 Back
BackChapter 18: The Cardiovascular System II – Blood Vessels and Hemodynamics
Study Guide - Smart Notes

The Cardiovascular System II: The Blood Vessels
Overview of Arteries and Veins
The vasculature consists of blood vessels that transport blood throughout the body, regulate blood flow, control blood pressure, and secrete chemicals. The pulmonary and systemic circuits are composed of three main types of blood vessels: arteries, capillaries, and veins.
Arteries: Distribution system; branch into smaller vessels as they move away from the heart, supplying tissues with blood.
Capillaries: Exchange system; form networks (capillary beds) for rapid exchange of gases, nutrients, and wastes.
Veins: Collection system; drain blood from capillary beds and return it to the heart, merging into larger vessels as they approach the heart.
Structure and Function of Blood Vessels
All blood vessels are tubular organs with a central lumen surrounded by three tissue layers (tunics): tunica intima, tunica media, and tunica externa.
Tunica intima: Innermost layer, composed of endothelium, subendothelial connective tissue, and internal elastic lamina. Provides a smooth surface for blood flow and elasticity for vessel distensibility.
Tunica media: Middle layer, contains smooth muscle cells and external elastic lamina. Controls vessel diameter via vasoconstriction and vasodilation, regulated by the sympathetic nervous system.
Tunica externa (adventitia): Outermost layer, composed of dense irregular collagenous connective tissue. Supports the vessel and prevents overstretching. Contains vaso vasora, small vessels that supply the outer layers.
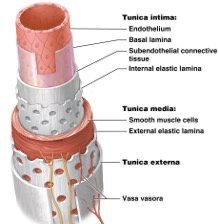
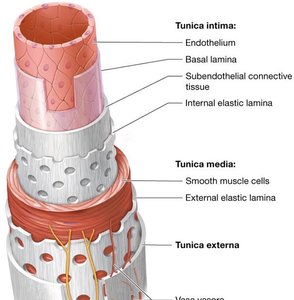

Comparison of Arteries and Veins
Arteries have thicker tunica media and more extensive elastic laminae than veins, reflecting their role in controlling blood pressure and withstanding higher pressure. Veins have thinner walls, larger lumens, and function as blood reservoirs.
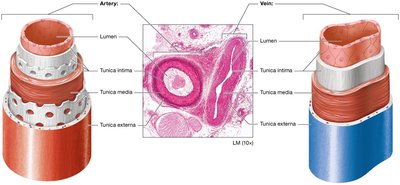
Classification of Blood Vessels
Blood vessels are classified by size and function:
Type | Diameter | Structure | Function |
|---|---|---|---|
Elastic arteries | 2.5–1.0 cm | Large arteries with extensive elastic lamina | Conduct blood under high pressure to organs |
Muscular arteries | 1.0 cm–0.3 mm | Thick tunica media with smooth muscle | Distribute blood to organs, regulate blood pressure |
Arterioles | 0.3 mm–10 μm | Thin walls with all three tunics | Control blood flow to tissues, feed capillary beds |
Venules | 8.0–100 μm | Thin walls, little smooth muscle | Drain capillary beds |
Veins | 100 μm–1.5 cm | Thin layer of smooth muscle, large lumen | Return blood to the heart |
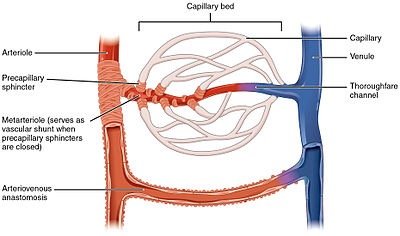
Vascular Anastomoses
Vascular anastomoses are connections between vessels via collateral pathways. Types include arterial anastomoses (heart, brain, joints), venous anastomoses (most common, web-like patterns), and arteriovenous anastomoses (direct artery-to-vein connections).

