 Back
BackMuscle Tissue: Structure, Function, and Physiology
Study Guide - Smart Notes

Muscle Tissue
Types of Muscle Tissue
Muscle tissue is specialized for contraction and is essential for movement, posture, and various physiological processes. There are three main types of muscle tissue, each with distinct structural and functional characteristics:
Skeletal Muscle: Attaches to bones, skin, or fascia; striated with visible light and dark bands; under voluntary control.
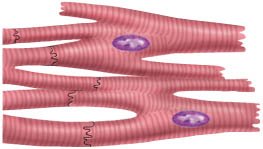
Cardiac Muscle: Found only in the heart; striated; involuntary; autorhythmic due to a built-in pacemaker.
Smooth Muscle: Located in walls of hollow organs and attached to hair follicles; non-striated; involuntary.
Functions of Muscle Tissue
Muscle tissue performs several vital functions in the body:
Producing body movements
Stabilizing body positions
Regulating organ volumes (e.g., sphincters)
Movement of substances (e.g., blood, lymph, urine, air, food, sperm)
Producing heat (e.g., shivering)
Properties of Muscle Tissue
Muscle tissue exhibits five key properties:
Excitability: Ability to respond to stimuli (e.g., neurotransmitters)
Conductivity: Ability to propagate electrical signals
Contractility: Ability to shorten and generate force
Extensibility: Ability to stretch without damage
Elasticity: Ability to return to original shape after stretching
Skeletal Muscle Structure
Organization of Skeletal Muscle
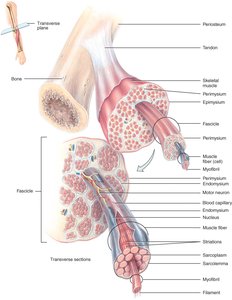
Each skeletal muscle is an organ composed of muscle fibers (cells) and connective tissue layers:
Epimysium: Surrounds the entire muscle
Perimysium: Surrounds bundles (fascicles) of 10–100 muscle cells
Endomysium: Separates individual muscle cells
Tendons: Extensions of connective tissue attaching muscle to bone
Aponeuroses: Broad, flat tendons connecting muscle to muscle or bone
Nerve and Blood Supply
Each skeletal muscle receives a nerve, artery, and two veins. Motor neurons form neuromuscular junctions with muscle fibers, and capillaries supply nutrients and oxygen.
Muscle Fiber Structure
Muscle fibers are long, cylindrical, multinucleated cells with specialized structures:
Sarcolemma: Muscle cell membrane
Sarcoplasm: Cytoplasm containing myofibrils and myoglobin
T tubules: Invaginations of the sarcolemma that transmit action potentials
Mitochondria: Abundant for ATP production
Myofibrils, Sarcoplasmic Reticulum, and Myofilaments
Myofibrils are composed of repeating units called sarcomeres, the functional units of muscle contraction. The sarcoplasmic reticulum (SR) stores calcium ions, which are essential for contraction. Myofibrils contain two main types of myofilaments:
Thick filaments: Composed of myosin
Thin filaments: Composed of actin, troponin, and tropomyosin
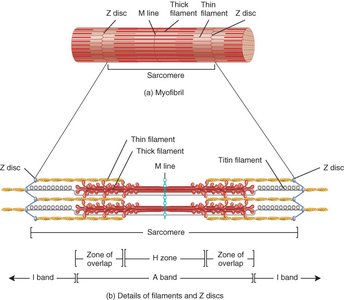
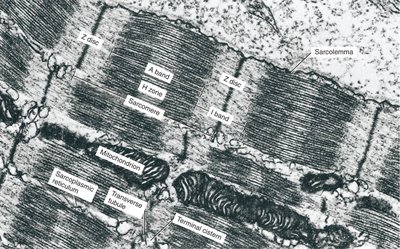
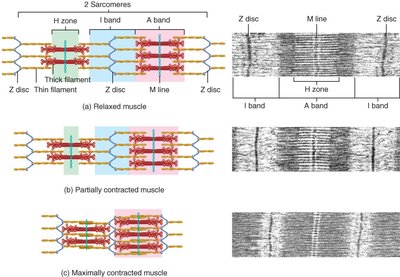
Sarcomere Structure
Sarcomeres are defined by Z discs and contain overlapping thick and thin filaments, creating striations:
I band: Contains only thin filaments
A band: Contains thick filaments and regions of overlap
M line: Center of the sarcomere, supporting proteins
Titin: Provides elasticity and structural support
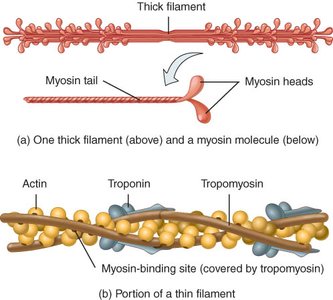
Muscle Proteins
Myofibrils are built from three classes of proteins:
Contractile proteins: Myosin (thick) and actin (thin)
Regulatory proteins: Troponin and tropomyosin (control contraction)
Structural proteins: Titin, myomesin, nebulin, dystrophin (alignment and elasticity)
Muscle Contraction Mechanism
Sliding Filament Theory
Muscle contraction occurs when myosin heads pull on actin filaments, sliding them toward the center of the sarcomere. This shortens the sarcomere and the muscle fiber, but the filaments themselves do not change length.
