 Back
BackChapter 4: Tissue—The Living Fabric (Study Notes)
Study Guide - Smart Notes

Chapter 4: Tissue—The Living Fabric
Introduction to Tissues
Tissues are groups of cells that are similar in structure and perform a common or related function. The study of tissues is called histology. The four basic tissue types in the human body are epithelial, connective, muscle, and nervous tissue.
Epithelial Tissue
General Characteristics of Epithelial Tissue
Cellularity: Composed almost entirely of closely packed cells with minimal extracellular material.
Polarity: Has an apical (free) surface and a basal (attached) surface.
Attachment: Supported by a basement membrane.
Avascular but Innervated: Contains no blood vessels but is supplied by nerve fibers.
Regeneration: High regenerative capacity due to frequent cell division.
Classification of Epithelia
Simple epithelia: Single cell layer; typically involved in absorption, secretion, and filtration.
Stratified epithelia: Two or more cell layers; mainly for protection.
Cell shape: Squamous (flat), cuboidal (cube-like), columnar (tall).
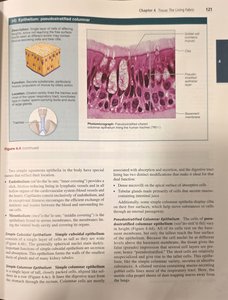
Pseudostratified Columnar Epithelium
This type appears to have multiple layers due to cell nuclei at different heights, but all cells rest on the basement membrane. It is often ciliated and found in the respiratory tract, where it helps move mucus.
Function: Secretion (especially of mucus); propulsion of mucus by ciliary action.
Location: Trachea and most of the upper respiratory tract.
Stratified Squamous Epithelium
This is the most widespread stratified epithelium, designed for protection in areas subject to abrasion. The surface cells are squamous, while deeper layers may be cuboidal or columnar.
Function: Protects underlying tissues in areas subjected to abrasion.
Location: Nonkeratinized type forms moist linings of the esophagus, mouth, and vagina; keratinized type forms the epidermis of the skin.
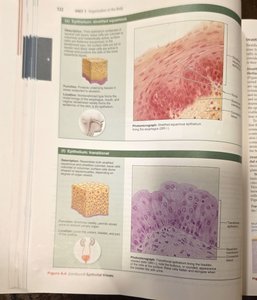
Transitional Epithelium
Transitional epithelium is specialized to stretch and is found lining the urinary organs. The appearance of the cells changes as the organ stretches.
Function: Stretches readily and permits distension of urinary organ by contained urine.
Location: Lines the ureters, bladder, and part of the urethra.

