 Back
BackDigestive System: Structure, Function, and Regulation
Study Guide - Smart Notes

Digestive System Overview
Major Components and Functions
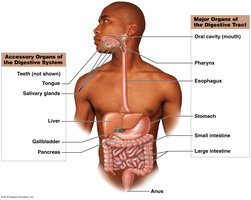
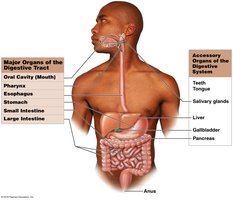
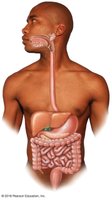
The digestive system is responsible for providing nutrients essential for cell maintenance and growth. It consists of the digestive tract (gastrointestinal or GI tract) and accessory organs. The digestive tract is a muscular tube extending from the mouth to the anus, while accessory organs secrete products into the digestive tract to aid in digestion.
Digestive Tract: Oral cavity, pharynx, esophagus, stomach, small intestine, large intestine, anus
Accessory Organs: Salivary glands, liver, gallbladder, pancreas
Histology of the Digestive Tract
Layers of the Digestive Tract
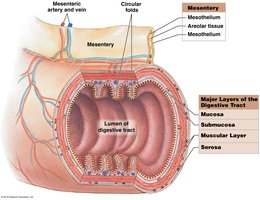
The digestive tract is a long muscular tube lined by a mucous membrane. It features permanent ridges and temporary folds to increase surface area for nutrient absorption. There are four major layers, from inside to outside:
Mucosa: Inner lining, consists of epithelium moistened by glandular secretions and lamina propria (areolar tissue)
Submucosa: Dense irregular connective tissue containing blood vessels, lymphatics, and exocrine glands
Muscularis: Smooth muscle in two layers (inner circular, outer longitudinal) for mechanical processing and movement
Serosa: Visceral peritoneum that attaches the tract to adjacent structures (not present above the stomach or from rectum down)
Mesenteries
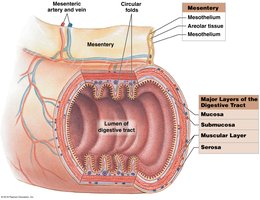
Mesenteries are double sheets of peritoneal membrane that stabilize attached organs and prevent entanglement of the intestines. They provide a route for blood vessels, nerves, and lymphatics.
Mucosa and Surface Specializations
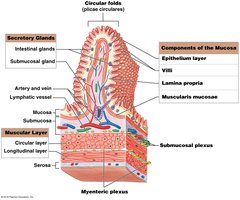
The mucosal epithelium varies by region: stratified squamous at the beginning and end, simple columnar with goblet cells in the stomach and intestines. The small intestine features villi and circular folds (plicae circulares) to increase surface area for absorption.
Villi: Fingerlike projections in the small intestine
Lamina propria: Areolar connective tissue with vessels and nerves
Muscularis mucosae: Smooth muscle layers that change the shape of the lumen
Nerve Plexuses
Local control of digestive activities is mediated by nerve plexuses:
Submucosal plexus: Innervates mucosa and submucosa, contains sensory neurons and autonomic fibers
Myenteric plexus: Located between muscle layers, coordinates muscle contractions
Smooth Muscle in the Digestive Tract
Structure and Function
Smooth muscle forms sheets, bundles, or sheaths around tissues and is organized into inner circular and outer longitudinal layers in the digestive tract. Sphincters regulate movement along passageways.
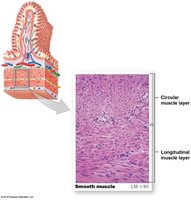
Smooth Muscle Cell Characteristics
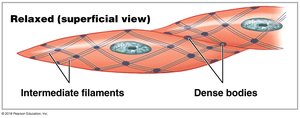
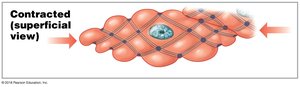
Smooth muscle cells are long and slender, with actin and myosin filaments organized differently than in skeletal or cardiac muscle. Thin filaments attach to dense bodies, and contraction causes the cell to twist like a corkscrew.
