 Back
BackChapter 18: The Cardiovascular System II – Blood Vessels
Study Guide - Smart Notes

Overview of the Cardiovascular System: Blood Vessels
Introduction
The cardiovascular system is composed of the heart and an extensive network of blood vessels that transport blood throughout the body. Blood vessels are essential for delivering oxygen, nutrients, and removing waste products from tissues. The vasculature collectively measures over 60,000 miles in length, highlighting its vastness and importance.
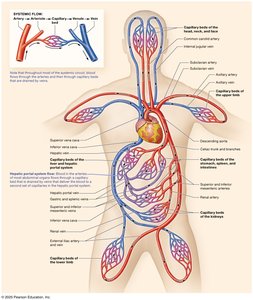
Types of Blood Vessels
Arteries, Capillaries, and Veins
Blood vessels are classified into three main types based on their function and structure:
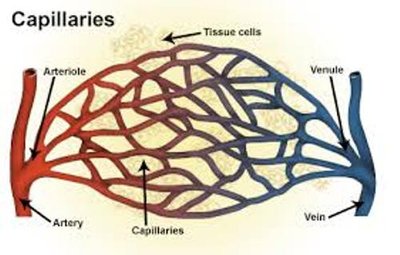
Arteries: Distribution system; carry blood away from the heart under high pressure.
Capillaries: Exchange system; facilitate the exchange of gases, nutrients, and wastes between blood and tissues.
Veins: Collection system; return blood to the heart, often under lower pressure.
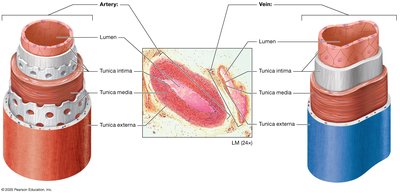
Structure of Arteries and Veins
Arteries and veins have three layers:
Tunica intima: Innermost layer, composed of endothelium.
Tunica media: Middle layer, contains smooth muscle and elastic fibers.
Tunica externa: Outermost layer, provides structural support.

Blood Distribution in the Cardiovascular System
Blood is distributed unevenly among different vessel types:
Systemic veins: 55%
Pulmonary veins: 15%
Systemic arteries: 10%
Capillaries: 5%
Pulmonary arteries: 3%
Right and left heart: 6% each

Structural Differences Among Vessel Types
Type | Structure |
|---|---|
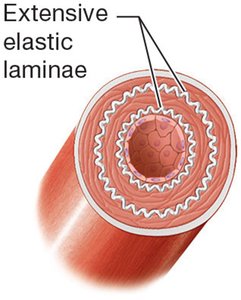
Elastic arteries | Extensive elastic laminae in tunica intima and media |
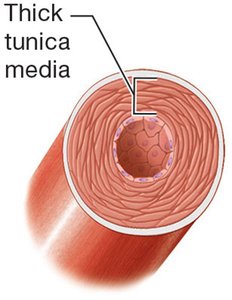
Muscular arteries | Thick tunica media with smooth muscle |
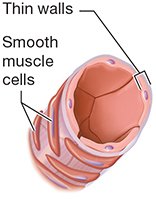
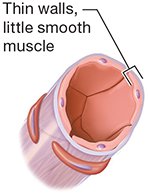
Arterioles | Thin walls, all three tunics, dispersed smooth muscle |
Venules | Thin walls, little smooth muscle |
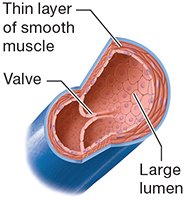
Veins | Thin smooth muscle, large lumen, valves present |
Functions of Blood Vessels
Key Functions
Conduct blood under high pressure to organs
Control blood flow to organs and tissues
Regulate blood pressure
Feed and drain capillary beds
Return blood to the heart
Atherosclerosis
Definition and Pathology
Atherosclerosis is the leading cause of death in the developed world. It affects large and medium-sized muscular arteries and is characterized by the formation of atherosclerotic plaques composed of lipids, cholesterol, calcium salts, and cellular debris within the tunica intima. Plaques often form at vessel branching points or curves.

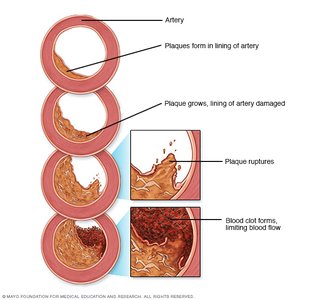
Development and Consequences
Endothelial injury (from high blood pressure, cholesterol, toxins, infections, high blood glucose) triggers inflammation.
Phagocytes are drawn to the site, causing further vessel damage.
Clots may form, leading to myocardial infarction or stroke.
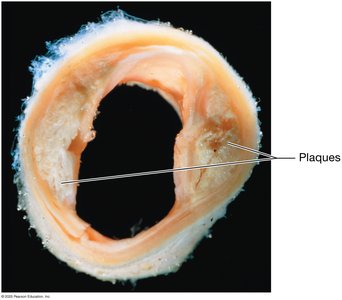
Treatment of Atherosclerosis
Dietary modifications
Physical activity
Medications to lower cholesterol, blood pressure, and manage glucose
Smoking cessation
Surgical interventions (e.g., stents, bypass grafts)

