 Back
BackMuscle Tissue: Structure, Function, and Physiology
Study Guide - Smart Notes

Muscle Tissue
Overview of Muscle Tissue
Muscle tissue is a primary tissue type responsible for contraction and movement in the human body. There are three main types of muscle tissue, each with distinct structures and functions:
Skeletal muscle: Moves the body by pulling on bones.
Cardiac muscle: Pumps blood through the cardiovascular system.
Smooth muscle: Pushes fluids and solids through internal passageways and organs.
Common Properties of Muscle Tissue
Excitability (Responsiveness): Ability to receive and respond to stimuli.
Contractility: Ability of cells to shorten and generate force.
Extensibility: Ability of the muscle to stretch without being damaged.
Elasticity: Ability of the muscle to recoil to its resting length after stretching.
Functions of Skeletal Muscle
Producing movement by pulling on tendons to move bones.
Maintaining posture and body position.
Supporting soft tissues.
Guarding body entrances and exits (e.g., urinary and digestive tracts).
Maintaining body temperature through heat production.
Storing nutrients as a source of proteins and amino acids.
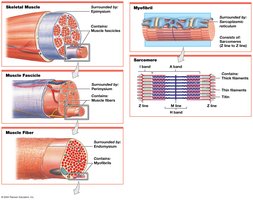
Organization of Skeletal Muscle
Muscle Structure at the Tissue Level
Skeletal muscles are composed of muscle tissue, connective tissues, blood vessels, and nerves. They are organized into several layers:
Epimysium: Surrounds the entire muscle and separates it from surrounding tissues; connected to deep fascia.
Perimysium: Surrounds individual fascicles (bundles of muscle fibers); contains blood vessels and nerves.
Endomysium: Surrounds individual muscle fibers; contains capillaries, nerve fibers, and stem cells for repair.
The collagen fibers of these layers converge to form tendons (attach muscle to bone) or aponeuroses (attach muscle to muscle or bone).
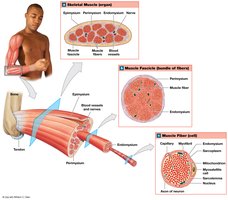
Blood Supply and Innervation
Skeletal muscles have extensive blood vessels to deliver oxygen and nutrients and remove wastes.
Muscle contraction is initiated by stimulation from the central nervous system via motor neurons.
Most skeletal muscles are voluntary, but some (e.g., diaphragm) can function subconsciously.
Skeletal Muscle Fibers
Characteristics of Skeletal Muscle Fibers
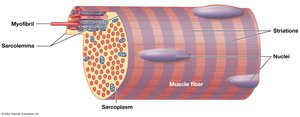
Skeletal muscle fibers are large, multinucleate, and striated due to the arrangement of myofibrils. These fibers are also known as striated muscle cells.
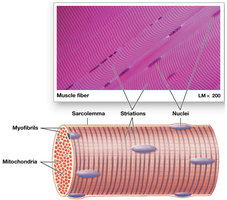
Internal Organization of Muscle Fibers
Sarcolemma: Plasma membrane of a muscle fiber; surrounds the sarcoplasm (cytoplasm).
Transverse tubules (T tubules): Extensions of the sarcolemma that transmit action potentials into the cell interior for coordinated contraction.
Sarcoplasmic reticulum (SR): Specialized endoplasmic reticulum that stores and releases calcium ions; forms terminal cisternae adjacent to T tubules, creating a triad.
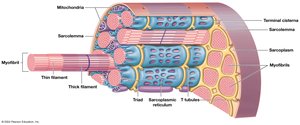
Myofibrils and Myofilaments
Myofibrils: Long, rod-like structures composed of myofilaments; responsible for muscle contraction.
Myofilaments: Protein filaments of two types:
Thin filaments: Primarily actin.
Thick filaments: Primarily myosin.
