Back
BackDigestive System Disorders and Gut Health: Structure, Function, and Clinical Perspectives
Study Guide - Smart Notes

Digestive System Overview
Structure and Function of the Digestive System
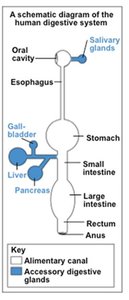
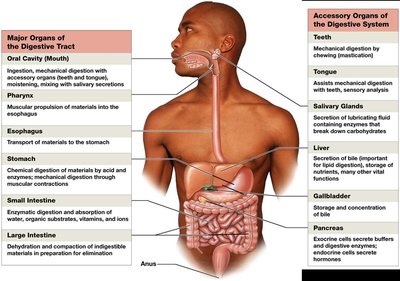
The human digestive system is a complex series of organs and glands that process food, extract nutrients, and eliminate waste. It consists of the alimentary canal (gastrointestinal tract) and accessory digestive organs.
Alimentary Canal: Includes the oral cavity, pharynx, esophagus, stomach, small intestine, large intestine, rectum, and anus.
Accessory Organs: Teeth, tongue, salivary glands, liver, pancreas, and gallbladder assist in digestion but are not part of the main tract.
Structure | Description/Functions | Mechanical Digestion | Chemical Digestion |
|---|---|---|---|
Mouth | Receives food; contains teeth and tongue; tongue manipulates food and monitors quality | Teeth tear and crush food into smaller pieces | Digestion of carbohydrates begins |
Pharynx | Passageway for food and air | None | None |
Esophagus | Tube that transports food from mouth to stomach | None | None |
Stomach | J-shaped muscular sac for food storage | Churning of stomach mixes food with gastric juice, creating chyme | Protein digestion begins |
Small intestine | Long tube where digestion is completed and nutrients are absorbed | Segmental contractions mix food with intestinal enzymes, pancreatic enzymes, and bile | Carbohydrate, protein, and fat digestion are completed |
Large intestine | Final tubular region of tract; absorbs water and electrolytes; forms and stores feces | None | Some digestion is carried out by bacteria |
Anus | Terminal outlet of digestive tract | None | None |
Stomach: Heartburn, GERD, and Ulcers
Stomach Structure and Function
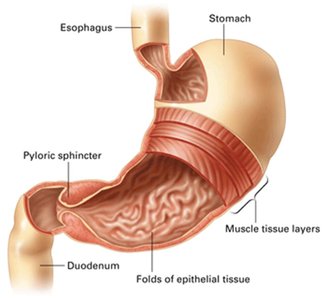
The stomach is a hollow, muscular organ that temporarily stores ingested food, mechanically digests it through muscular contractions, and chemically digests proteins with gastric juice (hydrochloric acid and enzymes).
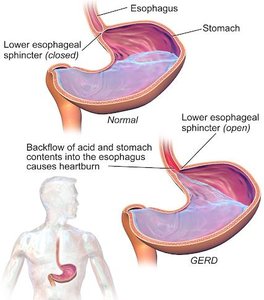
Heartburn and Gastroesophageal Reflux Disease (GERD)
Heartburn is a burning sensation in the chest caused by stomach acid refluxing into the esophagus, often due to a weak lower esophageal sphincter (LES). Chronic, frequent heartburn is termed GERD (Gastroesophageal Reflux Disease).
Symptoms: Burning pain, sour taste, hoarseness, trouble swallowing, coughing, nausea.
Risk Factors: Alcohol, obesity, smoking, pregnancy, certain foods (citrus, chocolate, caffeine, fatty foods), medications (aspirin, ibuprofen).
Complications: Esophageal ulcers, inflammation, bleeding, anemia, increased cancer risk, tooth decay, respiratory issues.
Treatment: Lifestyle changes (small, low-fat meals, avoid triggers, elevate bed, weight loss, stop smoking), medications (antacids, proton pump inhibitors).
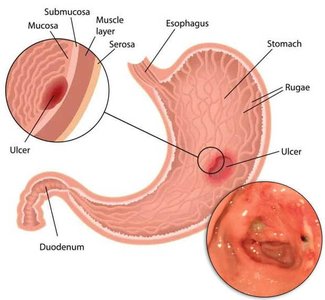
Stomach Ulcers
Stomach ulcers (gastric ulcers) are painful sores in the stomach lining caused by the breakdown of the protective mucus layer, allowing acid to damage tissue.
Symptoms: Burning stomach pain, fullness, bloating, intolerance to fatty foods, nausea, vomiting, weight loss. Some cases are asymptomatic.
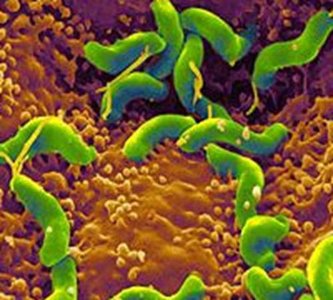
Causes: Helicobacter pylori infection (treated with antibiotics), long-term NSAID use (treated with acid-reducing medications).
Complications: Severe bleeding, perforation of the stomach wall.
