 Back
BackCellular Immune Response and Disorders of Immunity
Study Guide - Smart Notes

The Immune System: Innate and Adaptive Body Defenses
Cellular Immune Response
The cellular immune response is a critical component of adaptive immunity, primarily mediated by T cells. T cells defend against intracellular antigens, such as cells infected with viruses or bacteria, cancerous cells, and foreign transplanted cells. Some T cells directly kill infected cells, while others regulate the immune response through chemical signals.
T cells are more complex than B cells in both classification and function.
Two main populations: CD4 cells (helper T cells, regulatory T cells, memory T cells) and CD8 cells (cytotoxic T cells, memory T cells).
Helper, cytotoxic, and regulatory T cells are activated T cells; naive T cells are simply termed CD4 or CD8 cells.
CD4 cells activate B cells, other T cells, and macrophages; CD8 cells destroy cells harboring foreign antigens.
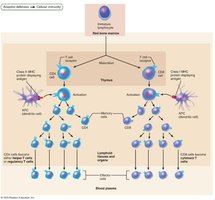
MHC Proteins and Antigen Presentation
T cells respond only to processed fragments of antigens displayed on cell surfaces by major histocompatibility complex (MHC) proteins. Antigen presentation is essential for activation of naive T cells and normal functioning of effector T cells.
Two classes of MHC proteins: Class I (displayed by all cells except RBCs) and Class II (displayed by antigen-presenting cells: dendritic cells, macrophages, B cells).
Class I MHC proteins bind short fragments of endogenous antigens (self or nonself proteins synthesized inside the cell).
Class II MHC proteins bind longer fragments of exogenous antigens (extracellular, engulfed and broken down by APCs).
CD8 cells are activated by Class I MHC; CD4 cells are activated by Class II MHC.
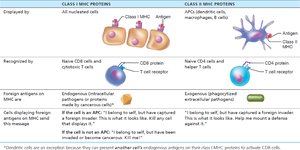
MHC Restriction
CD4 and CD8 cells have different requirements for MHC protein presentation:
CD4 cells (helper T cells) bind only to Class II MHC proteins on APC surfaces.
CD8 cells (cytotoxic T cells) bind only to Class I MHC proteins found on all cell surfaces.
Dendritic cells can display both endogenous and exogenous antigens to activate CD8 cells.
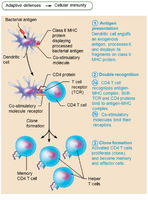
Activation and Differentiation of T Cells
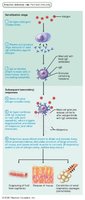
T cell activation requires antigen presentation and co-stimulation, both occurring on the surface of the same APC. This two-step process ensures clonal selection and prevents unwanted activation.
Step 1: Antigen binding – T cell receptors (TCRs) bind to antigen-MHC complex on APC surface, requiring double recognition of both MHC and foreign antigen.
Step 2: Co-stimulation – T cell must also bind to co-stimulatory signals on APC surface. Without co-stimulation, T cells become tolerant, unable to divide, and do not secrete cytokines (anergy).
Activated T cells proliferate and differentiate in response to cytokines, peaking within a week. Apoptosis occurs between days 7 and 30 to prevent excessive inflammation.
Memory T cells remain to mediate secondary responses.
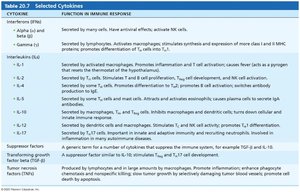
Cytokines
Cytokines are chemical messengers that mediate cell development, differentiation, and immune responses. They include interferons and interleukins.
Interleukin 1 (IL-1) is released by macrophages and stimulates T cells to release interleukin 2 (IL-2) and synthesize more IL-2 receptors.
IL-2 is a key growth factor, encouraging activated T cells to divide rapidly.
Other cytokines amplify and regulate innate and adaptive responses (e.g., gamma interferon enhances macrophage killing power).
Roles of Specific Effector T Cells
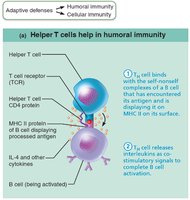
Helper T (TH) Cells
Helper T cells play a central role in adaptive immunity, activating both humoral and cellular arms. Once primed by APC presentation, they help activate B cells and other T cells, induce proliferation, and secrete cytokines to recruit other immune cells.
Without helper T cells, there is no immune response.
Most antigens are T cell–dependent and require TH co-stimulation for B cell activation.
