 Back
BackChapter 3: Tissues – Structure and Function in Human Anatomy
Study Guide - Smart Notes

Chapter 3: Tissues
Overview of Tissue Types
Human tissues are collections of cells with similar structure and function, forming the foundation for organs and systems. There are four primary tissue types:
Epithelial Tissue: Tightly bound, avascular sheets of cells covering surfaces and lining cavities.
Connective Tissue: Diverse group with specialized cells, protein fibers, and ground substance; functions include support, protection, and transport.
Muscular Tissue: Specialized for contraction; includes skeletal, cardiac, and smooth muscle.
Nervous Tissue: Specialized for conducting electrical impulses throughout the body.
Germ Layers and Tissue Origins
During embryonic development, three primary germ layers give rise to all tissues:
Ectoderm: Forms nervous system, epidermis, and associated glands.
Mesoderm: Middle layer; gives rise to connective tissues, muscles, and some organs.
Endoderm: Forms epithelia and glands of digestive, respiratory, and portions of urinary systems.
Epithelial Tissue
Structure and Characteristics
Epithelial tissue consists of layers of cells covering surfaces or lining internal passages. It includes both epithelia and glands.
Cellularity: Cells are tightly joined.
Polarity: Distinct apical (top) and basal (bottom) surfaces.
Attachment: Anchored to a basement membrane (basal lamina and reticular lamina).
Avascularity: Lacks blood supply; nutrients diffuse from underlying tissues.
Regeneration: Damaged cells are rapidly replaced.
Functions of Epithelial Tissue
Protection
Lubrication
Secretion
Absorption
Sensory reception
Reproduction
Classification of Epithelial Tissue
Epithelial tissues are classified by layer arrangement and cell shape:
Layer Arrangement: Simple (one layer), Stratified (multiple layers), Pseudo-stratified (appears layered, but is not).
Cell Shape: Squamous (flat), Cuboidal (cube-shaped), Columnar (tall), Transitional (stretchy).
Examples of Epithelial Types
Simple Squamous: Lines heart, blood vessels, alveoli; reduces friction, controls permeability.
Stratified Squamous: Skin, mouth, anus, vagina; protects against abrasion and pathogens.
Simple Cuboidal: Kidney tubules; involved in secretion and absorption.
Transitional: Bladder lining; stretches as bladder fills.
Simple Columnar: Stomach, gall bladder; absorption and secretion.
Pseudo-stratified (ciliated): Nasal cavity, bronchi; protection and secretion.
Glands
Exocrine: Secrete via ducts (e.g., sweat, mammary, goblet cells).
Endocrine: Ductless; secrete hormones directly into blood (e.g., pituitary, ovary).
Cell suffixes: -blast (immature, dividing), -cyte (mature, non-dividing).
Connective Tissue
Basic Components and Functions
Connective tissue is characterized by specialized cells, extracellular protein fibers, and ground substance. It supports, connects, protects, insulates, separates, and transports substances in the body.
Specialized Cells: Fixed (maintenance, repair, storage) and wandering (defense, repair).
Extracellular Protein Fibers: Collagen (strength), Reticular (network), Elastic (flexibility).
Ground Substance: Amorphous, can be fluid, gel, or solid.
Classification of Connective Tissue
Connective Tissue Proper: Many cell types, syrupy ground substance (e.g., adipose, tendons).
Fluid Connective Tissue: Distinct cell populations in watery matrix (e.g., blood, lymph).
Supporting Connective Tissue: Less diverse cells, matrix with closely packed fibers (e.g., bone, cartilage).
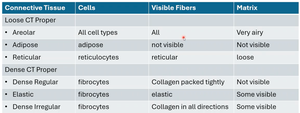
Connective Tissue Proper: Loose and Dense Types
Loose connective tissue has loosely arranged fibers and cells, while dense connective tissue has tightly packed fibers.
Loose: Areolar (airy, all cell types), Adipose (fat storage), Reticular (network, support).
Dense: Regular (parallel collagen, tendons/ligaments), Irregular (meshwork, dermis), Elastic (elastic fibers).
Supporting Connective Tissue: Cartilage and Bone
Supporting connective tissues provide structural strength and framework for the body. Cartilage is made of chondrocytes in lacunae, is avascular, and has a fibrous perichondrium. Bone is composed of osteocytes in lacunae, surrounded by a mineralized matrix.
Cartilage: Matrix of chondroitin sulfate, avascular, growth via appositional (cellular dimension) and interstitial (matrix production).
Bone: Collagen fibers surrounded by calcium; osteocytes in lacunae connected by canaliculi.

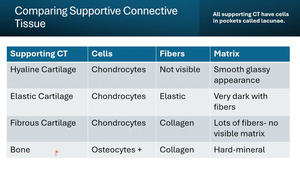
Comparison of Supporting Connective Tissue Types
Different types of cartilage and bone are distinguished by their cells, fibers, and matrix characteristics.
Supporting CT | Cells | Fibers | Matrix |
|---|---|---|---|
Hyaline Cartilage | Chondrocytes | Not visible | Smooth, glassy appearance |
Elastic Cartilage | Chondrocytes | Elastic | Very dark with fibers |
Fibrous Cartilage | Chondrocytes | Collagen | Lots of fibers, no visible matrix |
Bone | Osteocytes | Collagen | Hard, mineralized |
Muscular Tissue
Types and Functions
Muscular tissue is specialized for contraction and movement.
Skeletal Muscle: Striated, voluntary, multinucleate cells.
Smooth Muscle: Non-striated, involuntary, found in organs and blood vessels.
Cardiac Muscle: Striated, involuntary, found only in the heart.
Nervous Tissue
Structure and Function
Nervous tissue conducts electrical impulses and coordinates body functions. It consists of nerves and neurons, which transmit signals along their plasma membranes.
Neurons: Specialized for impulse transmission.
Functions: Sensory input, motor output, integration, and regulation.
Key Terms and Concepts
Lacunae: Small pockets in cartilage and bone where cells reside.
Perichondrium: Fibrous layer surrounding cartilage.
Appositional Growth: Increase in cellular dimension.
Interstitial Growth: Production of additional matrix material.
Summary Table: Connective Tissue Proper
Connective Tissue | Cells | Visible Fibers | Matrix |
|---|---|---|---|
Areolar | All cell types | All | Very airy |
Adipose | Adipose | Not visible | Not visible |
Reticular | Reticulocytes | Reticular | Loose |
Dense Regular | Fibrocytes | Collagen packed tightly | Not visible |
Elastic | Fibrocytes | Elastic | Some visible |
Dense Irregular | Fibrocytes | Collagen in all directions | Some visible |
Summary Table: Supporting Connective Tissue
Supporting CT | Cells | Fibers | Matrix |
|---|---|---|---|
Hyaline Cartilage | Chondrocytes | Not visible | Smooth, glassy appearance |
Elastic Cartilage | Chondrocytes | Elastic | Very dark with fibers |
Fibrous Cartilage | Chondrocytes | Collagen | Lots of fibers, no visible matrix |
Bone | Osteocytes | Collagen | Hard, mineralized |
Additional info:
Fat cells (adipocytes) are metabolically active and responsible for energy storage; they can increase in number but are not lost.
Connective tissue cells include fibroblasts (fiber production), macrophages (immune defense), adipocytes (fat storage), mesenchymal cells (stem cells), melanocytes (pigment production), mast cells (histamine production), lymphocytes (antibody production), and microphages (phagocytosis).
Blood is a fluid connective tissue with red blood cells (no nucleus, hemoglobin) and white blood cells (granulocytes and agranulocytes).
