 Back
BackHistology: Structure and Function of Tissues
Study Guide - Smart Notes

Histology: The Study of Tissues
Introduction to Histology
Histology is the study of the normal structures of tissues. Tissues are groups of cells related in structure and function, surrounded by a material called the extracellular matrix (ECM). Understanding tissue structure is essential for comprehending organ function and pathology.

Types of Tissues
Overview of the Four Primary Tissue Types
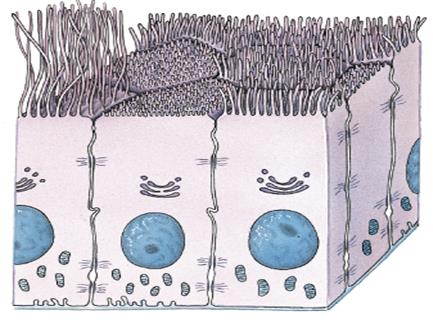
Epithelial tissues (epithelia): Tightly packed sheets of cells with little or no visible ECM. They cover and line all body surfaces and cavities and form glands that manufacture secretions or chemical messengers.
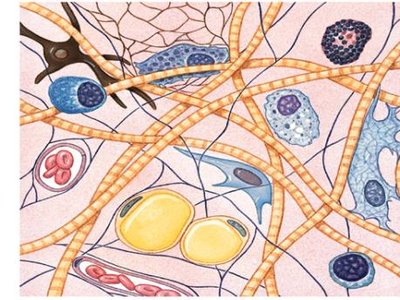
Connective tissues (CT): Connect tissues to one another, with ECM as a prominent feature. Functions include binding, support, protection, and transportation of substances.
Muscle tissues: Specialized for contraction, enabling movement.
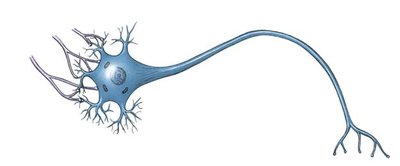
Nervous tissues: Consist of neurons (generate, send, and receive messages) and neuroglia (support neuronal activity).

