 Back
BackCardiovascular System Disorders: Structure, Function, and Pathology
Study Guide - Smart Notes

Cardiovascular System: Structure and Function
Overview of the Circulatory System
The circulatory system is responsible for transporting blood, nutrients, gases, and wastes throughout the body. It consists of the heart (the pump), blood vessels (arteries, veins, capillaries), and blood (the fluid).
Systemic circulation: Delivers oxygenated blood from the heart to the body and returns deoxygenated blood back to the heart.
Pulmonary circulation: Carries deoxygenated blood from the heart to the lungs and returns oxygenated blood to the heart.
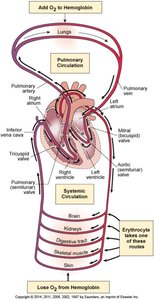
Heart Anatomy
The heart is a muscular organ located in the mediastinum, within the pericardial sac. It is composed of several layers and contains four chambers separated by valves to ensure unidirectional blood flow.
Layers: Parietal pericardium, epicardium (visceral pericardium), myocardium, endocardium
Valves: Atrioventricular (tricuspid and mitral) and semilunar (aortic and pulmonary)
Septum: Divides the right and left sides of the heart
Heart Conduction System
The heart's rhythmic contractions are coordinated by its conduction system, which generates and transmits electrical impulses.
Sinoatrial (SA) node: Pacemaker, initiates sinus rhythm
Atrioventricular (AV) node: Delays impulse, located in the right atrium
AV bundle (bundle of His): Transmits impulses to ventricles
Purkinje fibers: Distribute impulse through ventricles
Electrocardiogram (ECG): Records electrical activity (P wave: atrial depolarization, QRS: ventricular depolarization, T wave: ventricular repolarization)
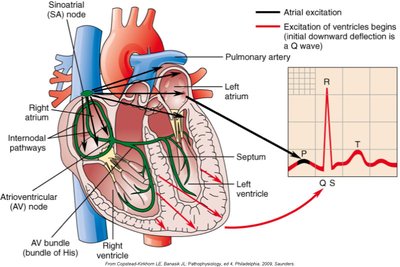
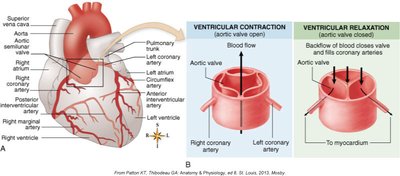
Coronary Circulation
The coronary arteries supply oxygenated blood to the myocardium. The right and left coronary arteries branch from the aorta and further divide to supply the heart muscle.
Left coronary artery: Divides into left anterior descending and circumflex arteries
Right coronary artery: Branches into right marginal and posterior interventricular arteries
Collateral circulation is limited, making blockages dangerous
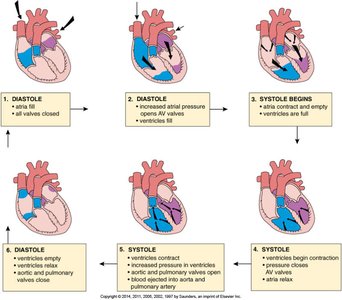
Cardiac Cycle
The cardiac cycle describes the sequence of events in one heartbeat, including periods of relaxation (diastole) and contraction (systole).
Diastole: Myocardium relaxes, chambers fill with blood
Systole: Myocardium contracts, blood is ejected
Valves open and close to direct blood flow
Cardiac Output and Regulation
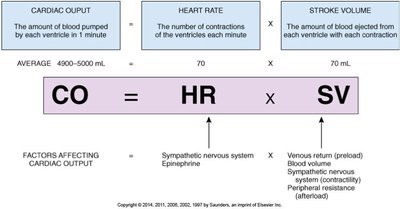
Cardiac output (CO) is the volume of blood ejected by a ventricle per minute. It is determined by heart rate (HR) and stroke volume (SV):
CO = HR × SV
Preload: Volume of blood returning to the heart
Afterload: Resistance the heart must overcome to eject blood
Factors affecting cardiac output include sympathetic stimulation, venous return, and peripheral resistance.
Cardiovascular Pathology
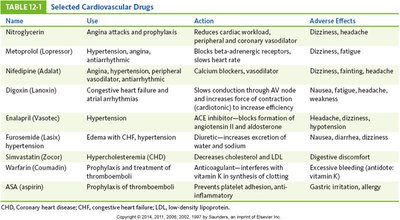
Selected Cardiovascular Drugs
Various drugs are used to manage cardiovascular disorders, each with specific actions and adverse effects.