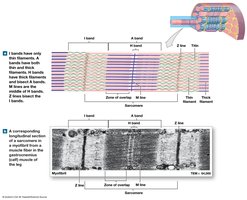
Sarcomere Structure
The sarcomere is the smallest functional unit of a muscle fiber, defined by the arrangement of thick and thin filaments. Sarcomeres are responsible for the striated appearance of skeletal muscle and are the site of muscle contraction.
A bands: Dark bands containing thick filaments.
I bands: Light bands containing only thin filaments.
M line: Center of the A band; stabilizes thick filaments.
H band: Region with only thick filaments.
Zone of overlap: Area where thick and thin filaments overlap.
Z lines: Define the boundaries of each sarcomere; bisect the I bands.
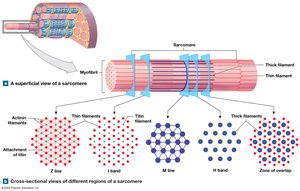
Levels of Functional Organization
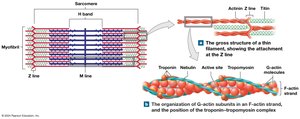
Thin and Thick Filaments
Thin filaments contain:
F-actin: Twisted strand of G-actin molecules with active sites for myosin binding.
Tropomyosin: Covers active sites on actin, preventing myosin binding.
Troponin: Binds to tropomyosin and calcium ions; moves tropomyosin off active sites when calcium is present.
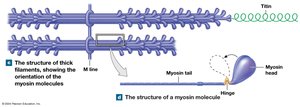
Thick filaments contain:
Myosin: Each molecule has a tail (binds other myosin) and a head (binds actin).
Titin: Elastic protein that helps return the sarcomere to resting length.
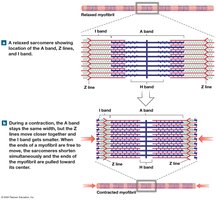
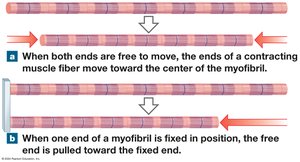
Sliding Filament Theory
During muscle contraction, thin filaments slide toward the M line alongside thick filaments, causing the sarcomere to shorten. The A band remains constant, while the H and I bands narrow, and Z lines move closer together.
Muscle Contraction
Excitable Membranes and Action Potentials
All cells maintain a negative resting membrane potential; in skeletal muscle, this is about -85 mV.
Depolarization: Membrane potential becomes less negative (Na+ influx).
Repolarization: Return to resting potential after depolarization.
Action potentials: Electrical impulses that propagate along the membrane, triggering contraction.
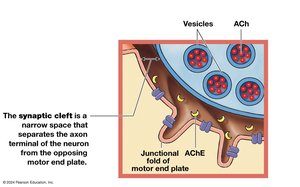
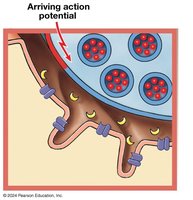
Neuromuscular Junction (NMJ)
The NMJ is the synapse between a motor neuron and a skeletal muscle fiber. Key components include:
Axon terminal: End of the motor neuron.
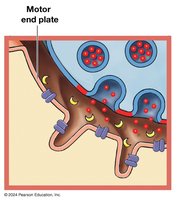
Motor end plate: Folded region of the muscle fiber's membrane.
Synaptic cleft: Space between axon terminal and motor end plate.
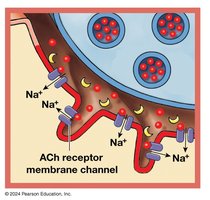
Neurotransmitter (acetylcholine, ACh): Released from the axon terminal, binds to receptors on the motor end plate, causing Na+ influx and depolarization.
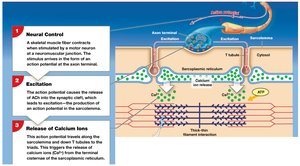
Excitation–Contraction Coupling
This process links the generation of an action potential in the sarcolemma to the start of muscle contraction. The action potential travels down T tubules, triggering calcium release from the SR. Calcium binds to troponin, moving tropomyosin and exposing actin active sites for contraction.
