 Back
BackComprehensive Study Notes: Muscles and Muscle Tissue (Chapter 9)
Study Guide - Smart Notes

Muscle Overview
Types of Muscle Tissue
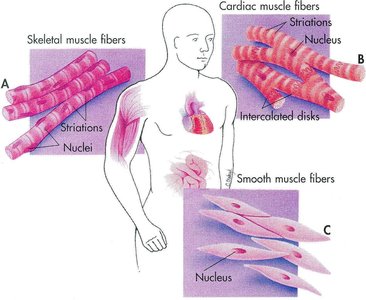
Muscle tissue is essential for movement, posture, and various bodily functions. There are three primary types of muscle tissue, each with distinct characteristics, locations, and functions.
Skeletal Muscle: Attached to bones and skin, striated, voluntary, and powerful. Responsible for body movement and posture.
Cardiac Muscle: Found only in the heart, striated, involuntary, and specialized for continuous rhythmic contraction.
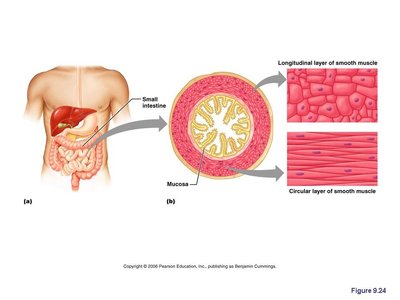
Smooth Muscle: Located in the walls of hollow organs (e.g., stomach, bladder, airways), not striated, involuntary, and responsible for movements such as peristalsis.
Muscle Terminology and Structure
Key Terms and Cellular Components
Muscle cells, also known as muscle fibers, possess specialized structures and terminology:
Sarcolemma: The plasma membrane of a muscle cell.
Sarcoplasm: The cytoplasm of a muscle cell.
Myofibrils: Rod-like organelles within muscle fibers, containing the contractile units called sarcomeres.
Roots: Prefixes such as myo, mys, and sarco refer to muscle.
Connective Tissue Sheaths
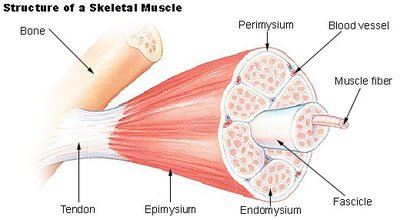
Skeletal muscle is organized and protected by several layers of connective tissue:
Epimysium: Surrounds the entire muscle.
Perimysium: Surrounds groups of muscle fibers called fascicles.
Endomysium: Surrounds individual muscle fibers.
Skeletal Muscle Attachments
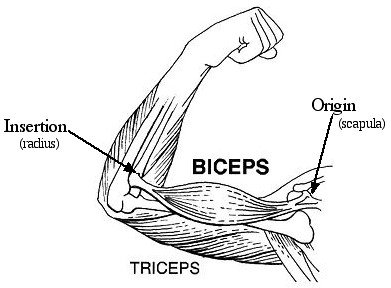
Origin and Insertion
Most skeletal muscles span joints and attach to bones at two points:
Origin: The immovable or less movable bone.
Insertion: The movable bone, which moves toward the origin during contraction.

Microscopic Anatomy of Skeletal Muscle
Muscle Fiber Structure
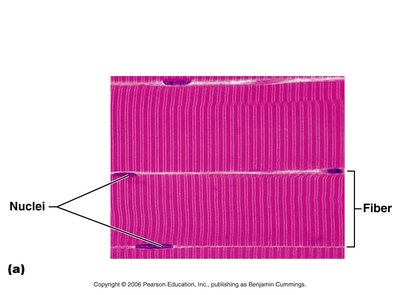
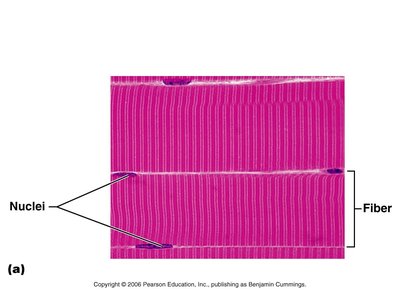
Skeletal muscle fibers are large, multinucleated cells containing numerous mitochondria, myofibrils, and specialized organelles for contraction.
Myofibrils: Densely packed, rod-like structures that make up about 80% of cell volume.
Striations: Alternating dark (A bands) and light (I bands) regions due to the arrangement of myofilaments.
