 Back
BackChapter 25: The Urinary System – Structure and Function
Study Guide - Smart Notes

Overview of the Urinary System
Major Functions of the Urinary System
The urinary system is essential for maintaining the body's internal environment by regulating water, electrolytes, and waste products. It consists of the kidneys, ureters, urinary bladder, and urethra.
Water and Solute Regulation: Maintains blood pressure and osmotic balance by controlling water and solute excretion.
Ion Concentration Regulation: Adjusts levels of ions such as sodium, potassium, and calcium in the extracellular fluid (ECF).
pH Regulation: Excretes hydrogen ions and reabsorbs bicarbonate to maintain acid-base balance.
Excretion of Metabolic Wastes: Removes urea, creatinine, drugs, and toxins from the blood.
Hormone Production: Produces erythropoietin (EPO) for red blood cell synthesis and renin for blood pressure regulation.
Vitamin D Activation: Converts vitamin D to its active form, aiding calcium absorption.
Gluconeogenesis: Generates glucose from non-carbohydrate sources during fasting.
Filtration: Approximately 200 liters of fluid are filtered daily by the kidneys.
Gross Anatomy of the Urinary System
Organs and Their Functions
The urinary system is composed of several organs, each with specialized roles in urine formation and excretion.
Kidneys: Filter blood, remove wastes, and regulate fluid and electrolyte balance.
Ureters: Transport urine from the kidneys to the urinary bladder.
Urinary Bladder: Temporarily stores urine until excretion.
Urethra: Conducts urine from the bladder to the outside of the body.
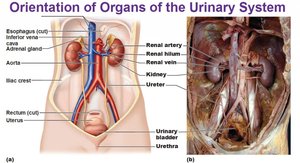
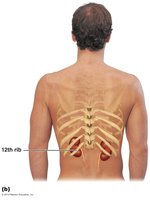
Location of the Kidneys
The kidneys are retroperitoneal organs, located on either side of the vertebral column. The right kidney is slightly lower than the left due to the position of the liver. The lower ribs provide partial protection.
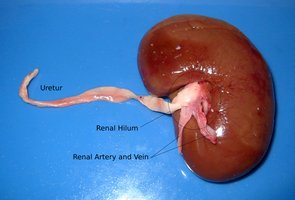
External Gross Anatomy of the Kidney
Hilum: The entry and exit site for the renal artery, vein, and ureter.
Adrenal Glands: Sit atop each kidney but are part of the endocrine system.
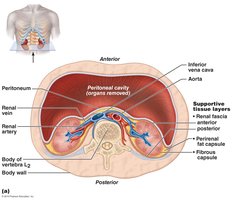
Coverings:
Renal Fascia: Dense connective tissue anchoring the kidney.
Perirenal Fat Capsule: Cushions and protects the kidney.
Fibrous Capsule: Prevents infection and maintains kidney shape.
Internal Gross Anatomy of the Kidney
Renal Cortex: The outer region containing renal corpuscles and convoluted tubules.
Renal Medulla: Contains renal pyramids and nephron loops.
Renal Pelvis: Funnel-shaped structure collecting urine before it enters the ureter.
Nerve Supply to the Kidneys
The kidneys receive autonomic innervation, primarily sympathetic fibers from the renal plexus, which regulate blood flow by altering the diameter of renal blood vessels.
Common Disorders of the Urinary System
Renal Ptosis: Dropping of the kidney due to loss of fat support.
Hydronephrosis: Swelling of the kidney due to urine buildup.
Pyelitis: Infection of the renal pelvis.
Pyelonephritis: Infection of the entire kidney, more common in females.
Microscopic Anatomy of the Kidney
Nephrons: The Functional Units
Each kidney contains over a million nephrons, which filter blood and form urine. Nephrons consist of a renal corpuscle and a renal tubule, and each drains into a collecting duct.
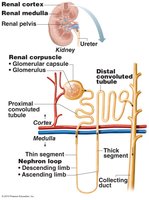
Renal Corpuscle
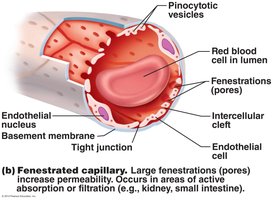
Glomerulus: A tuft of fenestrated capillaries specialized for filtration.
