 Back
BackChapter 6: The Bone Tissue – Structure, Function, and Growth
Study Guide - Smart Notes

Bone and Skeletal System: Functions
Overview of Bone Functions
The skeletal system is essential for multiple physiological and structural roles in the human body. Bones are dynamic organs that provide support, protection, movement, mineral storage, blood cell production, and energy storage.
Support: Bones form the structural framework of the body, supporting soft tissues and providing attachment points for tendons of skeletal muscles.
Protection: Bones protect vital internal organs. For example, the cranium protects the brain, vertebrae protect the spinal cord, and ribs protect the lungs and heart.
Assistance in Movement: Skeletal muscles attach to bones, and muscle contraction pulls on bones to produce movement.
Mineral Homeostasis: Bone tissue stores minerals, primarily calcium (99% of the body’s content) and phosphorus, as well as magnesium, sodium, and bicarbonate. Bones act as a reservoir, releasing minerals into the blood as needed.
Blood Cell Production: Red bone marrow within certain bones produces red blood cells, white blood cells, and platelets through a process called hemopoiesis.
Triglyceride Storage: Yellow bone marrow stores triglycerides in adipose cells, serving as a potential chemical energy reserve.
Structure of Bone
Gross Anatomy of a Long Bone
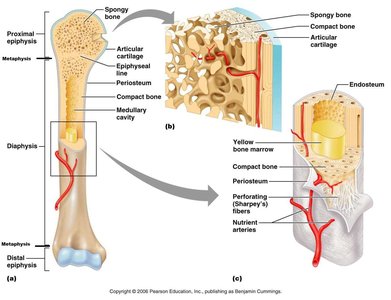
Long bones, such as the humerus, have a complex structure that supports their function in movement and mineral storage.
Diaphysis: The shaft or central part of a long bone.
Epiphysis: The ends of the bone, which are involved in joint formation.
Metaphysis: The region between the diaphysis and epiphysis, containing the epiphyseal (growth) plate in growing bones.
Articular Cartilage: A thin layer of hyaline cartilage covering the epiphysis, reducing friction and absorbing shock at joints.
Periosteum: A connective tissue membrane covering the bone, containing osteogenic cells for growth and repair, and serving as an attachment point for tendons and ligaments.
Medullary Cavity: The hollow space within the diaphysis, containing yellow bone marrow in adults.
Endosteum: The thin membrane lining the medullary cavity.
Histology of Bone Tissue
Composition of Bone Matrix
The bone matrix is a composite material that provides both strength and flexibility to bone tissue.
Matrix Components: 25% water, 25% collagen fibers, 50% crystallized mineral salts (mainly calcium phosphate, calcium carbonate, and calcium hydroxide).
Calcification: The process by which osteoblasts deposit and crystallize mineral salts in the collagen fiber framework, giving bone its hardness.
Collagen Fibers: Provide bone with flexibility and tensile strength.
Cell Types in Bone Tissue
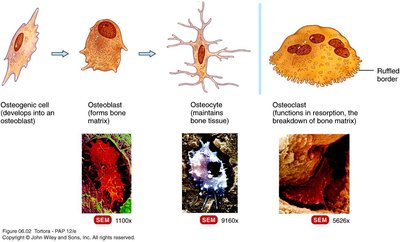
Bone tissue contains four main types of cells, each with specialized functions in bone formation, maintenance, and resorption.
Osteogenic Cells: Stem cells that undergo division to produce osteoblasts.
Osteoblasts: Bone-building cells that synthesize the extracellular matrix.
Osteocytes: Mature bone cells that maintain bone tissue and exchange nutrients and wastes with the blood. Osteocytes are former osteoblasts trapped in the matrix.
Osteoclasts: Large cells that release enzymes to digest bone matrix (bone resorption), playing a role in calcium regulation.
Types of Bone Tissue: Compact and Spongy Bone
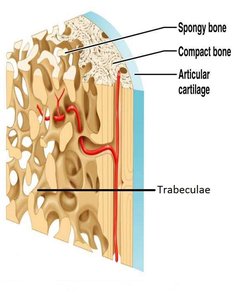
Bones are composed of two types of tissue: compact bone and spongy bone, each with distinct structures and functions.
Compact Bone: Dense and strong, forming the outer layer of bones. It is organized into osteons (Haversian systems), which consist of concentric lamellae, central canals, lacunae, and canaliculi.
Spongy Bone: Lighter and less dense, found mainly at the ends of long bones and inside flat bones. It consists of a lattice of trabeculae, with spaces containing red bone marrow for hemopoiesis.
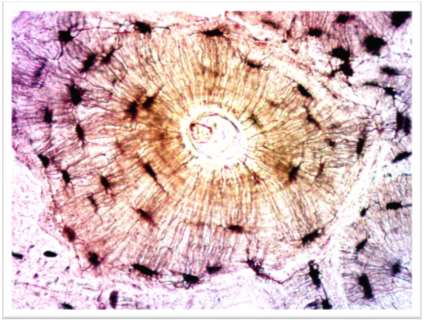
Osteon Structure in Compact Bone
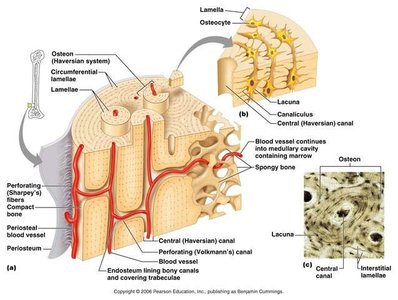
The osteon is the fundamental structural unit of compact bone, designed to resist stress and provide strength.
