 Back
BackInfectious Diseases Affecting the Genitourinary System: Structure, Defenses, and Major Pathologies
Study Guide - Smart Notes

Genitourinary Tract: Structure and Function
Overview of the Genitourinary Tract
The genitourinary tract consists of two distinct organ systems: the urinary tract and the genital (reproductive) system. Both systems are closely associated anatomically and functionally, and are subject to a variety of infectious diseases.
Urinary tract: Removes metabolic wastes from the blood, regulates body processes, forms urine, and transports it out of the body.
Genital system: Primarily functions in reproduction, with distinct male and female anatomical structures.
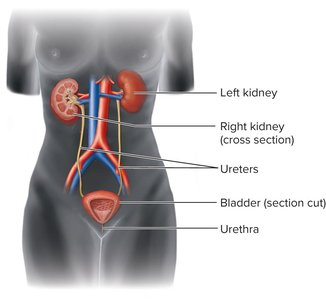
Urinary Tract Anatomy
Kidneys: Filter blood and remove metabolic wastes.
Ureters: Tubes that transport urine from kidneys to bladder.
Bladder: Stores urine until excretion.
Urethra: Conduit for urine to exit the body; in males, also part of the reproductive tract.
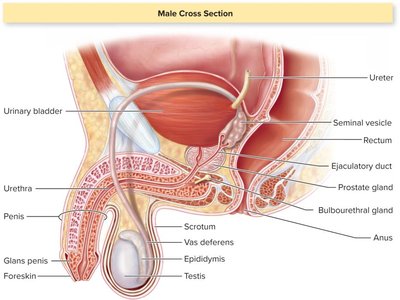
Male Reproductive System Anatomy
Testes: Produce sperm and hormones.
Epididymides: Coiled tubes for sperm maturation.
Vas deferens: Transports sperm to the ejaculatory duct.
Prostate gland: Contributes fluid to semen.
External organs: Scrotum (houses testes), penis (contains urethra).
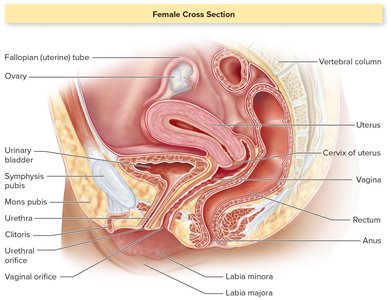
Female Reproductive System Anatomy
Ovaries: Produce eggs and hormones.
Fallopian tubes: Transport eggs from ovaries to uterus.
Uterus: Site of fetal development.
Vagina: Muscular canal connecting cervix to external body.
Cervix: Lower part of uterus, common site of infection.
Defenses of the Genitourinary Tract
Urinary Tract Defenses
Flushing action of urine: Physically removes microbes.
Desquamation: Shedding of epithelial cells with attached microbes.
Chemical defenses in urine:
Acidic pH
Lysozyme (breaks down bacterial cell walls)
Lactoferrin (binds iron, inhibiting bacterial growth)
Secretory IgA (immune antibody)
Male Reproductive Tract Defenses
Flushing action of urine
Physical barriers (intact skin and mucosa)
Female Reproductive Tract Defenses
Mucous membranes: Provide a nonspecific barrier, especially during childhood and menopause.
Secretory IgA: Provides specific immune protection.
Acidic vaginal pH: Maintained by Lactobacillus species fermenting glycogen to acid (pH 4.2–5 during reproductive years).
Before puberty and after menopause, vaginal pH is near neutral, and biota resembles that of the urethra.
Normal Biota of the Genitourinary Tract
Urinary Tract
Lower urethra harbors diverse microbiota (e.g., Streptococcus, Staphylococcus, Corynebacterium, Lactobacillus).
Upper urinary tract has fewer microbes.
Male Genital Tract
Similar to urinary tract; outer surface of penis colonized by Pseudomonas and Staphylococcus.
Uncircumcised penis harbors more anaerobic gram-negatives.
Female Genital Tract
During reproductive years, Lactobacillus predominates, maintaining acidic pH.
Candida albicans present at low levels; overgrowth leads to yeast infection.
Biota shifts with hormonal changes (puberty, menopause).
Summary Table: Defenses and Normal Biota
Site | Defenses | Normal Biota |
|---|---|---|
Urinary Tract (Both Sexes) | Flushing action, secretory IgA, lysozyme, lactoferrin | Streptococcus, Staphylococcus, Corynebacterium, Lactobacillus, etc. |
Female Genital Tract (Childhood/Postmenopause) | Mucus, secretory IgA | Same as urinary tract |
Female Genital Tract (Childbearing Years) | Acidic pH, mucus, secretory IgA | Lactobacillus, Prevotella, Streptococcus, Candida albicans |
Male Genital Tract | Same as urinary tract | Urethra: same as urinary tract; Penis: Pseudomonas, Staphylococcus, anaerobes |
Urinary Tract Infections (UTIs)
Overview and Types
Cystitis: Infection of the bladder; symptoms include pain, frequent urination, dysuria, cloudy urine, hematuria, low-grade fever, and nausea.
Pyelonephritis: Infection of the kidneys; symptoms include back pain and high fever, can cause permanent kidney damage.
Urethritis: Infection limited to the urethra.
Causative Agents
95% of UTIs are caused by normal biota of the GI tract.
Escherichia coli is responsible for 80% of cases.
Other agents: Staphylococcus saprophyticus, Klebsiella pneumoniae, Proteus mirabilis.
Transmission and Epidemiology
Community-acquired UTIs are not transmitted person-to-person but originate from the GI tract.
More common in women due to anatomical proximity of urethra and anus.
Catheter-associated UTIs (CA-UTIs) are a significant concern in healthcare settings.