Name | Use | Action | Adverse Effects |
|---|---|---|---|
Nitroglycerin | Angina attacks and prophylaxis | Reduces cardiac workload, peripheral and coronary vasodilator | Dizziness, headache |
Metoprolol | Hypertension, angina, antidysrhythmic | Beta blocker, slows heart rate | Dizziness, fatigue |
Nifedipine | Angina, hypertension, peripheral vasodilator, antianginal | Calcium blocker, vasodilator | Dizziness, fainting, headache |
Digoxin | Congestive heart failure and atrial dysrhythmias | Slows AV node conduction, increases force of contraction | Nausea, fatigue, headache |
Enalapril | Hypertension | ACE inhibitor, blocks formation of angiotensin II | Headache, dizziness |
Furosemide | Edema with CHF, hypertension | Diuretic, increases excretion of sodium and water | Nausea, diarrhea, dizziness |
Simvastatin | Hypercholesterolemia (CHD) | Decreases cholesterol and LDL | Digestive discomfort |
Warfarin | Prophylaxis and treatment of thromboemboli | Anticoagulant, interferes with vitamin K | Excessive bleeding |
ASA (aspirin) | Prophylaxis of thromboemboli, anti-inflammatory | Prevents platelet adhesion, anti-inflammatory | Gastric irritation, allergy |
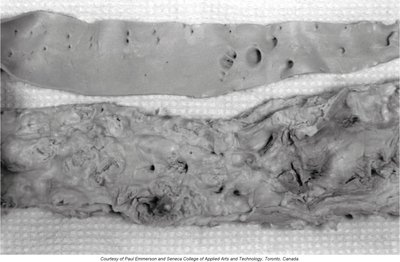
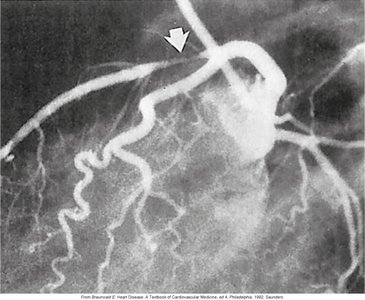
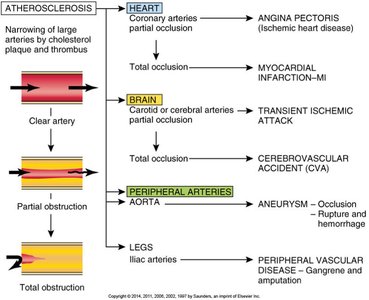
Arteriosclerosis and Atherosclerosis
Arteriosclerosis is a general term for arterial wall thickening and loss of elasticity, leading to narrowed lumens and increased blood pressure. Atherosclerosis is a specific type involving the formation of atheromas (plaques) composed of lipids, calcium, and clots in large arteries.
Major risk factors: Age, gender, genetics, obesity, sedentary lifestyle, smoking, diabetes, hypertension
Complications: Ischemic heart disease, myocardial infarction, stroke, peripheral vascular disease
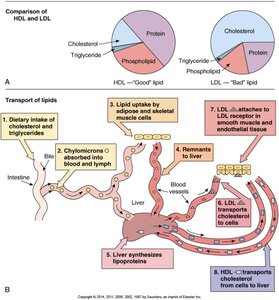
Lipid Transport
Lipids are transported in the blood as lipoproteins:
Low-density lipoprotein (LDL): Transports cholesterol from liver to cells; contributes to atheroma formation
High-density lipoprotein (HDL): Transports cholesterol from cells to liver for excretion; considered "good" cholesterol
Atherosclerosis: Diagnosis and Treatment
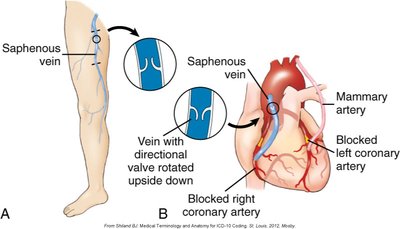
Diagnosis is based on serum lipid levels and imaging studies. Treatment includes lifestyle modifications, medications, and surgical interventions such as coronary artery bypass grafting.
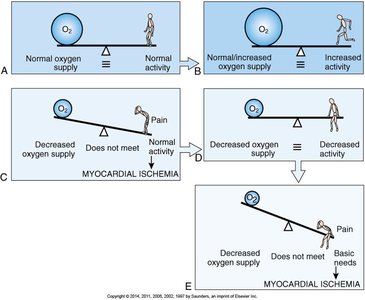
Angina Pectoris and Myocardial Infarction
Angina pectoris is chest pain due to myocardial ischemia (oxygen supply-demand imbalance). Myocardial infarction (MI) occurs when a coronary artery is totally obstructed, leading to tissue necrosis.
