 Back
BackDigestive System: Stomach, Liver, Gallbladder, and Pancreas
Study Guide - Smart Notes

Digestive System: Stomach, Liver, Gallbladder, and Pancreas
Pharynx and Esophagus
The pharynx and esophagus are essential conduits in the digestive system, responsible for moving food from the mouth to the stomach. The pharynx allows passage of food, fluids, and air, while the esophagus is a muscular tube that propels food via coordinated muscle contractions.
Pharynx: Food passes from the mouth into the oropharynx and then into the laryngopharynx.
Esophagus: Collapsed when not involved in food propulsion; runs from laryngopharynx to stomach.
Major function: Propulsion, starting with deglutition (swallowing), which involves coordination of 22 muscle groups and occurs in 2-3 phases.
Heartburn and Gastroesophageal Reflux Disease (GERD)
Heartburn is caused by stomach acid regurgitating into the esophagus, often the first symptom of GERD. It can result from excess food/drink, obesity, pregnancy, or physical activity.
Symptoms: Burning sensation in the chest.
Causes: Stomach acid entering the esophagus.
The Stomach: Structure and Function
The stomach is a temporary storage tank that initiates the chemical breakdown of proteins. It converts the bolus of food into a paste-like substance called chyme. The stomach can expand from a volume of ~50 ml when empty to up to 4 L when full. The mucosa forms folds called rugae when empty.
Major regions: Cardia, fundus, body, pyloric part (including pyloric canal and pylorus).
Pylorus: Continuous with the duodenum through the pyloric sphincter (valve).
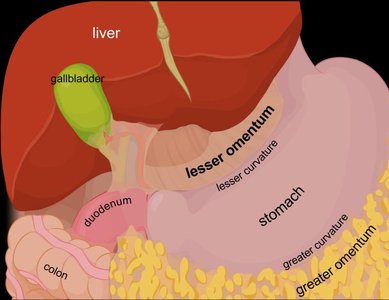
Curvatures: Greater curvature (lateral), lesser curvature (medial).
Mesenteries: Lesser omentum (connects lesser curvature to liver), greater omentum (drapes from greater curvature over intestines).


Modified Stomach Layers
The stomach wall contains four layers, with modifications in the muscularis and mucosa. The muscularis externa has three layers: longitudinal, circular, and an extra inner oblique layer, which increases the physical breakdown of food.
Muscularis externa: Longitudinal, circular, and oblique layers allow churning, mixing, and pummeling of chyme.
Mucosa: Simple columnar epithelium composed entirely of mucous cells, secreting a two-layer coat of alkaline mucus.
Gastric pits: Lead into gastric glands that produce gastric juice.

Microscopic Anatomy of the Stomach
Gastric glands in the fundus and body produce most gastric juice and contain several types of secretory cells:
Mucous neck cells: Secrete thin, acidic mucus.
Parietal cells: Secrete hydrochloric acid (HCl) and intrinsic factor for vitamin B12 absorption.
Chief cells: Secrete pepsinogen (inactive enzyme activated to pepsin by HCl) and lipases.
Enteroendocrine cells: Secrete hormones into the lamina propria.