Bowman's (Glomerular) Capsule: Surrounds the glomerulus and collects filtrate.
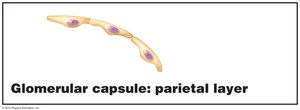
Parietal Layer: Simple squamous epithelium forming the outer wall.
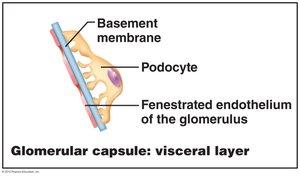
Visceral Layer: Composed of podocytes with foot processes and filtration slits.
Capsular Space: The area between the parietal and visceral layers where filtrate collects.
Renal Tubule Segments
The renal tubule consists of several segments, each with distinct histological features and functions:
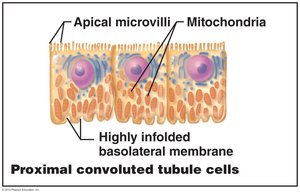
Proximal Convoluted Tubule (PCT): Simple cuboidal cells with a brush border for reabsorption.
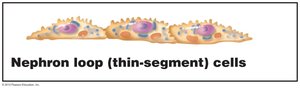
Nephron Loop (Loop of Henle):
Descending Limb: Thin segment, simple squamous epithelium.
Ascending Limb: Thin segment (simple squamous) and thick segment (simple cuboidal/columnar).
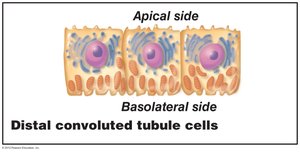
Distal Convoluted Tubule (DCT): Simple cuboidal cells, fewer microvilli than PCT.
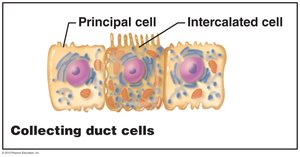
Collecting Duct
Principal Cells: Regulate water and sodium balance.
Intercalated Cells: Involved in acid-base (pH) regulation.
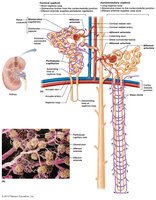
Types of Nephrons
Cortical Nephrons: Located mostly in the cortex; have short nephron loops; associated with peritubular capillaries.
Juxtamedullary Nephrons: Located near the cortex-medulla junction; have long nephron loops; associated with vasa recta; crucial for producing concentrated urine.
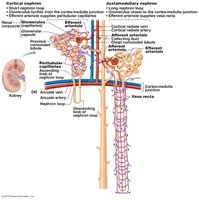
Nephron-Associated Capillaries
Glomerulus: Specialized for filtration; unique in being fed and drained by arterioles (afferent and efferent).
Peritubular Capillaries: Surround cortical nephrons; involved in reabsorption and secretion.
Vasa Recta: Surround juxtamedullary nephrons; play a role in concentrating urine and supplying nutrients to the medulla.
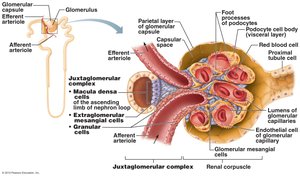
Juxtaglomerular Apparatus (JGA)
The JGA is a specialized structure where the distal tubule contacts the afferent and efferent arterioles. It regulates blood pressure and filtration rate.
Macula Densa: Chemoreceptors in the ascending limb of the nephron loop; sense NaCl concentration.
Juxtaglomerular (Granular) Cells: Located in arterioles; act as mechanoreceptors and secrete renin.
Extraglomerular Mesangial Cells: Facilitate communication between macula densa and granular cells.
Summary Table: Main Structures and Functions of the Urinary System
Structure | Main Function |
|---|---|
Kidney | Filtration of blood, regulation of fluid and electrolytes, hormone production |
Ureter | Transport of urine to bladder |
Urinary Bladder | Temporary storage of urine |
Urethra | Excretion of urine from body |
Nephron | Filtration, reabsorption, secretion, urine formation |
Collecting Duct | Final concentration of urine, water and pH regulation |
Additional info: The above notes integrate textbook-level explanations and context for each anatomical and physiological feature, ensuring a comprehensive review for exam preparation.
