 Back
BackChapter 22: The Respiratory System – Structure, Function, and Physiology
Study Guide - Smart Notes

Chapter 22: The Respiratory System
Introduction to the Respiratory System
The respiratory system is essential for gas exchange, supplying oxygen to the body and removing carbon dioxide. It also plays roles in maintaining acid-base balance, olfaction, and speech.
Primary Functions: Oxygen intake, carbon dioxide expulsion, acid-base balance.
Secondary Functions: Olfaction, speech, straining (e.g., coughing).
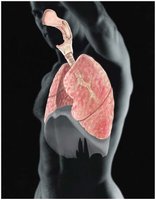
Major Divisions of the Respiratory System
By Location
Upper Respiratory Tract: Nasal/oral cavity through pharynx (sometimes includes larynx). Functions: warms, humidifies, and filters air.
Lower Respiratory Tract: Larynx to alveoli. Main site for gas exchange.
By Function
Conducting Zone: Nose to terminal bronchioles; not directly involved in gas exchange.
Respiratory Zone: Respiratory bronchioles to alveoli; site of gas exchange.
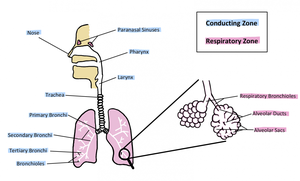
Upper Respiratory System
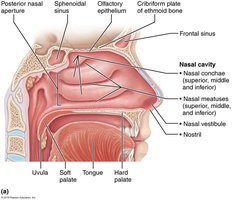
Nasal Cavity and Paranasal Sinuses
The nasal cavity is the entry point for air, lined with respiratory epithelium to filter, warm, and humidify incoming air. The conchae (superior, middle, inferior) increase surface area and turbulence for better filtration. Paranasal sinuses lighten the skull and add resonance to the voice.
Nasal Septum: Formed by the ethmoid bone, vomer, and septal cartilage.
Hard Palate: Maxilla (anterior 3/4) and palatine bone (posterior 1/4).
Respiratory Epithelium: Pseudostratified columnar epithelium with goblet cells (mucus production) and cilia (move mucus toward throat).
Pharynx
The pharynx is a muscular tube divided into three regions: nasopharynx (air only), oropharynx (air, food, liquid), and laryngopharynx (air, food, liquid). It serves as a passageway for both respiratory and digestive tracts.
Nasopharynx: Contains adenoids, auditory tube openings; closed off during swallowing.
Oropharynx: Contains palatine and lingual tonsils.
Laryngopharynx: Opens anteriorly into the larynx and posteriorly into the esophagus.
Lower Respiratory System
Larynx
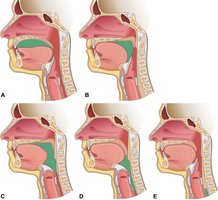
The larynx connects the pharynx to the trachea and is responsible for sound production. It is composed of several cartilages, including the epiglottis (covers airway during swallowing), thyroid cartilage (Adam's apple), and cricoid cartilage (only complete ring).
Glottis: Opening between the true vocal cords, which vibrate to produce sound.
False Vocal Cords: Vestibular folds, found laterally to the glottis.
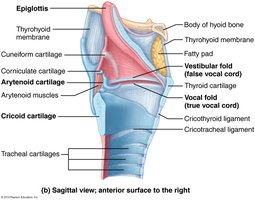
Trachea and Bronchial Tree
The trachea is supported by C-shaped hyaline cartilage rings and divides at the carina into the right and left primary bronchi. The right bronchus is more vertical and wider, making it more likely for aspirated objects to lodge there. The bronchial tree continues to branch into secondary (lobar), tertiary (segmental) bronchi, and bronchioles.
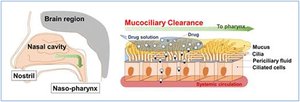
Mucociliary Escalator: Cilia and mucus work together to trap and move debris out of the respiratory tract.
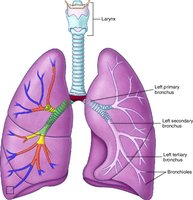
Respiratory Zone: Alveoli and Gas Exchange
Alveoli are the primary sites of gas exchange, lined by simple squamous epithelium. Their close association with capillaries allows for efficient diffusion of oxygen and carbon dioxide.
Type I Alveolar Cells: Squamous epithelial cells for gas exchange.
Type II Alveolar Cells: Produce surfactant to reduce surface tension and prevent alveolar collapse; secrete antimicrobial proteins.
Alveolar Macrophages: Engulf debris and pathogens.
Pleurae and Lung Structure
Pleural Membranes
Each lung is surrounded by a double-layered pleural membrane: the visceral pleura (on the lung surface) and the parietal pleura (lining the thoracic cavity). The pleural cavity contains serous fluid, reducing friction and helping lung inflation.
Pneumothorax: Air in the pleural space, causing lung collapse.
Pleurisy: Inflammation of the pleura, causing pain.
Pleural Effusion: Fluid accumulation in the pleural space.
Mechanics of Breathing
Boyle’s Law and Air Movement
Boyle’s Law states that the pressure and volume of a gas are inversely related. During inspiration, thoracic volume increases and pressure decreases, causing air to flow into the lungs. During expiration, volume decreases and pressure increases, pushing air out.
Inspiration: Active process involving diaphragm contraction and external intercostal muscles.
Expiration: Passive at rest; active during forced expiration (internal intercostals, abdominal muscles).
Respiratory Volumes and Capacities
Spirometry measures lung volumes and capacities, important for assessing respiratory health.
Tidal Volume (TV): ~500 mL, normal breath in and out.
Inspiratory Reserve Volume (IRV): Extra air inhaled after normal inspiration.
Expiratory Reserve Volume (ERV): Extra air exhaled after normal expiration.
Residual Volume (RV): Air remaining after maximal exhalation (~1200 mL).
Obstructive Diseases: Increased airway resistance (e.g., COPD), increased TLC and RV, decreased FEV1. Restrictive Diseases: Limited lung expansion (e.g., fibrosis), decreased TLC and RV, FEV1 may be normal percentage of reduced volume.
Gas Exchange and Transport
Gas Laws in Respiration
Dalton’s Law: Total pressure of a gas mixture equals the sum of partial pressures of individual gases.
Henry’s Law: The amount of gas dissolved in a liquid is proportional to its partial pressure and solubility.
External and Internal Respiration
External Respiration: Gas exchange between alveoli and blood.
Internal Respiration: Gas exchange between blood and tissues.
Oxygen and Carbon Dioxide Transport
Oxygen: Mostly transported bound to hemoglobin; the oxyhemoglobin dissociation curve is S-shaped due to cooperative binding.
Carbon Dioxide: Transported as bicarbonate ions (70%), bound to hemoglobin (20%), and dissolved in plasma (10%).
Control of Respiration
Neural Regulation
Respiratory centers in the brainstem (medulla and pons) regulate breathing rhythm and pattern. Chemoreceptors monitor CO2, O2, and pH levels, adjusting ventilation as needed.
CO2: Most powerful stimulus for breathing; increased CO2 lowers blood pH, stimulating increased ventilation.
O2: Plays a minor role except in severe hypoxia.
Acid-Base Balance
Normal Blood pH: 7.35–7.45.
Alkalosis: Blood pH above normal (less acidic).
Acidosis: Blood pH below normal (more acidic).
Buffers: Chemical buffers, respiratory system (rapid), renal system (slower but powerful).
Additional info: This guide covers the structure, function, and physiology of the respiratory system, integrating anatomical, physiological, and clinical concepts relevant for ANP college students.