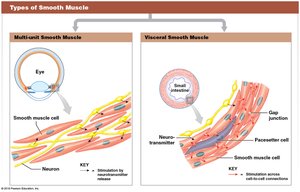
Types of Smooth Muscle
Multi-unit smooth muscle: Each cell innervated individually (e.g., iris, arrector pili)
Visceral smooth muscle: Electrically connected by gap junctions, contract as a unit (e.g., digestive tract walls)
Motility of the Digestive Tract
Peristalsis
Peristalsis is a wave of muscle contraction that propels a bolus (moist, compact mass of food) along the digestive tract.
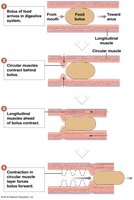
Segmentation
Segmentation involves cycles of contraction that churn and fragment the bolus, mixing it with intestinal secretions. This process occurs mainly in the small and some of the large intestine and does not move contents in a set direction.
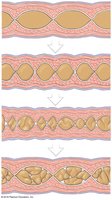
Regulation of Digestive Activities
Local, Neural, and Hormonal Mechanisms
Local factors: Changes in pH, stretch, and chemical composition stimulate digestive activities
Neural mechanisms: Short reflexes (myenteric) and long reflexes (CNS involvement)
Hormonal mechanisms: At least 18 hormones produced by enteroendocrine cells regulate digestive function
Anatomy and Functions of the Digestive Tract Organs
Major Organs and Their Functions
Oral cavity: Mechanical processing, moistening, mixing with saliva
Pharynx: Muscular propulsion of food into esophagus
Esophagus: Transports materials to the stomach
Stomach: Chemical breakdown and mechanical processing
Small intestine: Enzymatic digestion and absorption (most digestion and absorption occur here)
Large intestine: Dehydration and compaction of indigestible materials
Digestive Processes
Ingestion: Entry of food and liquid into the oral cavity
Mechanical digestion and propulsion: Crushing, shredding, mixing, and churning of food
Chemical digestion: Breakdown of food into small organic molecules
Secretion: Release of water, acids, enzymes, buffers, and salts
Absorption: Movement of nutrients into the bloodstream
Defecation: Elimination of indigestible food as feces
Anatomy of the Oral Cavity
Boundaries and Structures
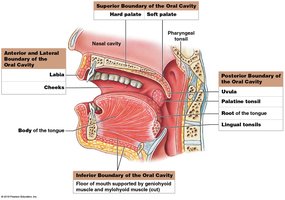
The oral cavity contains the tongue, teeth, and gums, and is lined by oral mucosa. The roof is formed by the hard and soft palate, while the cheeks, lips, and tongue form the other boundaries. The fauces is the space between the oral cavity and oropharynx.
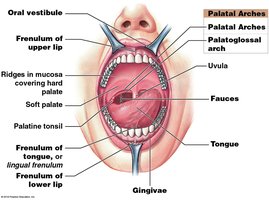
Teeth: Structure and Types
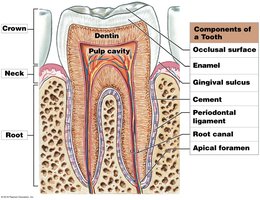
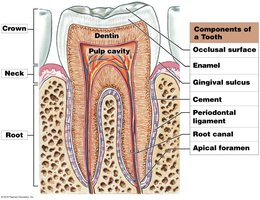
Regions and Components of a Tooth
