 Back
BackFluid and Electrolyte Balance: Water and Sodium Regulation
Study Guide - Smart Notes

Fluid and Electrolyte Balance
The Concept of Balance
Fluid and electrolyte balance is essential for maintaining homeostasis in the body. The kidneys play a central role in regulating both fluid-electrolyte and acid-base balance by controlling the volume and composition of plasma.
Input: Includes ingestion and absorption from the digestive tract.
Output: Includes excretion via urine and feces, as well as losses from sweating, hemorrhage, and respiration.
Production/Utilization: Cellular metabolism contributes to water production and utilization.
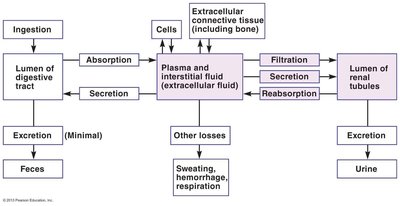
Example: The kidneys filter blood, reabsorb necessary solutes and water, and excrete waste products in urine.
Factors Affecting Plasma Composition
The kidneys regulate plasma volume and composition by adjusting solute and water content. Plasma volume is crucial due to its impact on mean arterial pressure (MAP).
Ingestion and Absorption: Water and solutes enter the body via the digestive tract.
Filtration, Secretion, Reabsorption: Occur in the renal tubules, affecting plasma and interstitial fluid.
Other Losses: Include sweating, hemorrhage, and respiration.
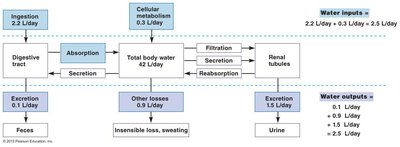
Example: Daily water input (2.5 L/day) matches output (2.5 L/day), maintaining balance.
Water Balance
Kidney Regulation of Water Excretion
The kidneys are the only organs that regulate water excretion to maintain balance. Water balance affects both plasma volume and osmolarity, which are critical for cardiovascular and cellular function.
Normovolemia: Normal plasma volume.
Hypervolemia: Increased plasma volume.
Hypovolemia: Decreased plasma volume.
Plasma Osmolarity: Changes affect fluid movement between compartments (ICF vs. ECF).
Example: Exercise and sweating increase plasma osmolarity, signaling kidneys to reabsorb water.
Water Reabsorption Mechanisms
The kidneys adjust water reabsorption rates to compensate for changes in plasma volume and osmolarity. Water is never secreted, only filtered and reabsorbed.
Osmotic Gradient: Drives water reabsorption, primarily due to Na+ in the extracellular fluid.
Proximal Tubule: 70% of Na+ is reabsorbed here, and water follows.
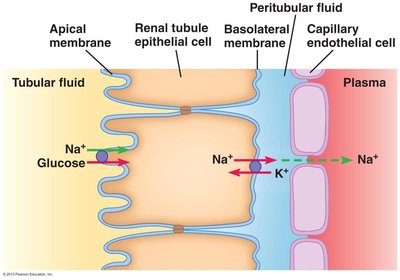
Example: Active transport of Na+ out of the renal filtrate creates an osmotic gradient for water reabsorption.
Water Reabsorption in the Loop of Henle
Juxtamedullary nephrons establish a medullary osmotic gradient via the loop of Henle, which is essential for water reabsorption.
Descending Limb: Permeable to water, but not to Na+, K+, or Cl-.
Thick Ascending Limb: Impermeable to water; actively transports Na+, K+, and Cl-.
Countercurrent Multiplier: Establishes the gradient.
Urea: Facilitated diffusion out of the collecting duct helps maintain the gradient.
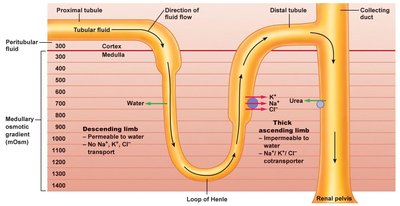
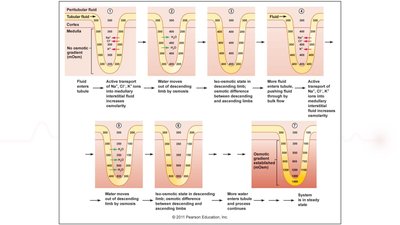
Example: The osmotic gradient allows water to be reabsorbed from the descending limb, concentrating urine.
Water Reabsorption in the Distal Convoluted Tubule (DCT) and Collecting Duct
The permeability of the late DCT and collecting duct to water is regulated by hormones and tight junctions.
Impermeable State: Results in high-volume, low-osmolarity urine.
Permeable State: Results in low-volume, high-osmolarity urine.
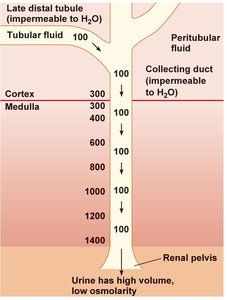
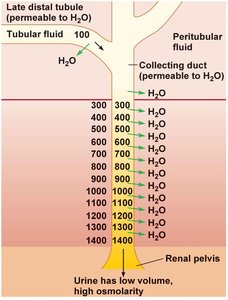
Example: Hormonal regulation (e.g., ADH) changes water permeability, affecting urine concentration.
Hormonal Regulation of Water Permeability
Aquaporins are required for water permeability in the late DCT and collecting duct. Antidiuretic hormone (ADH) increases aquaporin activity, enhancing water reabsorption.
ADH: Binds to receptors, activates cAMP pathway, and increases aquaporin-2 insertion in the apical membrane.
Result: Water moves from tubular fluid into plasma.