Gastric Secretions and Regulation
The stomach produces over 3 L of gastric juice per day, regulated by neural and hormonal mechanisms. Gastric secretions occur in three phases:
Cephalic (reflex) phase: Triggered by aroma, taste, sight, or thought of food.
Gastric phase: Lasts 3–4 hours; stimulated by food entry, chemical stimuli, and gastrin release.
Intestinal phase: Begins with a brief stimulatory component, followed by inhibition as chyme enters the duodenum.
Neural regulation: Vagus nerve increases secretion; sympathetic stimulation decreases secretion.
Hormonal regulation: Gastrin stimulates enzyme and HCl secretion; antagonists from the small intestine inhibit secretion.
Digestive Processes in the Stomach
The stomach carries out several key digestive processes:
Breakdown of food
Serves as a holding area for food
Delivers chyme to the small intestine
Denatures proteins by HCl
Pepsin carries out enzymatic digestion of proteins
Lipid-soluble alcohol and aspirin are absorbed into the blood
Secretion of intrinsic factor for vitamin B12 absorption (essential for red blood cell maturation)
Protection of the Stomach: Mucosal Barrier
The stomach is protected from harsh digestive conditions by a mucosal barrier, which consists of:
Thick layer of base-rich mucus
Tight junctions between epithelial cells to prevent juice seeping underneath tissue
Rapid replacement of damaged epithelial cells by stem cell division (surface cells replaced every 3–6 days)
Regulation of Gastric Motility and Emptying
The stomach stretches to accommodate incoming food, with pressure remaining constant until about 1.5 L is ingested. Gastric contractile activity involves peristaltic waves moving toward the pylorus, with contractions most vigorous near the pylorus region. Only liquids and small particles pass through the pyloric valve.
Gastric emptying: Controlled by the duodenum to prevent overfilling; typically occurs in ~4 hours, but fatty chyme can increase this time.
Liver, Gallbladder, and Pancreas: Accessory Digestive Organs
The liver, gallbladder, and pancreas are accessory organs associated with the small intestine. The liver produces bile, the gallbladder stores and concentrates bile, and the pancreas supplies most of the digestive enzymes and bicarbonate to neutralize stomach acid.
Liver: Largest gland in the body; produces bile for fat emulsification.
Gallbladder: Stores and concentrates bile; releases it via the cystic duct.
Pancreas: Produces pancreatic juice containing digestive enzymes and bicarbonate.
Liver Structure and Function
The liver is composed of hexagonal lobules made of plates of hepatocytes. Each lobule contains a portal triad (branch of hepatic artery, branch of hepatic portal vein, and bile duct). Blood from both sources filters through sinusoids and empties into the central vein. Stellate macrophages remove debris and old RBCs.
Hepatocyte functions: Produce bile, process nutrients, store vitamins, detoxify blood, and synthesize plasma proteins.
Bile: Yellow-green, alkaline solution containing bile salts, bilirubin, cholesterol, triglycerides, phospholipids, and electrolytes.
Enterohepatic circulation: Recycles bile salts; about 95% are reused.
Homeostatic Imbalances of the Liver
Hepatitis: Usually caused by viral infection, drug toxicity, or poisoning.
Cirrhosis: Chronic inflammation from hepatitis or alcoholism; can lead to liver failure.
Liver regeneration: Can regenerate to full size in 6–12 months after 80% removal.
Gallbladder: Structure and Function
The gallbladder is a thin-walled muscular sac that stores and concentrates bile. It releases bile via the cystic duct into the bile duct. Gallstones can form from excess cholesterol or too few bile salts, causing pain and possible jaundice.
Pancreas: Structure and Function
The pancreas is mostly retroperitoneal and produces pancreatic juice, which contains digestive enzymes and bicarbonate. Enzymes include proteases (for proteins), amylase (for carbohydrates), lipases (for lipids), and nucleases (for nucleic acids). Proteases are secreted in inactive forms to prevent self-digestion.
Regulation of Bile and Pancreatic Secretions
Bile and pancreatic juice secretions are regulated by neural and hormonal controls. Hormones include cholecystokinin (CCK) and secretin, which stimulate the release of bile and pancreatic juice into the duodenum.
CCK: Stimulates gallbladder contraction and secretion of enzyme-rich pancreatic juice.
Secretin: Stimulates secretion of bicarbonate-rich pancreatic juice.
Vagus nerve: Weakly stimulates during cephalic and gastric phases.
Summary Table: Digestive Functions of Stomach, Liver, Gallbladder, and Pancreas
Organ | Main Function | Key Secretions |
|---|---|---|
Stomach | Protein digestion, food storage, chyme formation | Gastric juice (HCl, pepsinogen, mucus, intrinsic factor) |
Liver | Bile production, nutrient processing, detoxification | Bile (bile salts, bilirubin) |
Gallbladder | Bile storage and concentration | Bile |
Pancreas | Enzyme and bicarbonate secretion | Pancreatic juice (proteases, amylase, lipases, nucleases, HCO3-) |
Key Equations and Concepts
Protein digestion: Pepsinogen (inactive) + HCl → Pepsin (active)
Bicarbonate neutralization:
Additional info:
Some images in the original file are humorous or pop culture references and are not included, as they do not directly reinforce the academic content.
All included images are anatomical diagrams directly relevant to the explanation of the digestive system.
