 Back
BackHeart Physiology: Structure, Function, and Clinical Relevance
Study Guide - Smart Notes

Heart Physiology
Pacemaker Cells
Pacemaker cells are specialized cardiac muscle cells responsible for initiating and regulating the heartbeat. These cells are primarily located in the sinoatrial (SA) node, which acts as the heart's natural pacemaker.
Definition: Pacemaker cells generate spontaneous action potentials, setting the rhythm for cardiac contraction.
Location: Mainly in the SA node, but also found in the atrioventricular (AV) node and Purkinje fibers.
Function: Ensure coordinated contraction of the heart chambers.
Example: The SA node initiates impulses that spread throughout the atria, causing them to contract.
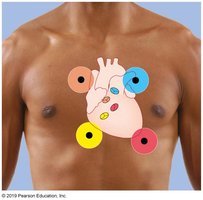
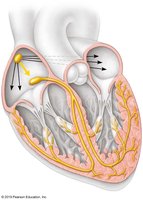
Intrinsic Cardiac Conduction System
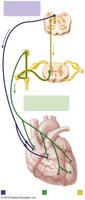
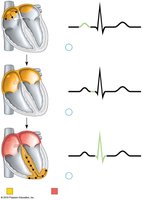
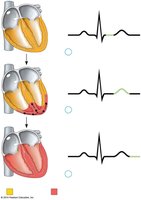
The intrinsic cardiac conduction system is a network of specialized cells that coordinate the electrical activity of the heart, ensuring efficient pumping of blood.
Components: SA node, AV node, AV bundle (Bundle of His), bundle branches, and Purkinje fibers.
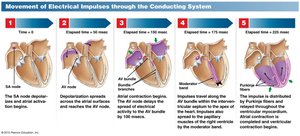
Pathway: Electrical impulses originate in the SA node, travel to the AV node, then through the AV bundle, bundle branches, and Purkinje fibers.
Purpose: Synchronizes atrial and ventricular contractions.
Example: The AV node delays the impulse, allowing the atria to finish contracting before the ventricles contract.
Autonomic Innervation of the Heart
The heart receives autonomic innervation from both the sympathetic and parasympathetic nervous systems, which modulate heart rate and contractility.
Sympathetic Innervation: Increases heart rate and force of contraction via norepinephrine release.
Parasympathetic Innervation: Decreases heart rate through acetylcholine release, primarily via the vagus nerve.
Clinical Relevance: Balance between these systems maintains normal cardiac function.
Action Potential of Cardiac Muscle
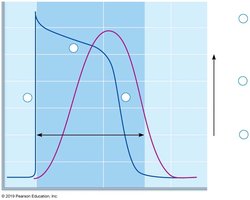
Cardiac muscle cells generate action potentials that differ from those in skeletal muscle, featuring a prolonged plateau phase due to calcium influx.
Phases: Rapid depolarization (Na+ influx), plateau (Ca2+ influx), repolarization (K+ efflux).
Importance: The plateau phase prevents tetanus, ensuring rhythmic contractions.
Equation:
Electrocardiogram (ECG)
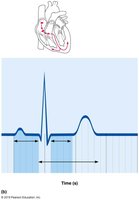
An electrocardiogram (ECG) is a clinical tool used to record the electrical activity of the heart, providing information about heart rhythm and function.
Key Waves: P wave (atrial depolarization), QRS complex (ventricular depolarization), T wave (ventricular repolarization).
Clinical Use: Diagnoses arrhythmias, myocardial infarction, and other cardiac conditions.
Example: A normal ECG shows regular P, QRS, and T waves.
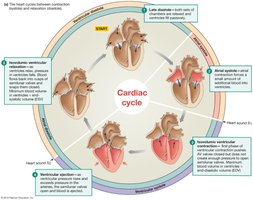
Cardiac Cycle
The cardiac cycle describes the sequence of events during one heartbeat, including systole (contraction) and diastole (relaxation) of the heart chambers.
Phases: Atrial systole, ventricular systole, and diastole.
Key Events: Blood flows from atria to ventricles, then from ventricles to arteries.
Clinical Relevance: Understanding the cycle is essential for interpreting heart sounds and ECG.
Heart Sounds
Heart sounds are produced by the closing of heart valves during the cardiac cycle and are important for clinical assessment.
First Sound (S1): Closure of AV valves (mitral and tricuspid).
Second Sound (S2): Closure of semilunar valves (aortic and pulmonary).
Clinical Use: Abnormal sounds (murmurs) may indicate valve disease.
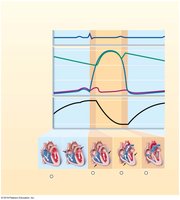
Wiggers Diagram
The Wiggers diagram integrates electrical, mechanical, and pressure changes in the heart during the cardiac cycle, providing a comprehensive overview of cardiac function.
Components: Shows ECG, heart sounds, pressure changes, and volume changes.
Clinical Relevance: Used to understand timing of events in the cardiac cycle.
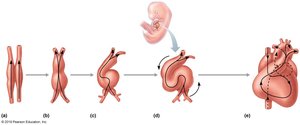
Development of the Heart
Heart development is a complex embryological process that forms the mature heart from a simple tube structure.
Stages: Formation of the heart tube, looping, chamber formation, and septation.
Importance: Errors in development can lead to congenital heart defects.
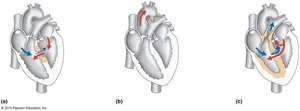
Types of Congenital Heart Defects
Congenital heart defects are structural abnormalities present at birth, affecting normal blood flow through the heart.
Common Types: Septal defects (ASD, VSD), patent ductus arteriosus, tetralogy of Fallot.
Clinical Impact: May require surgical correction or medical management.
Additional info: Congenital defects are often detected via echocardiography or clinical examination.
