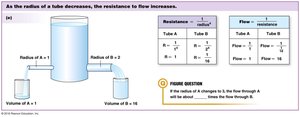
Resistance (R): Opposes flow; determined by vessel length, viscosity, and radius.
Flow (Q): Proportional to ΔP and inversely proportional to R.
Velocity of Flow (v): Depends on flow rate and vessel cross-sectional area.




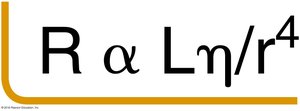


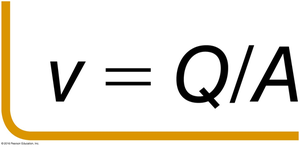
Key Equations:
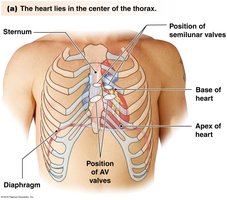
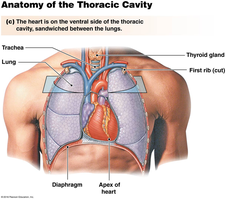
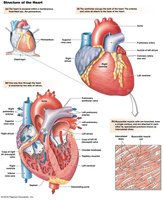
Internal and External Anatomy of the Heart
The heart is a hollow, muscular organ located in the thoracic cavity. It has three layers: epicardium, myocardium, and endocardium. The heart's structure ensures efficient blood flow and separation of oxygenated and deoxygenated blood.
Epicardium: Outer layer.
Myocardium: Muscular middle layer responsible for contraction.
Endocardium: Inner lining.
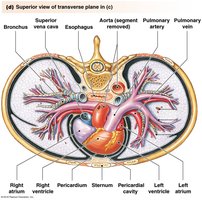
Major Blood Vessels and Blood Flow Pathways
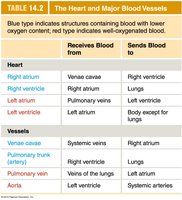
Blood flows through a series of vessels, with the heart acting as a central pump. The organization of the heart and major vessels ensures proper oxygenation and distribution of blood.
Structure | Receives Blood From | Sends Blood To |
|---|---|---|
Right atrium | Venae cavae | Right ventricle |
Right ventricle | Right atrium | Lungs |
Left atrium | Pulmonary vein | Left ventricle |
Left ventricle | Left atrium | Body except for lungs |
Venae cavae | Systemic veins | Right atrium |
Pulmonary trunk (artery) | Right ventricle | Lungs |
Pulmonary vein | Veins of the lungs | Left atrium |
Aorta | Left ventricle | Systemic arteries |

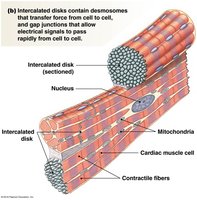
Myocardial Cells: Autorhythmic vs. Contractile
The heart contains two types of myocardial cells: autorhythmic (pacemaker) cells and contractile cells. Their arrangement and function are critical for coordinated heart contractions.
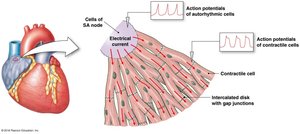
Autorhythmic Cells: Generate action potentials spontaneously; lack a stable resting membrane potential.
Contractile Cells: Responsible for forceful contractions; have prolonged action potentials to prevent summation.
Intercalated Disks: Specialized junctions for rapid electrical signal transmission.
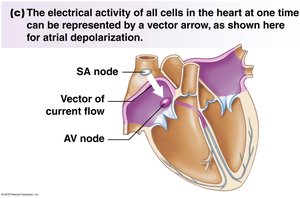
Electrical Conduction and Action Potentials
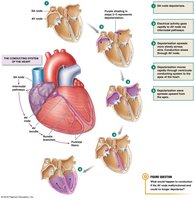
Electrical signals originate in the SA node and propagate through the heart, triggering coordinated contractions. The conduction system includes the SA node, AV node, bundle of His, and Purkinje fibers.
SA Node: Primary pacemaker.
AV Node: Delays signal to allow atrial contraction.
Bundle of His and Purkinje Fibers: Rapidly distribute the signal to ventricles.
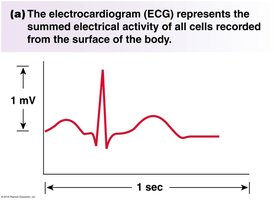
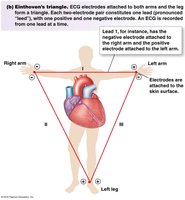
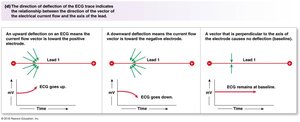
Electrocardiogram (ECG) and Cardiac Cycle
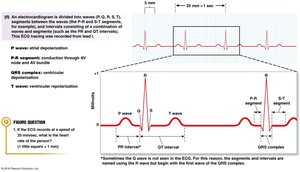
An ECG records the summed electrical activity of the heart. The waves and segments correspond to specific mechanical events in the cardiac cycle.
P wave: Atrial depolarization.
QRS complex: Ventricular depolarization.
T wave: Ventricular repolarization.