The Contraction Cycle
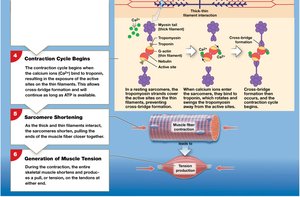
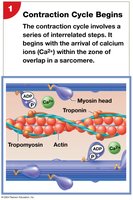
The contraction cycle involves several steps:
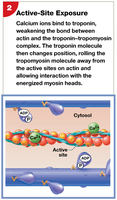
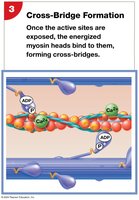
Calcium binds to troponin, exposing active sites on actin.
Myosin heads bind to actin, forming cross-bridges.
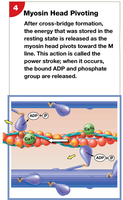
Power stroke: Myosin head pivots, pulling actin toward the M line (uses ATP).
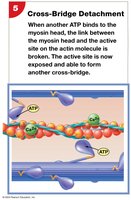
ATP binds to myosin, causing detachment from actin.
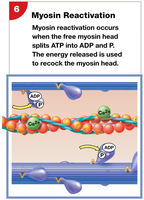
Myosin head is reactivated by ATP hydrolysis.
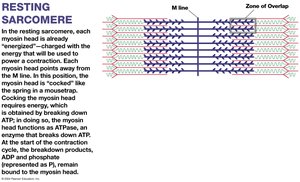
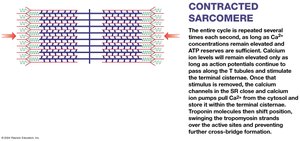
Relaxation
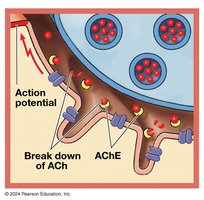
Contraction ends when stimulation ceases, ACh is broken down, and calcium is pumped back into the SR.
Troponin and tropomyosin return to their original positions, covering actin active sites.
Rigor Mortis
After death, ATP production ceases, calcium remains in the cytosol, and cross-bridges cannot detach, resulting in muscle stiffness (rigor mortis).
Muscle Tension
Mechanisms of Tension Production
The amount of tension produced by a muscle fiber depends on:
Number of power strokes performed (cross-bridge cycling).
Resting length of the muscle fiber (length-tension relationship).
Frequency of stimulation.
Length–Tension Relationship
Tension is maximal when the optimal overlap between thick and thin filaments allows the greatest number of cross-bridges to form. Too little or too much overlap reduces tension.
Frequency of Stimulation
Twitch: Single stimulus-contraction-relaxation sequence.
Treppe: Increased tension with repeated stimulation after relaxation.
Wave summation: Increased tension with successive stimuli before relaxation is complete.
Tetanus: Maximum tension; can be incomplete (partial relaxation) or complete (no relaxation).
Types of Muscle Contractions
Motor Units and Recruitment
Motor unit: A motor neuron and all the muscle fibers it controls.
Recruitment: Increasing the number of active motor units to increase tension.
Motor unit summation: Alternating active and resting motor units for sustained contractions.
Muscle Tone
Resting tension that stabilizes bones and joints and maintains posture.
Elevated muscle tone increases resting energy consumption.
Types of Contractions
Isotonic contractions: Muscle changes length.
Concentric: Muscle shortens as tension exceeds load.
Eccentric: Muscle lengthens as tension is less than load.
Isometric contractions: Muscle develops tension but does not change length.
Load and Speed of Contraction
The heavier the load, the slower the contraction and the less the muscle shortens. There is an optimal combination of tension and speed for each muscle and load.
Muscle Relaxation and Return to Resting Length
Return to resting length is passive, aided by elastic forces, opposing muscle contractions, and gravity.
Energy for Muscle Contraction
ATP Generation and Muscle Metabolism
ATP is the direct energy source for muscle contraction; stores are depleted in 4–6 seconds of activity.
