 Back
BackInfectious Diseases Affecting the Respiratory System: Microbiology Fundamentals
Study Guide - Smart Notes

Overview of the Respiratory System
Anatomy of the Respiratory Tract
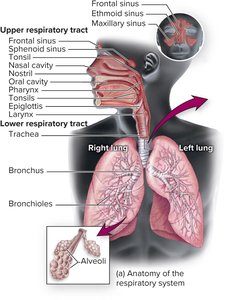
The respiratory tract is divided into two main parts: the upper and lower respiratory tracts. Each part contains specific anatomical structures that play crucial roles in respiration and defense against pathogens.
Upper respiratory tract: Mouth, nose, nasal cavity, sinuses, throat (pharynx), epiglottis, larynx
Lower respiratory tract: Trachea, bronchi, bronchioles, alveoli
Defenses of the Respiratory Tract
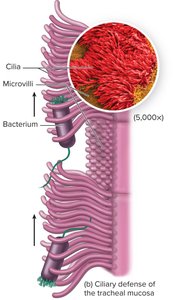
The respiratory tract is equipped with multiple defense mechanisms to prevent infection by pathogens.
Anatomical defenses: Nasal hair traps particles; cilia propel particles upward and out; mucus traps microorganisms.
Second and third line defenses: Complement system, antimicrobial peptides, cytokines, macrophages, secretory IgA.
Normal Biota of the Respiratory Tract
Composition and Function
The upper respiratory tract harbors a diverse community of commensal microorganisms, including bacteria and fungi. Even the lungs have a limited normal biota. The composition of the lung microbiome can differ in individuals with chronic diseases (e.g., COPD, asthma, cystic fibrosis) and between smokers and nonsmokers.
Common normal biota: Neisseria meningitidis, Staphylococcus, Streptococcus, Aspergillus, Streptococcus pyogenes, Haemophilus influenzae, Streptococcus pneumoniae, Staphylococcus aureus, Candida albicans
Microbial antagonism: Normal biota compete with pathogens for resources and space, reducing the likelihood of infection.
Diseases of the Respiratory System
Upper Respiratory Tract Diseases
Pharyngitis
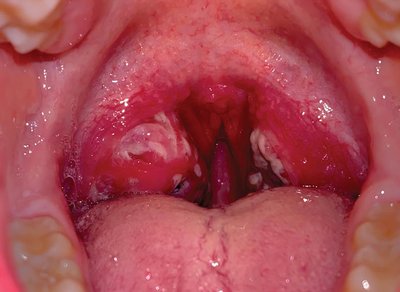
Pharyngitis is inflammation of the throat, often resulting in pain, redness, and swelling. Bacterial pharyngitis is typically more severe than viral forms and may be accompanied by fever, headache, and nausea.
Causative agents: Most commonly Streptococcus pyogenes (Group A Streptococcus) and Fusobacterium necrophorum.
Other causes: Viruses (same as common cold), mechanical irritation.
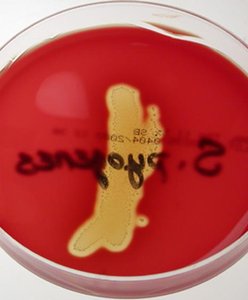
Streptococcus pyogenes: Characteristics and Pathogenesis
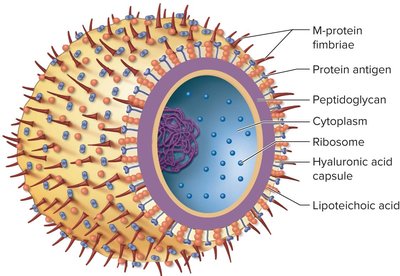
Gram-positive coccus growing in chains, nonmotile, forms capsules and slime layers, facultative anaerobe, does not produce catalase.
Pathogenesis: Untreated infections can lead to scarlet fever (erythrogenic toxin, sandpaper-like rash, high fever) and rheumatic fever (immunologic cross-reaction with heart tissue).
Virulence Factors of Streptococcus pyogenes
Surface antigens mimic host proteins and possess superantigens.
Specialized polysaccharides protect against lysozyme.
Lipoteichoic acid: Adherence to pharyngeal epithelial cells.
M protein: Resists phagocytosis, aids adherence.
Hyaluronic acid capsule: Contributes to adhesiveness.
Extracellular Toxins
Streptolysins (O and S): Cause beta-hemolysis, rapidly injure cells and tissues.
Erythrogenic toxin: Responsible for rash and fever in scarlet fever; produced only by lysogenic strains.
Transmission, Diagnosis, and Treatment
Transmission: Respiratory droplets or direct contact with mucus; humans are the only significant reservoir.
