 Back
BackEfferent Division: Autonomic and Somatic Motor Control – Study Notes
Study Guide - Smart Notes

Chapter 12: Efferent Division – Autonomic and Somatic Motor Control
Overview of the Efferent Division
The efferent division of the peripheral nervous system (PNS) transmits commands from the central nervous system (CNS) to muscles and glands. It is divided into the somatic motor division and the autonomic division, each with distinct roles in regulating body functions and maintaining homeostasis.
Somatic motor division: Controls voluntary movements of skeletal muscles.
Autonomic division: Regulates involuntary functions of smooth muscle, cardiac muscle, glands, and some adipose tissue.
Core Concepts
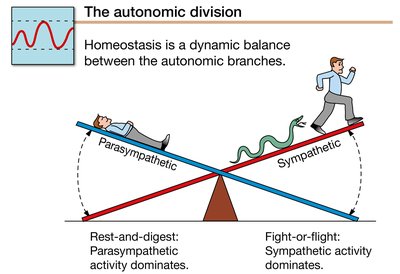
Homeostasis: The autonomic division is primarily responsible for maintaining homeostasis, while the somatic division contributes to thermoregulation.
Communication: Efferent pathways use both electrical and chemical signaling. Communication between neurons and their targets is primarily chemical, involving neurotransmitters and receptors.
Molecular Interactions: The effects of efferent neurons are determined by the interaction between neurotransmitters and their specific receptors on target tissues.



The Autonomic Division
Subdivisions of the Autonomic Division
The autonomic division is divided into two main branches, each with distinct anatomical and functional characteristics:
Sympathetic branch: Prepares the body for 'fight-or-flight' responses.
Parasympathetic branch: Promotes 'rest-and-digest' activities.
These branches are best distinguished by their activity during different physiological states and their anatomical origins.

Autonomic Reflexes and Homeostasis
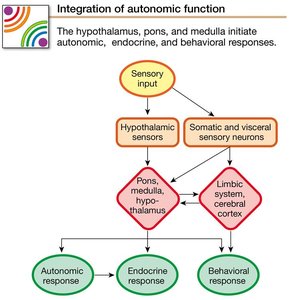
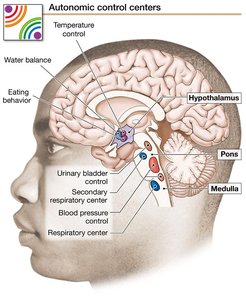
Autonomic reflexes are essential for maintaining homeostasis and often work in conjunction with the endocrine and behavioral state systems. Sensory information from somatosensory and visceral receptors is integrated in the hypothalamus, pons, and medulla, which serve as homeostatic control centers. Motor output from these centers leads to autonomic, endocrine, and behavioral responses.
Some autonomic reflexes are integrated at the spinal cord level (spinal reflexes).
Emotional states, processed in the cortex and limbic system, can influence autonomic output.
Antagonistic and Cooperative Control
Most internal organs receive antagonistic control from both sympathetic and parasympathetic branches, where one branch is excitatory and the other inhibitory. Some organs, such as sweat glands and most blood vessels, receive only sympathetic innervation (tonic control). Cooperative control occurs when both branches work together to achieve a common physiological goal.
The response of a target tissue is often determined by the type of neurotransmitter receptor present.
Anatomy of Autonomic Pathways
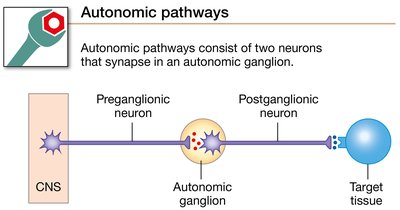
Autonomic pathways consist of two efferent neurons in series:
Preganglionic neuron: Cell body in the CNS; projects to an autonomic ganglion.
Postganglionic neuron: Cell body in the autonomic ganglion; projects to the target tissue.
Ganglion: A cluster of neuronal cell bodies outside the CNS, serving as mini-integration centers.
Sympathetic vs. Parasympathetic Anatomy
Sympathetic: Originates in thoracic and lumbar spinal cord; ganglia are close to the spinal cord.