Crown: Projects into the oral cavity
Neck: Boundary between crown and root
Root: Sits in the bony tooth socket (alveolus)
Pulp cavity: Contains vessels and nerves
Dentin: Mineralized matrix similar to bone
Enamel: Hardest biological substance, covers crown
Cement: Covers dentin in root
Periodontal ligament: Connects root to alveolar bone
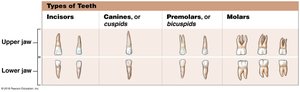
Types of Teeth
Type | Shape | Function |
|---|---|---|
Incisors | Blade-shaped, single root | Clipping or cutting |
Canines (Cuspids) | Conical, pointed tip, single root | Tearing/slashing |
Premolars (Bicuspids) | Flattened crowns, 1-2 roots | Crushing, mashing, grinding |
Molars | Large, flattened crowns, 2-3 roots | Crushing, grinding |
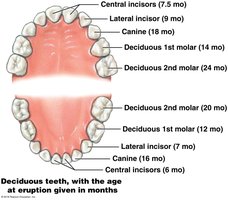
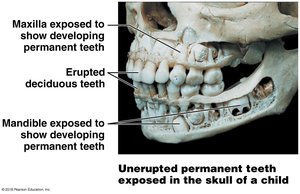
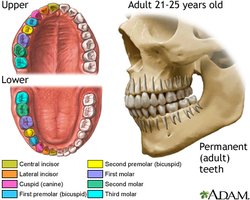
Deciduous and Permanent Teeth
Deciduous teeth: 20 primary teeth, appear by age 2
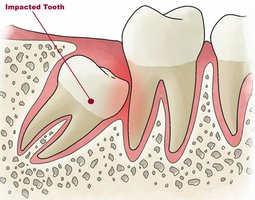
Permanents teeth: 32 adult teeth, replace deciduous teeth, include wisdom teeth (third molars)
Pharynx and Esophagus
Pharynx
The pharynx is a membrane-lined cavity posterior to the nose and mouth, serving as a common passageway for food, liquids, and air. It has three regions: nasopharynx, oropharynx, and laryngopharynx.
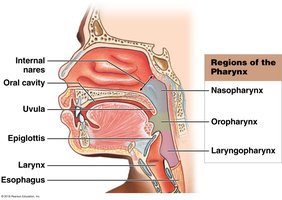
Esophagus
The esophagus is a hollow, muscular tube that actively moves food and liquids to the stomach. It features upper and lower esophageal sphincters to regulate entry and prevent backflow.
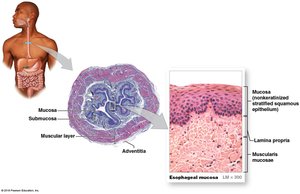
Swallowing (Deglutition)
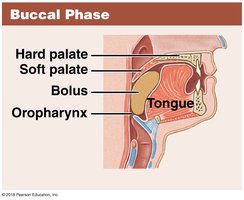
Swallowing is initiated voluntarily but proceeds automatically through three phases:
Buccal phase: Voluntary, tongue pushes bolus into oropharynx
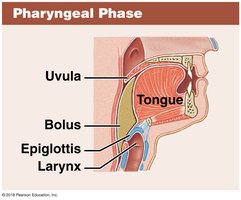
Pharyngeal phase: Reflex, bolus moves through pharynx as larynx elevates and epiglottis folds
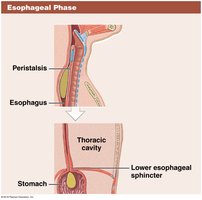
Esophageal phase: Peristalsis pushes bolus toward stomach
Peritoneum and Mesenteries
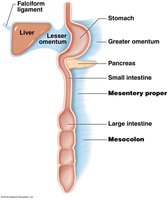
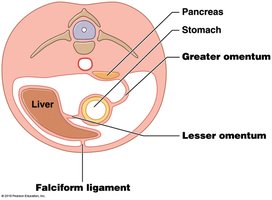
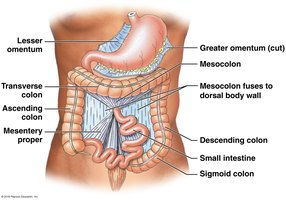
Peritoneal Cavity and Mesenteries
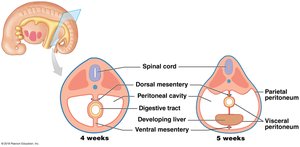
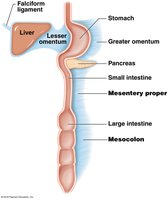
The peritoneum is a serous membrane that encloses the stomach and most of the intestines. Mesenteries are formed during embryonic development and suspend the digestive tract and accessory organs, providing support and routes for vessels and nerves.