Physiology of Blood Flow (Hemodynamics)
Blood Pressure and Flow
Hemodynamics is the study of blood flow. Blood pressure is the force exerted by blood on vessel walls, measured in mm Hg. Blood flows down a pressure gradient from high pressure near the heart to lower pressure in peripheral vessels.

Blood flow: Directly proportional to pressure gradient; inversely proportional to resistance.
Velocity: Determined by cross-sectional area; fastest in aorta, slowest in capillaries.
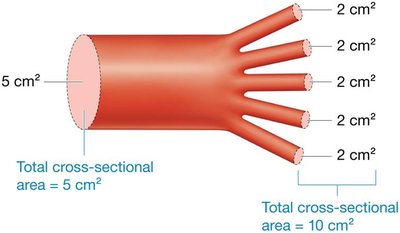
Factors Affecting Blood Pressure
Three main factors influence blood pressure: peripheral resistance, cardiac output, and blood volume.
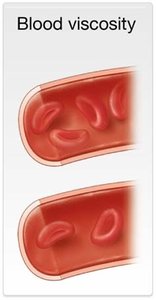
Peripheral resistance: Greatest in vessels farthest from the heart. Influenced by vessel radius (inverse relationship), blood viscosity (direct relationship), and vessel length (direct relationship).
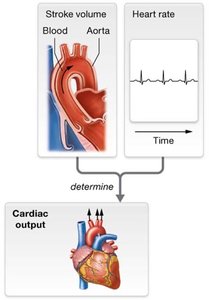
Cardiac output: Product of stroke volume and heart rate.
Blood volume: Directly linked to water content; more water increases blood volume and pressure.