Hemodynamics: Physiology of Blood Flow
Blood Flow, Pressure, and Resistance
Hemodynamics refers to the study of blood flow. Blood flow is the volume of blood that flows per minute and is influenced by pressure and resistance.
Blood Pressure: Outward force blood exerts on vessel walls.
Resistance: Opposition to blood flow, affected by vessel radius, length, and blood viscosity.
Equation:

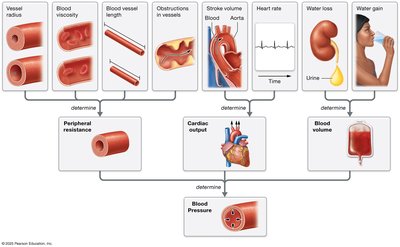
Factors Affecting Blood Pressure
Vessel radius (greatest effect on resistance)
Vessel length (increases with body size)
Blood viscosity (increases with more RBCs or dehydration)
Blood volume (increases with water intake)
Sympathetic and parasympathetic nervous system activity
Blood Pressure in Different Portions of Circulation
Systolic Pressure: Pressure during ventricular systole (~110–120 mm Hg)
Diastolic Pressure: Pressure during ventricular diastole (~70–80 mm Hg)
Pulse Pressure: Difference between systolic and diastolic (~40 mm Hg)


Mean Arterial Pressure (MAP)
MAP is the average pressure in systemic arteries during a cardiac cycle. It is estimated as:
Pressures in Pulmonary and Systemic Circuits
Circuit | Pressure |
|---|---|
Pulmonary arteries | 15 mm Hg |
Pulmonary veins | 5 mm Hg |
Systemic arteries | 120 mm Hg (systolic), 80 mm Hg (diastolic) |
Arterioles | 80–35 mm Hg |
Capillaries | 35–15 mm Hg |
Venules | 15–5 mm Hg |
Veins | 5–0 mm Hg |
Venous Return Mechanisms
Mechanisms
Valves prevent backflow
Smooth muscle contraction
Skeletal muscle pump
Respiratory pump
Varicose Veins
Varicose veins are dilated, bulging veins caused by decreased venous return, often due to pregnancy, prolonged standing, obesity, or genetics. Blood pools in the lower limbs, stretching the veins.
Blood Pressure Regulation
Short-Term Maintenance
Nervous system and endocrine system adjust resistance and cardiac output.
Baroreceptor reflex and chemoreceptor stimulation play key roles.
Hormones: Epinephrine, norepinephrine, thyroid hormone, angiotensin-II, ADH, ANP.
Long-Term Maintenance
Endocrine and urinary systems adjust blood volume.
Renin-angiotensin-aldosterone system regulates sodium and water retention.
ADH increases water retention; ANP promotes water and sodium excretion.
Disorders of Blood Pressure
Hypertension
May be acute or chronic
Associated with coronary artery disease, stroke, heart failure, dementia, kidney disease, vascular disease
Often called "the silent killer" due to lack of symptoms
Treatment: Lifestyle modifications and medications
Hypotension
May be chronic or acute
Severe hypotension leads to circulatory shock, loss of consciousness, organ failure, death
Causes: Blood loss, fluid loss, decreased cardiac output, excessive vasodilation (anaphylactic or septic shock)
Capillary Structure and Function
Types of Capillaries
Type | Structure | Location | Function |
|---|---|---|---|
Continuous | Tight junctions | Skin, nervous tissue, muscle | Least leaky; narrow range of substances cross |
Fenestrated | Small pores (fenestrations) | Kidneys, endocrine glands, small intestine | Moderately leaky; large volumes and larger substances cross |
Sinusoidal | Large pores, irregular basal lamina | Liver, lymphoid organs, bone marrow, spleen | Leakiest; large substances and cells cross |
Capillary Exchange Mechanisms
Diffusion
Transcytosis
Bulk flow (filtration and reabsorption)

Pressures at Work in a Capillary
Hydrostatic and Osmotic Pressure
Hydrostatic Pressure (HP): Drives water out of capillary
Osmotic Pressure (OP): Draws water into capillary
Net Filtration Pressure (NFP):
Overall NFP drives water out by filtration, with 2–4 liters lost daily and returned by the lymphatic system.
Edema
Edema is the accumulation of excess water in interstitial fluid. Peripheral edema affects legs and feet; ascites affects the abdomen. Causes include increased hydrostatic pressure or decreased osmotic pressure.
Cerebrovascular Accident (CVA)
Types and Risk Factors
Ischemic: Blockage of brain artery by clot; treated with clot-dissolving medications
Hemorrhagic: Ruptured cerebral artery; treated with surgery
Risk factors: Hypertension, atherosclerosis, diabetes, smoking, hypercholesterolemia, atrial fibrillation
Symptoms: Sudden paralysis, loss of vision, difficulty speaking
The Big Picture of Blood Vessel Anatomy
Summary
Blood vessels are integral to the cardiovascular system, providing distribution, exchange, and collection functions. Their structure and function are closely tied to their role in maintaining blood flow, pressure, and tissue health.
*Additional info: Academic context and explanations were expanded for clarity and completeness. Tables were recreated and images included only when directly relevant to the paragraph content.*
