 Back
BackChapter 18: The Cardiovascular System – Blood Vessels
Study Guide - Smart Notes

The Blood Vessels: Structure and Function
Overview of the Vasculature
The vasculature is a network of billions of blood vessels responsible for transporting blood throughout the body. These vessels facilitate the exchange of gases, nutrients, and wastes, regulate blood flow, control blood pressure, and secrete various chemicals.
Arteries: Carry blood away from the heart; systemic arteries transport oxygenated blood, pulmonary arteries transport deoxygenated blood.
Veins: Return blood to the heart; systemic veins carry deoxygenated blood, pulmonary veins carry oxygenated blood.
Capillaries: Smallest vessels; site of exchange between blood and tissues.
Structure of Blood Vessel Walls
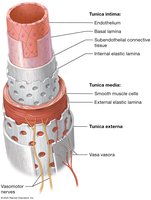
Blood vessels are composed of three main layers, or tunics, surrounding a central lumen:
Tunica Intima: Innermost layer; consists of endothelium and internal elastic lamina. Provides a smooth, frictionless surface and produces important chemicals.
Tunica Media: Middle layer; contains smooth muscle and external elastic lamina. Controls vessel diameter via vasoconstriction and vasodilation.
Tunica Externa (Adventitia): Outermost layer; dense irregular connective tissue. Contains vasa vasora, small vessels that supply the outer layers of large vessels.
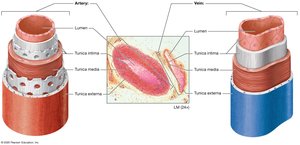
Comparison of Arteries and Veins
Arteries have thicker tunica media and more elastic fibers than veins, allowing them to withstand higher pressures. Veins have thinner walls, larger lumens, and often contain valves to prevent backflow.
Blood Distribution
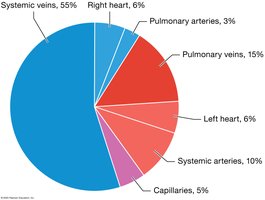
Veins serve as blood reservoirs, holding up to 70% of the total blood volume. The distribution of blood in the cardiovascular system is as follows:
Systemic veins: 55%
Pulmonary veins: 15%
Systemic arteries: 10%
Capillaries: 5%
Heart: 12% (right and left combined)
Types of Arteries and Veins
Arteries
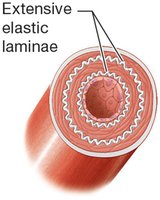
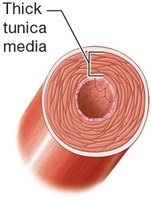
Elastic (Conducting) Arteries: Largest diameter; extensive elastic laminae; include the aorta and its branches.
Muscular (Distributing) Arteries: Intermediate diameter; well-developed tunica media; supply organs.
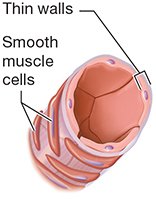
Arterioles: Smallest arteries; thin tunics; regulate blood flow to capillary beds.
Veins
Venules: Smallest veins; drain capillary beds.
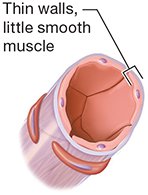
Medium Veins: Thin walls, little smooth muscle.
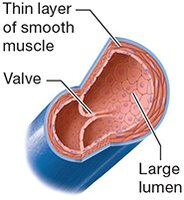
Large Veins: Thin layer of smooth muscle, large lumen, contain valves.
Atherosclerosis
Pathology and Clinical Significance
Atherosclerosis is the formation of plaques within the tunica intima of arteries, leading to vessel obstruction and increased risk of heart attack or stroke. Plaques consist of lipids, cholesterol, calcium salts, and cellular debris.

Hemodynamics: Blood Flow and Pressure
Key Concepts
Blood Pressure: The force exerted by blood on vessel walls, measured in mm Hg.
Blood Flow: Volume of blood per minute; directly proportional to pressure gradient, inversely proportional to resistance.
Resistance: Impedance to blood flow; affected by vessel radius, length, and blood viscosity.
