 Back
BackMuscle Tissue Types: Cardiac and Smooth Muscle Structure and Function
Study Guide - Smart Notes

Cardiac Muscle Tissue
Structure and Location
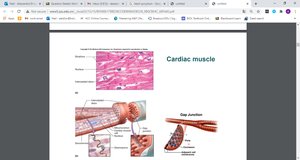
Cardiac muscle tissue is found exclusively in the walls of the heart. It is composed of branching chains of cells that are typically uni- or binucleate and display striations due to the organized arrangement of contractile proteins.
Involuntary control: Cardiac muscle contracts without conscious control, regulated by the autonomic nervous system and intrinsic pacemaker cells.
Striated and branched: The tissue exhibits visible striations and branched fibers, distinguishing it from smooth muscle.
Single or binucleate cells: Most cardiac muscle cells contain one nucleus, but some may have two.

Electrical Properties and Intercalated Discs
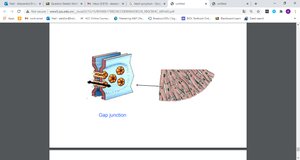
Cardiac muscle cells are electrically connected by specialized structures called intercalated discs, which contain gap junctions. These allow the heart to function as a coordinated unit, or electrical syncytium.
Gap junctions: Permit the rapid transmission of action potentials between cells, ensuring synchronized contraction.
Desmosomes: Provide mechanical strength by anchoring cells together.
Pacemaker Activity and Cardiac Conduction System
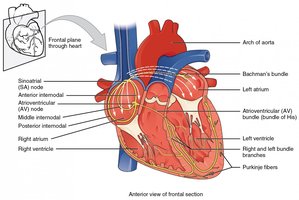
The heart's rhythm is established by the sinoatrial (SA) node, a cluster of specialized myocardial cells in the right atrium. The SA node initiates the sinus rhythm, which is the normal electrical pattern of the heart.
Pacemaker cells: The SA node has the highest rate of spontaneous depolarization, setting the pace for the heart.
Conduction pathway: The electrical impulse travels from the SA node through the atria, atrioventricular (AV) node, bundle branches, and Purkinje fibers, coordinating contraction.
Neural and Hormonal Regulation
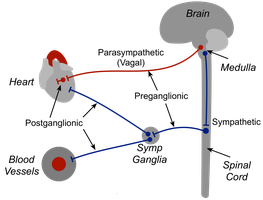
Cardiac muscle is primarily controlled by intrinsic pacemaker activity but can be modulated by the autonomic nervous system and hormones such as epinephrine and norepinephrine.
Sympathetic stimulation: Increases heart rate and force of contraction.
Parasympathetic stimulation: Decreases heart rate.
Action Potentials and Calcium Dynamics
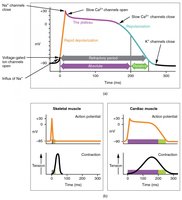
Cardiac muscle action potentials are characterized by a prolonged depolarization phase (plateau) due to the influx of calcium ions through slow calcium channels. This results in a longer refractory period compared to skeletal muscle, preventing tetanus and allowing the heart to relax between beats.
Plateau phase: Maintained by Ca2+ influx, lasting 200-250 ms.
Role of Ca2+: Essential for contraction and the prolonged refractory period.
Smooth Muscle Tissue
Structure and Location
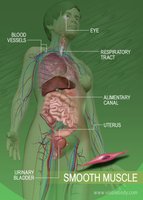
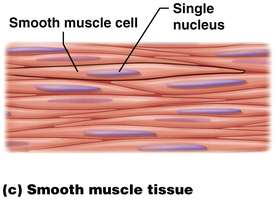
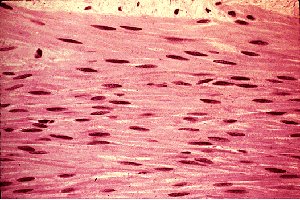
Smooth muscle tissue is found in the walls of hollow organs such as the stomach, intestines, blood vessels, and bladder. The cells are spindle-shaped, uninucleate, and lack striations.
Involuntary control: Smooth muscle contracts without conscious control, often regulated by the autonomic nervous system, hormones, or local factors.
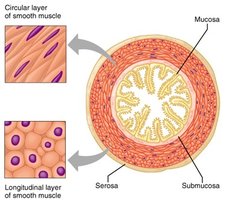
Sheet arrangement: Cells are organized into sheets, often in two layers (longitudinal and circular) that facilitate coordinated contractions.

