 Back
BackChapter 28: Male Reproductive System – Structure and Function
Study Guide - Smart Notes

Male Reproductive System
Overview and Functions
The male reproductive system is responsible for producing, storing, and delivering male gametes (sperm) and synthesizing male sex hormones. It ensures the continuation of the human species through sexual reproduction.
Gonads (Testes): Produce sperm and secrete androgens (mainly testosterone).
Ducts: Transport sperm from the testes to the exterior.
Accessory glands: Secrete fluids that form semen.
External genitalia: Includes the penis and scrotum.
Comparison of Male and Female Reproductive Systems
Male: Produces millions of sperm daily; delivers sperm to the female reproductive tract.
Female: Releases one oocyte per month; supports fertilization and development of the embryo.
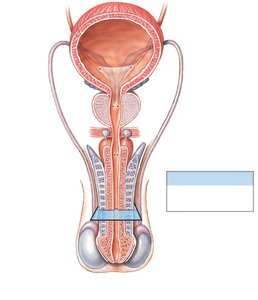
Structures of the Male Reproductive System
Pathway of Sperm
Sperm travel through a series of ducts and are mixed with secretions from accessory glands to form semen.
Testis → Epididymis → Ductus deferens → Ejaculatory duct → Urethra
Accessory glands: Seminal glands, prostate, bulbo-urethral glands
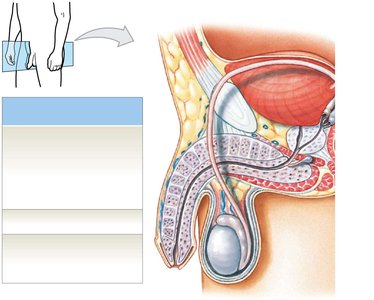
Scrotum and Testes
Scrotum: Divided into two chambers, each containing a testis. The raphe is the raised thickening on the scrotal surface.
Tunica vaginalis: Serous membrane lining the scrotal cavity, reducing friction.
Temperature regulation: Sperm development requires temperatures about 1.1ºC lower than body temperature. Muscles in the scrotum move the testes closer or farther from the body to maintain optimal temperature.
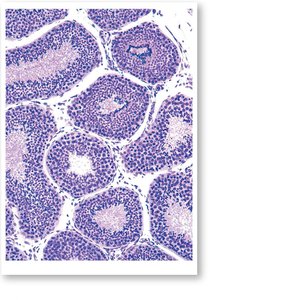
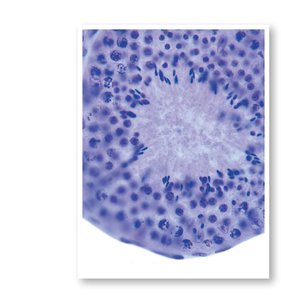
Histology of the Testes
The testes are composed of seminiferous tubules, where sperm production occurs. Interstitial endocrine cells (Leydig cells) between the tubules produce testosterone.
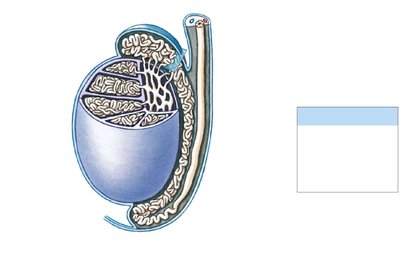
Epididymis
The epididymis is a coiled tube attached to the testis where sperm mature and are stored. It monitors and adjusts the composition of the fluid, recycles damaged sperm, and facilitates sperm maturation.
Ductus Deferens (Vas Deferens)
Approximately 40–45 cm long; part of the spermatic cord.
Transports sperm from the epididymis to the ejaculatory duct.
Wall contains thick smooth muscle for peristaltic movement.
Male Urethra
Shared by urinary and reproductive systems.
Divided into three regions: prostatic, membranous, and spongy urethra.
Accessory Glands
Accessory glands produce the fluid component of semen, each with unique biochemical properties.
Seminal glands (vesicles): Produce most of the semen volume; secretions are alkaline and rich in fructose.
Prostate: Secretes slightly acidic fluid (about 25% of semen volume) containing enzymes and antimicrobial proteins.
Bulbo-urethral glands: Secrete thick, alkaline mucus to neutralize urinary acids and lubricate the urethra.
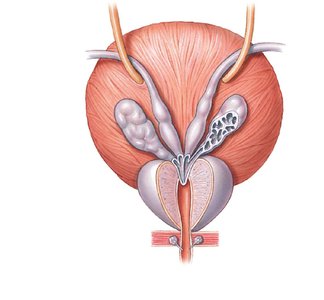
Penis and Erectile Tissue
Penis: Tubular organ for urination and semen delivery.
Root: Fixed portion attached to the body wall.
Body (shaft): Movable portion.
Glans penis: Expanded distal end surrounding the external urethral orifice.
Corpora cavernosa: Two cylindrical masses of erectile tissue.
Corpus spongiosum: Surrounds the urethra and forms the glans penis.
Mitosis, Meiosis, and Spermatogenesis
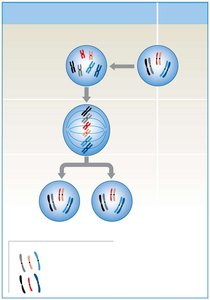
Mitosis
Mitosis is the process of somatic cell division, producing two genetically identical diploid (2n) daughter cells. It maintains chromosome number and is essential for growth and tissue repair.
Each daughter cell receives a complete set of homologous chromosomes.