Glandular Epithelium
Glands consist of one or more cells that make and secrete a particular product. Glands are classified as endocrine (ductless, secrete hormones into blood) or exocrine (secrete products onto body surfaces or into body cavities).
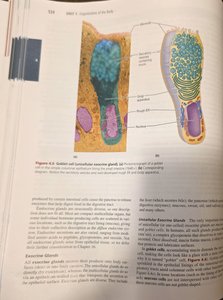
Unicellular exocrine glands: Goblet cells (produce mucus).
Multicellular exocrine glands: Composed of a duct and a secretory unit; classified by duct structure (simple or compound) and secretory unit shape (tubular, alveolar, or tubuloalveolar).
Connective Tissue
General Features of Connective Tissue
Most abundant and widely distributed tissue type.
Functions: Binding and support, protection, insulation, storing reserve fuel, and transporting substances (blood).
Common origin: All connective tissues arise from mesenchyme (an embryonic tissue).
Degrees of vascularity: Varying from avascular (cartilage) to highly vascular (bone).
Extracellular matrix: Connective tissues are largely nonliving extracellular matrix, which separates the living cells of the tissue.
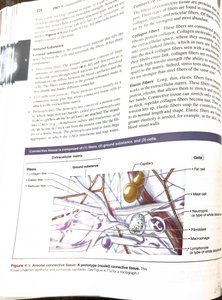
Structural Elements of Connective Tissue
Ground substance: Unstructured material that fills the space between cells and contains fibers.
Fibers: Collagen (strongest and most abundant), elastic (long, thin, allow for stretch), and reticular (short, fine, support soft tissue).
Cells: "-blast" cells are immature and actively mitotic; "-cyte" cells are mature and maintain the matrix. Other cells include fat cells, white blood cells, mast cells, and macrophages.
Classification of Connective Tissues
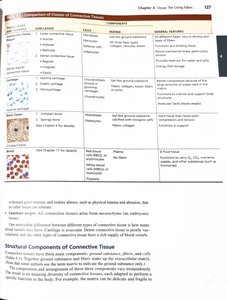
Connective tissues are classified into four main classes: connective tissue proper, cartilage, bone, and blood. Each class has several subclasses.
Class | Subclasses | Cells | Matrix | General Features |
|---|---|---|---|---|
Connective tissue proper | Loose (areolar, adipose, reticular); Dense (regular, irregular, elastic) | Fibroblasts, fibrocytes, defense cells, fat cells | Gel-like ground substance; all three fiber types | Six different types; functions as a binding tissue; resists mechanical stress |
Cartilage | Hyaline, elastic, fibrocartilage | Chondroblasts, chondrocytes | Gel-like ground substance; collagen, elastic fibers | Resists compression; cushions and supports body structures |
Bone tissue | Compact, spongy | Osteoblasts, osteocytes | Gel-like ground substance calcified with inorganic salts; collagen fibers | Hard tissue; supports and protects; stores calcium |
Blood | Blood cell formation | Red blood cells, white blood cells, platelets | Plasma (fluid matrix); no fibers | Fluid tissue; transports substances |

Types of Connective Tissue Proper
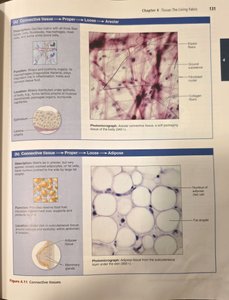
Loose connective tissue: Areolar, adipose, and reticular tissues.
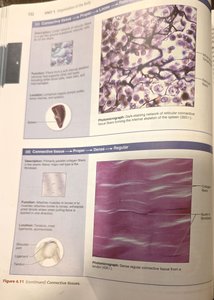
Dense connective tissue: Dense regular, dense irregular, and elastic tissues.

Cartilage
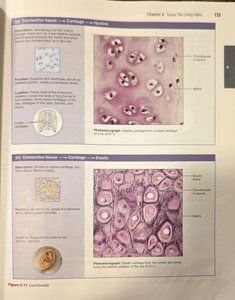
Hyaline cartilage: Most abundant; supports and reinforces; found in nose, trachea, larynx, and at ends of long bones.
Elastic cartilage: Maintains shape while allowing flexibility; found in external ear and epiglottis.
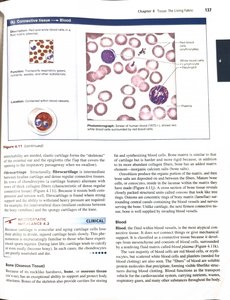
Blood
Blood is a connective tissue with a fluid matrix (plasma) and formed elements (red and white blood cells, platelets). It functions in transport of respiratory gases, nutrients, wastes, and other substances.
Muscle Tissue
General Features of Muscle Tissue
Muscle tissue is responsible for body movement. It is highly cellular, well-vascularized, and contains myofilaments (actin and myosin) for contraction. There are three types: skeletal, cardiac, and smooth muscle.
Skeletal Muscle
Long, cylindrical, multinucleate cells with striations.
Voluntary movement; locomotion; manipulation of the environment; facial expression.
Location: In skeletal muscles attached to bones or skin.
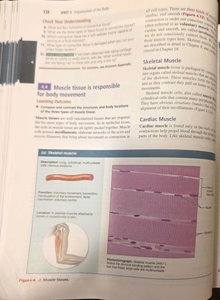
Cardiac Muscle
Branching, striated, generally uninucleate cells that interdigitate at intercalated discs.
Involuntary control; propels blood into the circulation.
Location: Walls of the heart.
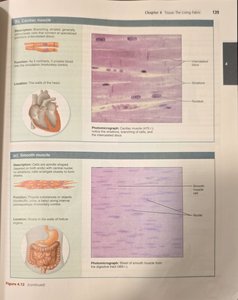
Smooth Muscle
Spindle-shaped cells with central nuclei; no striations; cells arranged closely to form sheets.
Involuntary control; propels substances or objects along internal passageways.
Location: Walls of hollow organs.