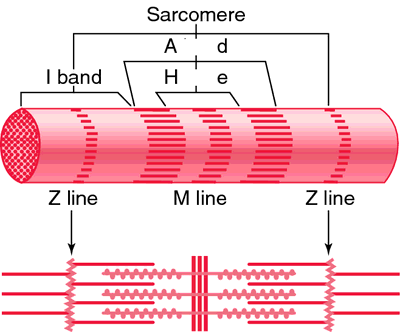
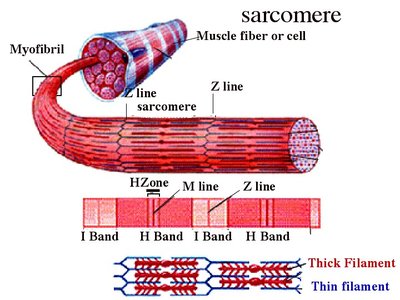
Sarcomere: The Functional Unit
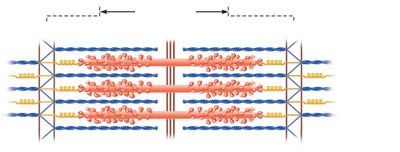
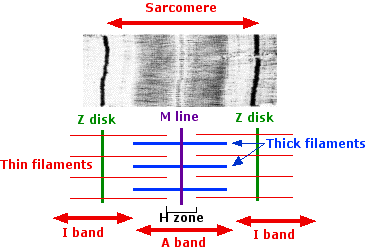
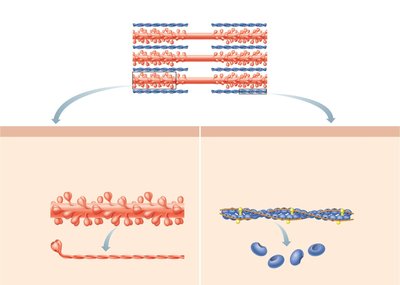
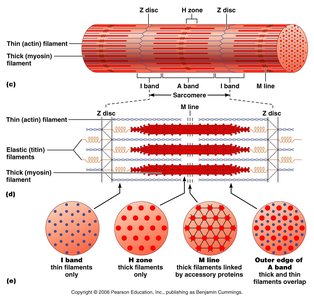
The sarcomere is the smallest contractile unit of muscle, defined as the region between two Z discs. It contains thick (myosin) and thin (actin) filaments arranged in a precise pattern.
A band: Contains thick filaments and overlapping thin filaments.
I band: Contains only thin filaments.
H zone: Lighter region in the middle of the A band where only thick filaments are present.
M line: Holds thick filaments together.
Z disc: Anchors thin filaments and connects sarcomeres.
Specialized Structures: Sarcoplasmic Reticulum and T Tubules
Sarcoplasmic Reticulum (SR)
The SR is a specialized smooth endoplasmic reticulum that stores calcium ions (Ca2+) necessary for muscle contraction.
Terminal cisternae: Enlarged areas of the SR that release Ca2+ during contraction.
T Tubules
T tubules are invaginations of the sarcolemma that help transmit action potentials deep into the muscle fiber, ensuring coordinated contraction.
A triad consists of a T tubule and two terminal cisternae.
Sliding Filament Model of Contraction
Mechanism of Muscle Contraction
During contraction, thin filaments slide past thick filaments, increasing overlap and shortening the sarcomere. This process is powered by ATP and regulated by Ca2+.
Distance between Z discs decreases.
I bands shorten, H zones disappear.
Neuromuscular Junction and Muscle Contraction
Events at the Neuromuscular Junction
The neuromuscular junction is the site where a motor neuron communicates with a muscle fiber, initiating contraction.
Acetylcholine (ACh) is released from the neuron and binds to receptors on the sarcolemma.
This triggers an action potential, leading to muscle contraction.
ACh is quickly broken down by acetylcholinesterase to prevent continuous contraction.
Resting Membrane Potential and Action Potential
Resting Membrane Potential (RMP)
RMP is the voltage difference across the cell membrane, typically around -70 mV in muscle cells. It is maintained by ion gradients and the Na+/K+ pump.
Inside of the cell is negative relative to the outside.
Na+/K+ pump moves 3 Na+ out and 2 K+ in per ATP used.
Action Potential
An action potential is a rapid change in membrane potential that triggers muscle contraction.
Depolarization: Na+ enters the cell, making it positive.
Repolarization: K+ leaves the cell, restoring negativity.
Hyperpolarization: Excess K+ leaves, making the cell more negative than RMP.
Excitation-Contraction Coupling
Sequence of Events
Excitation-contraction (E-C) coupling links the action potential to muscle contraction.
AP travels along sarcolemma and T tubules.
Ca2+ is released from SR.
Ca2+ binds to troponin, moving tropomyosin and exposing actin binding sites.
Cross bridge cycle begins.
When stimulation ceases, Ca2+ is pumped back into SR and contraction ends.
