 Back
BackChapter 18: The Urinary System – Renal Function
Study Guide - Smart Notes

The Urinary System: Renal Function
Overview of Kidney Function
The kidneys are essential organs responsible for regulating the composition and volume of all body fluids by controlling the plasma. Any changes in plasma composition affect both interstitial and intracellular fluids, making the kidneys central to homeostasis.
Ionic composition: Regulate ions such as Na+, K+, Mg2+, Ca2+, Cl-, and HCO3-.
Volume: Control total body water.
Osmolarity: Maintain osmotic balance.
pH: Regulate acid-base balance.
Metabolic wastes and foreign substances: Remove urea, creatinine, drugs, and toxins.
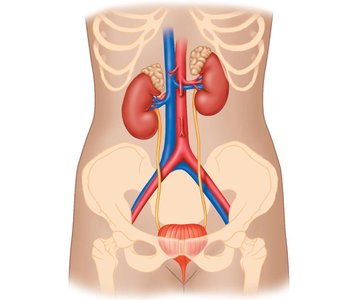
Macroscopic and Microscopic Anatomy of the Kidney
The kidneys, though less than 1% of body weight, receive about 20% of cardiac output at rest. They are composed of distinct anatomical regions and structures that facilitate their function.
Renal cortex: The outer region containing glomeruli and convoluted tubules.
Renal medulla: The inner region containing renal pyramids and loops of Henle.
Renal pelvis: Collects urine before it enters the ureter.
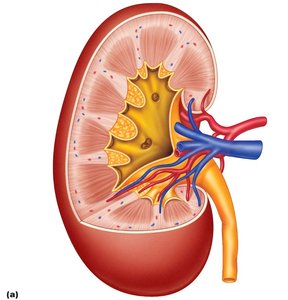
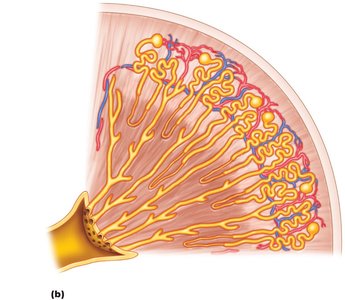
The Nephron: Functional Unit of the Kidney
Each kidney contains about one million nephrons, which are the basic functional units responsible for urine formation. Nephrons consist of a renal corpuscle and a renal tubule.
Renal corpuscle: Includes Bowman’s capsule and the glomerulus, where filtration occurs.
Renal tubule: Includes the proximal tubule, loop of Henle, distal tubule, and collecting duct.

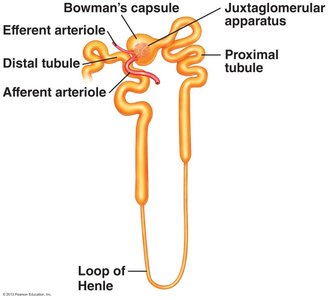
Types of Nephrons
Cortical nephrons: Located mostly in the cortex; have short loops of Henle.
Juxtamedullary nephrons: Located near the medulla; have long loops of Henle essential for concentrating urine.
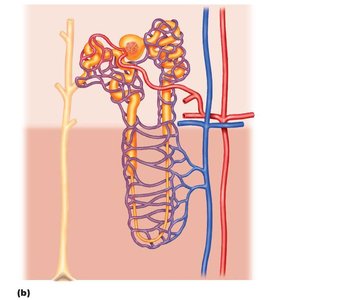
Blood Flow in the Kidney
The kidneys have a unique blood flow system, including two capillary beds in series: the glomerulus and the peritubular capillaries (including the vasa recta in juxtamedullary nephrons).
Afferent arteriole: Brings blood to the glomerulus.
Efferent arteriole: Carries blood away from the glomerulus to peritubular capillaries or vasa recta.
Basic Nephron Functions
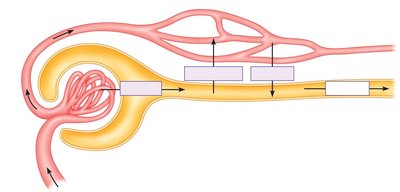
Filtration, Reabsorption, and Secretion
The nephron performs three main processes to form urine:
Filtration: Bulk flow of protein-free plasma from the glomerulus into Bowman’s capsule.