Nervous Tissue
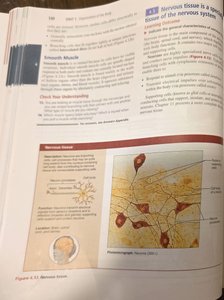
General Features of Nervous Tissue
Nervous tissue is the main component of the nervous system, which regulates and controls body functions. It is composed of neurons (nerve cells) and supporting cells (neuroglia).
Neurons: Specialized cells that generate and conduct nerve impulses.
Neuroglia: Supporting cells that protect, insulate, and support neurons.
Covering and Lining Membranes
Types of Membranes
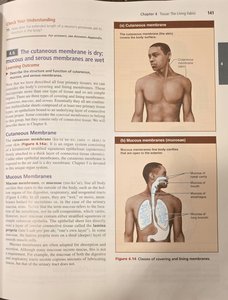
Cutaneous membrane: The skin; a dry membrane exposed to air.
Mucous membranes: Line body cavities open to the exterior (digestive, respiratory, urogenital tracts); moist membranes bathed by secretions.
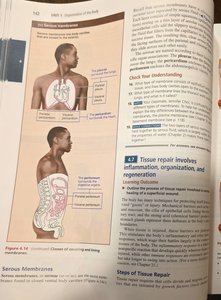
Serous membranes: Line body cavities closed to the exterior; consist of simple squamous epithelium on a thin layer of areolar connective tissue.
Tissue Repair
Steps of Tissue Repair
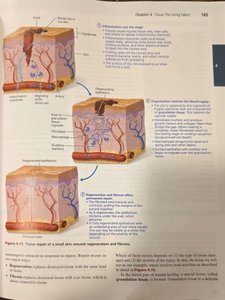
Tissue repair occurs in three steps: inflammation, organization, and regeneration/fibrosis.
Inflammation: Severed blood vessels bleed and inflammatory chemicals are released; clotting occurs.
Organization: Clot is replaced by granulation tissue, which restores blood supply; fibroblasts produce collagen fibers.
Regeneration and fibrosis: The epithelium thickens; a fully regenerated epithelium with underlying scar tissue results.
Cancer and Tissue Regeneration
Cancer: The Intimate Enemy
Cancer is characterized by uncontrolled cell division and the ability to invade other tissues (metastasis).
Carcinogenesis: The process by which normal cells are transformed into cancer cells, often involving mutations in genes that regulate cell growth.
Diagnosis and staging: Involves identifying the type and extent of cancer spread.
Treatments: Surgery, radiation, chemotherapy, and emerging therapies such as immunotherapy.

Regenerative Capacity of Different Tissues
High regenerative capacity: Epithelial tissues, bone, areolar connective tissue, dense irregular connective tissue, and blood-forming tissue.
Moderate regenerative capacity: Smooth muscle and dense regular connective tissue.
Weak regenerative capacity: Skeletal muscle and cartilage.
Virtually no functional regenerative capacity: Cardiac muscle and nervous tissue in the brain and spinal cord.
Review Questions
Review questions at the end of the chapter test understanding of tissue types, their functions, and clinical applications.