Types of angina: Classic (exertional), variant (vasospasm), unstable (prolonged, at rest)
MI warning signs: Chest pressure, shortness of breath, nausea, anxiety, pain radiating to arm/jaw
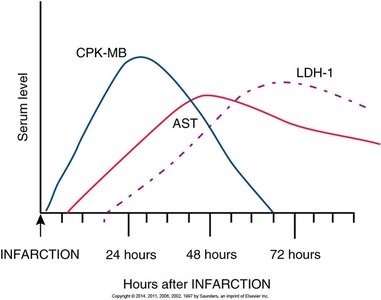
Diagnosis: ECG changes, elevated cardiac enzymes (CK, AST, LDH), troponin
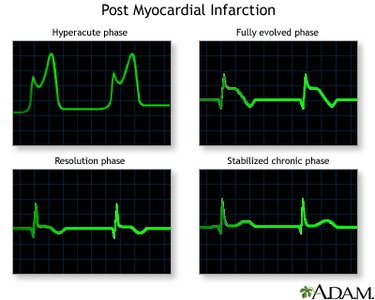
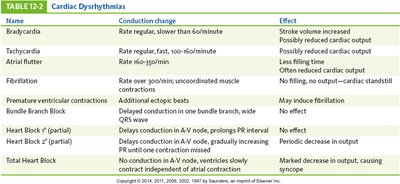
Cardiac Dysrhythmias (Arrhythmias)
Dysrhythmias are abnormal heart rhythms caused by conduction disturbances. They can reduce cardiac output and may be life-threatening.
Sinus node abnormalities: Bradycardia, tachycardia, sick sinus syndrome
Atrial conduction: Premature atrial contractions, atrial flutter, atrial fibrillation
AV node: Heart blocks (first, second, third degree)
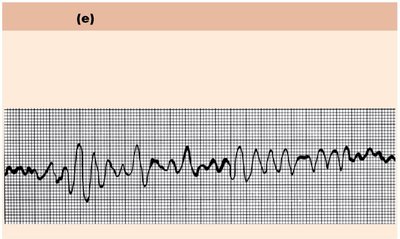
Ventricular: Bundle branch block, ventricular tachycardia, ventricular fibrillation, PVCs
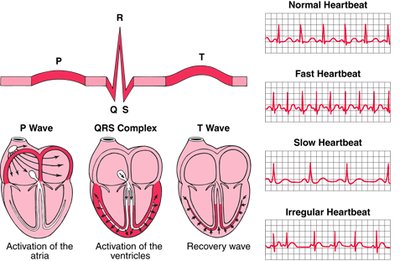
Name | Conduction Change | Effect |
|---|---|---|
Bradycardia | Rate regular, slower than 60/min | Stroke volume increased |
Tachycardia | Rate regular, fast, 100–160/min | Possibly reduced cardiac output |
Atrial flutter | Rate 160–350/min | AV node delays conduction |
Fibrillation | Uncoordinated muscle contractions | No filling, output—cardiac standstill |
Premature ventricular contractions | Additional ectopic beats | May induce fibrillation |
Bundle branch block | Delayed conduction in one bundle branch | Wide QRS wave |
Heart Block I | Delays conduction in AV node | Prolongs PR interval |
Heart Block II | Delays conduction in AV node, gradually increasing PR until one contraction missed | Periodic decrease in output |
Total Heart Block | No conduction in AV node, ventricles slowly contract independent of atrial contraction | Marked decrease in output, causing syncope |
Congestive Heart Failure (CHF)
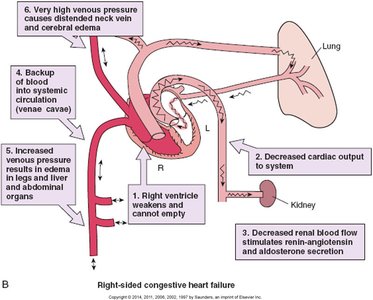
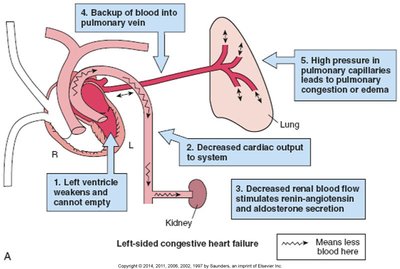
CHF occurs when the heart cannot pump enough blood to meet the body's needs. It may affect the left, right, or both sides of the heart, leading to systemic and pulmonary congestion.