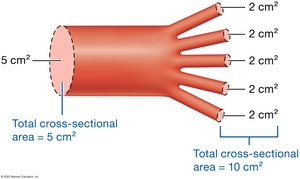
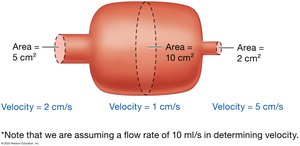
Cross-Sectional Area and Velocity
As vessels branch, total cross-sectional area increases and blood velocity decreases. Blood flows fastest in large vessels (e.g., aorta) and slowest in capillaries.
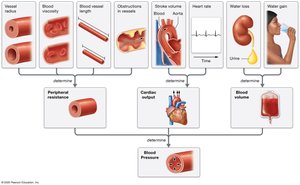
Factors Affecting Blood Pressure
Peripheral Resistance: Most resistance occurs in the periphery; inversely related to vessel radius.
Cardiac Output: Product of stroke volume and heart rate; increases blood pressure when elevated.
Blood Volume: Directly related to blood pressure; vessel compliance affects how volume changes impact pressure.
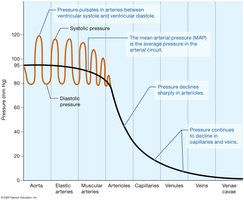
Pressure Profile in the Systemic Circuit
Pressure is highest in the aorta and declines through arteries, arterioles, capillaries, venules, and veins.
Capillary Structure and Function
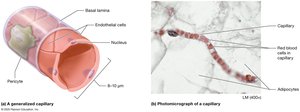
Capillary Anatomy
Capillaries are composed of a single layer of endothelial cells and a basal lamina. Pericytes surround some capillaries and help regulate blood flow.
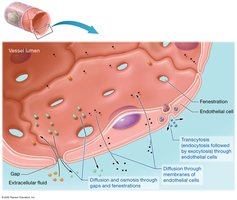
Capillary Exchange Mechanisms
Diffusion and Osmosis: Through gaps and fenestrations.
Transcytosis: Endocytosis and exocytosis for larger substances.
Diffusion through Membranes: For lipid-soluble substances.
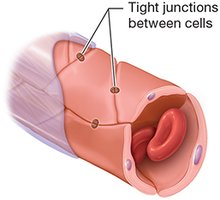
Types of Capillaries
Continuous Capillaries: Tight junctions; least leaky; found in muscle, skin, nervous tissue.
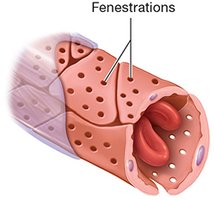
Fenestrated Capillaries: Pores for rapid diffusion; found in endocrine glands, intestines, kidneys.
Sinusoidal Capillaries: Large pores; found in liver, spleen, bone marrow.
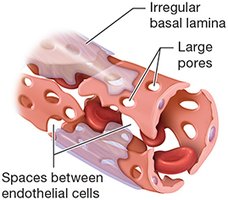
Blood Flow Through Capillary Beds
Microcirculation and Regulation
Blood flow through capillary beds is regulated by precapillary sphincters and local mechanisms (myogenic and metabolic controls).
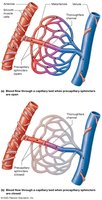
Pressures at Work in a Capillary
Hydrostatic and Osmotic Pressures
Hydrostatic Pressure (HP): Drives water out of capillaries.
Osmotic Pressure (OP): Draws water into capillaries; determined by solutes that cannot cross the membrane (e.g., albumin).
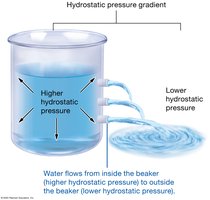
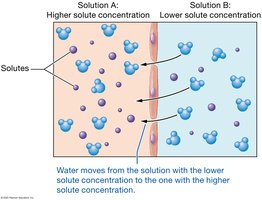
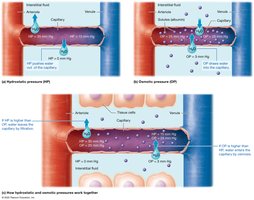
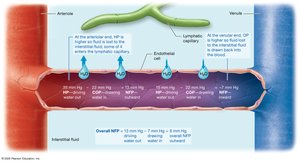
Net Filtration Pressure (NFP)
At the arteriole end, hydrostatic pressure dominates, causing filtration. At the venule end, osmotic pressure dominates, causing absorption. The net effect is a small loss of water to the interstitial fluid, which is returned by the lymphatic system.
