 Back
BackDigestive System: Pancreas, Small Intestine, and Large Intestine
Study Guide - Smart Notes

The Pancreas
Anatomy and Function
The pancreas is a glandular organ located deep to the stomach, extending from the spleen (tail) to the duodenum (head). It is situated in the retroperitoneal area and plays a crucial role in both the digestive and endocrine systems.
Exocrine function: The majority of the pancreas consists of exocrine tissue (acini), which produces pancreatic juice containing digestive enzymes.
Endocrine function: The islets of Langerhans secrete hormones such as insulin and glucagon, regulating blood glucose levels.
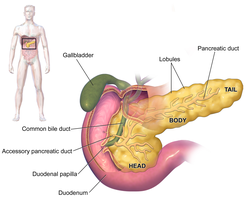
Pancreatic Juice
Pancreatic juice is essential for chemical digestion in the small intestine. It is composed of water, digestive enzymes, and electrolytes (mainly bicarbonate ions), making it alkaline (pH ~8).
Bicarbonate ions (HCO3-): Secreted by duct cells, neutralize acidic chyme from the stomach.
Enzymes: Secreted by acinar cells, include:
Proteases (e.g., trypsinogen, chymotrypsinogen, procarboxypeptidase): Digest proteins; secreted as inactive zymogens.
Amylases: Digest carbohydrates.
Lipases: Digest lipids.
Nucleases: Digest nucleic acids.
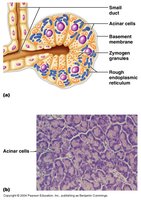
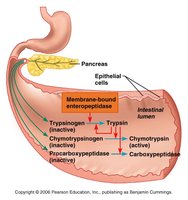
Protease Activation
Proteases are secreted in inactive forms to prevent autodigestion. Activation occurs in the small intestine:
Trypsinogen is activated to trypsin by membrane-bound enterokinase (enteropeptidase) in the intestinal mucosa.
Trypsin then activates other proteases (chymotrypsinogen and procarboxypeptidase).
Pancreatic Disorders
Pancreatitis: Inflammation of the pancreas, often due to duct blockage (gallstones) or alcohol, leading to premature enzyme activation and autodigestion.
Pancreatic cancer: Highly aggressive and difficult to treat; removal of the pancreas requires lifelong enzyme replacement.
The Small Intestine
Gross Anatomy and Function
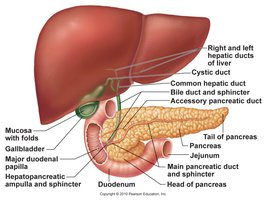
The small intestine (SI) is the major site for digestion and absorption of nutrients. It is a long, convoluted tube extending from the pyloric sphincter to the ileocecal valve and consists of three sections: duodenum, jejunum, and ileum.
Duodenum: Receives chyme from the stomach, bile from the liver/gallbladder, and pancreatic juice.
Jejunum and Ileum: Main sites for nutrient absorption; suspended by the mesentery.
Blood supply: Superior mesenteric artery; venous drainage via the hepatic portal vein.
Microscopic Anatomy
The mucosa of the small intestine is highly specialized for absorption, featuring several adaptations to increase surface area:
Circular folds (plicae circulares): Permanent folds that slow chyme movement and increase absorption time.
Villi: Fingerlike projections lined with absorptive columnar epithelial cells; each villus contains a capillary bed and a lacteal (lymphatic capillary).
Microvilli: Tiny extensions of the epithelial cell membrane, forming the brush border with enzymes for final digestion.
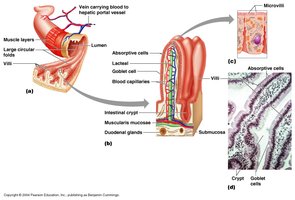
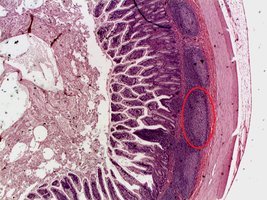
Histology
Mucosa: Simple columnar epithelium with absorptive cells and goblet cells.
Submucosa: Contains Brunner’s glands (secrete alkaline mucus) and Peyer’s patches (lymphoid follicles for immune defense).
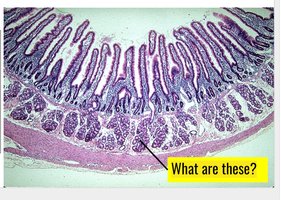
Digestion and Absorption of Nutrients
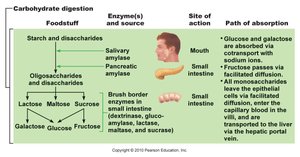
Carbohydrate Digestion
Carbohydrates are primarily digested into monosaccharides for absorption.
Starch digestion begins in the mouth (salivary amylase), pauses in the stomach, and resumes in the small intestine (pancreatic amylase).
Brush-border enzymes (e.g., sucrase, lactase, maltase) complete digestion to monosaccharides (glucose, fructose, galactose).
Monosaccharides are absorbed via cotransport with sodium ions or facilitated diffusion.