Electrical and Contractile Properties
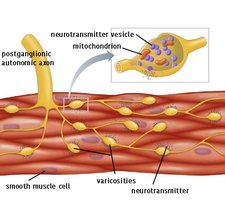
Smooth muscle cells communicate via gap junctions, allowing for slow, synchronized contractions. Some cells act as pacemakers, generating spontaneous action potentials that spread through the tissue.
Autorhythmicity: Some smooth muscle cells can contract spontaneously without external stimulation.
Varicosities: Autonomic nerve fibers release neurotransmitters from varicosities, affecting multiple cells simultaneously.
Ultrastructure and Calcium Handling
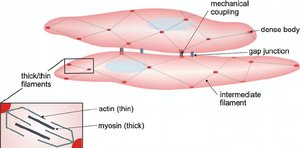
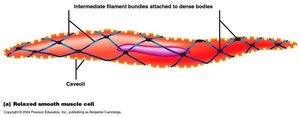
Smooth muscle contains actin and myosin filaments, but they are not arranged in sarcomeres. Dense bodies serve as anchoring points for actin, and caveolae in the plasma membrane function similarly to T-tubules, facilitating calcium entry from the extracellular fluid (ECF).
No striations: Filaments are arranged diagonally, resulting in a non-striated appearance.
Caveolae: Invaginations in the membrane that concentrate Ca2+ channels.
Calcium source: Most Ca2+ for contraction comes from the ECF, not the sarcoplasmic reticulum.

Mechanism of Contraction
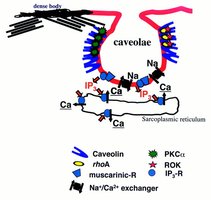
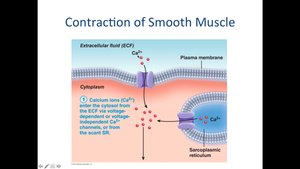
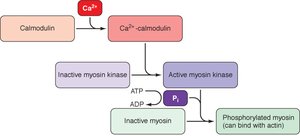
Smooth muscle contraction is initiated by an increase in intracellular Ca2+, which binds to calmodulin. The Ca2+-calmodulin complex activates myosin light chain kinase (MLCK), which phosphorylates myosin, allowing it to bind to actin and generate tension.
Ca2+ enters the cell from the ECF and sarcoplasmic reticulum.
Ca2+ binds to calmodulin, forming a complex.
The complex activates MLCK.
MLCK phosphorylates myosin, increasing ATPase activity.
Phosphorylated myosin binds to actin, resulting in contraction.
Comparison of Smooth and Skeletal Muscle Contraction
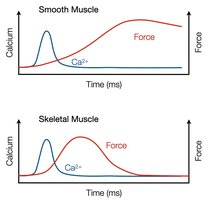
While both muscle types rely on Ca2+ for contraction, the mechanisms differ. In skeletal muscle, Ca2+ binds to troponin, moving tropomyosin and exposing myosin-binding sites on actin. In smooth muscle, Ca2+ binds to calmodulin, leading to myosin phosphorylation.
Skeletal muscle: Fast contraction, Ca2+ from sarcoplasmic reticulum, troponin-tropomyosin regulation.
Smooth muscle: Slow, sustained contraction, Ca2+ mainly from ECF, calmodulin-MLCK regulation.
Regulation of Smooth Muscle Contraction
Smooth muscle contraction can be regulated by neural, hormonal, and local factors. Neurotransmitters such as acetylcholine and norepinephrine, as well as hormones and changes in pH, oxygen, and carbon dioxide, can modulate contraction.
No neuromuscular junctions: Neurotransmitters are released from varicosities.
Multiple stimuli: Action potentials, stretching, hormones, and local chemical changes can all trigger contraction.

Summary Table: Comparison of Muscle Types
Characteristic | Skeletal Muscle | Cardiac Muscle | Smooth Muscle |
|---|---|---|---|
Body Location | Attached to bones or skin | Walls of the heart | Walls of hollow organs (stomach, blood vessels, etc.) |
Cell Shape & Appearance | Long, cylindrical, multinucleate, striated | Branching chains, uni- or binucleate, striated | Spindle-shaped, uninucleate, no striations |
Control | Voluntary | Involuntary | Involuntary |
Special Features | Rapid contraction, fatigues easily | Intercalated discs, pacemaker cells | Gap junctions, autorhythmicity, slow sustained contraction |

