 Back
BackLiver, Pancreas, and Urinary System: Structure and Function
Study Guide - Smart Notes

Liver: Anatomy and Segmentation
Gross Anatomy of the Liver
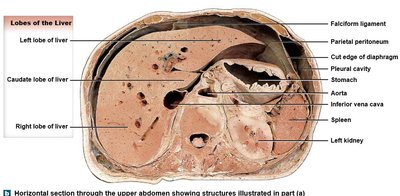
The liver is the largest internal organ, located inferior to the diaphragm and protected by the rib cage. It is divided into anatomical lobes and functional segments, each with distinct vascular and ductal supply.
Lobes: Right, left, caudate, and quadrate lobes, defined by fissures and ligaments.
Falciform ligament: Divides right and left lobes; attaches liver to anterior abdominal wall.
Bare area: Region not covered by peritoneum, fused to the diaphragm.
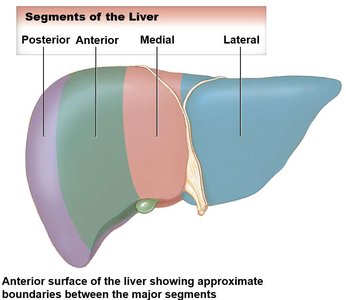
Segments: Each segment contains its own branch of the hepatic artery, portal vein, and bile duct.
Visceral Surface and Ligaments
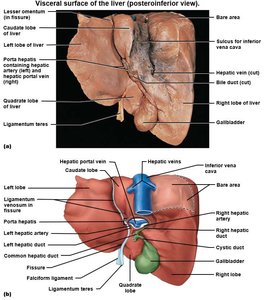
The visceral (inferior) surface of the liver is marked by fissures and ligaments that further define its structure and provide attachment points.
Fissures: Separate caudate and quadrate lobes from the right lobe, but these are functionally part of the left lobe.
Round ligament: Remnant of fetal umbilical vein, extends from liver to navel.
Microscopic Structure: Liver Lobules
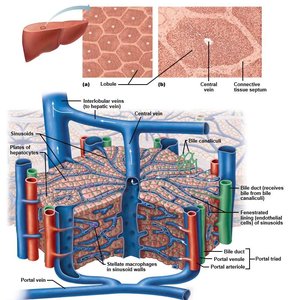
The liver is composed of hexagonal lobules, each containing plates of hepatocytes. Blood and bile flow through specialized channels to support metabolic and excretory functions.
Portal triads: Located at lobule corners; contain branches of the hepatic artery, portal vein, and bile duct.
Central vein: Located at the center of each lobule; collects blood after it passes through hepatocytes.
Direction of flow: Blood flows from portal triads through sinusoids to the central vein; bile flows in the opposite direction toward bile ducts.
Gall Bladder and Biliary Apparatus
Gall Bladder Anatomy
The gall bladder is a pear-shaped organ located on the inferior surface of the liver. It stores and concentrates bile produced by the liver.
Fundus: Located at the intersection of the costal margin and linea semilunaris.
Cystic duct: Merges with the common hepatic duct to form the bile duct.
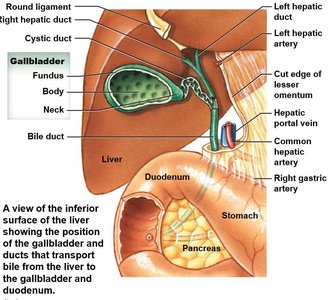
Biliary Apparatus
The biliary apparatus is a network of ducts that transport bile from the liver and gall bladder to the duodenum. Bile is continuously secreted by the liver and stored in the gall bladder when not needed for digestion.
Bile duct: Formed by the union of the common hepatic and cystic ducts.
Hepatopancreatic ampulla: Regulates the flow of bile and pancreatic juice into the duodenum.
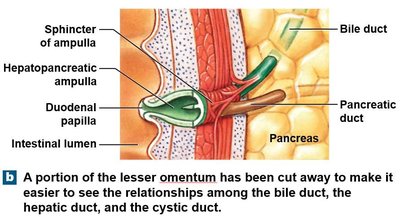
Pancreas: Structure and Function
Gross Anatomy of the Pancreas
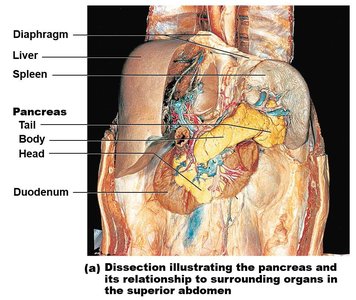
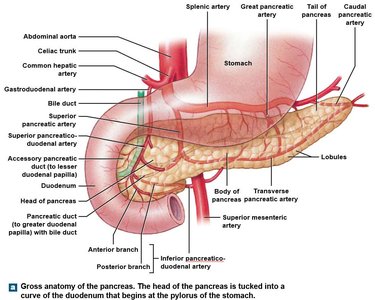
The pancreas is a retroperitoneal organ located inferior to the stomach. It has three regions: head (within the curve of the duodenum), body, and tail (lateral).
Exocrine function: Acinar cells produce digestive enzymes, drained by small ducts into the main and accessory pancreatic ducts.
Endocrine function: Islets of Langerhans secrete hormones (insulin, glucagon) into the bloodstream.
Urinary System: Structure and Function
Overview of the Urinary System
The urinary system removes nitrogenous wastes, regulates blood volume, chemistry, and pressure, and transports urine for excretion. It consists of the kidneys, ureters, urinary bladder, and urethra.