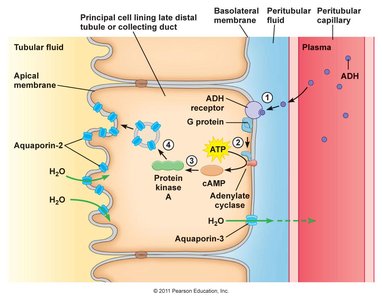
Example: ADH secretion increases during dehydration, promoting water conservation.
Regulation of ADH Secretion
ADH secretion is regulated by changes in plasma osmolarity and blood volume, detected by osmoreceptors and baroreceptors.
Osmoreceptors: Detect increased osmolarity, stimulate ADH release.
Baroreceptors: Detect decreased blood volume or MAP, stimulate ADH release.
Negative Feedback: Conserves body water and blood volume.
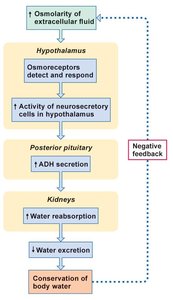
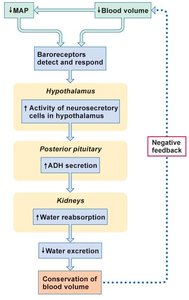
Example: During hemorrhage, baroreceptors trigger ADH release to conserve water.
Sodium (Na+) Balance
Importance of Sodium
Sodium is the primary solute in extracellular fluid and is crucial for cellular excitation and transport of other solutes. Regulation of Na+ is essential for maintaining plasma volume and osmolarity.
Hypernatremia: High plasma Na+ leads to hypervolemia.
Hyponatremia: Low plasma Na+ leads to hypovolemia.
Regulation: Na+ is freely filtered and reabsorbed, but not secreted.
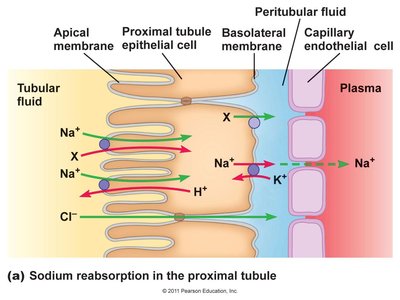
Example: Na+ reabsorption is driven by Na+/K+ pumps at the basolateral membrane.
Aldosterone and Sodium Reabsorption
Aldosterone is a steroid hormone released from the adrenal cortex in response to angiotensin II (ANG II). It increases Na+ reabsorption in the late distal tubule and collecting duct.
Mechanism: Aldosterone binds to cytosolic receptors, increasing Na+ channel and pump activity.
Result: Enhanced Na+ reabsorption and K+ secretion.
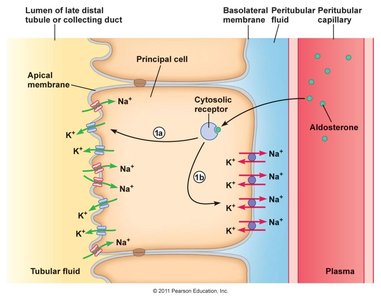
Example: During low blood pressure, aldosterone secretion increases to retain Na+ and water.
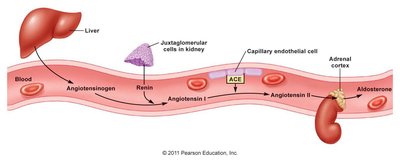
Renin-Angiotensin-Aldosterone System (RAAS)
The RAAS is activated by low blood pressure, leading to renin release from juxtaglomerular cells, conversion of angiotensinogen to angiotensin I, and subsequent formation of angiotensin II. Angiotensin II stimulates aldosterone and ADH secretion, increasing Na+ and water reabsorption.
Renin: Released in response to decreased afferent arteriole pressure, sympathetic activity, and low Na+/Cl- in distal tubules.
Angiotensin II: Causes vasoconstriction, aldosterone and ADH secretion, and thirst stimulation.
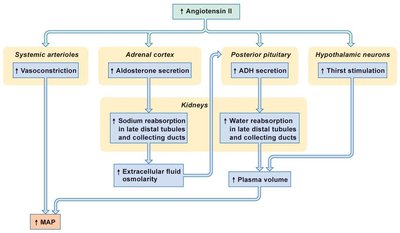
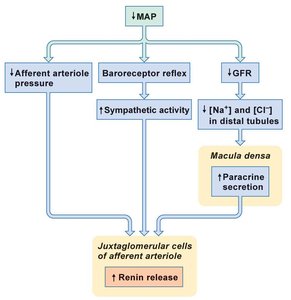
Example: RAAS increases MAP and plasma volume during hypotension.
Atrial Natriuretic Peptide (ANP) and Sodium Regulation
ANP is a peptide hormone secreted by the atrial walls in response to increased plasma volume and atrial stretch. It promotes natriuresis (increased Na+ excretion) by dilating afferent arterioles, constricting efferent arterioles, and inhibiting Na+ reabsorption, renin, and aldosterone secretion.
Stimulus: Increased plasma volume and atrial stretch.
Physiological Response: Increased GFR, decreased Na+ reabsorption, decreased renin and aldosterone.
Result: Increased Na+ excretion and reduced plasma volume.
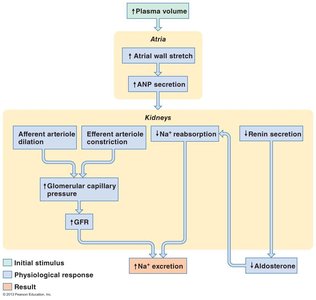
Example: ANP helps prevent hypervolemia by promoting sodium and water loss.
Summary
Fluid and electrolyte balance is maintained by the kidneys through precise regulation of water and sodium reabsorption and excretion. Hormonal mechanisms, including ADH, aldosterone, RAAS, and ANP, ensure homeostasis in response to changes in plasma volume, osmolarity, and blood pressure.
