 Back
BackMuscle Tissue and Physiology: Structured Study Notes for ANP College Students
Study Guide - Smart Notes

Muscle Tissue and Physiology
Overview of Muscle Tissue
Muscle tissue is essential for movement, posture, joint stabilization, heat generation, and regulation of material flow through hollow organs. It consists of muscle cells (myocytes) and the surrounding endomysium, which transmits tension and holds cells together. There are three main types of muscle tissue: skeletal, cardiac, and smooth.
Types of Muscle Tissue
Each muscle tissue type has unique structural and functional characteristics:
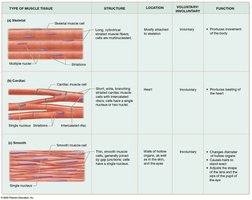
Skeletal Muscle Tissue: Long, thin, striated, multinucleated cells arranged parallel; voluntary; attached to skeleton; responsible for body movement.
Cardiac Muscle Tissue: Shorter, branched, usually single nucleus; striated; contains intercalated discs; involuntary; found only in the heart.
Smooth Muscle Tissue: Long, flattened cells with pointed ends; single, centrally located nucleus; involuntary; lines hollow organs, eyes, skin, and ducts.
Type | Structure | Location | Voluntary/Involuntary | Function |
|---|---|---|---|---|
Striated (Skeletal) | Long, cylindrical, multinucleated, striated | Mostly attached to skeleton | Voluntary | Produces movement |
Cardiac | Short, branched, single nucleus, striated, intercalated discs | Heart | Involuntary | Pumps blood |
Smooth | Long, flattened, single nucleus, no striations | Hollow organs, eyes, skin, ducts | Involuntary | Changes diameter, moves materials |
Properties of Muscle Cells
Muscle cells possess several key properties:
Contractility: Ability to contract and generate force.
Excitability: Ability to respond to stimuli.
Conductivity: Ability to conduct electrical charges.
Distensibility: Ability to stretch without rupture.
Elasticity: Ability to return to original length after stretching.
Structure of Muscle Cells
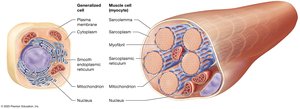
Muscle cells contain specialized structures:
Sarcoplasm: Cytoplasm of muscle cell.
Sarcolemma: Plasma membrane of muscle cell.
Myofibrils: Bundles of proteins involved in contraction; make up 50–80% of cell volume.
Sarcoplasmic Reticulum (SR): Modified smooth ER surrounding myofibrils; stores and releases calcium ions.
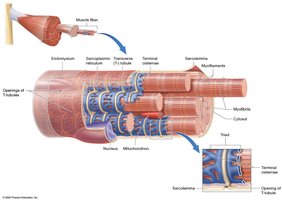
Structure of the Skeletal Muscle Fiber
Skeletal muscle fibers are long, cylindrical, multinucleated, and striated. They arise from fused embryonic myoblasts and contain abundant myofibrils surrounded by sarcoplasmic reticulum. The sarcolemma forms inward extensions called transverse tubules (T-tubules), which surround each myofibril and form a tunnel-like network. Terminal cisternae flank each T-tubule, and a triad consists of a T-tubule and two terminal cisternae.

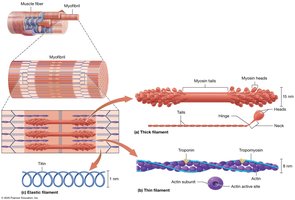
Structure of the Myofibril
Myofibrils are composed of protein bundles called myofilaments:
Thick Filaments: Made of myosin; contain two globular heads and a tail.
Thin Filaments: Made of actin (with active sites), tropomyosin (covers active sites), troponin (holds tropomyosin), and nebulin (determines filament length).
Elastic Filaments: Made of titin; provide elasticity and resist excessive stretching.
Myofilament Arrangement and the Sarcomere
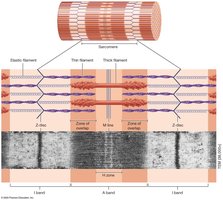
The arrangement of myofilaments creates visible bands:
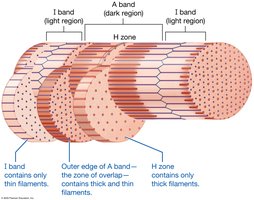
I band: Light region; only thin filaments.
A band: Dark region; thick and thin filaments.
H zone: Middle of A band; only thick filaments.
M line: Middle of A band; structural proteins hold thick filaments.
Z-disk: Structural proteins anchor thin filaments and attach myofibrils.