Central (Haversian) Canal: Runs longitudinally, containing blood vessels and nerves.
Concentric Lamellae: Rings of calcified matrix surrounding the central canal.
Lacunae: Small spaces between lamellae housing osteocytes.
Canaliculi: Tiny canals radiating from lacunae, allowing nutrient and waste exchange between osteocytes.
Osteon Organization: The arrangement of osteons adapts to physical demands on the skeleton.
Bone Formation (Ossification)
Overview of Ossification
Ossification, or osteogenesis, is the process by which bone forms. It occurs in four main situations:
Formation of bone in the embryo
Growth of bones until adulthood
Remodeling of bone throughout life
Repair of bone fractures
Patterns of Bone Formation
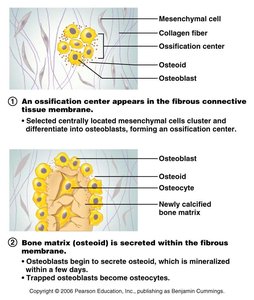
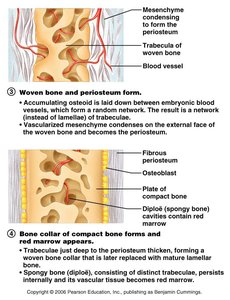
Intramembranous Ossification: Bone develops directly from mesenchymal tissue. This process forms flat bones of the skull and mandible.
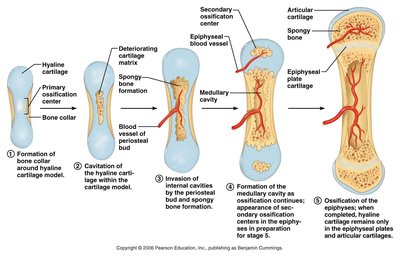
Endochondral Ossification: Bone replaces a cartilage model. Most bones, including long bones, are formed this way.
Bone Growth
Growth in Length
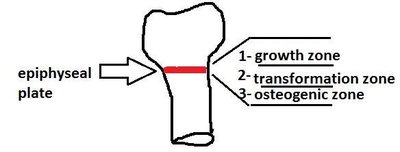
Long bones grow in length through the activity of the epiphyseal (growth) plate, which consists of three zones:
Growth Zone: Cartilage cells undergo mitosis.
Transformation Zone: Matrix begins to calcify, and cartilage cells die.
Osteogenic Zone: New bone tissue forms as osteoblasts lay down bone matrix.
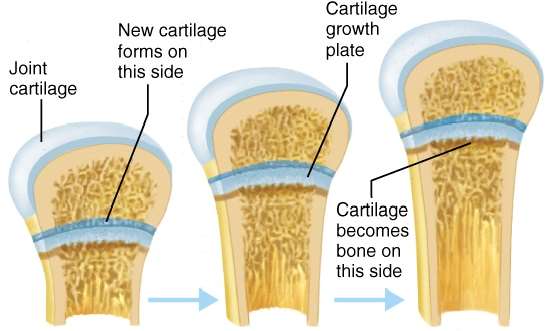
Growth in length involves both the proliferation of cartilage and its replacement by bone tissue. At adulthood, the epiphyseal plates close, and bone replaces all cartilage, leaving the epiphyseal line.
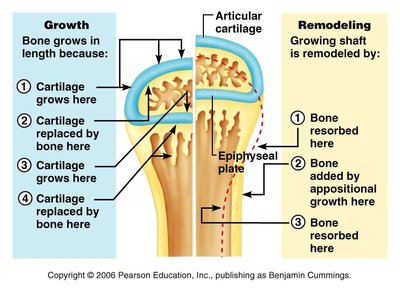
Growth in Thickness (Appositional Growth)
Bones grow in thickness by appositional growth, which involves the addition of new bone tissue to the outer surface by osteoblasts. Osteoclasts at the medullary cavity resorb bone tissue at a much lower rate, allowing the bone to thicken while maintaining a light structure.
Appositional Growth: Osteoblasts in the periosteum add new bone tissue to the outer surface.
Medullary Cavity Expansion: Osteoclasts resorb bone on the inner surface, enlarging the medullary cavity as the bone thickens.
Summary Table: Types of Bone Cells
Cell Type | Function |
|---|---|
Osteogenic Cell | Stem cell; divides to form osteoblasts |
Osteoblast | Bone-building cell; synthesizes matrix |
Osteocyte | Mature bone cell; maintains bone tissue |
Osteoclast | Resorbs bone matrix; regulates calcium |
Key Equations
Bone Matrix Mineralization:
Conclusion
Bone tissue is a dynamic, living structure essential for support, protection, movement, mineral storage, blood cell production, and energy storage. Its complex structure and cellular composition allow for growth, remodeling, and repair throughout life, making it a critical component of the human body.