Prevention: Avoid smoking, limit NSAIDs, moderate coffee/tea/alcohol/spices, eat regular nutritious meals, chew well, maintain healthy weight.
Liver and Gallbladder: NAFLD and Gallstones
Liver Structure and Function
The liver is a major metabolic organ responsible for detoxification, protein synthesis, carbohydrate metabolism, nutrient storage, and bile production for fat digestion.
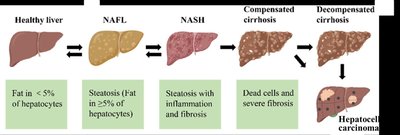
Nonalcoholic Fatty Liver Disease (NAFLD)
NAFLD is characterized by excessive fat accumulation in the liver, not due to alcohol use. It can progress to nonalcoholic steatohepatitis (NASH), cirrhosis, or liver cancer.
Risk Factors: Obesity, diabetes, high cholesterol, sleep apnea, polycystic ovary syndrome, hypothyroidism.
Symptoms: Often asymptomatic; may include fatigue, nausea, poor appetite, jaundice, right upper abdominal pain.
Treatment: Gradual weight loss, reduced calorie intake, avoid alcohol, nutritious diet.
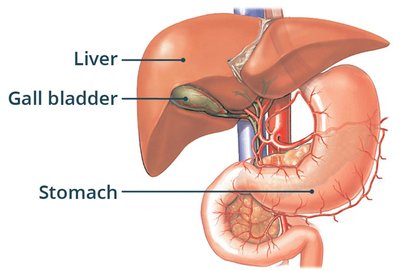
Gallbladder and Gallstones
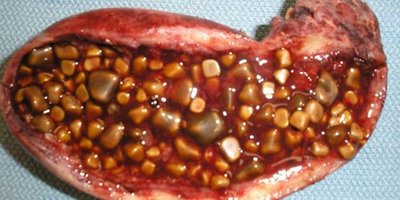
The gallbladder stores and concentrates bile, releasing it into the small intestine to aid fat digestion. Gallstones form when cholesterol and bile pigments crystallize.
Symptoms: Most are asymptomatic; biliary colic (right upper abdominal pain after fatty meals), pain radiating to right arm/shoulder, nausea, vomiting, bloating.
Prevention: Maintain healthy weight, avoid rapid weight loss, eat high-fiber and magnesium-rich foods, use unsaturated fats, exercise.
Complications: Cholecystitis (gallbladder inflammation), pancreatitis, bile duct infection; may require surgical removal of the gallbladder.
Small Intestine: Food Intolerance and Gluten-Related Diseases
Small Intestine Structure and Function
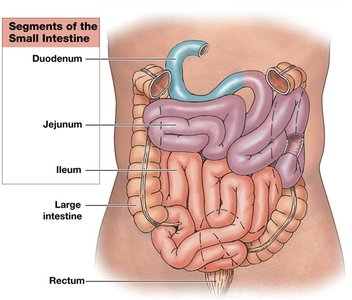
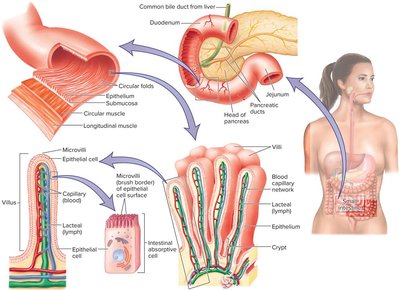
The small intestine is the main site for enzymatic digestion and nutrient absorption. It is lined with circular folds, villi, and microvilli to maximize surface area.
Segments: Duodenum, jejunum, ileum.
Absorption: Capillaries absorb proteins/carbohydrates; lacteals absorb fats.
Food Intolerances
Food intolerance is digestive distress due to inability to digest or absorb certain foods, or sensitivity to food chemicals. It does not involve the immune system (unlike allergies).
Symptoms: Bloating, gas, diarrhea, constipation, nausea, headaches, skin rashes.
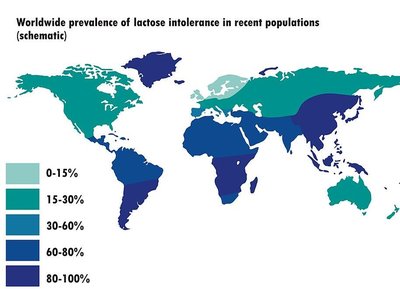
Lactose Intolerance
People with lactose intolerance lack the enzyme lactase, leading to undigested lactose in the colon, where bacteria ferment it, causing gas and diarrhea.
Symptoms: Diarrhea, nausea, vomiting, cramps, bloating, gas.
Genetics: The ability to digest lactose is due to a genetic mutation in some populations.
Gluten-Related Disorders
Non-celiac gluten sensitivity (NCGS) causes gastrointestinal and extraintestinal symptoms in response to gluten, but does not involve the immune system as in celiac disease.
Symptoms: Abdominal pain, bloating, diarrhea/constipation, nausea, headaches, fatigue, skin rash, depression.