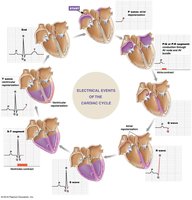
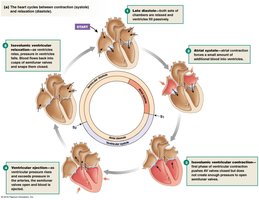
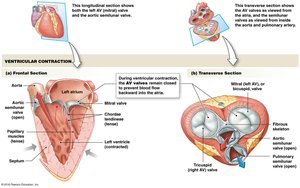
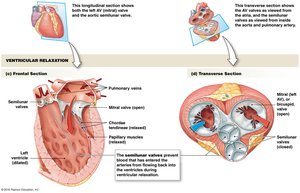
Pressure Changes and Flow During the Cardiac Cycle
Pressure changes in the heart drive blood flow through the chambers and into the vessels. The cardiac cycle includes systole (contraction) and diastole (relaxation).
Systole: Ventricular contraction ejects blood.
Diastole: Chambers relax and fill with blood.
Wiggers Diagram: Illustrates the relationship between electrical, pressure, and volume changes.
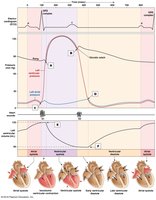
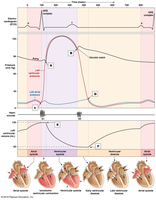
Heart Rate, Stroke Volume, and Cardiac Output
Cardiac output is the volume of blood pumped by the heart per minute, determined by heart rate and stroke volume.
Stroke Volume (SV): Difference between end-diastolic volume (EDV) and end-systolic volume (ESV).
Cardiac Output (CO): Product of heart rate (HR) and stroke volume.
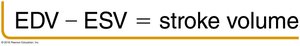



Autonomic Regulation of Heart Rate
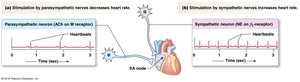
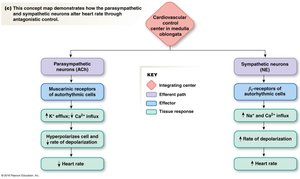
The autonomic nervous system (ANS) regulates heart rate and contractility. The parasympathetic division decreases heart rate, while the sympathetic division increases both heart rate and contractility.
Parasympathetic (PNS): Negative chronotropic effect; affects only heart rate.
Sympathetic (SNS): Positive chronotropic and inotropic effects; affects heart rate and contractility.
Factors Influencing Stroke Volume
Stroke volume is influenced by venous return, myocardial stretch (preload), arterial resistance (afterload), contractility, and mechanisms such as the skeletal muscle pump and respiratory pump.
Venous Return: Amount of blood returning to the heart.
Preload: Degree of stretch before contraction.
Afterload: Resistance the heart must overcome to eject blood.
Contractility: Force of contraction at a given preload.
Skeletal Muscle Pump: Muscle contractions help return blood to the heart.
Respiratory Pump: Breathing movements facilitate venous return.
Inotropic Agents: Substances that affect contractility.
Frank-Starling Law: The force of contraction is directly proportional to the initial length of the cardiac muscle fibers (sarcomeres).
Additional info: The Frank-Starling mechanism ensures that the heart pumps out all the blood returned to it, maintaining balance between venous return and cardiac output.
----------------------------------------