Structure | Description | Mnemonic |
|---|---|---|
A band | Dark band; thick and thin filaments | A is the dArk band |
I band | Light band; only thin filaments | I is the lIght band |
H zone | Middle of A band; only thick filaments | "H" because H is in the A band |
M line | Middle of A band; structural proteins | M for "middle" or "myosin" |
Z-disk | Line bisecting I band; anchors filaments | Z shape |
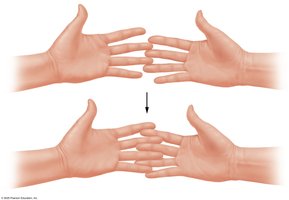
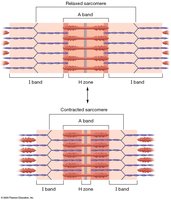
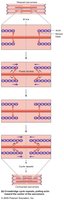
The Sliding-Filament Mechanism of Contraction
Muscle contraction occurs when thin filaments slide past thick filaments, generating tension. The I bands and H zone narrow as myosin heads pull thin filaments toward the M line, bringing Z-discs closer and shortening the sarcomere. The A band remains unchanged.
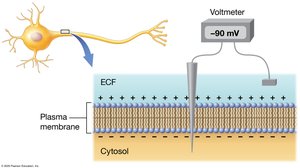
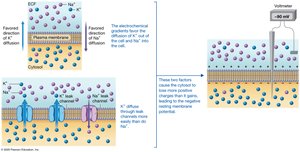
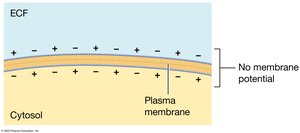
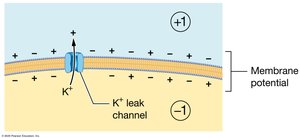
Membrane Potential in Muscle Cells
Muscle fibers maintain an electrical gradient across their plasma membrane, known as the resting membrane potential (typically −90 mV). This is established by the movement of sodium and potassium ions through leak and gated channels, and the action of the sodium-potassium pump.
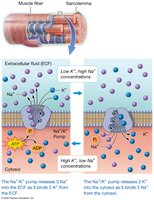
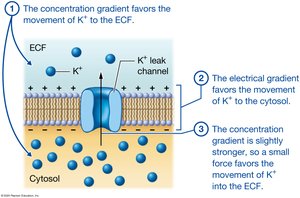
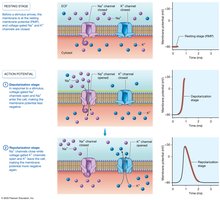
Action Potentials
An action potential is a rapid change in membrane potential, involving depolarization (sodium ions enter, membrane becomes less negative) and repolarization (potassium ions exit, membrane returns to negative). Action potentials are propagated along the sarcolemma and T-tubules.
The Neuromuscular Junction
The neuromuscular junction (NMJ) is the synapse between a motor neuron and a muscle fiber. It consists of the axon terminal (with synaptic vesicles containing acetylcholine), the synaptic cleft, and the motor end plate (with acetylcholine receptors).
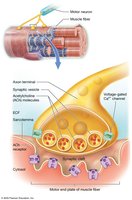
Skeletal Muscle Contraction
Phases of Contraction
Excitation Phase: Acetylcholine released from motor neuron stimulates sarcolemma.
Excitation-Contraction Coupling: Action potential travels down T-tubules, triggers calcium release from SR.
Contraction Phase: Calcium binds to troponin, tropomyosin moves, myosin binds actin, crossbridge cycle occurs.
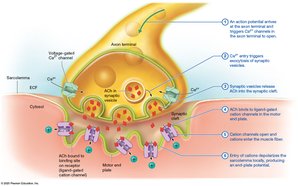
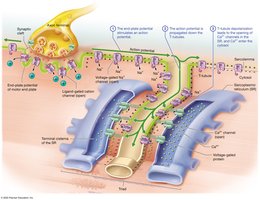
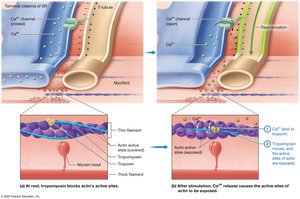
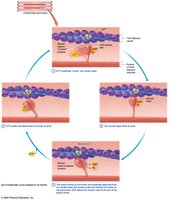
Muscle Relaxation
Muscle relaxation occurs when acetylcholine is degraded, calcium is pumped back into the SR, and troponin/tropomyosin block actin's active sites. Muscle spasms occur when relaxation is impaired.