Cross Bridge Cycle
Steps of the Cycle
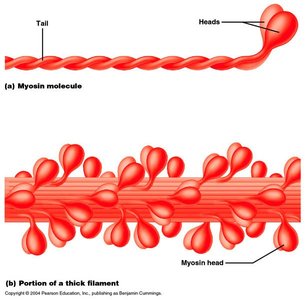
The cross bridge cycle is the process by which myosin heads pull actin filaments, resulting in muscle contraction.
Cross bridge formation: Myosin head binds to actin.
Power stroke: Myosin head pivots, pulling actin toward the M line.
Detachment: ATP binds to myosin, causing it to release actin.
Cocking: ATP hydrolysis re-energizes the myosin head.
Motor Units and Muscle Twitch
Motor Unit
A motor unit consists of a motor neuron and all the muscle fibers it innervates. The number of fibers per unit varies by muscle function.
Small motor units: Fine movements (e.g., fingers, eyes).
Large motor units: Weight-bearing muscles (e.g., thighs, hips).
Muscle Twitch
A muscle twitch is the response to a single, brief stimulus. It consists of three phases:
Latent period: EC coupling occurs.
Contraction period: Cross bridges form and muscle shortens.
Relaxation period: Ca2+ is pumped back into SR, muscle lengthens.
Graded Muscle Responses
Frequency and Strength of Stimulation
Muscle contractions can be graded by changing the frequency and strength of stimulation.
Wave summation: Increased frequency leads to stronger contractions.
Tetanus: Incomplete (some relaxation) or complete (sustained contraction).
Recruitment: Increasing stimulus strength activates more motor units.
Muscle Tone and Types of Contraction
Muscle Tone
Muscle tone is the constant, slightly contracted state of all muscles, keeping them firm and ready to respond.
Types of Contraction
Isometric: Muscle tension increases, but length does not change.
Isotonic: Muscle changes length and moves the load. Includes concentric (shortening) and eccentric (lengthening) contractions.
Muscle Metabolism: Energy for Contraction
ATP Production
ATP is the direct energy source for muscle contraction. It is regenerated by:
Interaction of ADP with creatine phosphate (CP).
Anaerobic glycolysis (no oxygen, produces lactic acid).
Aerobic respiration (uses oxygen, produces more ATP).
Key Equations:
(energy released)
(energy required)
Muscle Fatigue and Oxygen Debt
Causes of Muscle Fatigue
ATP production fails to keep pace with use.
Lactic acid accumulation lowers pH.
Ionic imbalances (Na+, K+).
Oxygen debt is the extra oxygen required after exercise to restore muscle to its resting state.
Force of Muscle Contraction
Factors Affecting Force
Number of muscle fibers contracting.
Relative size of the muscle.
Degree of muscle stretch (optimal at 80-120% resting length).
Muscle Fiber Types
Classification by Speed and Metabolism
Slow oxidative fibers: Slow contraction, fatigue resistant, aerobic metabolism.
Fast oxidative fibers: Fast contraction, moderate fatigue resistance, aerobic metabolism.
Fast glycolytic fibers: Fast contraction, easily fatigued, anaerobic glycolysis.
Red fibers (slow oxidative) contain myoglobin; white fibers (fast glycolytic) contain less myoglobin.
Smooth Muscle
Structure and Function
Smooth muscle is composed of spindle-shaped cells organized in two layers (longitudinal and circular) and found in hollow organs. It contracts slowly and synchronously, often in response to stretch.
Peristalsis: Alternating contractions and relaxations that move substances through organs.
Can undergo hyperplasia (increase in cell number).

Muscular Dystrophy and Developmental Aspects
Muscular Dystrophy
Muscular dystrophy is a group of inherited diseases causing muscle degeneration. Duchenne muscular dystrophy (DMD) is the most common, affecting males and leading to progressive muscle weakness.
Developmental Aspects
Cardiac and skeletal muscle become amitotic after birth but can lengthen and thicken.
Muscular development reflects neuromuscular coordination, which improves with training.
Men have greater muscle mass due to testosterone, but strength per unit muscle is similar in both sexes.
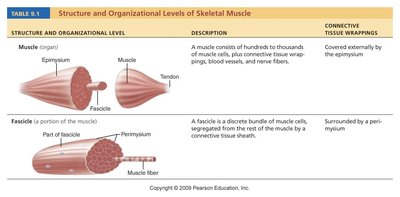
Summary Table: Structure and Organizational Levels of Skeletal Muscle
Structure and Organizational Level | Description | Connective Tissue Wrappings |
|---|---|---|
Muscle (organ) | Hundreds to thousands of muscle cells, plus connective tissue wrappings, blood vessels, and nerve fibers | Epimysium |
Fascicle (portion of muscle) | Discrete bundle of muscle cells, segregated from the rest of the muscle by a connective tissue sheath | Perimysium |
Muscle fiber (cell) | Elongated multinucleate cell; has a banded (striated) appearance | Endomysium |