Stomach Anatomy and Function
Regions and Structure
The stomach is a muscular, expandable, J-shaped organ with three muscle layers (longitudinal, circular, oblique) that aid in mixing and churning food to form chyme. It has four regions: cardia, fundus, body, and pylorus.
Histology and Secretions
Mucosa: Simple columnar epithelium, produces alkaline mucus
Gastric glands: Contain parietal cells (secrete HCl and intrinsic factor), chief cells (secrete pepsinogen), and G cells (secrete hormones)
Gastric juice: About 1.5 L produced per day
Small Intestine: Structure and Function
Surface Specializations
The small intestine is specialized for absorption, with circular folds (plicae circulares), villi, and microvilli increasing surface area. Intestinal glands and Paneth cells contribute to immunity and secretion.
Segments of the Small Intestine
Duodenum: 25 cm, receives chyme and digestive secretions, neutralizes acid
Jejunum: 2.5 m, major site of digestion and absorption
Ileum: 3.5 m, ends at ileocecal valve, contains lymphoid nodules
Hormonal Regulation of Digestion
Major Digestive Hormones
Gastrin: Increases gastric secretion and motility
Secretin: Increases pancreatic buffer secretion, bile release, slows gastric activity
Gastric Inhibitory Peptide (GIP): Slows gastric activity, triggers insulin release
Cholecystokinin (CCK): Increases pancreatic enzyme secretion, bile release
Vasoactive Intestinal Peptide (VIP): Stimulates intestinal secretion, inhibits stomach acid
Enterocrinin: Increases alkaline mucus secretion in duodenum
Large Intestine: Structure and Function
Segments and Functions
Cecum: Receives material from ileum, begins compaction
Colon: Four regions (ascending, transverse, descending, sigmoid), compacts and stores feces
Rectum: Temporary storage, triggers defecation
Histology and Absorption
No villi, abundant goblet cells for mucus secretion
Water reabsorption is the main function
Vitamin absorption: Biotin, vitamin K, and B5 produced by bacteria
Defecation Reflex
The defecation reflex is triggered by distension of the rectal wall and involves both long (parasympathetic) and short (myenteric) reflexes to coordinate mass movements and relaxation of sphincters.
Accessory Digestive Organs
Salivary Glands
Parotid: Serous secretion, salivary amylase
Submandibular: Mixed secretion, most saliva production
Sublingual: Mucous secretion, buffer/lubricant
Liver
The liver is the largest visceral organ, divided into four lobes (right, left, caudate, quadrate). It performs nearly 200 functions, including bile production, metabolism, and detoxification.
Liver Histology
Liver lobules: Hexagonal units with hepatocytes, sinusoids, and portal triads (branch of hepatic portal vein, hepatic artery, bile duct)
Stellate macrophages (Kupffer cells): Engulf pathogens and debris
Gallbladder
The gallbladder stores and concentrates bile produced by the liver. Bile is released into the duodenum to emulsify fats, increasing the surface area for digestive enzymes.
Pancreas
The pancreas has both exocrine (digestive enzyme and buffer secretion) and endocrine (insulin and glucagon) functions. Pancreatic juice contains enzymes for digestion of carbohydrates, proteins, lipids, and nucleic acids.
Clinical Considerations: Digestive System Disorders
Common Disorders
Periodontal disease: Inflammation and breakdown of gums and bone
Mumps: Viral infection of salivary glands
Esophagitis and GERD: Inflammation and acid reflux
Hepatitis and cirrhosis: Inflammation and scarring of the liver
Gallstones and cholecystitis: Crystallization and inflammation in the gallbladder
Gastritis and peptic ulcers: Inflammation and erosion of stomach/duodenal lining (often due to Helicobacter pylori)
Pancreatitis: Inflammation and self-digestion of the pancreas
Enteritis, dysentery, gastroenteritis: Inflammation of intestines, often infectious
Colitis, constipation, colorectal cancer: Disorders of the large intestine
Additional info: This guide covers the anatomy, histology, physiology, and clinical relevance of the digestive system, suitable for ANP college-level study.
