 Back
BackEfferent Division: Autonomic and Somatic Motor Control – Study Notes
Study Guide - Smart Notes

Efferent Division of the Peripheral Nervous System
Overview of Efferent Pathways
The efferent division of the peripheral nervous system transmits commands from the central nervous system (CNS) to muscles and glands. It is divided into two main subdivisions: the somatic motor neurons, which control skeletal muscles and are mostly voluntary, and the autonomic neurons, which control smooth muscle, cardiac muscle, many glands, and some adipose tissue, and are mostly involuntary.
The Autonomic Division
Subdivisions of the Autonomic Division
The autonomic division is further divided into two branches:
Sympathetic branch – Responsible for the "fight-or-flight" response.
Parasympathetic branch – Responsible for the "rest-and-digest" response.
These branches are anatomically distinguishable and are best differentiated by their activity in various physiological situations.
Autonomic Reflexes and Homeostasis
Autonomic reflexes are crucial for maintaining homeostasis. They work in conjunction with the endocrine and behavioral state systems. Sensory information from somatosensory and visceral receptors, as well as hypothalamic sensors, is integrated in the hypothalamus, pons, and medulla, which serve as homeostatic control centers. Motor output from these centers leads to autonomic, endocrine, and behavioral responses. Some autonomic reflexes are spinal reflexes and do not require brain integration.
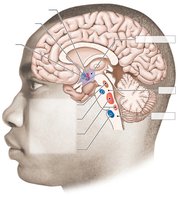
Autonomic Control Centers
The hypothalamus, pons, and medulla are key autonomic control centers. They regulate functions such as eating behavior, water balance, temperature control, blood pressure, and urinary bladder control.
Antagonistic and Cooperative Control
Most internal organs are under antagonistic control, meaning one autonomic branch is excitatory while the other is inhibitory. Some organs, like sweat glands and most blood vessels, receive only sympathetic innervation (tonic control). Cooperative control occurs when both branches work on different tissues to achieve a common goal. The response in target tissues is often determined by the type of neurotransmitter receptor present.
Autonomic Pathways Structure
Autonomic pathways consist of two efferent neurons in series:
Preganglionic neuron: Cell body in the CNS, projects to an autonomic ganglion outside the CNS.
Postganglionic neuron: Cell body in the autonomic ganglion, projects to the target tissue.
Ganglia also contain interneurons and act as mini-integration centers.
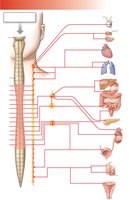
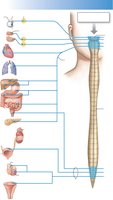
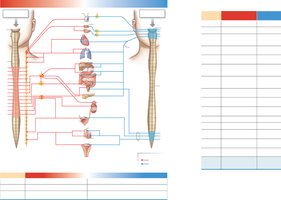
Sympathetic vs. Parasympathetic Origins
Sympathetic: Originates in thoracic and lumbar regions of the spinal cord; ganglia are located in chains alongside the vertebral column.
Parasympathetic: Originates in the brainstem and sacral spinal cord; ganglia are located on or near target organs. The vagus nerve contains about 75% of all parasympathetic fibers.
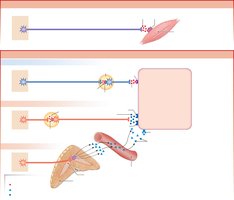
Chemical Signaling in the Autonomic Nervous System
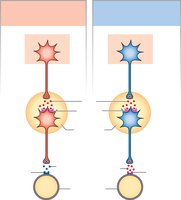
Both sympathetic and parasympathetic preganglionic neurons release acetylcholine (ACh) onto nicotinic cholinergic receptors. Most postganglionic sympathetic neurons secrete norepinephrine (NE) onto adrenergic receptors, while most postganglionic parasympathetic neurons secrete ACh onto muscarinic cholinergic receptors. There are exceptions, such as sympathetic cholinergic neurons innervating sweat glands.
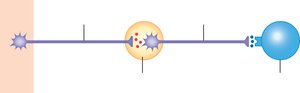
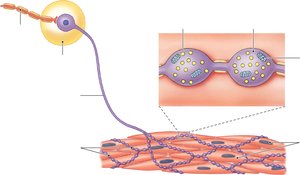
Neuroeffector Junctions and Varicosities
The neuroeffector junction is the synapse between a postganglionic autonomic neuron and its target cell. Neurotransmitters are released from varicosities, which are swellings at the end of the neuron. The release and removal of neurotransmitters, such as norepinephrine, involve exocytosis, receptor binding, reuptake, and enzymatic degradation.