Parasympathetic: Originates in the brainstem and sacral spinal cord; ganglia are on or near target organs.
Vagus nerve: Contains about 75% of all parasympathetic fibers, carrying sensory information from organs to the brain and motor output from the brain to organs.
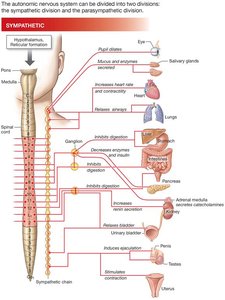
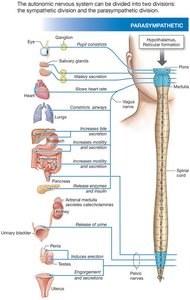
Functional Comparison of Sympathetic and Parasympathetic Responses
The sympathetic and parasympathetic divisions often innervate the same organs but produce opposing effects. The following tables summarize these effects:
Effector Organ | Sympathetic Response | Adrenergic Receptor | Parasympathetic Response |
|---|---|---|---|
Pupil of eye | Dilates | Alpha | Constricts |
Salivary glands | Mucus, enzymes | Alpha, Beta2 | Watery secretion |
Heart | Increases rate and force | Beta1 | Slows rate |
Lungs | Bronchioles dilate | Beta2 | Bronchioles constrict |
Digestive tract | Decreases motility/secretion | Alpha, Beta2 | Increases motility/secretion |
Urinary bladder | Urinary retention | Alpha, Beta2 | Release of urine |
Additional info: All parasympathetic responses are mediated by muscarinic receptors.
Chemical Signaling in the Autonomic Nervous System
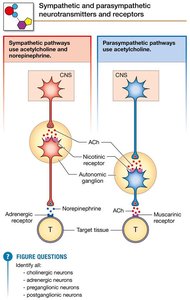
Both sympathetic and parasympathetic preganglionic neurons release acetylcholine (ACh) onto nicotinic cholinergic receptors (nAChR) on postganglionic cells.
Most postganglionic sympathetic neurons secrete norepinephrine (NE) onto adrenergic receptors on target cells.
Most postganglionic parasympathetic neurons secrete ACh onto muscarinic cholinergic receptors (mAChR) on target cells.
Exceptions include sympathetic cholinergic neurons (e.g., sweat glands) and nonadrenergic, noncholinergic neurons.
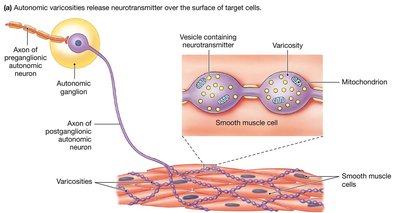
Neuroeffector Junctions and Varicosities
The neuroeffector junction is the synapse between a postganglionic autonomic neuron and its target cell. Neurotransmitters are released from swellings called varicosities along the axon, allowing widespread and diffuse signaling.
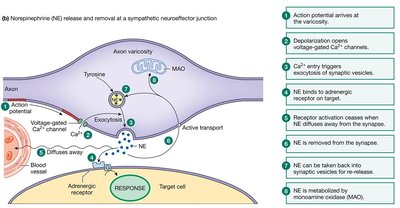
Autonomic Receptors and Signal Transduction
All autonomic receptors are G protein-coupled receptors.
Adrenergic receptors:
Alpha (α) receptors: Strongly respond to NE; α1 cause muscle contraction or secretion, α2 decrease cAMP and cause smooth muscle relaxation.
Beta (β) receptors: β1 respond equally to NE and E; β2 more sensitive to E; β3 more sensitive to NE.
Cholinergic receptors:
Nicotinic (nAChR): Open nonspecific cation channels, always excitatory.
Muscarinic (mAChR): M1,3,5 increase IP3 and Ca2+; M2,4 decrease cAMP and open K+ channels.
The Adrenal Medulla
The adrenal medulla is a neuroendocrine tissue that acts as a modified sympathetic ganglion. It is innervated by sympathetic preganglionic fibers, and its chromaffin cells (postganglionic neurons lacking axons) secrete epinephrine (a neurohormone) directly into the blood.