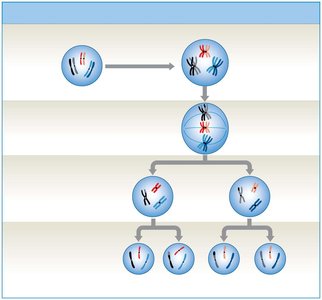
Meiosis
Meiosis is a specialized cell division that produces gametes (sperm in males, oocytes in females). It reduces the chromosome number by half, resulting in four haploid (n) cells, each genetically unique due to crossing over and independent assortment.
Meiosis I: Homologous chromosomes separate, reducing chromosome number.
Meiosis II: Sister chromatids separate, similar to mitosis.
Crossing over: Exchange of genetic material increases genetic diversity.
Spermatogenesis
Spermatogenesis is the process of sperm production, beginning at puberty and continuing throughout life. It occurs in the seminiferous tubules and involves three main phases: mitosis, meiosis, and spermiogenesis.
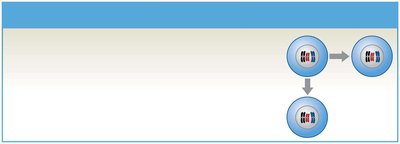
Spermatogonia: Stem cells that divide by mitosis; one remains a stem cell, the other becomes a primary spermatocyte.
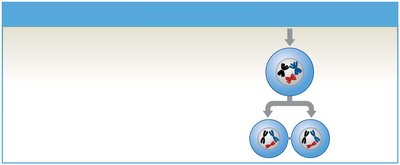
Primary spermatocytes: Undergo meiosis I to form secondary spermatocytes.
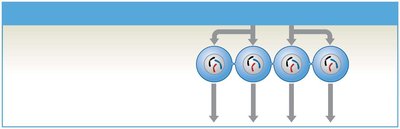
Secondary spermatocytes: Undergo meiosis II to form spermatids.
Spermatids: Immature gametes that differentiate into sperm during spermiogenesis.
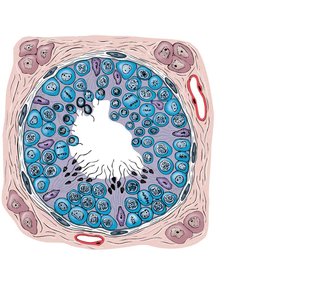
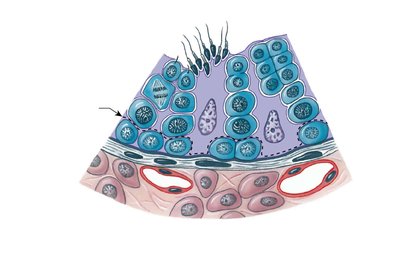
Seminiferous Tubule Structure
Seminiferous tubules contain spermatogonia, spermatocytes, spermatids, sperm, and large nurse (Sertoli) cells. Nurse cells support and regulate the process of spermatogenesis.
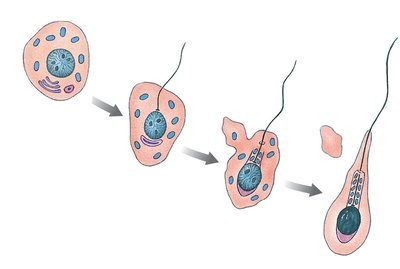
Spermiogenesis
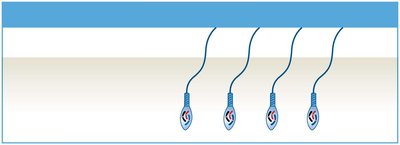
Spermiogenesis is the final stage of spermatogenesis, where spermatids undergo structural changes to become mature spermatozoa. This includes the development of the acrosome, condensation of the nucleus, formation of the flagellum, and shedding of excess cytoplasm.
Role of Nurse Cells (Sertoli Cells)
Maintain the blood-testis barrier, isolating the seminiferous tubules from the immune system.
Support mitosis, meiosis, and spermiogenesis by providing nutrients and regulatory signals.
Secrete inhibin (regulates FSH), androgen-binding protein (ABP), and other factors.
Hormonal Regulation of Male Reproductive Function
The hypothalamic-pituitary-gonadal axis regulates spermatogenesis and androgen production.
GnRH (Gonadotropin-releasing hormone): Released from the hypothalamus; stimulates the anterior pituitary to secrete FSH and LH.
FSH (Follicle-stimulating hormone): Stimulates nurse cells to promote spermatogenesis and secrete ABP.
LH (Luteinizing hormone): Stimulates interstitial cells to produce testosterone.
Testosterone: Maintains male sexual function, stimulates spermatogenesis, and establishes secondary sex characteristics.
Inhibin: Provides negative feedback to regulate FSH and GnRH secretion.
Anatomy of Sperm
Head: Contains the nucleus and acrosome (enzymes for fertilization).
Middle piece: Packed with mitochondria for ATP production.
Tail (flagellum): Provides motility.
Capacitation
Sperm leaving the epididymis are mature but immobile.
They become motile when mixed with seminal gland secretions and capable of fertilization after exposure to the female reproductive tract.
Summary Table: Key Structures and Functions of the Male Reproductive System
Structure | Main Function |
|---|---|
Testes | Produce sperm and testosterone |
Epididymis | Store and mature sperm |
Ductus deferens | Transport sperm |
Seminal glands | Produce seminal fluid (nutrients, buffers) |
Prostate | Secrete enzymes and antimicrobial proteins |
Bulbo-urethral glands | Secrete mucus for lubrication and pH balance |
Penis | Delivers semen to female tract |
