 Back
BackComprehensive Study Notes: The Human Reproductive Systems
Study Guide - Smart Notes

The Human Reproductive Systems
Introduction
The human reproductive systems are specialized to ensure the continuation of the species through sexual reproduction. Both male and female systems have unique and complementary structures and functions, regulated by hormones, that facilitate gamete production, fertilization, and development of offspring.
Sexual Reproduction and Gametogenesis
Overview of Sexual Reproduction
Sexual reproduction involves two parents and results in offspring with genetic variation.
Gametes are specialized sex cells: sperm (male) and ovum (female).
Fertilization is the fusion of sperm and ovum to form a zygote.
Reproductive hormones regulate the development of secondary sexual characteristics and reproductive capability, which begins at puberty.
The Male Reproductive System
Structural Organization
The male reproductive system consists of essential and accessory organs. Essential organs are the testes, which produce sperm. Accessory organs include ducts, glands, and external genitalia.
Ducts: Epididymis, vas (ductus) deferens, ejaculatory duct, urethra
Glands: Seminal vesicles, prostate gland, bulbourethral (Cowper) glands
External genitalia: Penis and scrotum
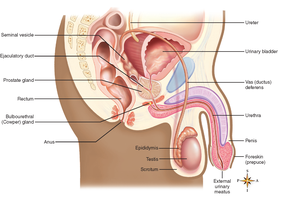
Testes: Structure and Function
Located in the scrotum, which maintains a temperature 1–3°C below body temperature for optimal sperm production.
Covered by the tunica albuginea, dividing the testis into lobules containing seminiferous tubules.
Interstitial cells (Leydig cells) produce testosterone.
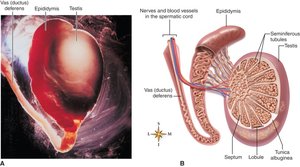
Spermatogenesis
Spermatogenesis is the process of sperm production, regulated by FSH from the pituitary gland.
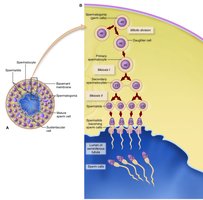
Spermatogonia (precursor cells) undergo mitosis and meiosis to form spermatids (each with 23 chromosomes).
Spermatids mature into spermatozoa (sperm cells).
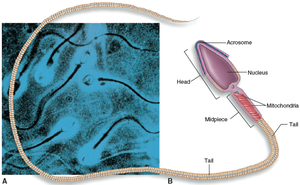
The head contains genetic material and an acrosome with enzymes for penetrating the ovum.
Mitochondria in the midpiece provide energy for motility.
Production of Testosterone
Produced by interstitial cells in response to LH (luteinizing hormone).
Responsible for development of male secondary sexual characteristics and accessory organs.
Stimulates protein synthesis and muscle growth (anabolic effects).
Male Reproductive Ducts
Epididymis: Site of sperm maturation and storage; sperm gain motility here.
Vas (ductus) deferens: Transports sperm from epididymis through the inguinal canal to the ejaculatory duct.
Ejaculatory duct: Formed by the union of vas deferens and duct of seminal vesicle; empties into the urethra.
Urethra: Conducts both urine and semen to the exterior.
Accessory Sex Glands
Seminal vesicles: Produce 60% of seminal fluid, rich in fructose for sperm energy.
Prostate gland: Secretes a thin, milky fluid (30% of semen) that activates sperm and enhances motility.
Bulbourethral (Cowper) glands: Secrete mucus-like fluid for lubrication (<5% of semen), often released before ejaculation.
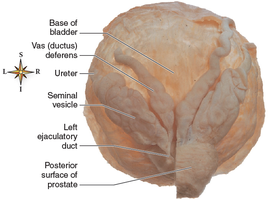
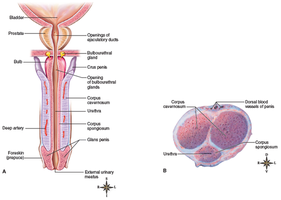
Male External Genitalia
Penis: Contains three columns of erectile tissue (two corpora cavernosa, one corpus spongiosum).
Glans penis: Distal end, covered by foreskin (prepuce); removal is circumcision.
Scrotum: Skin-covered pouch housing the testes and associated structures.
Common Male Reproductive Disorders
Oligospermia: Low sperm count, leading to infertility.
Cryptorchidism: Undescended testes, increasing risk of infertility and cancer.
Testicular cancer: Most common in males aged 15–30; self-examination recommended.