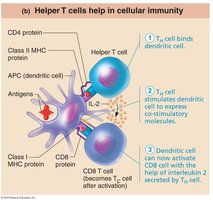
Activation of CD8 Cells
CD8 cells require helper T cells to become activated into cytotoxic T cells. Helper T cells stimulate dendritic cells to express co-stimulatory molecules required for CD8 cell activation.
Amplification of Innate Defenses
Helper T cells amplify innate immune responses by activating macrophages and mobilizing lymphocytes and other white blood cells.
Subsets of Helper T Cells
TH1 – mediates most aspects of cellular immunity.
TH2 – defends against parasitic worms, mobilizes eosinophils, promotes humoral immunity and allergies.
TH17 – links adaptive and innate immunity by releasing IL-17; may play a role in autoimmune disease.
Cytotoxic T (TC) Cells
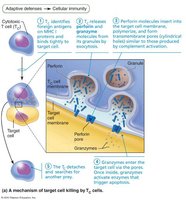
Cytotoxic T cells directly attack and kill infected, cancerous, or foreign cells. They circulate in blood, lymph, and lymphoid organs searching for cells displaying recognized antigens.
TC cells deliver lethal hits using two mechanisms: release of perforins and granzymes (stimulating apoptosis), or binding to membrane receptors to induce apoptosis.
Natural Killer (NK) Cells
NK cells recognize abnormality signs not detected by cytotoxic T cells, such as lack of MHC proteins or antibodies coating target cells. NK cells use similar mechanisms as TC cells for killing.
Regulatory T (TReg) Cells
Regulatory T cells dampen immune response by direct contact or by secreting inhibitory cytokines (e.g., IL-10, TGF-β). They are important in preventing autoimmune reactions and suppress self-reactive lymphocytes.
Organ Transplants and Prevention of Rejection
Allografts and Immunosuppression
Allografts are transplants from the same species. Success depends on tissue similarity, including ABO, other blood antigens, and MHC antigens. Patients receive immunosuppressive therapy post-surgery, which increases risk of infection and mortality.
Immunodeficiencies
Types and Causes
Immunodeficiency is a congenital or acquired condition impairing immune cell function or production.
SCID syndrome is a genetic defect with marked deficit in B and T cells, often fatal without bone marrow transplant.
Hodgkin’s disease is an acquired immunodeficiency causing cancer of B cells.
AIDS is caused by HIV, which cripples the immune system by destroying helper T cells, leading to opportunistic infections and dementia.
HIV is transmitted via body fluids and uses reverse transcriptase to produce DNA from viral RNA, resulting in high mutation rates and drug resistance.
Autoimmune Diseases
Mechanisms and Examples
Autoimmune diseases occur when the immune system fails to distinguish self from foreign, producing autoantibodies and sensitized TC cells that destroy body tissues.
Examples: rheumatoid arthritis, myasthenia gravis, multiple sclerosis, Graves’ disease, type 1 diabetes mellitus, systemic lupus erythematosus, glomerulonephritis.
Treatments include immunosuppressive drugs, blocking cytokine action, and research into regulatory T cell activation.
Autoimmunity may be triggered by foreign antigens resembling self-antigens, gene mutations, hapten attachment, or trauma.
Hypersensitivities
Types and Mechanisms
Hypersensitivities are immune responses to perceived threats that cause tissue damage. They are classified by time course and whether antibodies or T cells are involved.
Immediate hypersensitivity (allergies) – begins seconds after contact with allergen; IgE binds to mast cells and basophils, causing histamine release and inflammation. Can be local or systemic (anaphylactic shock).
Subacute hypersensitivity – caused by IgM and IgG; slower onset and longer duration. Includes cytotoxic reactions (e.g., mismatched blood transfusion) and immune complex hypersensitivity (e.g., SLE).
Delayed hypersensitivity – slow onset, depends on helper T cells, cytokine-activated macrophages, and cytotoxic T cells (e.g., allergic contact dermatitis).
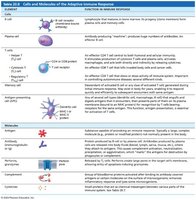
Summary Table: Key Cells and Molecules
See above tables for detailed comparisons of MHC proteins, cytokines, and adaptive immune response cells and molecules.
Additional info:
Immunodeficiencies and autoimmune diseases are major clinical concerns in transplantation and immune system disorders.
Understanding the mechanisms of T cell activation, differentiation, and effector functions is essential for clinical applications in immunology.