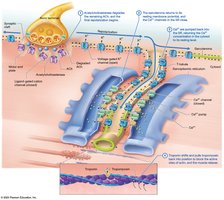
Rigor Mortis
Rigor mortis is the stiffening of muscles after death due to lack of ATP, preventing detachment of myosin from actin. Muscles remain contracted until proteins degrade.

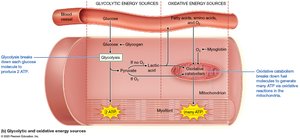
Energy Sources for Skeletal Muscle
Muscle fibers use ATP for contraction and relaxation, regenerated by:
Immediate sources: Creatine phosphate reaction (via creatine kinase).
Glycolytic catabolism: Anaerobic breakdown of glucose to pyruvate/lactic acid.
Oxidative catabolism: Aerobic breakdown in mitochondria using oxygen and myoglobin.
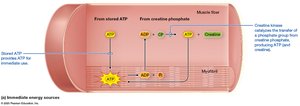
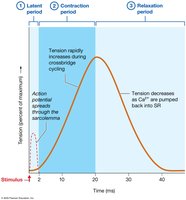
Muscle Tension at the Fiber Level
A muscle twitch is the response to a single action potential. It consists of latent, contraction, and relaxation periods. Tension varies with timing, frequency, and fiber type.
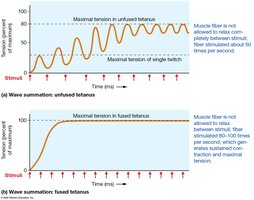
Tension Production and Timing/Frequency of Stimulation
Repeated stimulation leads to wave summation and tetanus (unfused or fused). Fused tetanus produces maximal tension. Tetanus disease is caused by Clostridium tetani toxin.
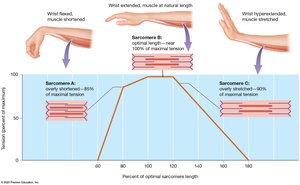
The Length-Tension Relationship
Optimal sarcomere length allows maximal crossbridge formation and tension. Overly shortened or stretched muscles produce less tension.
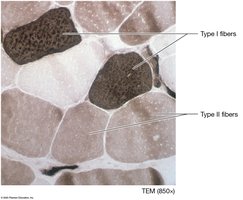
Classes of Skeletal Muscle Fibers
Fast-Twitch Fibers: Rapid contraction, fatigue quickly, rely on glycolytic energy.
Slow-Twitch Fibers: Slow contraction, sustained activity, rely on oxidative energy.
Subtypes: Fast oxidative glycolytic (FOG) and fast glycolytic (FG).
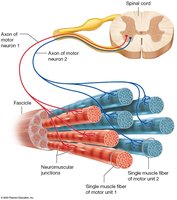
Motor Units
A motor unit is a motor neuron and the muscle fibers it innervates. Recruitment increases force by activating more units. Muscle tone is maintained by involuntary activation.
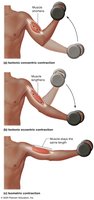
Types of Muscle Contractions
Isotonic Concentric: Muscle shortens, force > load.
Isotonic Eccentric: Muscle lengthens, force < load.
Isometric: Muscle length unchanged.
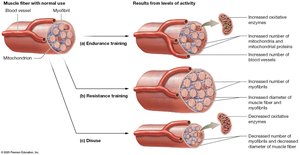
Changes Caused by Physical Training
Endurance Training: Increases oxidative enzymes, mitochondria, blood vessels; improves fatigue resistance.
Resistance Training: Increases myofibrils and fiber diameter (hypertrophy); decreases endurance capacity.
Disuse: Decreases fiber diameter (atrophy), oxidative enzymes, and endurance.
Muscle Fatigue and Recovery
Muscle fatigue is the inability to maintain exercise intensity, caused by depletion of metabolites, decreased oxygen, accumulation of chemicals, and environmental factors. Recovery involves excess postexercise oxygen consumption (EPOC) to restore homeostasis.
Key Equations
Creatine Phosphate Reaction:
Glycolysis:
Na+/K+ Pump:
Summary Table: Muscle Fiber Types
Type | Diameter | Contraction Speed | Energy Source | Fatigue Resistance |
|---|---|---|---|---|
Slow Oxidative | Small-Intermediate | Slow | Oxidative | High |
Fast Oxidative Glycolytic | Intermediate-Large | Fast | Mixed | Moderate |
Fast Glycolytic | Largest | Very Fast | Glycolytic | Low |
Example: Postural muscles contain mostly slow-twitch fibers for sustained contraction, while eye muscles contain fast-twitch fibers for rapid movement.
Additional info: These notes expand on brief points with academic context, definitions, and examples to ensure completeness and clarity for exam preparation.