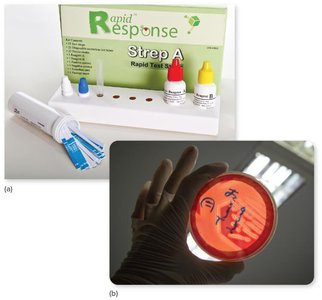
Diagnosis: Rapid antigen detection tests, culture on sheep blood agar (beta-hemolysis), bacitracin sensitivity.
Treatment: Penicillin (first choice), cephalexin for allergies; antibiotics prevent complications.
Prevention: No vaccine; good hygiene practices are essential.
Fusobacterium necrophorum
Emerging cause of severe sore throat, especially in adolescents and young adults.
Can progress to Lemierre’s syndrome (thrombophlebitis of veins).
The Common Cold
Causative agents: Over 200 viruses (rhinoviruses, coronaviruses, adenoviruses, RSV).
Transmission: Indirect contact, droplets.
Symptoms: Sneezing, scratchy throat, runny nose, fever (in children).
Sinusitis
Causative agents: Viruses, bacteria, fungi; allergies and structural abnormalities are noninfectious causes.
Treatment: Broad-spectrum antibiotics (bacterial), antifungals/surgery (fungal).
Lower Respiratory Tract Diseases
Pneumonia
Pneumonia is an inflammatory condition of the lung in which fluid fills the alveoli. It can be caused by bacteria, viruses, or fungi, and is a leading cause of death in children under 5 worldwide.
Key pathogens: Streptococcus pneumoniae, Legionella pneumophila, Mycoplasma pneumoniae, Chlamydophila pneumoniae, Histoplasma capsulatum, Hantavirus, respiratory viruses.
Community-acquired vs. healthcare-associated: Community-acquired is often due to S. pneumoniae; healthcare-associated is often polymicrobial and includes MRSA and Gram-negative rods.
Streptococcus pneumoniae
Small, gram-positive coccus, often in pairs.
Risk factors: old age, underlying disease, diabetes, substance abuse.
Vaccination (PPSV23, PCV13) recommended for older adults.
Legionella pneumophila
Weakly gram-negative, survives in water systems, resistant to chlorine, can live with amoebas.
Transmitted via aerosols from contaminated water sources.
Mycoplasma pneumoniae
Causes "walking pneumonia" with mild symptoms, spread in close quarters.
Hantavirus
Enveloped virus, transmitted via rodent excreta in dust.
Causes severe lung edema; outbreaks linked to rodent exposure.

Histoplasma capsulatum
Fungus found in nitrogen-rich soils, especially with bird/bat droppings.
Distribution determined by skin testing for allergic reaction.

Healthcare-Associated Pneumonia
Common in ventilated patients; high mortality (30-50%).
Caused by MRSA, Gram-negative rods, often polymicrobial.
Prevention: Elevate head of bed, deep breathing, proper equipment care.
Influenza
Overview and Symptoms
Influenza is a viral infection with cyclical increases in winter. It can cause pandemics and is characterized by fever, cough, body aches, and fatigue. Secondary infections and pneumonia are possible complications.
Causative Agents and Structure
Influenza A, B, and C viruses (family Orthomyxoviridae).
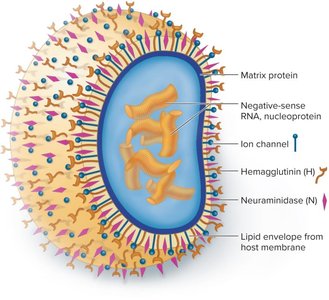
Spherical, enveloped, with glycoprotein spikes: hemagglutinin (H) and neuraminidase (N).
ssRNA genome, 10 genes on 8 segments, highly variable.
Antigenic Drift and Shift
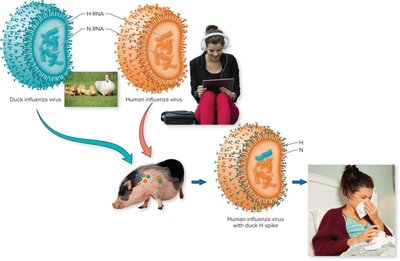
Antigenic drift: Gradual mutation of H and N proteins, requiring new vaccines annually.
Antigenic shift: Major genetic reassortment between viruses, can produce pandemic strains.
Pathogenesis, Transmission, and Diagnosis
Virus binds to ciliated respiratory cells, causing cell death and inflammation (cytokine storm).
Spread by aerosols, droplets, and fomites; facilitated by crowding and dry air.
Diagnosis: RT-PCR is preferred.
Prevention and Treatment
Vaccination: Inactivated or live attenuated vaccines, high-dose for elderly.