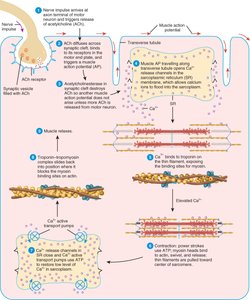
Excitation-Contraction Coupling
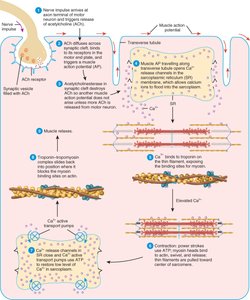
The process linking muscle excitation to contraction involves several steps:
Nerve impulse triggers release of acetylcholine (ACh) at the neuromuscular junction.
ACh binds to receptors on the sarcolemma, opening Na+ channels and generating an action potential.
Action potential travels down T tubules, triggering Ca2+ release from the SR.
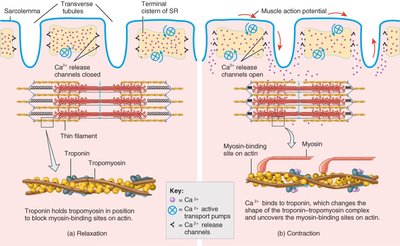
Ca2+ binds to troponin, shifting tropomyosin and exposing myosin-binding sites on actin.
Contraction cycle begins.
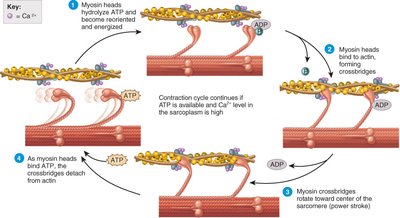
Contraction Cycle
The contraction cycle consists of four main steps:
ATP hydrolysis by myosin heads
Attachment of myosin to actin (crossbridge formation)
Power stroke (myosin head pivots, pulling actin)
Detachment of myosin from actin (new ATP binds)
Relaxation
Relaxation occurs when ACh is broken down by acetylcholinesterase, Ca2+ is pumped back into the SR, and the troponin-tropomyosin complex covers the myosin-binding sites on actin.
Muscle Tension and Control
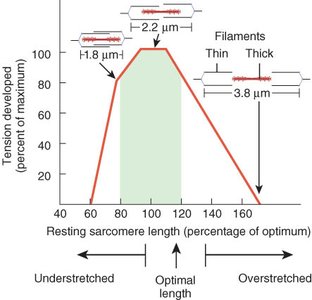
Length-Tension Relationship
The force of muscle contraction depends on the initial length of the sarcomeres. Optimal overlap of thick and thin filaments produces maximal tension. Overstretching or excessive shortening reduces force production.
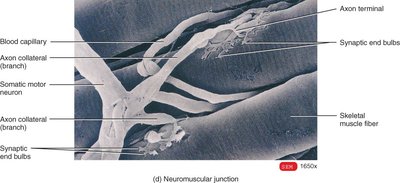
Neuromuscular Junction (NMJ)
The NMJ is the synapse between a motor neuron and a skeletal muscle fiber. It includes the synaptic end bulb (containing ACh vesicles) and the motor end plate (with ACh receptors).
Muscle Metabolism
Muscle fibers generate ATP through three main pathways:
Creatine phosphate: Short-term, high-intensity energy (about 15 seconds)
Anaerobic glycolysis: Produces ATP and lactic acid (30–40 seconds)
Aerobic respiration: Long-term ATP production using oxygen
Muscle Fatigue
Fatigue is the inability to contract after prolonged activity, caused by factors such as depletion of ACh, creatine phosphate, Ca2+, oxygen, or glycogen, and accumulation of lactic acid and ADP.
Motor Units and Recruitment
A motor unit consists of one motor neuron and all the muscle fibers it stimulates. The strength of contraction depends on the number and size of motor units activated.
Muscle Contraction Types
Isotonic contractions: Muscle changes length (concentric = shortens, eccentric = lengthens)
Isometric contractions: Muscle develops tension without changing length

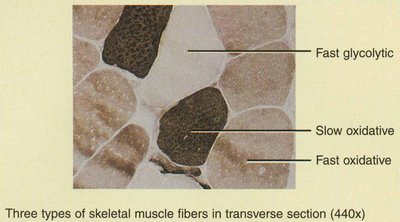
Muscle Fiber Types
Classification of Muscle Fibers
Muscle fibers are classified based on their contraction speed and metabolic properties:
Type | Color | Features | Function |
|---|---|---|---|
Slow oxidative (SO) | Red | Many mitochondria, myoglobin, blood vessels | Posture, endurance |
Fast oxidative-glycolytic (FOG) | Red | Intermediate properties | Walking, sprinting |
Fast glycolytic (FG) | White | Few mitochondria, low myoglobin | Short, powerful movements |
Muscle Disorders and Adaptations
Muscle Disorders
Myasthenia gravis: Autoimmune disorder blocking ACh receptors, causing muscle weakness
Muscular dystrophies: Inherited diseases causing muscle degeneration (e.g., Duchenne muscular dystrophy)
Abnormal contractions: Spasms, cramps, tics, tremors, fasciculations
Atrophy: Wasting of muscle due to disuse or nerve damage
Hypertrophy: Increase in muscle fiber size due to intense activity
Rigor mortis: Post-mortem muscle rigidity due to Ca2+ leakage and lack of ATP
Muscle Adaptations
Exercise-induced muscle damage: Microscopic tears, soreness, and adaptation
Aging: Replacement of muscle with fat, decreased strength, and slower reflexes
Anabolic steroids: Increase muscle mass but have serious side effects
Additional info: This guide integrates foundational concepts of muscle tissue structure, function, and physiology, suitable for introductory anatomy and physiology courses.