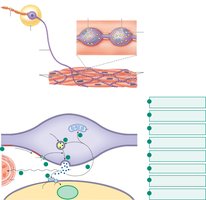
Autonomic Receptor Subtypes
Autonomic receptors are G protein-coupled and have multiple subtypes:
Adrenergic receptors (sympathetic):
Alpha (α) receptors: α1 (muscle contraction/secretion), α2 (decrease cAMP, smooth muscle relaxation)
Beta (β) receptors: β1 (responds equally to NE and E), β2 (more sensitive to E), β3 (more sensitive to NE)
Cholinergic receptors (parasympathetic):
Muscarinic receptors (M1, M2, M3, M4, M5)
Nicotinic receptors (NN, NM)
Receptor | Found in | Sensitivity | Effect on Second Messenger |
|---|---|---|---|
α1 | Most sympathetic target tissues | NE > E | Increases IP3 and Ca2+; increases PKC |
α2 | GI tract, pancreas | NE > E | Decreases cAMP |
β1 | Heart muscle, kidney | NE = E | Increases cAMP |
β2 | Certain blood vessels, smooth muscle | E > NE | Increases cAMP |
β3 | Adipose tissue | NE > E | Increases cAMP |
NN | Postganglionic autonomic neurons | ACh | Opens nonspecific cation channels |
NM | Skeletal muscle | ACh | Opens nonspecific cation channels |
M1, M3, M5 | Nervous system, parasympathetic targets | ACh | Increases IP3 and Ca2+; increases PKG |
M2, M4 | Nervous system, parasympathetic targets | ACh | Decreases cAMP; opens K+ channels |
Agonists and Antagonists of Neurotransmitter Receptors
Receptor Type | Neurotransmitter | Agonist | Antagonists | Indirect Agonists/Antagonists |
|---|---|---|---|---|
Muscarinic | Acetylcholine | Muscarine | Atropine, scopolamine | AChE inhibitors: neostigmine |
Nicotinic | Acetylcholine | Nicotine | α-bungarotoxin (muscle), TEA (ganglia), curare | |
Alpha (α) | NE, E | Phenylephrine | Alpha-blockers | Stimulate NE release: ephedrine, amphetamines; Prevent NE uptake: cocaine |
Beta (β) | NE, E | Isoproterenol, albuterol | Beta-blockers: propranolol, metoprolol |

Comparison of Sympathetic and Parasympathetic Branches
Feature | Sympathetic | Parasympathetic |
|---|---|---|
Point of CNS Origin | First thoracic to second lumbar segments | Midbrain, medulla, second to fourth sacral segments |
Location of Peripheral Ganglia | Paravertebral chain, outlying ganglia | On or near target organs |
Neurotransmitter at Target Synapse | Norepinephrine | Acetylcholine |
Receptors on Target Cells | Adrenergic | Muscarinic |
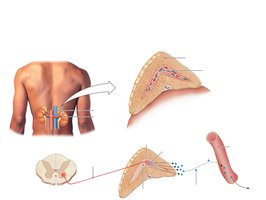
The Adrenal Medulla
The adrenal medulla is a neuroendocrine tissue that acts as a modified sympathetic ganglion. It is innervated by sympathetic preganglionic fibers, and its chromaffin cells (modified postganglionic neurons) secrete epinephrine (a neurohormone) directly into the blood.
The Somatic Motor Division
Somatic Motor Pathways
Somatic motor pathways consist of a single neuron originating in the CNS (brain or ventral horn of spinal cord). These neurons are myelinated, very long, and always excitatory. Each terminal branch innervates a single skeletal muscle fiber. The synapse between a somatic motor neuron and a skeletal muscle fiber is called the neuromuscular junction (NMJ).
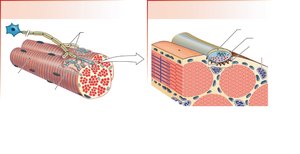
Neuromuscular Junction Structure and Function
The NMJ consists of axon terminals, motor end plates on the muscle membrane, and Schwann cell sheaths. The motor end plate contains high concentrations of nicotinic acetylcholine receptors (nAChR). Acetylcholinesterase (AChE) in the synaptic cleft rapidly degrades ACh to terminate the signal.
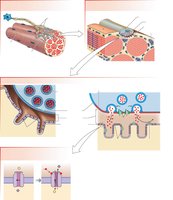
Mechanism of Neuromuscular Transmission
When an action potential arrives at the axon terminal, voltage-gated Ca2+ channels open, causing synaptic vesicles to release ACh into the synaptic cleft. ACh binds to nAChR on the motor end plate, opening nonspecific monovalent cation channels. The net influx of Na+ depolarizes the muscle fiber, leading to muscle contraction. ACh is then degraded by AChE.
Key Equations
Neurotransmitter breakdown (acetylcholine):
Second messenger (cAMP) pathway:
Summary Table: Postganglionic Autonomic Neurotransmitters
Division | Neurotransmitter | Receptor Types | Synthesized from | Inactivation Enzyme | Varicosity Membrane Transporters for |
|---|---|---|---|---|---|
Sympathetic | Norepinephrine (NE) | α- and β-adrenergic | Tyrosine | Monoamine oxidase (MAO) | Norepinephrine |
Parasympathetic | Acetylcholine (ACh) | Nicotinic and muscarinic cholinergic | Acetyl CoA + choline | Acetylcholinesterase (AChE) | Choline |