Reabsorption: Movement of substances from the renal tubule back into the blood (peritubular capillaries).
Secretion: Active transport of substances from the blood into the renal tubule.
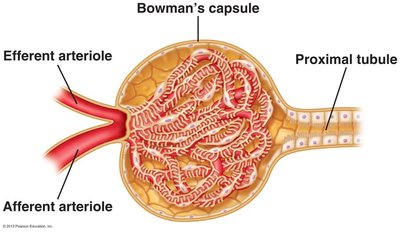
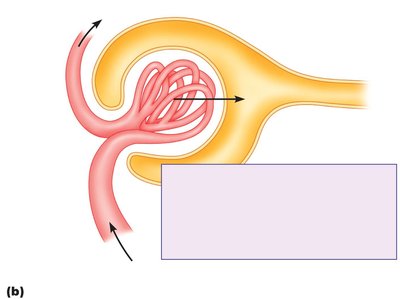
Filtration: The Glomerulus
Filtration occurs at the renal corpuscle, where the glomerular capillaries are surrounded by Bowman’s capsule. The filtration barrier consists of fenestrated endothelium, a basement membrane, and podocyte foot processes with filtration slits.
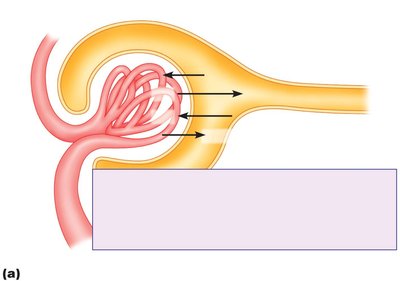
Filtration Pressures (Starling Forces)
Filtration is driven by the balance of hydrostatic and osmotic pressures across the glomerular capillaries:
Glomerular capillary hydrostatic pressure (PGC)
Bowman’s capsule osmotic pressure (πBC)
Bowman’s capsule hydrostatic pressure (PBC)
Glomerular capillary osmotic pressure (πGC)
The net filtration pressure (GFP) is calculated as:
Glomerular Filtration Rate (GFR) and Filtration Fraction
GFR: The volume of plasma filtered per minute (normal ≈ 125 mL/min).
Filtration fraction: The fraction of plasma that is filtered (normally about 20%).
Filtered Load
The filtered load is the quantity of a solute filtered per minute:
Where [X]plasma is the plasma concentration of the solute.
Regulation of GFR
GFR is tightly regulated to maintain fluid and electrolyte balance. Even small changes in GFR can have large effects on fluid and solute excretion.
Mean arterial pressure (MAP): The primary determinant of GFR.
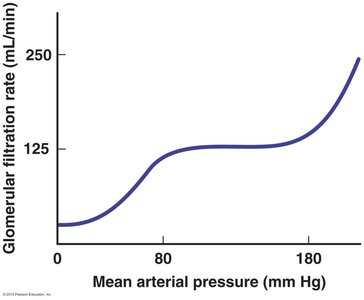
Intrinsic Controls
Myogenic regulation: Afferent arteriole constricts in response to increased pressure, maintaining stable GFR.
Tubuloglomerular feedback: Macula densa cells sense flow and signal afferent arteriole constriction or dilation.
Extrinsic Controls
Sympathetic nervous system: During stress (e.g., hemorrhage), vasoconstriction reduces GFR to conserve fluid.
Reabsorption and Secretion
Reabsorption
Most filtered substances are reabsorbed, primarily in the proximal tubule. Reabsorption can be active (requiring energy) or passive (by diffusion/osmosis).