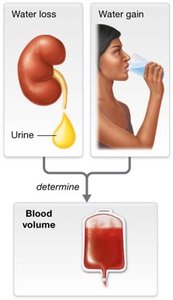
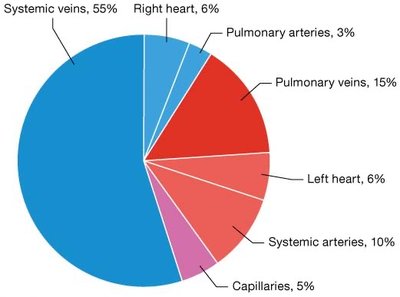
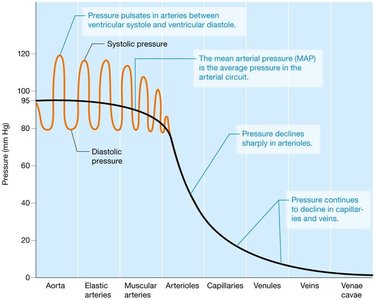
Blood Pressure in Circulation
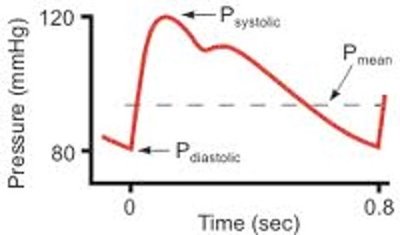
Blood pressure is highest in systemic arteries and lowest in veins. Mean arterial pressure (MAP) is the average pressure in systemic arteries during the cardiac cycle.
Systolic pressure: ~120 mm Hg
Diastolic pressure: ~80 mm Hg
Pulse pressure: Systolic − Diastolic
MAP:
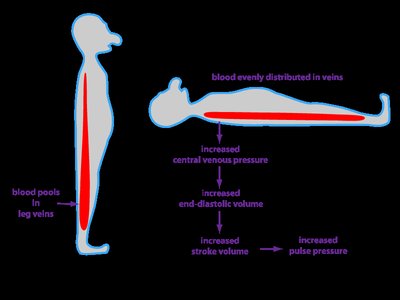
Venous Return Mechanisms
Venous blood returns to the heart via several mechanisms:
Venous valves prevent backflow.
Smooth muscle contraction increases venous return.
Skeletal muscle pumps propel blood upward.
Respiratory pump uses pressure changes during breathing.
Pulse Points
Pulse points are superficial arteries where the pulse can be palpated to assess heart rate and blood flow.
Maintenance of Blood Pressure
Short-Term Regulation
Short-term control is primarily by the nervous and endocrine systems, adjusting resistance and cardiac output.
Sympathetic stimulation: Increases heart rate, cardiac output, and vasoconstriction.
Parasympathetic stimulation: Decreases heart rate and cardiac output, allows vasodilation.
Baroreceptor reflex: Maintains homeostasis by detecting changes in vessel stretch and adjusting autonomic output.
Chemoreceptor reflex: Responds to changes in blood oxygen, CO2, and pH.
Endocrine Regulation
Hormones such as epinephrine, norepinephrine, thyroid hormone, angiotensin-II, and ANP regulate cardiac output and resistance.
Long-Term Regulation
Long-term control is managed by the urinary system and hormones affecting kidney function, adjusting blood volume by water retention or loss.
ANP decreases blood volume and pressure.
ADH and aldosterone increase blood volume and pressure.
Renin-angiotensin system increases blood volume and pressure.
Disorders of Blood Pressure
Hypertension and Hypotension
Blood pressure must be maintained within normal range. Hypertension (high BP) and hypotension (low BP) can cause severe disturbances.
Hypertension: Essential (unknown cause) or secondary (known cause).
Hypotension: Systolic < 90 mm Hg or diastolic < 60 mm Hg; can lead to shock and organ failure.
Causes: Reduced blood volume, decreased heart rate or stroke volume, excessive vasodilation.
Capillaries and Tissue Perfusion
Capillary Structure and Function
Capillaries are thin-walled vessels for exchange of nutrients, gases, and wastes. Types include:
Continuous capillaries: Least leaky, found in muscles, skin, nervous tissue.
Fenestrated capillaries: Leakier, found in endocrine glands, intestines, kidneys.
Sinusoidal capillaries: Leakiest, found in liver, spleen, bone marrow.
Capillary Exchange Mechanisms
Diffusion and osmosis through gaps and pores.
Diffusion through endothelial membranes.
Transcytosis for larger molecules.
Blood Flow through Capillary Beds
Microcirculation involves true capillaries and central vessels. Precapillary sphincters regulate blood flow; thoroughfare channels drain capillary beds.

Local Regulation of Tissue Perfusion
Autoregulation ensures proper blood flow to tissues via myogenic and metabolic mechanisms.
Myogenic mechanism: Alters arteriolar resistance in response to pressure changes.
Metabolic controls: Respond to local concentrations of oxygen, CO2, and H+.
Tissue Perfusion in Special Circuits
Heart: Perfusion decreases during systole; regulated by metabolic controls.
Brain: Maintains constant blood flow; regulated by myogenic and metabolic controls.
Skeletal muscle: Perfusion increases during exercise (hyperemia).
Skin: Perfusion regulated by temperature and sympathetic nervous system.
Capillary Pressures and Water Movement
Hydrostatic and Osmotic Pressures
Water movement across capillaries is driven by hydrostatic pressure (pushes water out) and osmotic pressure (draws water in).
Hydrostatic pressure: Force exerted by fluid; blood pressure equals hydrostatic pressure.
Osmotic pressure: Force needed to prevent water movement by osmosis; determined by solute concentration.
Colloid osmotic pressure: Created by plasma proteins, draws water into capillary.
Net Filtration Pressure (NFP)
NFP is the difference between hydrostatic and colloid osmotic pressures:
At arteriolar end: (water moves out)
At venular end: (water moves in)
Overall: (net filtration out)
Edema
Edema is excess water in interstitial fluid, caused by increased hydrostatic pressure or decreased colloid osmotic pressure. Peripheral edema occurs in hands and feet; ascites is fluid accumulation in the abdomen.
