 Back
BackChapter 11: The Cardiovascular System – Blood (Mini-Textbook Study Notes)
Study Guide - Smart Notes

The Cardiovascular System: Blood
Introduction to the Cardiovascular System
The cardiovascular system is the body's internal transport network, consisting of the heart, blood, and blood vessels. Blood is essential for transporting nutrients, gases, waste products, and chemical messengers throughout the body. It is the first organ system to become fully operational during embryonic development.
Major components: Heart, blood, blood vessels
Primary functions of blood:
Transport of dissolved gases, nutrients, hormones, and metabolic wastes
Regulation of interstitial fluid pH and ion composition
Restriction of fluid loss at injury sites
Defense against toxins and pathogens
Stabilization of body temperature
Composition and Physical Characteristics of Blood
Blood Composition
Blood is a specialized connective tissue composed of plasma (liquid matrix) and formed elements (cells and cell fragments).
Plasma: Makes up about 55% of blood volume; contains water, plasma proteins, and other solutes.
Formed elements: Make up about 45% of blood volume; include red blood cells (RBCs), white blood cells (WBCs), and platelets.
Blood volume: Adult males: 5–6 L; Adult females: 4–5 L
Physical Characteristics of Blood
Temperature: 38°C (slightly above body temperature)
Viscosity: Five times more viscous than water due to plasma proteins and formed elements
pH: Slightly alkaline (7.35–7.45)
Type: Connective tissue
Blood Collection and Analysis
Venipuncture: Common method for collecting blood, usually from the median cubital vein
Capillary collection: From fingertip or earlobe for blood smears
Arterial puncture: Used to evaluate gas exchange at the lungs
Plasma and Plasma Proteins
Composition of Plasma
Plasma, along with interstitial fluid, forms most of the extracellular fluid in the body. It is composed of:
Water: 92%
Plasma proteins: 7%
Other solutes: 1% (hormones, nutrients, gases)
Major Types of Plasma Proteins
Albumins: ~60%; maintain osmotic pressure
Globulins: ~35%; transport proteins and antibodies (immunoglobulins)
Fibrinogen: ~4%; functions in blood clotting as precursor to fibrin
Most plasma proteins are synthesized by the liver, except antibodies (produced by lymphocytes).
Other Solutes in Plasma
Organic nutrients: Lipids, carbohydrates, amino acids, vitamins
Electrolytes: Na+, K+, Ca2+, Mg2+, Cl-, HCO3-, etc.
Organic wastes: Urea, uric acid, creatinine, bilirubin, ammonium ions
Red Blood Cells (Erythrocytes)
Structure and Function
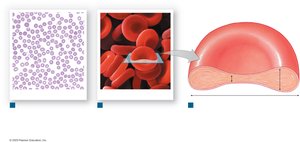
Red blood cells (RBCs) are specialized for oxygen and carbon dioxide transport. They account for 99.9% of formed elements and contain the pigment hemoglobin.
Biconcave shape: Increases surface area for gas exchange and flexibility for capillary passage
Lack organelles: No nucleus or mitochondria; rely on anaerobic metabolism
Hemoglobin Structure and Function
Structure: Four globular protein subunits, each with a heme group containing iron
Oxygen transport: O2 binds to heme; CO2 binds to globin
Oxygen loading/unloading: High plasma O2 promotes loading (lungs); low plasma O2 and high CO2 promote unloading (tissues)
Red Blood Cell Life Cycle and Recycling
Lifespan: ~120 days; cannot repair themselves
Recycling: Macrophages in liver, spleen, and bone marrow engulf old RBCs; hemoglobin is broken down and components recycled
Hemoglobin breakdown: Heme → biliverdin → bilirubin (excreted in bile); iron is stored or transported by transferrin
Jaundice: Excess bilirubin causes yellowing of skin and eyes
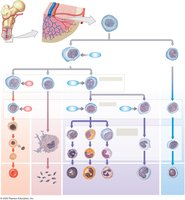
Erythropoiesis (RBC Formation)
Site: Red bone marrow in adults; yolk sac in embryo
Requirements: Amino acids, iron, vitamin B12 (requires intrinsic factor for absorption)
Stages: Hemocytoblast → myeloid stem cell → erythroblast → reticulocyte → erythrocyte
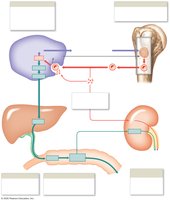
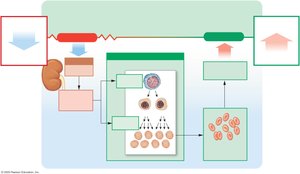
Regulation of Erythropoiesis
Stimulus: Hypoxia (low tissue oxygen)
Hormone: Erythropoietin (EPO) released by kidneys; stimulates RBC production in bone marrow
Clinical relevance: EPO used in anemia treatment and blood doping
Blood Types and Transfusions
ABO and Rh Blood Groups
Antigens: Surface markers on RBCs (A, B, Rh)
Antibodies: Found in plasma; attack foreign antigens
Blood types: A, B, AB, O; each can be Rh+ or Rh-
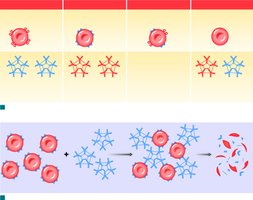
Transfusion Reactions
Cross-reaction: Occurs if antibodies attack donor RBC antigens, causing agglutination and hemolysis
Blood compatibility testing: Mixing blood with anti-A, anti-B, and anti-Rh antibodies to determine type
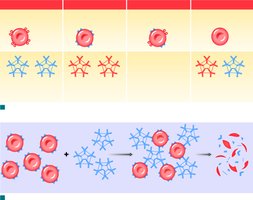
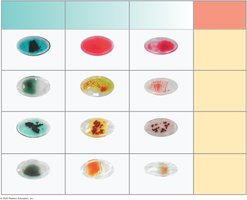
Universal Donors and Recipients
Universal donor: Type O- (no A, B, or Rh antigens)
Universal recipient: Type AB+ (no anti-A, anti-B, or anti-Rh antibodies)
White Blood Cells (Leukocytes)
Types and Functions
White blood cells defend the body against pathogens, remove toxins, and clean up damaged cells. They are classified as granulocytes or agranulocytes.