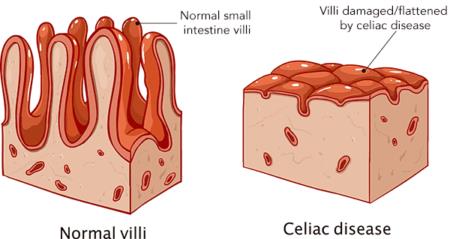
Celiac disease is an immune-mediated disorder triggered by gluten, leading to inflammation and destruction of intestinal villi, resulting in malabsorption and systemic symptoms.
Symptoms: GI symptoms (gas, bloating, diarrhea, constipation, pain), anemia, bone disorders, fatigue, dermatitis, neurological issues, infertility.
Pathology: Immune reaction damages villi, reducing nutrient absorption.
Large Intestine and Gut Microbiome
Large Intestine Structure and Function
The large intestine absorbs water, electrolytes, and vitamins, compacts waste into feces, and stores it for elimination. Digestion here is mainly due to bacterial action.
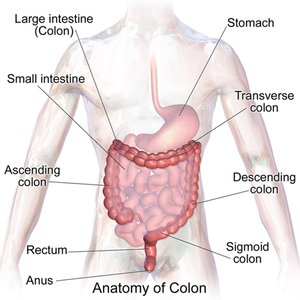
Gut Microbiome
The gut microbiome is the community of microorganisms in the large intestine, consisting of hundreds of species. It is influenced by age, diet, health, and environment.
Functions: Inhibit pathogens, digest undigested carbohydrates, synthesize vitamins (K, B7, B5), produce short-chain fatty acids, process waste, aid mineral absorption, regulate immune response.
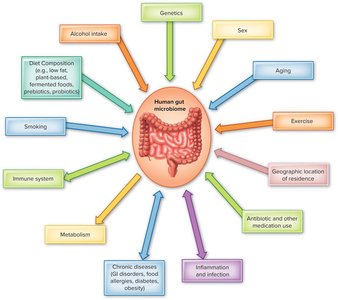
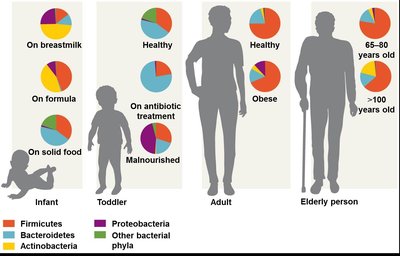
Microbiome-Gut-Brain Axis
Gut microorganisms produce neuroactive molecules that influence brain development and behavior. The gut-brain axis is a two-way biochemical signaling system between the gut and the central nervous system.
Clinical relevance: Probiotics (e.g., Bifidobacterium, Lactobacillus) may improve behavioral outcomes in some CNS disorders.
Probiotics and Prebiotics
Probiotics are live microorganisms that confer health benefits when consumed in adequate amounts. Prebiotics are non-digestible fibers that fuel beneficial gut bacteria, promoting a healthy microbiome.
Sources: Probiotics—yogurt, kefir, kimchi; Prebiotics—high-fiber foods.
Benefits: Support gut health, reduce inflammation, improve immune function.
Dysbiosis
Dysbiosis is an imbalance in the gut microbiota, with reduced beneficial bacteria or increased pathogens, often caused by poor diet, antibiotics, or stress. It leads to digestive issues and may require dietary intervention, probiotics, or fecal transplantation.
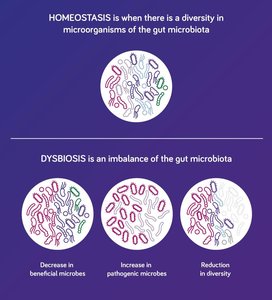
Common Digestive Disorders
Intestinal Gas (Flatus)
Intestinal gas is produced when bacteria ferment indigestible carbohydrates. Flatulence is normal but can be excessive in conditions like IBS or lactose intolerance.
Constipation
Constipation is defined as fewer than three bowel movements per week or passing hard, dry stools. Causes include dehydration, low fiber, inactivity, medications, and medical conditions. Prevention includes hydration, fiber, and exercise.
Diarrhea
Diarrhea is frequent, loose stools, often due to infection, food intolerance, or medications. It can cause dehydration and is a major global health issue, especially in children.

Irritable Bowel Syndrome (IBS)
IBS is a chronic functional disorder of the large intestine, causing abdominal pain, bloating, and alternating constipation or diarrhea. It is managed by dietary changes (low FODMAP diet), stress reduction, and medications.

Inflammatory Bowel Disease (IBD)
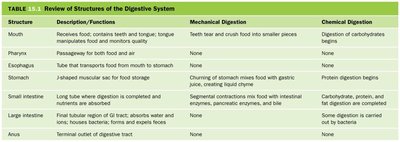
IBD includes Crohn’s disease and ulcerative colitis, which are chronic autoimmune conditions causing inflammation of the digestive tract. Symptoms include diarrhea, pain, bleeding, fatigue, and weight loss. Crohn’s can affect any part of the GI tract; ulcerative colitis is limited to the colon.
Ulcerative colitis: Continuous inflammation of the colon’s inner lining.
Crohn’s disease: Patchy inflammation, can affect all layers of the bowel wall.