Left-sided failure: Pulmonary congestion, dyspnea, orthopnea
Right-sided failure: Systemic congestion, edema in legs, hepatomegaly
Compensatory mechanisms may worsen the condition
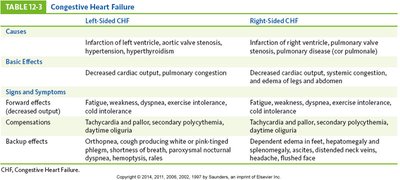
Left-Sided CHF | Right-Sided CHF | |
|---|---|---|
Causes | Infarction of left ventricle, aortic valve stenosis, hypertension, hyperthyroidism | Infarction of right ventricle, pulmonary valve stenosis, pulmonary disease (cor pulmonale) |
Basic Effects | Decreased cardiac output, pulmonary congestion | Decreased cardiac output, systemic congestion, edema of legs and abdomen |
Signs and Symptoms | Fatigue, weakness, dyspnea, exercise intolerance, cold intolerance, tachycardia, pallor, secondary polycythemia, daytime oliguria, orthopnea, cough, paroxysmal nocturnal dyspnea, hemoptysis | Fatigue, weakness, dyspnea, exercise intolerance, cold intolerance, tachycardia, pallor, secondary polycythemia, daytime oliguria, dependent edema in feet, hepatomegaly, splenomegaly, ascites, distended neck veins, flushed face |
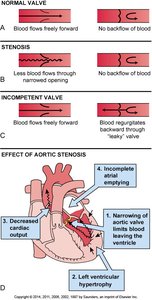
Valvular Defects
Valvular defects affect the heart's ability to maintain unidirectional blood flow. They are classified as:
Stenosis: Narrowed valve opening, impeding blood flow
Incompetence: Failure to close completely, causing regurgitation
Mitral valve prolapse: Floppy valve leaflets
Treatment may involve surgical replacement with mechanical or biological valves
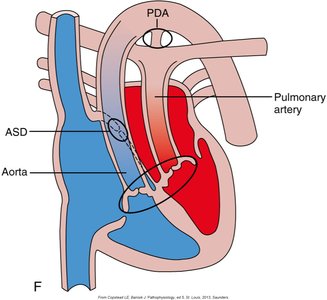
Congenital Heart Disease: Tetralogy of Fallot
Tetralogy of Fallot is the most common cyanotic congenital heart defect, involving four abnormalities:
Ventricular septal defect (VSD)
Dextroposition of the aorta
Right ventricular hypertrophy
Pulmonary stenosis
It causes right-to-left shunt, cyanosis, and altered blood flow. Diagnosis is by imaging and surgical repair is often required.
Vascular Disorders
Hypertension
Hypertension is persistently elevated blood pressure, classified as primary (essential), secondary, or malignant. It increases the risk of damage to the kidneys, heart, brain, and retina.
Primary: BP consistently above 140/90 mm Hg
Secondary: Due to renal or endocrine disease
Malignant: Severe, rapidly progressive
Treatment: Lifestyle changes, medications (diuretics, ACE inhibitors)
Aortic Aneurysm
An aortic aneurysm is a localized dilation and weakening of the arterial wall, which may be saccular, fusiform, or dissecting. Risk of rupture and hemorrhage is high.
Causes: Atherosclerosis, trauma, infection, congenital defects
Diagnosis: Imaging (ultrasound, CT, MRI)
Treatment: Blood pressure control, surgical repair
Venous Disorders
Varicose veins are dilated, tortuous superficial veins, often in the legs. Thrombophlebitis and phlebothrombosis involve clot formation in veins, with risk of pulmonary embolism.
Risk factors: Family history, obesity, pregnancy, prolonged standing
Treatment: Leg elevation, compression stockings, anticoagulants, surgery
Shock
Shock is a critical condition where blood pressure drops, leading to inadequate tissue perfusion and cellular hypoxia. Types include hypovolemic, cardiogenic, and distributive shock.
Symptoms: Anxiety, tachycardia, pallor, light-headedness, syncope, sweating, oliguria
Compensatory mechanisms: Increased heart rate, vasoconstriction, hormone secretion
Complications: Renal failure, respiratory distress, hepatic failure, DIC, cardiac depression
Additional info: This guide covers the essential structure, function, and pathology of the cardiovascular system, including major diseases, diagnostic methods, and treatments, as relevant to college-level anatomy and physiology.
