 Back
BackDigestive and Endocrine Systems: Structure, Function, and Regulation
Study Guide - Smart Notes

Digestive System
Lower GI Tract and Associated Accessory Digestive Structures
The lower gastrointestinal (GI) tract is responsible for the absorption of water, electrolytes, and vitamins, as well as the formation and elimination of feces. It includes the large intestine, which is divided into several regions, each with distinct anatomical and functional characteristics.
Large Intestine Functions: Absorbs water, sodium (Na+), chloride (Cl-), and vitamins B and K.
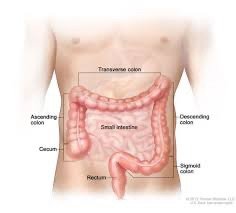
Gross Anatomy of the Large Intestine
Cecum: First portion; receives chyme from the ileum. The vermiform appendix projects from the cecum and contains lymph nodules, possibly serving as a bacterial reservoir.
Colon: Four regions—ascending, transverse, descending, and sigmoid colon. Each region is defined by anatomical flexures and transitions.
Rectum: Muscular tube for feces storage; contains rectal valves.
Anal Canal: Lined with stratified squamous epithelium, passes through the pelvic floor, and terminates at the anus. Contains anal columns and sinuses, and is regulated by internal (smooth muscle) and external (skeletal muscle) anal sphincters.
Specialized Structures of the Large Intestine
Teniae coli: Bands of smooth muscle that help form haustra (sacculations).
Omental appendices: Fat lobules attached to haustra.
Histology of the Large Intestine
Mucosa lined with simple columnar epithelium and goblet cells (secrete mucin).
No villi; numerous intestinal glands.
Lymphoid nodules and immune cells in the lamina propria.
Muscularis has two layers; outer longitudinal layer forms teniae coli.
Bacterial Action in the Large Intestine
Gut microbiome breaks down complex carbohydrates, proteins, and lipids.
Produces vitamins B and K, which are absorbed into the blood.
Feces composition: water, salts, epithelial cells, bacteria, undigested material.
Motility and Regulation
Peristalsis: Weak, sluggish contractions.
Haustral churning: Localized mixing movements.
Mass movement: Powerful contractions propelling contents toward the rectum (2–3 times/day).
Reflexes: Gastrocolic (initiated by stomach distention) and defecation reflex (rectal filling triggers urge to defecate via spinal reflexes).
Nutrients and Their Digestion
Carbohydrate Digestion
Classification: Monosaccharides (glucose), disaccharides (sucrose), polysaccharides (starch).
Oral cavity: Salivary amylase begins starch digestion; inactivated in the stomach.
Small intestine: Pancreatic amylase and brush border enzymes (dextrinase, glucoamylase, maltase, lactase, sucrase) complete digestion to monosaccharides.
Monosaccharide Absorption
Glucose & Galactose: Absorbed via SGLT (symport with Na+), exit via GLUT-2 (facilitated diffusion).
Fructose: Absorbed and exits via GLUT-5 (facilitated diffusion); mostly converted to glucose in epithelial cells.
All monosaccharides enter blood via the hepatic portal vein to the liver.
Protein Digestion
Stomach: HCl denatures proteins; pepsin (from pepsinogen) breaks proteins into oligopeptides.
Small intestine: Pancreatic enzymes (trypsin, chymotrypsin, carboxypeptidase) and brush border enzymes (dipeptidase, aminopeptidase) complete digestion to amino acids.
Amino Acid Absorption
Single amino acids absorbed via Na+-dependent transporters; di/tripeptides via H+/peptide co-transport, then hydrolyzed to amino acids.
All absorbed amino acids enter the hepatic portal vein to the liver.
Lipid Digestion
Stomach: Lingual and gastric lipases digest ~30% of triglycerides.
Small intestine: Bile salts emulsify fats; pancreatic lipase digests triglycerides to monoglycerides and fatty acids.
Lipid Absorption
Monoglycerides and fatty acids form micelles, enter epithelial cells by diffusion, are reassembled into triglycerides, and packaged as chylomicrons for lymphatic transport.
Nucleic Acid Digestion
Pancreatic nucleases and brush border enzymes break down nucleic acids to nucleotides, which are absorbed into the blood.
Water, Mineral, and Vitamin Absorption
Water: Absorbed by osmosis; most in small intestine, remainder in large intestine.
Minerals: Absorbed in small intestine; calcium absorption regulated by vitamin D, iron by hepcidin.
Vitamins: Fat-soluble (A, D, E, K) absorbed with micelles; water-soluble by diffusion or active transport; vitamin B12 requires intrinsic factor for absorption in the ileum.
Regulation of Blood Nutrient Levels
Fed (Absorptive) State
Occurs during and shortly after eating, when nutrients are being absorbed and stored. The hormone insulin is dominant, promoting nutrient storage and lowering blood glucose.
Stimulates glycogenesis, lipogenesis, and protein synthesis.
Fasting (Postabsorptive) State
Occurs between meals; glucagon is dominant, promoting nutrient mobilization and increasing blood glucose.
Stimulates glycogenolysis, gluconeogenesis, and lipolysis.
Endocrine System
Introduction to the Endocrine System
The endocrine system consists of glands that secrete hormones into the bloodstream to regulate various physiological processes. Hormones act on target cells with specific receptors and can have local or systemic effects.
Functions: Regulate development, metabolism, blood composition, digestion, and reproduction.
Major glands: Pituitary, pineal, thyroid, adrenal, and organs with endocrine tissue (e.g., pancreas, gonads).
Hormone Types and Transport
Steroid hormones: Lipid-soluble, derived from cholesterol.
Biogenic amines: Modified amino acids (e.g., catecholamines, thyroid hormone).
Proteins: Most hormones; water-soluble.
Local hormones (eicosanoids): Act locally (autocrine/paracrine).
Hormone Action on Target Cells
Lipid-soluble hormones: Cross membranes, bind intracellular receptors, alter gene expression.
Water-soluble hormones: Bind membrane receptors, activate second messenger pathways (e.g., cAMP, IP3/DAG).
Regulation of Hormone Levels
Controlled by feedback mechanisms (mostly negative feedback).
Biological half-life varies: lipid-soluble hormones last longer than water-soluble.
Hypothalamus and Pituitary Gland
Posterior pituitary (neurohypophysis): Stores and releases ADH and oxytocin made in the hypothalamus.
Anterior pituitary (adenohypophysis): Releases tropic hormones (e.g., GH, TSH, ACTH, FSH, LH, PRL) in response to hypothalamic releasing/inhibiting hormones.
Thyroid Gland
Composed of follicles (follicular cells and colloid) and parafollicular cells (produce calcitonin).
Thyroid hormone (T3, T4) increases metabolic rate, regulated by TRH (hypothalamus) and TSH (anterior pituitary).
Calcitonin lowers blood calcium by inhibiting osteoclasts and increasing renal excretion.
Adrenal Glands
Adrenal medulla: Releases epinephrine and norepinephrine (catecholamines) in response to sympathetic stimulation.
Adrenal cortex: Three zones—zona glomerulosa (mineralocorticoids, e.g., aldosterone), zona fasciculata (glucocorticoids, e.g., cortisol), zona reticularis (gonadocorticoids, e.g., androgens).
Cortisol increases blood nutrient levels, regulated by ACTH and negative feedback.
