 Back
BackChapter 18: Blood Vessels – Structure, Function, and Hemodynamics
Study Guide - Smart Notes

Blood Vessels: Structure and Function
Overview of Blood Vessels
Blood vessels form a closed system that transports blood throughout the body. They are classified into arteries, veins, and capillaries, each with distinct structural and functional characteristics.
Arteries: Carry blood away from the heart.
Capillaries: Sites of exchange with body tissues.
Veins: Collect and return blood to the heart.
Hemodynamics: Refers to the regulation of blood flow and blood pressure.
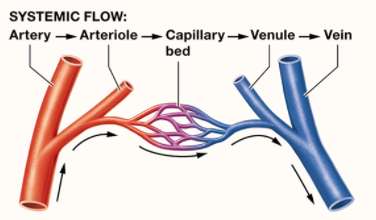
Blood Vessel Anatomy
Blood vessels share a basic structure but differ in the thickness and composition of their layers:
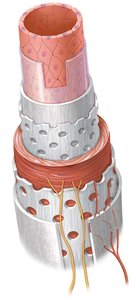
Tunica intima (interna): Innermost layer, composed of endothelium and basement membrane; may include an internal elastic lamina.
Tunica media: Middle layer, primarily smooth muscle; may contain an external elastic lamina.
Tunica adventitia (externa): Outermost layer, consisting of collagen and elastic fibers, with blood (vasa vasorum) and nerve supply.
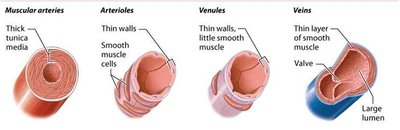
Types of Blood Vessels
Elastic arteries: Large arteries with abundant elastic fibers in the tunica media; recoil helps maintain blood pressure.
Muscular arteries: More smooth muscle in the tunica media; regulate blood flow via vasoconstriction and vasodilation.
Arterioles: Smallest arteries; control blood flow into capillaries.
Venules: Formed when capillaries unite; smallest have only endothelium and basement membrane, larger ones have some smooth muscle.
Veins: Thin tunica intima and media, thick adventitia, contain valves to prevent backflow.
Hemodynamics: Blood Flow and Pressure
Blood Pressure and Its Measurement
Blood pressure (BP) is the force exerted by circulating blood on the walls of blood vessels, measured in mm Hg. It is a key factor in tissue perfusion and is regulated by cardiac output, blood volume, and peripheral resistance.
Pulse pressure: Difference between systolic and diastolic pressure.
Mean arterial pressure (MAP): Average pressure in the arteries, calculated as:
Determinants of Blood Pressure
Cardiac Output (CO): Volume of blood pumped by the heart per minute.
Total Blood Volume: Increased volume raises BP.
Systemic Vascular Resistance (SVR): Opposition to blood flow due to friction between blood and vessel walls; affected by vessel diameter, blood viscosity, vessel length, and obstructions.
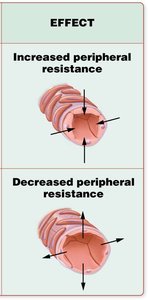
Peripheral Resistance
Peripheral resistance is primarily determined by the diameter of arterioles. Vasoconstriction increases resistance and BP, while vasodilation decreases resistance and BP.
Blood Flow and Velocity
Blood flow is the volume of blood moving through a tissue per unit time. Velocity is inversely related to the total cross-sectional area of blood vessels; it slows in capillaries to allow exchange.
Specialized Circulatory Routes
Vascular Anastomoses
Vascular anastomoses are connections between blood vessels that provide alternate pathways (collateral vessels) for blood flow. They are important in organs like the heart, brain, and joints. Types include arterial, venous, and arteriovenous anastomoses.
Capillaries and Tissue Perfusion
Capillary Structure and Types
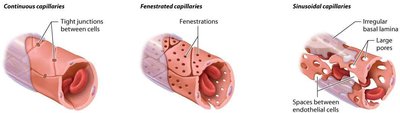
Capillaries are the smallest blood vessels, consisting of a single layer of endothelial cells and a basal lamina. Their thin walls facilitate exchange of gases, nutrients, and wastes.
Continuous capillaries: Least permeable, found in muscle and skin.
Fenestrated capillaries: Have pores, found in kidneys and intestines.
Sinusoidal capillaries: Most permeable, found in liver and bone marrow.
Capillary Exchange Mechanisms
Diffusion: Movement of substances down their concentration gradients.
Transcytosis: Vesicular transport of large, lipid-insoluble molecules.
Bulk flow: Movement of fluid driven by hydrostatic and osmotic pressure differences; regulates blood and interstitial fluid volumes.
Summary Table: Comparison of Vessel Types
Vessel Type | Wall Structure | Key Features | Main Function |
|---|---|---|---|
Elastic Artery | Thick tunica media, many elastic fibers | Pressure reservoir | Conduct blood from heart |
Muscular Artery | Thick tunica media, more smooth muscle | Vasoconstriction/dilation | Distribute blood to organs |
Arteriole | Thin wall, smooth muscle cells | Regulate flow into capillaries | Control resistance |
Capillary | Endothelium only | Thin for exchange | Exchange gases/nutrients |
Venule | Thin wall, little smooth muscle | Collect blood from capillaries | Drain capillary beds |
Vein | Thin tunica media, thick adventitia, valves | Low pressure, blood reservoir | Return blood to heart |
Clinical Application: Measuring Blood Pressure
Blood pressure is measured using a sphygmomanometer and stethoscope. The cuff is inflated to restrict blood flow, and pressure is released while listening for Korotkoff sounds:
Systolic pressure: First sound heard as blood begins to flow.
Diastolic pressure: Last sound heard as flow becomes smooth.

Summary
This chapter provides a comprehensive overview of the structure and function of blood vessels, the principles of hemodynamics, and the mechanisms that regulate blood pressure and tissue perfusion. Understanding these concepts is essential for the study of cardiovascular physiology and pathology.