Antivirals: Zanamivir (Relenza), oseltamivir (Tamiflu), baloxavir (Xofluza); must be taken early.
Whooping Cough (Pertussis)
Causative agent: Bordetella pertussis (Gram-negative coccobacillus).
Transmission: Droplet contact.
Symptoms: Catarrhal stage (runny nose), paroxysmal stage (severe coughing), convalescent phase (recovery).
Prevention: DTaP vaccine, antibiotics for contacts.
Virulence factors: Capsule, tracheal toxin (destroys cilia), pertussis toxin (increases mucus), FHA (adhesion).
Tuberculosis
Overview and Forms
Tuberculosis (TB) is a chronic infectious disease caused by Mycobacterium tuberculosis. It primarily affects the lungs but can disseminate to other organs.
Forms: Primary, secondary (reactivation), extrapulmonary (outside lungs).
Primary TB: Bacteria multiply in macrophages, form tubercles, may heal by calcification.
Secondary TB: Reactivation leads to chronic symptoms and lung damage.
Extrapulmonary TB: Affects lymph nodes, kidneys, bones, genital tract, brain; often fatal in immunosuppressed.
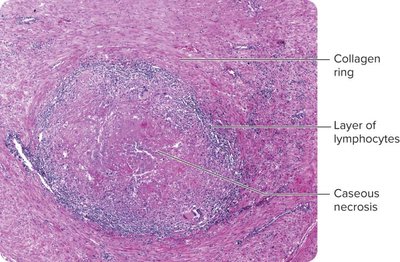
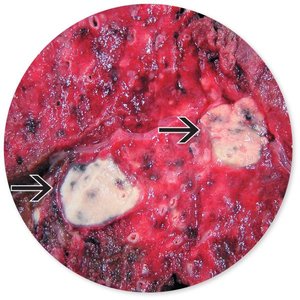
Causative Agent and Pathogenesis
Mycobacterium tuberculosis: Acid-fast bacillus, strict aerobe, slow-growing, waxy cell wall (mycolic acids), resistant to drying/disinfectants.
Virulence: Cord factor, survival in macrophages, strong cell-mediated immune response.
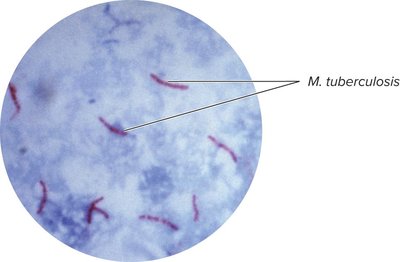
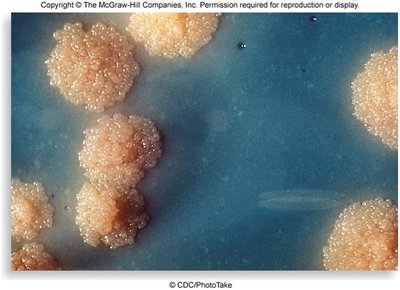
Transmission, Diagnosis, and Treatment
Transmission: Airborne droplets; survives long periods in aerosols.
Diagnosis: Tuberculin skin test (Mantoux), interferon-gamma release assays, acid-fast staining, gene amplification.
Prevention: Isolation, BCG vaccine (not used in U.S.).
Treatment: Long-term antibiotics (rifampin, isoniazid); noncompliance leads to drug resistance.
Drug-Resistant Tuberculosis
MDR-TB: Resistant to isoniazid and rifampin; requires prolonged, multi-drug therapy; high mortality.
XDR-TB: Resistant to additional drugs; few treatment options; very high mortality.
Summary Table: Major Infectious Diseases of the Respiratory System
Disease | Causative Agent | Type | Key Features |
|---|---|---|---|
Pharyngitis | Streptococcus pyogenes, Fusobacterium necrophorum, viruses | Bacteria, Virus | Sore throat, fever, possible complications (scarlet/rheumatic fever) |
Common Cold | Rhinoviruses, coronaviruses, others | Virus | Sneezing, runny nose, mild symptoms |
Sinusitis | Viruses, bacteria, fungi | Mixed | Facial pain, congestion |
Pneumonia | Streptococcus pneumoniae, Legionella, Mycoplasma, viruses, fungi | Mixed | Alveolar inflammation, cough, fever, can be fatal |
Influenza | Influenza A, B, C viruses | Virus | Fever, cough, body aches, risk of pandemics |
Whooping Cough | Bordetella pertussis | Bacteria | Severe coughing fits, vaccine-preventable |
Tuberculosis | Mycobacterium tuberculosis | Bacteria | Chronic cough, weight loss, can be latent or active |