Kidneys: Filter blood and form urine.
Ureters: Transport urine from kidneys to bladder.
Urinary bladder: Stores urine until excretion.
Urethra: Conducts urine out of the body.
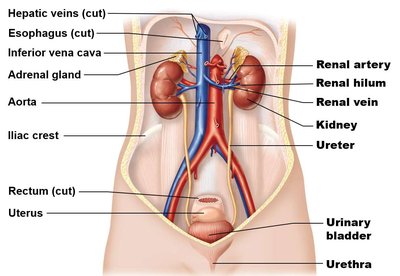
External and Internal Anatomy of the Kidneys
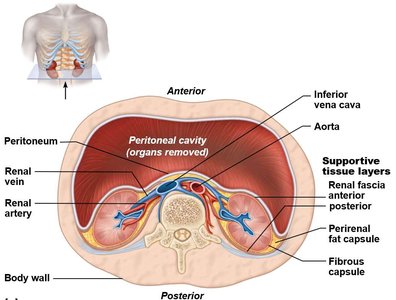
The kidneys are retroperitoneal organs extending from T11 to L2. The right kidney is slightly lower than the left due to the liver. Each kidney has a convex lateral edge and a concave medial edge (renal hilum).
Supportive tissues: Pararenal fat, renal fascia, perirenal fat capsule, and fibrous capsule protect and anchor the kidneys.
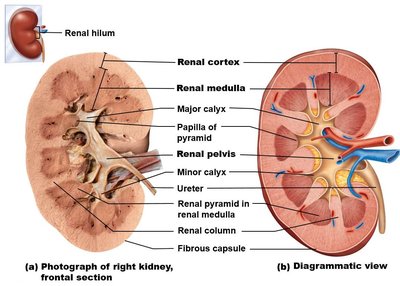
Internal structure: Renal cortex (outer, granular), renal medulla (pyramids), renal columns (cortical extensions).
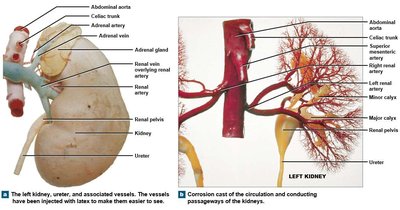
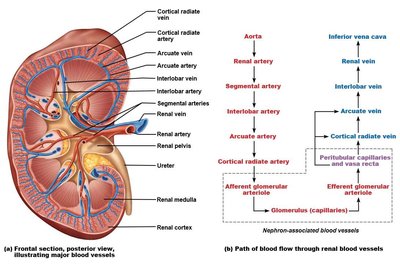
Blood Supply to the Kidneys
Renal arteries branch from the abdominal aorta and supply the kidneys through a series of progressively smaller arteries. Venous return follows a similar pattern in reverse.
Arterial branches: Renal artery → segmental arteries → lobar arteries → arcuate arteries → cortical radiate arteries.
Venous return: Cortical radiate veins → arcuate veins → interlobar veins → renal vein → inferior vena cava.
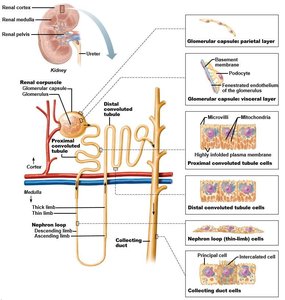
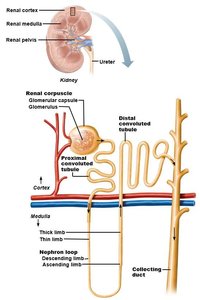
Nephron Structure and Types
The nephron is the functional unit of the kidney, responsible for filtering blood and forming urine. Each nephron consists of a renal corpuscle and a renal tubule.
Renal corpuscle: Glomerulus (capillary bed) + glomerular capsule.
Renal tubule: Proximal convoluted tubule (PCT), nephron loop (descending and ascending limbs), distal convoluted tubule (DCT), and collecting duct.
Types: Cortical nephrons (short loops, corpuscle near capsule) and juxtamedullary nephrons (long loops, corpuscle near medulla).
Urine Formation and Flow
Urine is formed through three main processes: filtration, reabsorption, and secretion. Once filtrate enters the collecting duct, it is termed urine and follows a specific path out of the kidney.
Filtration: Occurs in the glomerulus; blood plasma is filtered into the nephron.
Reabsorption: Useful substances are reabsorbed from the filtrate back into the blood.
Secretion: Additional wastes are secreted into the filtrate.
Urine flow: Collecting duct → papillae of pyramids → minor calyces → major calyces → renal pelvis → ureter.
Ureters, Urinary Bladder, and Urethra
The ureters transport urine from the kidneys to the bladder, which stores urine until micturition. The urethra conducts urine out of the body, with structural differences between males and females.
Ureters: Exit kidneys at L2, descend retroperitoneally, enter bladder at posterolateral corners.
Urinary bladder: Located inferior to the pubic symphysis; detrusor muscle forms the bladder wall.
Male urethra: 20 cm, three regions (prostatic, membranous, spongy); conducts urine and semen.
Female urethra: 3–4 cm, conducts urine only; external orifice posterior to clitoris.
Trigone: Triangular area formed by ureter and urethra openings in the bladder.
Urethral sphincters: Internal (smooth muscle, involuntary) and external (skeletal muscle, voluntary) sphincters control urination.
Example: The micturition reflex is initiated when stretch receptors in the bladder wall are activated, leading to relaxation of the sphincters and urination.