Water: 99.2% reabsorbed
Glucose: 100% reabsorbed
Na+: 99.4% reabsorbed
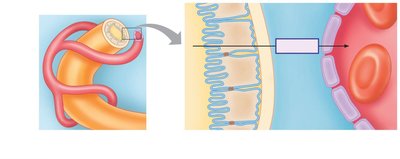
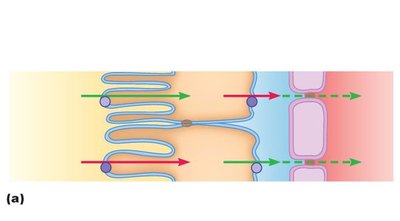
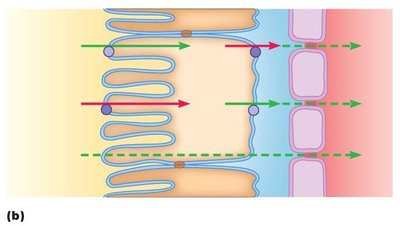
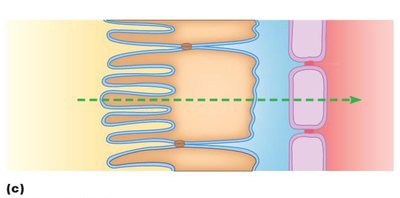
Mechanisms of Reabsorption
Active transport: Uses ATP to move substances against their gradient.
Passive transport: Simple diffusion or facilitated diffusion down a gradient.
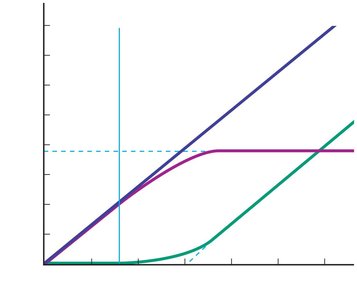
Transport Maximum (Tm) and Renal Threshold
Transport maximum (Tm): The highest rate at which a substance can be reabsorbed due to carrier protein saturation.
Renal threshold: The plasma concentration at which a substance begins to appear in urine.
Clinical Correlation: Diabetes Mellitus
In diabetes, elevated plasma glucose exceeds the renal threshold, leading to glucose in urine (glycosuria), increased osmolarity of filtrate, decreased water reabsorption, diuresis, dehydration, and thirst.
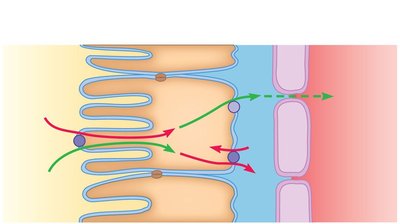
Secretion
Secretion is the movement of substances from the blood into the renal tubule, often for removal of excess ions (H+, HCO3-), waste products, and foreign substances (e.g., drugs).
Regional Specialization of the Renal Tubule
Proximal Convoluted Tubule (PCT)
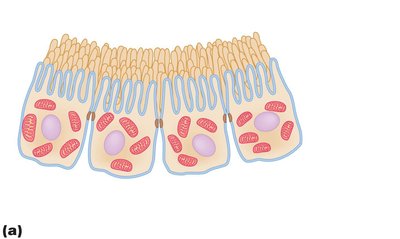
The PCT is specialized for nonregulated, bulk reabsorption. It has a brush border (microvilli), many mitochondria, and leaky tight junctions.
All glucose and most Na+ and water are reabsorbed here.
Loop of Henle
Juxtamedullary nephrons have long loops of Henle that create an osmotic gradient in the medulla, crucial for water conservation. This is discussed further in Chapter 19.
Distal Convoluted Tubule (DCT) and Collecting Duct
These segments are specialized for regulated reabsorption and secretion, with tight junctions and hormone receptors (e.g., for aldosterone and ADH) on the basolateral membrane.
Excretion
Excretion is the elimination of solute and water in the form of urine. Substances can enter the tubule by filtration or secretion, and are excreted unless reabsorbed.
Summary Table: Key Processes in the Nephron
Process | Direction | Main Location | Purpose |
|---|---|---|---|
Filtration | Blood → Tubule | Renal corpuscle | Initial formation of filtrate |
Reabsorption | Tubule → Blood | PCT, DCT, Loop of Henle, Collecting duct | Recovery of useful substances |
Secretion | Blood → Tubule | PCT, DCT, Collecting duct | Removal of excess ions, wastes |
Excretion | Tubule → External | Collecting duct → Ureter | Elimination as urine |
Additional info: For further details on water conservation and the countercurrent mechanism, see Chapter 19.