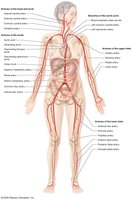
Anatomy of the Systemic Arteries
Major Arteries
Aorta: Largest artery; four divisions: ascending, arch, descending thoracic, descending abdominal.
Branches: Supply head, neck, thorax, abdomen, upper and lower limbs.
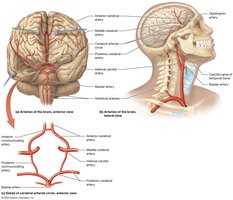
Arteries of the Head and Neck
Common Carotid Arteries: Split into external (supplies face/scalp) and internal (supplies brain).
Circle of Willis: Circular anastomosis in the brain for collateral circulation.
Arteries of the Thorax, Abdomen, Upper and Lower Limbs
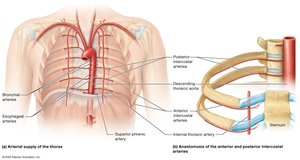
Thorax: Internal thoracic, anterior/posterior intercostal, bronchial, esophageal, superior phrenic arteries.
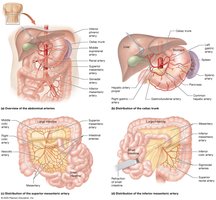
Abdomen: Celiac trunk, hepatic, splenic, gastric, mesenteric, renal, gonadal, iliac arteries.
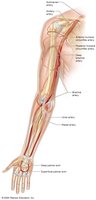
Upper Limb: Subclavian, axillary, brachial, radial, ulnar arteries.
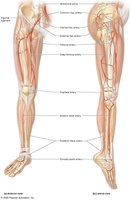
Lower Limb: External iliac, femoral, popliteal, tibial, dorsalis pedis, plantar arteries.
Pulse Points
Pulse points are superficial arteries where the pulse can be palpated, including carotid, radial, brachial, femoral, dorsalis pedis, and posterior tibial arteries.
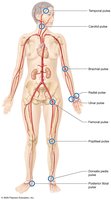
Anatomy of the Systemic Veins
Major Veins
Brachiocephalic Veins: Drain head, neck, thorax, upper limbs; form superior vena cava.
Common Iliac Veins: Drain lower limbs and pelvis; form inferior vena cava.
Venous Drainage of Head, Neck, Brain, Thorax, Abdomen, Limbs
Jugular Veins: Internal and external; drain head and neck.
Dural Sinuses: Drain brain; empty into internal jugular veins.
Azygos System: Drains posterior thoracic and abdominal walls.
Hepatic Portal System: Drains digestive organs; blood processed by liver before entering systemic circulation.
Superficial and Deep Veins of Limbs: Saphenous, femoral, popliteal, cephalic, basilic, brachial, axillary veins.
Clinical Correlations
Atherosclerosis, Hypertension, Hypotension, Varicose Veins, Stroke
Atherosclerosis: Plaque formation in arteries; risk factors include hypertension, smoking, diabetes, high cholesterol.
Hypertension: Chronic high blood pressure; managed by lifestyle changes and medications.
Hypotension: Low blood pressure; can lead to shock and organ failure.
Varicose Veins: Dilated veins due to decreased venous return.
Stroke (Cerebrovascular Accident): Disruption of blood flow to the brain; risk factors include hypertension, atherosclerosis, diabetes, smoking.
Summary Table: Types of Arteries and Veins
Type | Structure | Function |
|---|---|---|
Elastic Artery | Extensive elastic laminae | Conduct blood under high pressure |
Muscular Artery | Thick tunica media | Distribute blood to organs |
Arteriole | Thin walls, smooth muscle | Regulate blood flow to capillaries |
Venule | Thin walls, little smooth muscle | Drain capillary beds |
Vein | Thin layer of smooth muscle, valve, large lumen | Return blood to heart, prevent backflow |
Summary Table: Types of Capillaries
Type | Structure | Location |
|---|---|---|
Continuous | Tight junctions | Muscle, skin, nervous tissue |
Fenestrated | Fenestrations (pores) | Endocrine glands, intestines, kidneys |
Sinusoidal | Large pores, irregular basal lamina | Liver, spleen, bone marrow |