The Extracellular Matrix (ECM)
Composition and Function
The extracellular matrix is composed of substances in a liquid, gel, or solid that surround cells. It provides strength, directs cell positioning, and regulates cell development and survival.
Ground substance: Mostly extracellular fluid (water, nutrients, ions, macromolecules).
Protein fibers: Collagen (resists tension), elastic (provides elasticity), and reticular fibers (supportive meshwork).
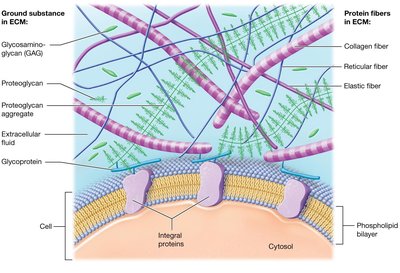
Key ECM Macromolecules
Glycosaminoglycans (GAGs): Large polysaccharides (e.g., chondroitin sulfate, hyaluronic acid) that trap water.
Proteoglycans: GAGs bound to a protein core, forming large aggregates.
Cell-adhesion molecules (CAMs): Glycoproteins that bind cells to each other and to ECM components.
Diseases of Collagen and Elastic Fibers
Ehlers-Danlos syndrome: Abnormal collagen fibers cause joint dislocations, hyperextensible skin, and fragile blood vessels.
Marfan syndrome: Abnormal elastic fibers result in tall stature, long limbs, skeletal and cardiovascular abnormalities.
Epithelial Tissues
Functions of Epithelial Tissues
Protection: Shields underlying tissues from injury; rapid mitosis for repair.
Immune defense: Forms barriers and contains immune cells.
Secretion: Produces sweat, hormones, and oils.
Transport: Selectively permeable membranes for substance movement.
Sensation: Detects environmental changes (e.g., taste buds).
Classification of Epithelia
Number of cell layers:
Simple epithelia: Single cell layer.
Stratified epithelia: Two or more layers.
Pseudostratified: Appears layered but is not.
Cell shape:
Squamous: Flattened cells.
Cuboidal: Cube-shaped cells.
Columnar: Tall, elongated cells.
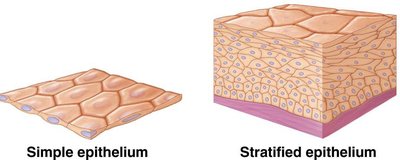
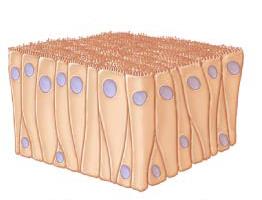
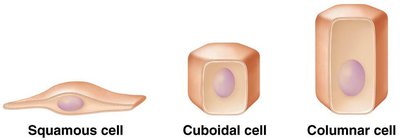
Types of Simple Epithelia
Simple squamous epithelium: Thin, rapid diffusion; found in air sacs of lungs, kidney, blood vessel walls.
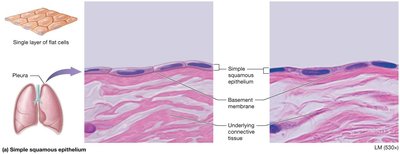
Simple cuboidal epithelium: Cube-shaped; found in renal tubules, respiratory passages, ducts of glands, thyroid gland.
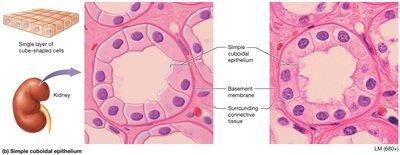
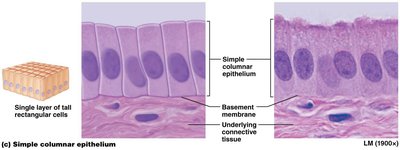
Simple columnar epithelium: Rectangular, often with microvilli or cilia; found in digestive tract.
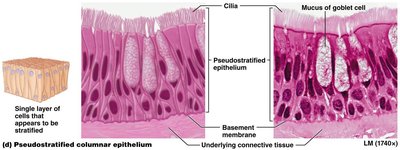
Pseudostratified ciliated columnar epithelium (PSCCE): Appears layered, ciliated; found in respiratory tract and nasal cavity.
Types of Stratified Epithelia
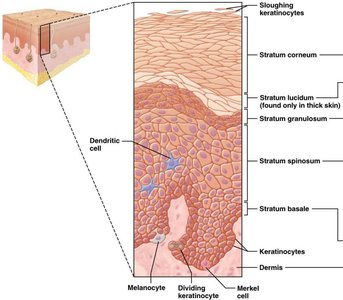
Stratified squamous epithelium:
Keratinized: Dead, keratin-filled cells; forms epidermis.
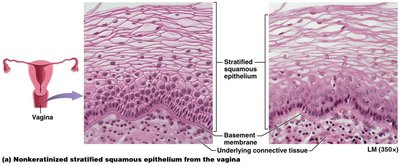
Nonkeratinized: Living cells with nuclei; lines mouth, throat, esophagus, anus, vagina.
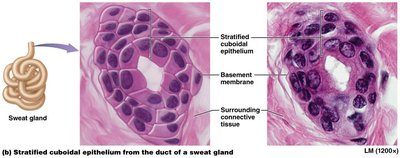
Stratified cuboidal epithelium: Rare; lines ducts of sweat glands.
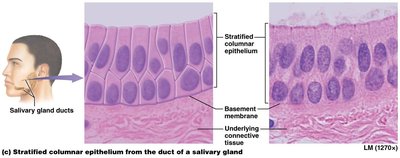
Stratified columnar epithelium: Rare; found in male urethra, cornea, salivary gland ducts.
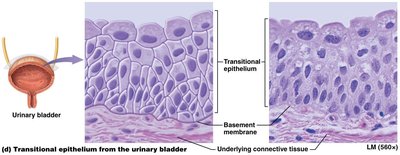
Transitional epithelium: Only in urinary system; dome-shaped apical cells flatten when stretched.
Glandular Epithelia
Endocrine glands: Ductless; secrete hormones directly into bloodstream (e.g., thyroid, pituitary).
Exocrine glands: Have ducts; secretions act locally (e.g., sweat, salivary glands). Can be unicellular (goblet cells) or multicellular.
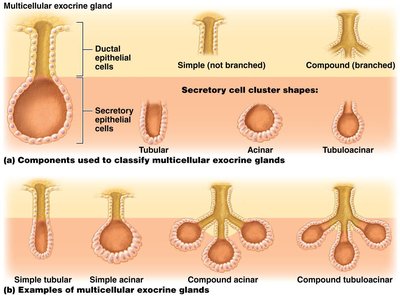
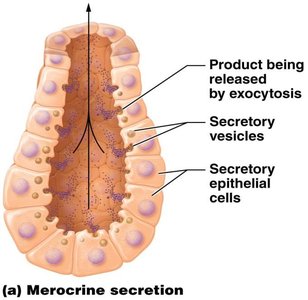
Modes of secretion:
Merocrine: Product released by exocytosis (e.g., sweat, salivary glands).
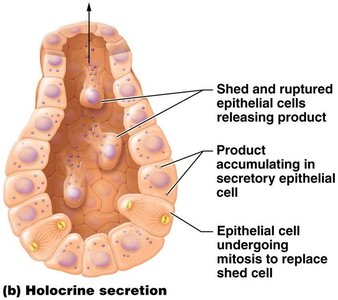
Holocrine: Entire cell ruptures to release product (e.g., sebaceous glands).
Carcinogens and Epithelial Tissues
Carcinogens: Agents that induce DNA changes, potentially leading to cancer.
Carcinoma: Cancer of epithelial tissue (e.g., lung adenocarcinoma, breast carcinoma, basal cell carcinoma).
Basement membrane: Provides a barrier to slow the spread of carcinomas.