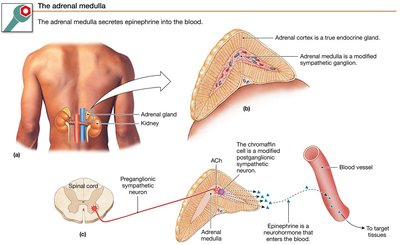
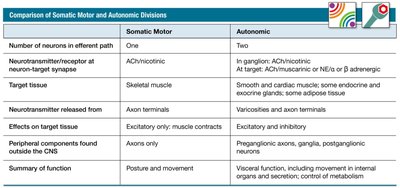
Comparison of Somatic Motor and Autonomic Divisions
Feature | Somatic Motor | Autonomic |
|---|---|---|
Number of neurons in efferent path | One | Two |
Neurotransmitter/receptor at neuron-target synapse | ACh/nicotinic | ACh/nicotinic (ganglion); ACh/muscarinic or NE/adrenergic (target) |
Target tissue | Skeletal muscle | Smooth/cardiac muscle, glands, adipose tissue |
Neurotransmitter released from | Axon terminals | Varicosities and axon terminals |
Effects on target tissue | Excitatory only | Excitatory or inhibitory |
Peripheral components outside CNS | Axons only | Preganglionic axons, ganglia, postganglionic neurons |
Summary of function | Posture and movement | Visceral function, internal organ movement, secretion, metabolism control |
The Somatic Motor Division
Somatic Motor Pathways
The somatic motor division consists of a single neuron pathway:
Originates in the CNS (brain or ventral horn of spinal cord).
Myelinated, long axons that are always excitatory.
Each terminal innervates a single skeletal muscle fiber.
The neuromuscular junction (NMJ) is the synapse between a somatic motor neuron and a skeletal muscle fiber. The motor end plate is the region of the muscle membrane with high concentrations of ACh receptors. Acetylcholinesterase (AChE) in the synaptic cleft rapidly degrades ACh.
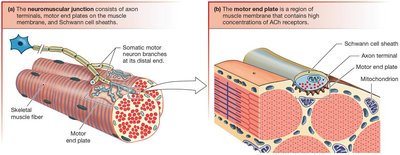
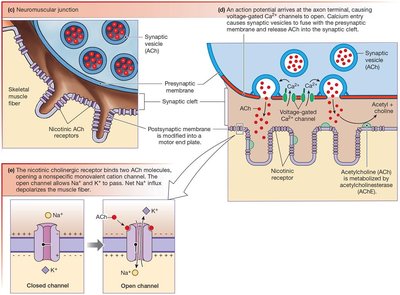
Nicotinic Receptors at the NMJ
nAChR channels on skeletal muscle are chemically gated ion channels with two binding sites for ACh.
Activation always leads to depolarization and muscle contraction.
These receptors are similar to neuronal nAChRs but are specific to muscle tissue.
Clinical Application: Nicotine Addiction and the NMJ
Nicotine and Nicotinic Receptors
Nicotine is an agonist at nAChRs, mimicking ACh and causing depolarization of the postsynaptic cell.
Chronic exposure to nicotine can lead to receptor desensitization and up-regulation, as seen in smokers.
Excessive nicotine can cause respiratory paralysis by keeping the muscle fiber depolarized, preventing further contraction.
Example: Nicotine replacement therapy helps prevent withdrawal symptoms while receptors down-regulate to normal levels.
Summary Table: Key Differences Between Somatic and Autonomic Divisions

Anatomy of the Efferent Divisions
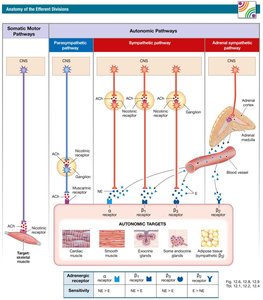
Additional info: For further details on neurotransmitter synthesis, receptor subtypes, and pharmacological agents, refer to the tables in the main text.