Granulocytes: Neutrophils, eosinophils, basophils
Agranulocytes: Lymphocytes, monocytes
Characteristics of WBCs
Amoeboid movement
Diapedesis (migration out of bloodstream)
Positive chemotaxis (movement toward chemical signals)
Phagocytosis (neutrophils, eosinophils, monocytes)
Types of White Blood Cells
Neutrophils: 50–70%; first responders, phagocytize bacteria
Eosinophils: 2–4%; attack parasites, involved in allergic reactions
Basophils: <1%; release histamine and heparin, enhance inflammation
Monocytes: 2–8%; become macrophages, aggressive phagocytes
Lymphocytes: 20–40%; specific immunity, produce antibodies
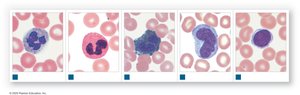
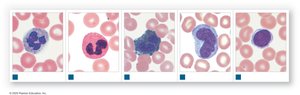
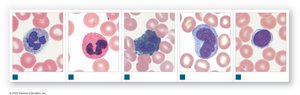
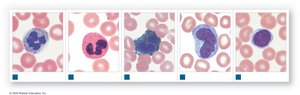
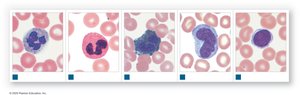
Differential WBC Count
Measures the percentage of each type of WBC in a blood sample
Leukopenia: Low WBC count
Leukocytosis: High WBC count
Leukemia: Cancer of blood-forming tissues, abnormal WBCs
WBC Formation
Originate from hemocytoblasts in red bone marrow
Lymphoid stem cells → lymphocytes (regulated by thymosins, antigens)
Myeloid stem cells → other formed elements (regulated by colony-stimulating factors, CSFs)
Platelets and Hemostasis
Platelets (Thrombocytes)
Cell fragments derived from megakaryocytes
Initiate clotting and help close injured blood vessels
Circulate for 9–12 days; normal count: 150,000–500,000/μL
Thrombocytopenia: Low platelet count; Thrombocytosis: High count
Hemostasis: Stopping Blood Loss
Hemostasis is the process of stopping bleeding and involves three phases:
Vascular phase: Vascular spasm constricts vessel, endothelium becomes sticky
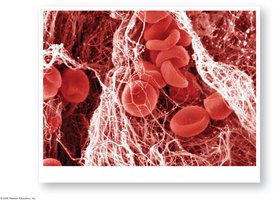
Platelet phase: Platelets adhere to exposed collagen and each other, forming a plug
Coagulation phase: Cascade of reactions converts fibrinogen to fibrin, forming a clot
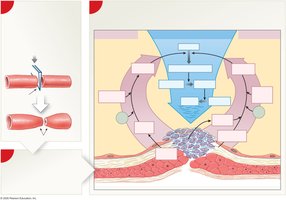
Clotting Pathways
Extrinsic pathway: Initiated by tissue factor from damaged tissues; rapid
Intrinsic pathway: Initiated by exposure of blood to collagen; slower
Common pathway: Both pathways activate Factor X, leading to conversion of prothrombin to thrombin, and fibrinogen to fibrin
Key factors: Calcium ions (Ca2+) and vitamin K are essential for clotting. Deficiency in either impairs the process.
Clot Retraction and Removal
Platelets contract, pulling vessel edges together (clot retraction)
Clot is dissolved by fibrinolysis (plasminogen → plasmin, which digests fibrin)
Summary Table: Major Formed Elements of Blood
Formed Element | Main Function | Relative Abundance |
|---|---|---|
Red Blood Cells (Erythrocytes) | Transport O2 and CO2 | ~99.9% of formed elements |
White Blood Cells (Leukocytes) | Defense against pathogens | ~0.1% of formed elements |
Platelets (Thrombocytes) | Clotting, vessel repair | ~0.1% of formed elements |
Key Equations and Concepts
Hematocrit (%):
Oxygen transport:
Coagulation cascade:
Additional info: These notes provide a comprehensive overview of blood as a component of the cardiovascular system, suitable for ANP college students preparing for exams or seeking a concise reference.