Treatment
Nitrofurantoin (Macrobid) is commonly used.
Phenazopyridine (Pyridium) relieves symptoms but is not an antibiotic.
Many E. coli strains are resistant to penicillins.
Sexually Transmitted Infections (STIs) Affecting the Genitourinary System
Major Bacterial STIs
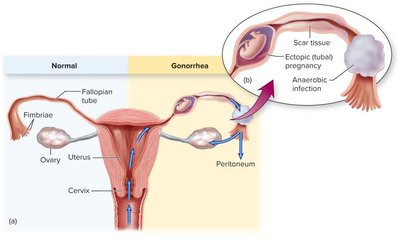
Gonorrhea (Neisseria gonorrhoeae):
Symptoms in males: urethritis, painful urination, yellowish discharge, possible infertility.
Symptoms in females: mucopurulent/bloody discharge, painful urination, risk of pelvic inflammatory disease (PID), infertility, ectopic pregnancy.
Virulence factors: fimbriae for attachment, antigenic variation, IgA protease, endotoxin.
Diagnosis: culture, catalase/oxidase tests, carbohydrate fermentation.
Treatment: dual therapy for gonorrhea and chlamydia due to frequent coinfection; antibiotic resistance is a growing concern.
Chlamydia (Chlamydia trachomatis):
Most common reportable infectious disease in the U.S.
Symptoms: similar to gonorrhea; often asymptomatic, especially in females (risk of PID).
Life cycle: alternates between infectious elementary body (EB) and replicative reticulate body (RB).
Diagnosis: PCR, ELISA, NAATs.
Treatment: doxycycline and/or azithromycin; treat all sexual partners.
Syphilis (Treponema pallidum):
Three clinical stages: primary (chancre), secondary (rash, systemic symptoms), tertiary (gummas, cardiovascular/neurological damage).
Congenital syphilis: can cause severe fetal abnormalities or death.
Diagnosis: dark-field microscopy, serology (RPR, immunoassay), NAATs.
Treatment: penicillin G is the drug of choice.

Major Fungal, Protozoal, and Viral STIs
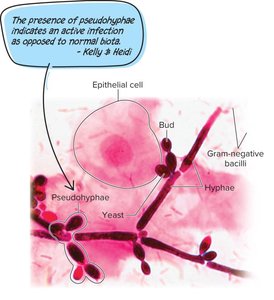
Candidiasis (Candida albicans):
Common cause of vaginitis; overgrowth leads to symptomatic infection.
Predisposing factors: antibiotics, diabetes, pregnancy, immune suppression.
Treatment: topical/oral azoles.
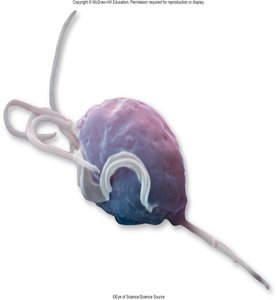
Trichomoniasis (Trichomonas vaginalis):
Protozoan infection; often asymptomatic but can cause frothy discharge in females.
Increases susceptibility to other infections and adverse pregnancy outcomes.
Treatment: oral metronidazole or tinidazole; treat both partners.
Genital Herpes (HSV-1 and HSV-2):
Causes painful vesicular lesions; can be latent and reactivate.
Neonatal herpes can be severe or fatal.
Treatment: acyclovir and derivatives reduce symptoms but do not cure.
Other Notable Conditions
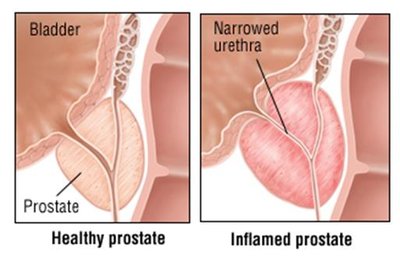
Prostatitis
Inflammation of the prostate gland; can be acute (usually bacterial) or chronic (often biofilm-related).
Symptoms: pelvic pain, urinary difficulties, painful ejaculation.
Treatment: ciprofloxacin or levofloxacin.
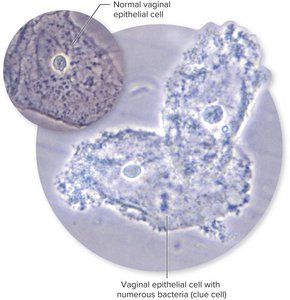
Vaginosis (Gardnerella species)
Non-inflammatory overgrowth of anaerobic bacteria; causes fishy-smelling discharge.
Diagnosis: presence of clue cells on vaginal smear.
Treatment: metronidazole or clindamycin.
Summary Table: Major Infectious Diseases of the Genitourinary System
Disease | Agent | Symptoms | Treatment |
|---|---|---|---|
UTI | E. coli, others | Dysuria, frequency, urgency | Nitrofurantoin, others |
Gonorrhea | Neisseria gonorrhoeae | Discharge, pain, PID | Dual antibiotic therapy |
Chlamydia | Chlamydia trachomatis | Discharge, PID, often asymptomatic | Doxycycline/azithromycin |
Syphilis | Treponema pallidum | Chancre, rash, gummas | Penicillin G |
Candidiasis | Candida albicans | Itching, discharge | Azole antifungals |
Trichomoniasis | Trichomonas vaginalis | Frothy discharge | Metronidazole |
Genital Herpes | HSV-1/2 | Vesicular lesions | Acyclovir |
Additional info: This guide integrates microbiology and clinical context for ANP college students, focusing on the structure, defenses, and infectious diseases of the genitourinary system. It covers both bacterial and non-bacterial pathogens, their pathogenesis, diagnosis, and treatment, with emphasis on public health relevance and current epidemiological trends.