ATP is regenerated by:
Creatine phosphate (CP): Transfers energy to ADP to form ATP (catalyzed by creatine kinase).
Glycolysis: Anaerobic breakdown of glucose to pyruvate (net 2 ATP per glucose).
Aerobic metabolism: Mitochondrial breakdown of pyruvate (or fatty acids) using oxygen (up to 15 ATP per pyruvate).
Muscle Metabolism at Different Activity Levels
At rest: Muscles use fatty acids, store glycogen and CP.
Moderate activity: ATP from aerobic breakdown of glucose.
Peak activity: ATP from glycolysis; lactic acid accumulates, causing fatigue.
Recovery Period and Oxygen Debt
Recovery period: Time needed for muscles to return to pre-exertion state; lactate is recycled in the liver (Cori cycle).
Oxygen debt (EPOC): Extra oxygen required after exercise to restore normal conditions.
Heat Production
Active muscles release up to 85% of the heat needed to maintain body temperature.
Hormonal Regulation
Growth hormone, testosterone, thyroid hormones, and epinephrine influence muscle metabolism and performance.
Muscle Performance and Fiber Types
Types of Skeletal Muscle Fibers
Fast fibers: Large, contract quickly, strong but fatigue rapidly; few mitochondria, white in color.
Slow fibers: Small, contract slowly, high endurance; many mitochondria, myoglobin, red in color.
Intermediate fibers: Mid-sized, moderate endurance and force; little myoglobin.
Muscle Hypertrophy and Atrophy
Hypertrophy: Increase in muscle size due to training (more myofibrils, mitochondria, glycogen).
Atrophy: Decrease in muscle size, tone, and power due to inactivity; severe atrophy is irreversible.
Aging and Muscle Tissue
Muscle fibers decrease in diameter and elasticity; increased fibrosis; reduced exercise tolerance and recovery; fewer satellite cells.
Muscle Fatigue
Occurs when muscles cannot perform at required levels due to metabolic depletion, damage, pH changes, or pain.
Physical Conditioning
Anaerobic endurance: Short, intense activity; improves power and hypertrophy.
Aerobic endurance: Prolonged, low-intensity activity; improves cardiovascular performance and increases slow fibers.
Cross-training: Combines aerobic and anaerobic exercises for overall improvement.
Cardiac Muscle Tissue
Structure and Function
Found only in the heart; small, branched, striated cells with a single nucleus.
Connected by intercalated discs (gap junctions and desmosomes) for synchronized contraction.
Dependent on aerobic metabolism; many mitochondria and myoglobin.
Automaticity: Pacemaker cells initiate contraction without neural input.
No wave summation or tetanus; longer contractions and refractory periods.
Smooth Muscle Tissue
Structure and Function
Found in walls of hollow organs and blood vessels; spindle-shaped, non-striated cells with a single nucleus.
No T tubules, myofibrils, or sarcomeres; thin filaments attached to dense bodies.
Functions in movement of materials, regulation of blood flow, and organ function.
Functional Characteristics
Excitation–contraction coupling involves calcium entry and calmodulin activation of myosin light chain kinase.
Plasticity: Can function over a wide range of lengths.
Multiunit and visceral types; control varies by location and function.
Smooth muscle tone: Maintains background activity, modulated by neural, hormonal, or chemical factors.
Summary Table: Muscle Tissue Types
Feature | Skeletal Muscle | Cardiac Muscle | Smooth Muscle |
|---|---|---|---|
Location | Attached to bones | Heart | Walls of hollow organs |
Cell Shape | Long, cylindrical, multinucleate | Short, branched, single nucleus | Spindle-shaped, single nucleus |
Striations | Yes | Yes | No |
Control | Voluntary | Involuntary (automaticity) | Involuntary |
Special Features | Rapid contraction, fatigue, regeneration | Intercalated discs, pacemaker cells | Plasticity, slow contraction |