Benign prostatic hypertrophy: Prostate enlargement, common in older men.
Prostate cancer: Detected by PSA test and rectal examination.
Phimosis/Paraphimosis: Foreskin disorders affecting retraction.
Erectile dysfunction: Inability to achieve erection.
Hydrocele: Fluid accumulation in scrotum.
Inguinal hernia: Protrusion of abdominal organs into scrotum.
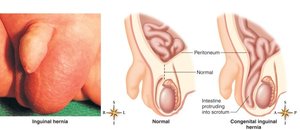
The Female Reproductive System
Structural Organization
The female reproductive system includes essential organs (ovaries) and accessory organs (ducts, glands, and external genitalia).
Ovaries: Produce ova and sex hormones.
Ducts: Uterine (fallopian) tubes, uterus, vagina.
Glands: Vestibular glands, mammary glands (breasts).
External genitalia: Mons pubis, clitoris, labia majora and minora, hymen, etc.
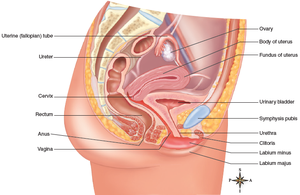
Ovaries: Structure and Function
Paired glands, each about 3 g, located in the pelvic cavity.
Contain ovarian follicles with oocytes (immature eggs).
At puberty, about 400,000 primary follicles remain; 350–500 mature and ovulate during reproductive years.
Corpus luteum forms after ovulation and produces progesterone.
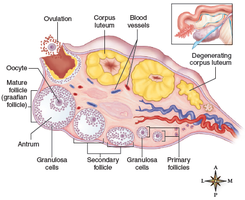
Oogenesis and Hormone Production
Oogenesis: Meiotic division producing one large ovum and polar bodies (which degenerate).
Estrogen: Produced by granulosa cells; responsible for secondary sex characteristics.
Progesterone: Produced by corpus luteum; prepares uterus for implantation and maintains pregnancy.
Female Reproductive Ducts
Uterine (fallopian) tubes: Transport ova from ovaries to uterus; fimbriae help capture ovum.
Uterus: Muscular organ (body, fundus, cervix); site of menstruation, pregnancy, and labor.
Vagina: Muscular tube for intercourse, birth canal, and menstrual flow.
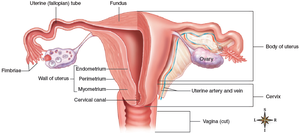
Female Accessory Glands and Breasts
Vestibular glands (Bartholin glands): Secrete mucus for lubrication; can become infected (e.g., gonorrhea).
Breasts: Contain glandular tissue for milk production; lymphatic drainage is important in cancer spread.
Female External Genitalia
Includes mons pubis, clitoris, labia majora and minora, hymen, and perineum.
Episiotomy: Surgical cut of perineum during childbirth.
The Menstrual Cycle
Phases of the Menstrual Cycle
Menses: Days 1–4/5; shedding of endometrial lining with bleeding.
Proliferative phase: End of menses to ovulation; endometrial repair and thickening.
Secretory phase: Ovulation to next menses; endometrial thickening and secretion in preparation for implantation.
Ovulation typically occurs 14 days before the next menses in a 28-day cycle. Hormonal regulation involves FSH and LH from the pituitary and estrogen and progesterone from the ovaries.
Common Female Reproductive Disorders
Dysmenorrhea: Painful menstruation.
Amenorrhea: Absence of menstruation.
Dysfunctional uterine bleeding (DUB): Irregular or excessive bleeding.
Premenstrual syndrome (PMS): Symptoms before menstruation.
Pelvic inflammatory disease (PID): Infection of reproductive organs, often causing infertility.
Endometriosis: Endometrial tissue outside uterus, causing pain and infertility.
Polycystic ovary syndrome (PCOS): Multiple cysts in ovaries, leading to infertility.
Ovarian cysts: Fluid-filled sacs, usually benign.
Cancers: Breast, ovarian, uterine, and cervical cancers; Pap smear for cervical cancer screening.
Sexually Transmitted Diseases (STDs)
Overview
STDs are the most common communicable diseases, transmitted primarily through sexual contact but also by other means.
Caused by bacteria, viruses, or other organisms.
Prevention and early treatment are essential to avoid complications such as infertility and systemic illness.
Summary
Both male and female reproductive systems are adapted for gamete production, fertilization, and development of offspring.
Hormonal regulation is essential for secondary sexual characteristics and reproductive function.
Disorders can affect fertility and overall health; regular self-examination and screening are important for early detection and treatment.