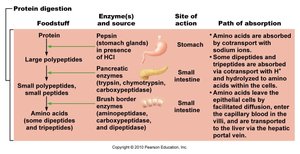
Protein Digestion
Proteins are digested into amino acids, which are absorbed by the small intestine.
Begins in the stomach (pepsin), continues in the small intestine (pancreatic proteases: trypsin, chymotrypsin, carboxypeptidase).
Brush-border enzymes (aminopeptidase, dipeptidase) complete digestion to amino acids.
Amino acids are absorbed via cotransport with sodium ions or facilitated diffusion.
Lipid Digestion and Absorption
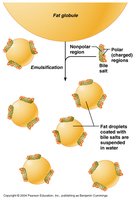
Lipid digestion primarily occurs in the small intestine, aided by bile salts and pancreatic lipases.
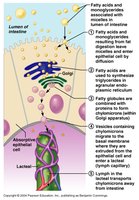
Triglycerides are emulsified by bile salts, then hydrolyzed by pancreatic lipases into monoglycerides and free fatty acids.
Products form micelles, which transport lipids to the intestinal epithelium for absorption.
Inside cells, triglycerides are reassembled and packaged into chylomicrons, which enter lacteals and the lymphatic system.
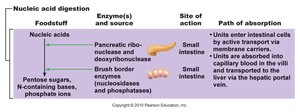
Nucleic Acid Digestion
Nucleic acids are digested by pancreatic nucleases and brush-border enzymes into pentose sugars, phosphate ions, and nitrogenous bases, which are absorbed by active transport.
Micromolecule Absorption
Calcium: Absorbed in the duodenum, regulated by parathyroid hormone (PTH) and vitamin D3 (calcitriol).
Iron: Absorbed in the duodenum, stored as ferritin, and transported by transferrin as needed.
Vitamin B12: Absorbed in the ileum, requires intrinsic factor for absorption.
Water Absorptive Imbalances
Diarrhea: Caused by reduced water reabsorption or increased water entry, leading to dehydration and electrolyte imbalance.
Constipation: Difficult or infrequent stool passage, often due to reduced GI motility.
The Large Intestine
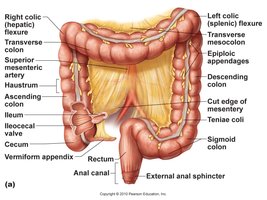
Gross Anatomy and Function
The large intestine (LI) extends from the ileocecal valve to the anus and is responsible for water reabsorption and feces elimination. It includes the cecum, appendix, colon, rectum, and anal canal.
Haustra: Pouches formed by the teniae coli (longitudinal muscle bands).
Appendix: Lymphoid tissue, reservoir for beneficial bacteria.
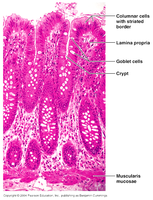
Microscopic Anatomy
Mucosa: Simple columnar epithelium, transitions to stratified squamous at the recto-anal junction.
Goblet cells: Abundant, secrete mucus for lubrication.
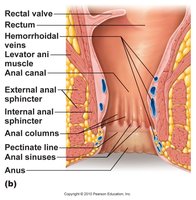
Terminal Anatomy
The anal canal is the terminal part of the GI tract, featuring the pectinate (dentate) line, internal (involuntary) and external (voluntary) anal sphincters, and venous plexuses (site of hemorrhoids).
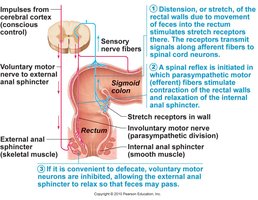
Motility and Defecation Reflex
Haustral contractions: Slow, segmenting movements that mix and promote water reabsorption.
Mass movements: Powerful peristaltic waves, often after meals.
Defecation reflex: Triggered by rectal wall stretching, involves both involuntary (internal sphincter) and voluntary (external sphincter) control.
Bacterial Flora
Resident bacteria metabolize residual matter, synthesize B vitamins and most of the body's vitamin K.
Symbiotic relationship: mutualists and commensals.
Common Disorders
Inflammatory Malabsorption: Caused by infections (bacterial, viral, parasitic) or immune disorders (celiac disease, Crohn’s disease).
Diverticulosis: Formation of mucosal outpouchings (diverticula), risk increases with age and low-fiber diet; can lead to diverticulitis and peritonitis.
Colon Cancer: Often arises from mucosal lining, associated with low-fiber, high red meat diets; treated with surgery, chemotherapy, and radiation.
Digestive System Overview Tables
Digestive Overview
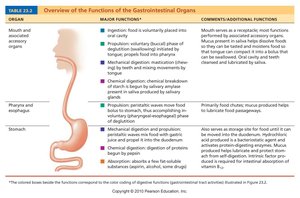
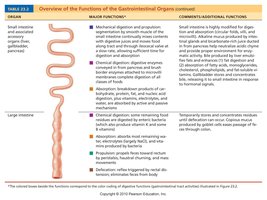
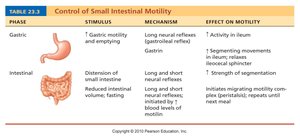
Control of Small Intestinal Motility