Connective Tissue
Types and Functions of Connective Tissue
Connective tissue proper: Loose, dense (regular & irregular), reticular, adipose.
Specialized connective tissue: Cartilage, bone, blood.
Functions: Connect and bind, support, protect, transport substances.
Connective Tissue Cells
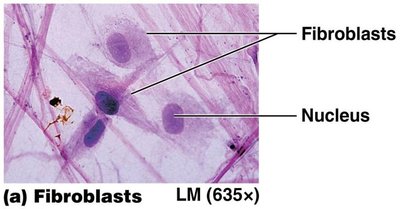
Fibroblasts: Produce fibers.
Adipocytes: Store fat.
Mast cells: Produce histamine (inflammation).
Phagocytes: Ingest foreign invaders (e.g., macrophages).
Connective Tissue Proper
Loose connective tissue (areolar): Mostly ground substance, supports epithelia, found beneath skin and in membranes.
Dense connective tissue:
Dense irregular: Disorganized collagen bundles; dermis, organ/joint capsules.
Dense regular: Parallel collagen bundles; tendons, ligaments.
Dense regular elastic: Parallel elastic fibers; large blood vessels, some ligaments.
Reticular tissue: Reticular fibers form networks supporting vessels, lymph nodes, spleen, liver, bone marrow.
Adipose tissue: Fat storage, insulation, shock absorption, protection.
Specialized Connective Tissues
Cartilage: Rigid matrix, chondroblasts/chondrocytes, mostly avascular.
Hyaline cartilage: Most abundant; ends of long bones, trachea, nose, fetal skeleton.
Fibrocartilage: Great tensile strength; intervertebral discs, menisci, pubic symphysis.
Elastic cartilage: Flexible; external ear, auditory tube, epiglottis.
Bone: Hard matrix, supports/protects, hemopoiesis, stores calcium and fat.
Blood: Fluid ECM (plasma), transports oxygen (erythrocytes), immunity (leukocytes), clotting (thrombocytes).
Muscle Tissues
Types and Functions
Skeletal muscle: Attached to bone, striated, voluntary movement.
Cardiac muscle: Heart, striated, involuntary, intercalated discs.
Smooth muscle: Walls of hollow organs and blood vessels, non-striated, involuntary.
Nervous Tissues
Structure and Function
Neurons: Send and receive messages.
Neuroglial cells: Support neurons, do not conduct impulses.

Tissues in Organs and Membranes
Organs
Organs are composed of two or more tissue types that function together (e.g., skeletal muscle and connective tissue in muscle organs; multiple tissue layers in the trachea).
Membranes
Serous membranes: Line pericardial, peritoneal, and pleural cavities.
Synovial membranes: Line joints, composed of connective tissue.
Mucous membranes: Line tubes/organs connecting to the outside; secrete mucus.
Cutaneous membrane: Skin.
Tissue Repair
Regeneration and Fibrosis
Regeneration: Damaged/dead cells replaced with same type; restores normal function.
Fibrosis: Fibroblasts produce collagen to fill injury, forming scar tissue (dense irregular connective tissue).
Concept Check
Why do the pharynx, esophagus, anus, and vagina have the same organization of epithelium? These areas are subject to wear and tear, so they are lined by nonkeratinized stratified squamous epithelium for protection.
The secretory cells of sebaceous glands fill with secretions and then rupture to release their contents. What is this type of secretion? Holocrine secretion.
A gland has no ducts to carry its secretion so it is released directly into the ECF. What type of gland is this? Endocrine gland.
An epithelial surface has many microvilli. What is the function of this epithelium? Increase surface area for absorption.
